The Importance of Biofilm Removal
Periodontal and peri-implant involvement has been described as microbially associated, host-mediated inflammation resulting in loss of attachment.1 Biofilm accumulates interproximally, increasing the pathogenic potential of the bacterial load — thus favoring the development of periodontal diseases. Daily interproximal biofilm disruption can reduce inflammation and disease, and, consequently, improve clinical outcomes.2–5
The availability of a user-friendly interdental cleaning device with a large body of evidence documenting its effectiveness in combatting inflammation would be advantageous for individuals diagnosed in various stages/grades of the American Academy of Periodontology (AAP) disease classification system. No single device or approach has been demonstrated in studies as unequivocally superior. Rather, limited (and largely low-quality) research suggests various interproximal oral hygiene devices may be of value, depending on factors related to patient parameters.2
When personalizing self-care recommendations, providers should consider the dexterity and preferences of the individual, along with the patient’s overall oral condition and AAP periodontal classification.
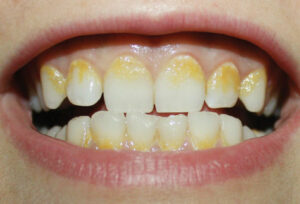
One classic sign of the inflammation associated with gingivitis is bleeding.6 With effective control of pathogenic biofilm, a decrease in bleeding can be evident to patients — although these changes can take up to a week to occur.7 By then, discouragement by not seeing tangible improvement could impact compliance with interdental cleaning. For those with “floss fatigue,” it can be refreshing when a device other than floss is recommended, such as interdental brushes, wooden sticks, and water flossers.
The use of interdental brushes is well accepted by patients and associated with higher biofilm removal levels than flossing or use of wooden sticks.8 Although evidence indicates interdental brushes remove interdental biofilm efficiently, direct evidence documenting their effects on gingival health is currently lacking.8
There are limited data from which to draw conclusions about gingival benefits with the use of wooden sticks. A systematic review concluded that while wooden sticks do not necessarily demonstrate visible biofilm removal, improvements were documented in gingival health.9
Mechanized devices that use bursts of either air and/or water to help clean interproximal areas are available. While studies of water flossers document improved clinical signs of gingivitis,10,11 corresponding biofilm removal is not as strongly demonstrable.12 One possible explanation is that water under pressure can disrupt and alter pathogenic bacteria, rendering it less pathogenic, yet not visibly change biofilm amounts when viewed with a disclosing solution. A randomized controlled trial on the safety and efficacy of the water flosser found that it was more effective at plaque control and addressing gingival inflammation when used with a toothbrush in comparison to the use of a toothbrush alone.13
Interdental cleaning in conjunction with toothbrushing may lead to a greater reduction in gingivitis or plaque, or both, compared to using only a toothbrush. However, the available evidence on the efficacy of interdental brushes, wooden sticks, and water flossers is limited and inconsistent.2
Future studies should aim to categorize participants’ periodontal status according to the updated classification of periodontal diseases. Additionally, these studies should extend over a sufficient duration to accurately measure impact on gingivitis and periodontal diseases.2
References
- Tonetti MS, Greenwell H, Korman KS. Staging and grading of periodontitis: framework and proposal of a new classification and case definition. J Periodontol. 2018;89(Suppl 1):S159–S172.
- Worthington HV, MacDonald L, Poklepovic Pericic T, et al. Home use of interdental cleaning devices, in addition to toothbrushing, for preventing and controlling periodontal diseases and dental caries. Cochrane Database Syst Rev. 2019;4(4):CD012018.
- Jackson MA, Kellett M, Worthington HV, Clerehugh V. Comparison of interdental cleaning methods: a randomized controlled trial. J Clin Periodontol. 2006;77:1421–1429.
- Salzer S, Slot DE, Van der Weijden FA, Dorfer CE. Efficacy of inter-dental mechanical plaque control in managing gingivitis — a meta-review. J Clin Periodontol. 2015;42(Suppl 16):S92–S105.
- Chapple IL, Van der Weijden F, Doerfer C, et al. Primary prevention of periodontitis: managing gingivitis. J Clin Periodontol. 2015;42(Suppl 16):S71–S76.
- Lang NP, Bartold PM. Periodontal health. J Clin Periodontol. 2018;45(Suppl 20):S9–S16.
- Loe H, Theilade E, Jensen SB, Schiott C. Experimental gingivitis in man. 3. Influence of antibiotics on gingival plaque development. J Periodontol. 1965;36:177–187.
- Sälzer S, Slot DE, Van der Weijden FA, Dörfer CE. Efficacy of inter-dental mechanical plaque control in managing gingivitis: a meta-review. J Clin Periodontol. 2015;42(Suppl 16):S92–S105.
- Hoenderdos NL, Slot DE, Paraskevas S, Van der Weijden GA. The efficacy of woodsticks on plaque and gingival inflammation: a systematic review. Int J Dent Hyg. 2008:6;280–289.
- Lyle DM, Qaqish JG, Goyal CR, Schuller R. Efficacy of the use of a water flosser in addition to an electric toothbrush on clinical signs of inflammation: 4-week randomized controlled trial. Compend Cont Edu Dent. 2020; 41:170–177.
- Xu X, Zhou Y, Liu C, et al. Effects of water flossing on gingival inflammation and supragingival plaque microbiota: a 12-week randomized controlled trial. Clin Oral Investig. 2023 May 25:1–11.
- Hussini A, Slot DE, Van der Weijden GA. The efficacy of oral irrigation in addition to a toothbrush on plaque and the clinical parameters of periodontal inflammation: a systematic review. Int J Dent Hyg. 2008;6:304–314.
- Ren X, He J, Cheng R, et al. The efficacy and safety of oral irrigator on the control of dental plaque and gingivitis: a randomized, single-blind, parallel-group clinical trial. Int J Environ Res Public Health. 2023;20:3726.
From Decisions in Dentistry. September 2023; 1(8):46.


