 GARO MANJIKIAN/ISTOCK/GETTY IMAGES PLUS
GARO MANJIKIAN/ISTOCK/GETTY IMAGES PLUS
Overcoming Soft Tissue Complications During Implant Restoration
Adopting a biological-driven approach will lead to functional and esthetic implant restorations, while supporting stability in the surrounding tissues.
In the initial era of endosteal implants, the location of implants was determined by bone availability. During the 2000s, the three-dimensional implant positioning concept was developed to enhance esthetic and functional outcomes. Currently, an extra layer has been added in implant dentistry — the biological-driven approach, which not only supports functional and esthetic implant restoration, but also harmony and stability in the surrounding tissues.1,2 The purpose of this article is to identify and explore various tissue reactions that may present when restoring dental implants.
Modern techniques include not only placing implants at bone-level height, but also providing adequate space for the restorations and development of the emergence profile.3,4 The latter is defined as the “contour of a tooth or restoration, such as the crown on a natural tooth, dental implant or dental implant abutment, as it relates to the emergence from circumscribed soft tissues.”5,6 In contrast, biological width is defined as the “combined width of connective tissue and junctional epithelial attachment formed adjacent to a tooth and superior to the crestal bone.”5–7 Biological width in implant cases will form regardless of the use of a healing abutment or a provisional restoration, while an optimal emergence profile can only be created by using adequately contoured provisional restorations.
The emergence profile of the implant restoration starts from the day of the surgery with a one-stage surgical approach, using either a healing abutment or provisional restoration. A generic healing abutment provides an emergence profile shape determined by the design itself. Thus, the use of a provisional restoration provides a more ideal shape that follows the natural contours of the teeth. The abutment/provisional traverses the soft tissues and is in direct contact with epithelium and connective tissue of the peri-implant socket.7 Ideally, the prosthetic connection should establish a biological seal and integrate with the surrounding tissues.8–12 Greater changes in the emergence profile during the provisional phase can generate an undesirable reaction of the tissue, thereby compromising and delaying the final restorations.
Even if operators respect these surgical and restorative principles, implant complications can still occur. A recent report by Adler et al13 evaluated long-term outcomes after implant therapy, as well as biological and technical complications rates in 1095 treated implants over a period of nine to 15 years. They concluded the prevalence of biological and technical complications at the patient level were 52% and 32%, respectively. The literature divided implant complications into two general categories: prosthetic and biologic.14 Prosthetic complications pertain to technical and mechanical damage to the implant, implant components, and/or prosthesis occurring after delivery of the definitive prosthesis. Biologic complications refer to adverse biologic outcomes affecting the supporting peri-implant hard and soft tissues. Biologic complications can be divided based on when they occur: complications before osseointegration (such as early implant failure or bone loss), and complications after osseointegration (such as peri-implant mucositis, peri-implantitis, bone loss, soft tissue recession or hypertrophy).15,16
Prosthetic factors may also influence the occurrence of biological complications.17,18 For example, prosthetic designs that inhibit adequate self-care plaque removal are considered a local risk factor for peri-implant inflammation. While it appears that prosthetic design factors may affect the prevalence of biological complications,19,20 there is a paucity of information on this subject.

PERI-IMPLANT ABSCESS
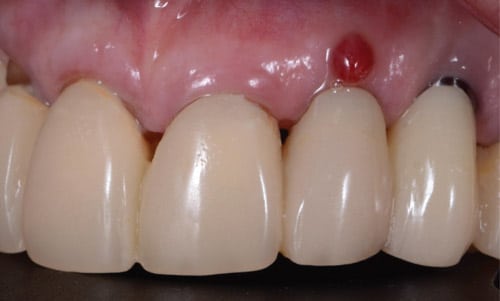
The Glossary of Periodontal Terms defines a gingival abscess as a localized purulent infection that involves the marginal gingiva or interdental papilla.21 In implant sites, however, abscesses can occur in the coronal part of the implant (always in the restorative area). These are unlikely to advance into the bone and create bone loss (Figure 1). Clinically, an abscess presents with swelling, bleeding or intermittent discharge of purulent matter, as well as patient discomfort following implant uncovering surgery.
A peri-implant abscess usually presents shortly after second-stage surgery due to poor oral hygiene, early invasion by microorganisms, or a contour that does not allow the patient to adequately clean around the provisional. The biological width forms from the top of the peri-implant mucosa to the first bone-to-implant contact. When implants are placed subcrestally, the coronal bone above the implant platform resorbs to form the biologic width. It presents with more collagen fibers that flow parallel to the surfaces, providing less adhesion compared to natural tooth attachment.22 One study concluded that peri-implant inflammatory cells increased near the implant abutment interface due to contamination during the initial implant placement, abutment connection, or transmission of microorganisms from the oral environment after prosthesis delivery.23
Treatment consists of removing the healing abutment and profuse irrigation of the implant connection and peri-implant soft tissue area with saline or an antiseptic to flush any microorganisms that could be present in the area (Figure 2).
Antiseptic treatment involves the application of a potent antiseptic.24 Irrigation with chlorhexidine gluconate 0.12% creates a layer that coats the implant components and limits accumulation of microflora at the implant connection and prosthetic components.25 Additionally, the use of dry steam vapor deodorizes and disinfects the surfaces via heat and moisture. Clinicians are also advised to steam clean the provisional before insertion in the patient’s mouth to improve epithelial cell attachment and proliferation, and therefore the biological connection around the peri-implant cuff.26
Both techniques were employed in the cases described here. First, dry steam vapor was used on the prosthetic implant components; next, the components were soaked in chlorhexidine prior to insertion in the mouth. At the abscess site, irrigation with a syringe and chlorhexidine flushed the bacteria and coated the internal connection of the implant body.
TISSUE IMPINGEMENT
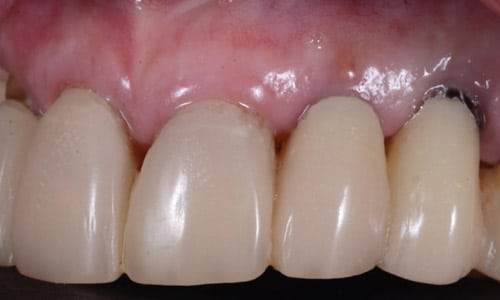
After healing from second-stage surgery, the patient was being treated for implant provisionalization and tissue contouring. When the patient presented for the final impression, swelling and erythema were observed in the distal-buccal area. Upon provisional removal, inflamed soft tissue was noted in the internal socket of the peri-implant tissue (Figure 3). In this case, the implant connection design was flat-to-flat; meaning, the platform of the implant body and seating area of the prosthetic component fit intimately when the components were connected.
In any given implant procedure, after removal of the prosthetic components, the soft tissue may start to collapse within minutes of the separation. Fabricating the provisional chairside, especially when developing contour, can take several minutes. During this time, the internal tissue of the implant socket can potentially become trapped between the implant platform and prosthetic component. When this occurs, swelling and inflammation of the tissue may result.

Possible reasons for this type of complication include: (1) increased apico-coronal depth, where the implant is placed too deep in comparison to the surrounding alveolar bone; (2) a flat-to-flat implant design; (3) collapsed tissue that was not removed at the time of the prosthetic connection; or (4) loosening or inadequate insertion torque of the prosthetic components.
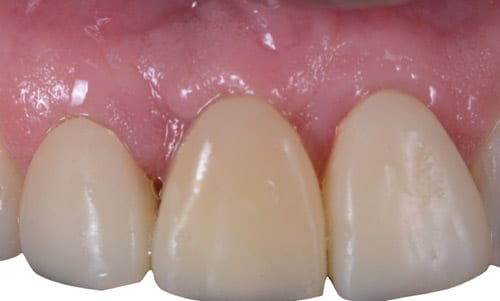
In this case, the area was treated by carefully removing the impinged tissue with a Gracey curet, while avoiding touching the implant platform to prevent scratching. Irrigation with saline solution helped flush blood from the site. At the time of reconnection of the provisional, special attention was paid to remove any tissue that could be on top of the platform. Figure 4 shows resolution after two weeks.
RESIN-ACRYLIC ALLERGIES
The patient shown in Figure 5 presented complaining of a burning and itchy sensation at the implant site following provisionalization. Swelling and inflammation were observed surrounding the tissue area of the implant provisional. The medical history noted a long list of allergies, including medications and food. At a previous appointment, an implant-supported provisional crown was fabricated using poly-methyl-methacrylate (PMMA) and a polyetheretherketone (PEEK) screw-retained implant cylinder.
While resin-based restorative materials are generally considered safe, their constituents can leach out and cause allergic contact stomatitis, as reported in a patient with mild erythema in the gingiva and buccal mucosa.27,28 The prevalence of contact allergy to methyl methacrylate is 1%.29 Various methods have been proposed to reduce the leachable substances from acrylic dentures, such as immersing in hot water (50° C) for one hour before insertion,29 or use of a different material for fabrication (such as resin composite or milled PMMA provisionals). The PMMA discs are pre-cured and then milled, and offer a lower level of residual monomer than conventional polymers.30,31

With this patient, the provisional restoration was removed and submerged in hot water for one hour. Subsequently, the provisional was polished using medium and fine pumice, followed by use of a high polisher.32 The internal socket of the peri-implant tissue was irrigated profusely with saline. Finally, the provisional was steam cleaned and placed back in the mouth.
At the two-week follow-up, improvement was observed in the site. However, some irritation was still present on the distal at the four-week follow-up. It was decided to make a final impression and deliver the final implant restoration for the site using the same material as previous restorations in the patient’s mouth. Figure 6 shows the two-week follow-up after delivery of the final restoration.
BONE GRAFTING ENCAPSULATION
The patient presented to start the prosthetic treatment after completing a two-stage surgical phase. In the first procedure, the implant was placed with simultaneous bone grafting (xenograft) and the site was allowed to heal. After healing and uncovering, a healing abutment was placed, and the tissue was allowed to heal. The use of bone grafting at the time of implant placement acts as a scaffold for the surrounding tissue. Common grafting techniques include the use of xenografts, autografts, or a 50:50 mix of both. Most of the time, these particles remain covered by a thin epithelium layer and will not cause adverse effect in the peri-implant socket.
At the restorative appointment, a provisional was fabricated to provide adequate soft and hard tissue architecture. A nonsurgical tissue sculpting procedure was planned, using a PEEK provisional cylinder and PMMA acrylic resin with moderate pressure in the tissue, allowing time for blood perfusion to return and prevent tissue necrosis.10
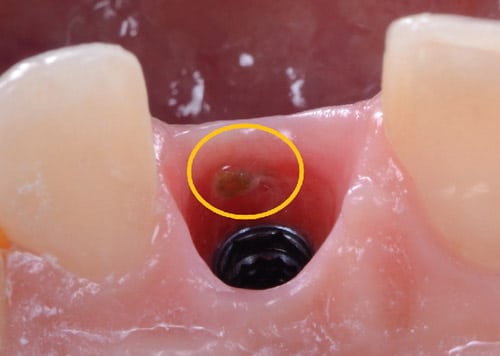
Changes in the emergence profile were made from a cylindrical to a triangular shape, which follows the coronal shape of the root of a central incisor. After three weeks, the patient returned, noting a slight discomfort in the implant site. A buccal abscess was observed in the soft tissue above the platform of the implant in the vicinity of the gingival margin. The tract of the abscess was traced with a periodontal probe. In the internal area of the peri-implant socket, an area of inflammation was seen surrounding a graft particle that was subsequently removed with a curet. (Figure 7). The area was irrigated with chlorhexidine gluconate 0.12% and the provisional was reinserted. At the two-week follow-up, the site had resolved and showed no signs of inflammation, bleeding or graft particles (Figure 8).
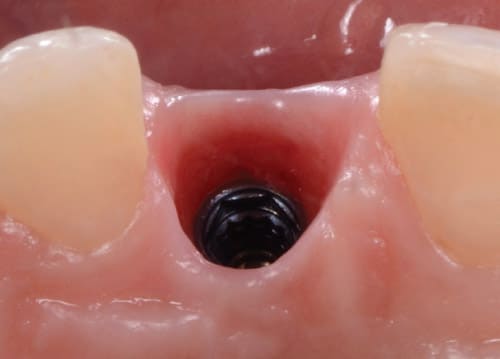
Graft particles can become embedded in the soft tissue, and, depending on the bone grafting material, can take a long time to reabsorb. Human studies show that demineralized autologous grafts or other alloplastic grafts left residual granules surrounded by connective tissue or immature bone after six to nine months.33 Changes in the emergence profile at the implant sites that underwent bone grafting procedures at the time of implant placement could expose the graft material in the peri-implant socket. Plaque and bacteria present in the peri-implant area also could colonize the exposed graft, possibly resulting in abscesses.
CONCLUSION
Successful outcomes hinge on the clinician’s biologic knowledge of the various tissues that surround dental implants, as this will allow operators to manage and address any complications that could present after loading. Soft tissue complications can occur during the implant’s healing period or restorative phase — but, when identified early, management should require minimum intervention. It is important to note, however, that soft tissue complications must be resolved completely before initiating the final restorative phase. Ultimately, taking a thorough medical and dental history is an essential tool in identifying, evaluating and addressing these types of complications.
Key Takeaways
- When restoring dental implants, adopting a biological-driven approach will support functional and esthetic implant restoration, as well as harmony and stability in the surrounding tissues.1,2
- Modern techniques include not only placing implants at bone-level height, but also providing adequate space for the restorations and development of the emergence profile.3,4
- Biological width in implant cases will form regardless of the use of a healing abutment or a provisional restoration, while an optimal emergence profile can only be created by using adequately contoured provisional restorations.
- The use of a provisional restoration provides a more ideal shape that follows the natural contours of the teeth.
- Ideally, the prosthetic connection should establish a biological seal and integrate with the surrounding tissues.8–12
- Successful restorative outcomes hinge on the clinician’s biologic knowledge of the various tissues that surround dental implants, as this will allow operators to manage and address any complications that could present after loading.
- Soft tissue complications can occur during the implant’s healing period or restorative phase — but, when identified early, management should require minimum intervention.
References
- Chu SJ, Salama MA, Salama H, et al. The dual-zone therapeutic concept of managing immediate implant placement and provisional restoration in anterior extraction sockets. Compend Contin Educ Dent. 2012;33:524–534.
- Mankoo T. Single-tooth implant restorations in the esthetic zone — contemporary concepts for optimization and maintenance of soft tissue esthetics in the replacement of failing teeth in compromised sites. Eur J Esthet Dent. 2007;2:274–295.
- Wittneben JG, Buser D, Belser UC, Brägger U. Peri-implant soft tissue conditioning with provisional restorations in the esthetic zone: the dynamic compression technique. Int J Periodontics Restorative Dent. 2013;33:447–455.
- Kan JYK, Rungcharassaeng K, Deflorian M, Weinstein T, Wang HL, Testori T. Immediate implant placement and provisionalization of maxillary anterior single implants. Periodontol 2000. 2018;77:197–212.
- Nordland WP, Tarnow D. A classification system for loss of papillary height. J Periodontol. 1998;69:1124–1126.
- The Academy of Prosthodontics. The glossary of prosthodontics terms. J Prosthet Dent. 2017;117(5s):e1–e105.
- Hermann JS, Buser D, Schenk R, et al. Biologic width around titanium implants. A physiologically formed and stable dimension over time. Clin Oral Implants Res. 2000;11:1–11.
- Schroeder HE, Listgarten MA. The gingival tissues: The architecture of periodontal protection. Periodontol 2000. 1997;13:91–120.
- Chee WW. Provisional restorations in soft tissue management around dental implants. Periodontol 2000. 2001;27:139–147.
- Zamzok J. Nonsurgical soft tissue sculpting. Alpha Omegan. 1997;90:65–69.
- Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19(Suppl):43–61.
- Cavallaro J, Greenstein G. Prosthodontic complications related to non-optimal dental implant placement. In: Froum SJ, ed. Dental Implant Complications: Etiology, Prevention, and Treatment. Ames, Iowa: Wiley-Blackwell; 2010:156–171.
- Adler L, Buhlin K, Jansson L. Survival and complications: A 9– to 15‐year retrospective follow‐up of dental implant therapy. J Oral Rehabil. 2020;47:67–77.
- Berglundh T, Persson L, Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J Clin Periodontol. 2002;29(Suppl 3):197–212.
- Derks J, Tomasi C. Peri-implant health and disease: a systematic review of current epidemiology. J Clin Periodontol. 2015;42:S158–S171.
- Berglundh T, Armitage G, Araujo MG, et al. Peri-implant diseases and conditions: consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri-implant Diseases and Conditions. J Periodontol. 2018;89:S313–S318.
- Wilson TG Jr. The positive relationship between excess cement and peri-implant disease: a prospective clinical endoscopic study. J Periodontol. 2009;80:1388–1392.
- Linkevicius T, Puisys A, Vindasiute E. Does residual cement around implant-supported restorations cause peri-implant disease? A retrospective case analysis. Clin Oral Implants Res. 2013;24:1179–1184.
- Kotsakis GA, Zhang L, Gaillard P, et al: Investigation of the association between cement retention and prevalent peri-implant diseases: a cross-sectional study. J Periodontol. 2016;87:212–220.
- Dalago HR, Schuldt Filho G, Rodrigues MAP, et al. Risk indicators for peri-implantitis. A cross-sectional study with 916 implants. Clin Oral Implants Res. 2017;28:144–150.
- American Academy of Periodontology. Glossary of Periodontal Terms. Available at: https://members.perio.org/libraries/glossary?ssopc=1. Accessed December 8, 2021.
- Sorní-Bröker M, Peñarrocha-Diago M, Peñarrocha-Diago M. Factors that influence the position of the peri-implant soft tissues: a review. Med Oral Patol Oral Cir Bucal. 2009;14:475–479.
- Thakur R, Gaur V, Yadav B, Venkitram NJ. Biology of peri implant tissues: A review. IOSR J Dent Med Sci. 2020;19:18–24.
- Lang NP, Wilson TG, Corbet EF. Biological complications with dental implants: their prevention, diagnosis and treatment. Clin Oral Implants Res. 2000;11(Suppl 1):146–155.
- van Winkelhoff AJ, Goené RJ, Benschop C, Folmer T. Early colonization of dental implants by putative periodontal pathogens in partially edentulous patients. Clin Oral Implants Res. 2000;11:511–520.
- Luchinskaya D, Du R, Owens DM, Tarnow D, Bittner N. Various surface treatments to implant provisional restorations and their effect on epithelial cell adhesion: A comparative in vitro study. Implant Dent. 2017;26:12–23.
- Stoeva I, Kisselova A, Zekova M. Allergic contact stomatitis from bisphenol-A-glycidyldimethacrylate during application of composite restorations. A case report. J IMAB-Ann Proc. 2008;Book 2:45–46.
- Johns DA, HemaraJ S, Varoli RK. Allergic contact stomatitis from bisphenol-A-glycidyl dimethacrylate during application of composite restorations: A case report. Indian J Dent Res. 2014;25:266–268.
- Syed M, Chopra R, Sachdev V. Allergic reactions to dental materials — a systematic review. J Clin Diagn Res. 2015;9:ZE04–ZE09.
- Engler MLPD, Güth J-F, Keul C, Erdelt K, Edelhoff D, Liebermann A. Residual monomer elution from different conventional and CAD/CAM dental polymers during artificial aging. Clin Oral Invest. 2020;24:277–284.
- Atay A, Gürdal I, BozokÇetıntas V, Üs ̧ümez A, Cal E. Effects of new generational l-ceramic and provisional materials on fibroblast cells. J. Prosthodont. 2019;28:e383–e394.
- Shim JS, Kim HC, Park SI, Yun HJ, Ryu JJ. Comparison of various implant provisional resin materials for cytotoxicity and attachment to human gingival fibroblasts. Int J Oral Maxillofac Implants. 2019;34:390–396.
- Carmagnola D, Abati S, Celestino S, Chiapasco M, Bosshardt D, Lang NP. Oral implants placed in bone defects treated with Bio-Oss, Ostim-Paste or PerioGlas: an experimental study in the rabbit tibiae. Clin Oral Implants Res. 2008;19:1246–1253.
From Decisions in Dentistry. January 2022;8(1):14,16-18.


