Wealth Equates With Oral Health for Seniors, Too
For a decade and a half, the annual A State of Decay report from Oral Health America, a Chicago-based nonprofit health advocacy group, has ranked states based on their quality of dental care for older adults.
For a decade and a half, the annual A State of Decay report1 from Oral Health America, a Chicago-based nonprofit health advocacy group, has ranked states based on their quality of dental care for older adults. This year’s report includes U.S. Centers for Disease Control and Prevention data that examine the impact of sociodemographic factors — such as income, education, race and gender — on the oral health of Americans age 65 and older.
As the chart shows, there is a strong association between higher incomes and two markers of oral health: number of dental visits in the past year, and less severe tooth loss. This is not surprising considering that National Health Interview Survey data show dental treatment is the No. 1 health care service people report going without due to cost.2
Being married, female and more educated also correlates with being more likely to having seen a dentist in the past year, and lower odds of severe tooth loss among adults age 65 and older.1 However, there was one surprise in the data: Adults age 70 to 74 had slightly better dental health markers (more dental visits, less tooth loss) than those between 65 and 69. One might expect oral health to decline with age, not improve.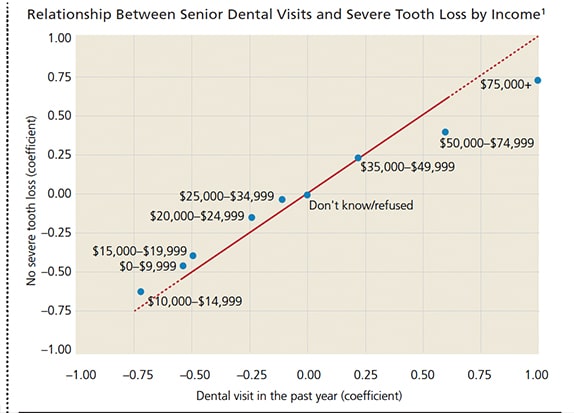
Further research is needed to explain why individuals in their early 70s might be better at taking care of their teeth than those in the their late 60s, but one frightening possibility is that some older adults with the worst oral health may not be making it into their 70s to be counted. Their early deaths could be the reason the remaining group’s dental health markers are better.
There is some evidence for this. A 2016 study in the Journal of the American Medical Association found that men in the lowest income group lived, on average, roughly 10 years less than men in the richest group — and that this gap was widening.3 Furthermore, Health and Human Services researchers report that when older adults have tooth loss, caries and periodontal disease combined, their risk of dying prematurely rises sharply.4 The researchers suggest the “association of multiple oral health conditions with mortality may be greater than the sum of the individual conditions,” and explain, “when an individual had all three oral health conditions, the mortality curve dramatically increased as he/she aged, whereas the mortality curve increased more slowly for those with no oral health issues.”4
As the national political discussion shifts to deficit reduction through entitlement reform, dentistry could be a powerful voice advocating for protection of income for the nation’s seniors and addressing disparities in access to care between rich and poor.
REFERENCES
- Oral Health America. A State of Decay, Vol. IV. Available at: https://oralhealthamerica.org/astateofdecay/. Accessed October 18, 2018.
- Peterson-Kaiser Health System Tracker. How does cost affect access to care? Available at: healthsystemtracker.org/chart-collection/cost-affect-access-care/. Accessed October 18, 2018.
- Chetty R, Stepner M, Abraham S, et al. The association between income and life expectancy in the United States, 2001–2014. JAMA. 2016;315:1750–1766.
- Kim JK, Baker LA, Davarian S, Crimmins E. Oral health problems and mortality. J Dent Sci. 2013;8:115–120.
From Decisions in Dentistry. November 2018;4(11):46.


