
Standards in Contemporary Endodontics
An exploration of the current standard of practice in endodontic treatment, with insights into appropriate — and possibly collaborative — multidisciplinary care.
As we approach the third decade of our advancing millennium, one of the realities of American dentistry is the expanding shift in the delivery of patient care. The private practice model is shrinking and giving way to corporate and group models that promote interdisciplinary treatment planning. This shift promises competence, reliability and cost control, which are all demanded by the corporate and industry structures that deliver the care.1
As dental schools graduate novice practitioners who are trained in a generalist model of care, many young practitioners will seek opportunities within group practices that provide patient services involving more and more complex endodontic procedures under an interdisciplinary umbrella. Thus, it is increasingly important for the generalist and specialist to participate in concerted patient management, with the overriding values of quality care and patient safety at its core.2
A sustainable practice model that promotes high-quality, collaborative treatment has been a hallmark of American dentistry for decades, and newer practice models must maintain this standard in order to provide value for patients, as well as effectively manage the complex dental problems that will invariably arise. The practice of endodontics has concurrently experienced a shift in the delivery of services and the advancement of scientific discovery within the field. Emerging technologies in instruments, magnification and imaging aimed at treating and salvaging the natural dentition with consistent outcomes have helped advance today’s standards of contemporary endodontic practice.
QUALITY CARE
The movement towards evidence-based health care in medicine and dentistry has been gaining ground quickly over the past few decades. It has been fueled by clinicians, politicians, management and the public, all of whom are concerned about quality, consistency and costs. It has facilitated the development of guidelines for the delivery of care,3 which are defined in order to:
- Describe appropriate care based on the best available scientific evidence and consensus
- Reduce inappropriate variation in practice
- Provide a more rational basis for referral to specialists
- Provide a focus for continuing education
- Promote efficient use of resources
- Act as a focus for quality control
When we speak about standards in contemporary endodontic practice, there is often a misunderstanding of the terms used to describe these standards. This discussion is intended to help clarify these terms.
Standard of Practice: This is defined as the acceptable level of performance or an expectation for professional intervention, formulated by professional organizations based upon current scientific knowledge and clinical expertise. When improved technology offers clearly superior results, it no longer becomes an issue of doctor/patient choice, but, rather, a requirement to fulfill the standard of practice. The use of microscopy for apical surgery with ultrasonic tips for retrofilling4–6 exemplifies improved technology and the current standard of practice in endodontics. Likewise, apical retrograde restorations should be performed with biocompatible materials, such as mineral trioxide aggregate, not with amalgam.7
Standard of Care: There is no medical definition for standard of care, although the term is firmly established in law. In tort law, the standard of care is defined as “the caution and prudence that a reasonable person under a duty of care, in similar circumstances, would exercise in providing care to a patient.” Peer review and the courts recognize only one standard of practice in endodontics — and that standard is determined by the endodontist.
Best Practice: This is defined as the recognized level of care provided by competent practitioners trained in that area of specialization. Endodontics is recognized by the American Dental Association as a dental specialty. The American Board of Endodontics is the recognized certification board of the specialty. The American Association of Endodontists (AAE) has developed and provided the profession and public with information and education about endodontic best practices. Best practice is a dynamic model that progressively changes and improves, and is continually redefined by scientific discovery, patient outcomes and the organized specialty.
In understanding these definitions, we quickly see that the courts determine the standards of care and the profession determines the standards for practice. This article will focus on the standards of practice, and best practices in contemporary endodontics.
CASE ASSESSMENT
The AAE’s Endodontic Case Difficulty Assessment Form and Guidelines8 provide a roadmap for when a general dentist should treat or refer to an endodontist. The case assessment document specifically states that “technology, instruments and materials are not a replacement for clinical skill and experience, but rather adjuncts that a practitioner can employ to reach a desired goal.” The Endodontic Case Difficulty Assessment Form is intended to assist practitioners with treatment planning, but can also be used to help with referral decisions and record keeping. The assessment form identifies three categories that may affect treatment complexity: patient considerations, diagnostic and treatment considerations, and additional considerations. Within each category, levels of difficulty are assigned, based upon potential risk factors. The levels of difficulty are sets of conditions that may not be controllable by the dentist. They range from minimal to high difficulty. The form and supporting information are available at aae.org/caseassessment.
General practitioners trained to render endodontic care are competent to treat minimal-difficulty cases. Experienced general dentists may treat the cases of moderate difficulty, but should always consider referring high-difficulty patients to endodontic specialists. As with any procedure, it is important for each clinician to recognize the limits of his or her skill and expertise in order to protect patients and provide quality care. Patient considerations that may complicate treatment include medical complications, difficulties with anesthesia, behavioral management issues, limited opening, and treatment complications. Additional considerations include previous endodontic treatment, a history of trauma, and periodontal/endodontic conditions.8
Because endodontists set the standard of practice for conventional endodontics, if the endodontist’s standard cannot be met — such as the use of microscopy, regenerative procedures, and three-dimensional (3D) imaging for complex anatomy, or the need for apical surgery — the generalist should seriously consider referring the patient to an endodontist.9 As clinicians, we can ensure the highest-quality care by planning treatment in such a way that we accurately assess the difficulty of the case, as well as our personal skill levels and formal training. This will help practitioners determine whether to treat or refer.
TREATMENT RECORDS
Endodontic Records and Clinician Responsibilities: Good clinicians keep good records. Documenting endodontic treatment serves as an important record which, together with objective data, helps guide clinicians to the correct diagnostic and treatment paths. Documentation is essential to decision-making. The dental record must contain sufficient information to identify the patient, support the diagnosis, justify the treatment, and document the course and result of treatment.
Records are designed to protect the patient’s welfare, and are also a fundamental means of communication among health care professionals. A thorough and complete record should contain:
- A thorough review of the patient’s medical and dental history
- Chief complaint(s), including onset, duration, frequency, type and intensity of any pain
- Diagnostic-quality radiographs
- Pulpal and periodontal diagnostic test results
- Objective clinical examination findings
- Differential diagnoses and final diagnosis
- The treatment plan and prognosis
- Documentation of the course of treatment
These are essential components of a quality record that will support the doctor/patient interaction. When other factors affect the prognosis of any tooth diagnosed for endodontic treatment — such as the tooth’s strategic value, restorability or proximity to vital structures — the clinician should consider consulting with an endodontist or other specialist (including a prosthodontist, periodontist or radiologist with 3D imaging),10 before initiating endodontic treatment.
Informed Consent: After an endodontic diagnosis is made, the benefits, risks, treatment plan, and alternatives to endodontic treatment should be presented to the patient or the patient’s guardian or caretaker. This includes any patient refusal of recommended treatment and the consequences of refused treatment. This will document acceptance or rejection of treatment recommendations. The patient or guardian/caretaker, along with a witness (who can be a staff member), should sign and date the consent form.11
An endodontic chart will help document information pertinent to the diagnosis, recommendations and treatment of the patient. Systematic acquisition and arrangement of data from the patient questionnaire, along with clinical and radiographic examinations, and careful logging of all treatment, will aid accurate diagnosis and maximize clinical efficiency.11
USE OF DENTAL DAMS
An example of a violation of the standard of practice includes any dentist who does not use dental dams for all root canal treatments. The 2010 AAE Position Statement on Dental Dams mandates that “tooth isolation using the dental dam is … integral and essential for any nonsurgical endodontic treatment.” The dental dam offers additional benefits, such as aiding visualization by providing a clean operating field, and preventing ingestion or aspiration of dental materials, irrigants and instruments.12
key takeaways
- In today’s practice, it is increasingly important for the general dentist and specialist to participate in concerted patient management, with the overriding goals of quality care and patient safety.2
- Innovations in instruments, magnification and imaging have helped advance the standards of contemporary endodontic practice.
- When improved technology offers clearly superior results, it no longer becomes an issue of doctor/patient choice, but, rather, a requirement to fulfill the standard of practice.
- The American Association of Endodontists’ (AAE) Endodontic Case Difficulty Assessment Form and Guidelines8 provide a roadmap for when a general dentist should refer to an endodontist.
- The AAE form is intended to assist practitioners with endodontic treatment planning, but can also be used to help with referral decisions and record keeping.
- The modern approach to periradicular surgery involves magnification, illumination and microsurgery, as prognoses are greatly improved when these techniques are used.16
ANATOMICAL COMPLEXITY
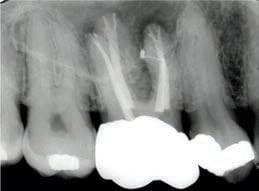
COURTESY SHERRY BLOOMFIELD, DDS
The morphology of root canal systems is complex and contains many inaccessible areas, such as apical canal ramifications, isthmus areas and canal wall irregularities13 (Figure 1), where pathogens may be present in the form of biofilm.14 In some cases, root canals can be highly mineralized to the extent they are extremely difficult to negotiate in a traditional manner. In addition, conventional radiographs taken in a bucco-lingual direction reveal only part of the intricate root canal system. Overlying anatomical structures, such as the zygomatic arch, maxillary sinuses, mylohyoid ridge or tori, can make detection of additional canals or roots difficult. All of these potential circumstances, as well as other case assessment issues, require the clinician to ask, “Do I possess the technical skills, training and equipment to deliver quality care in this case?”
MAGNIFICATION
A 2007 survey of 1091 endodontists indicated that 90% of respondents had access to, and used, the operating microscope in their practice, a dramatic increase from the 52% affirmative response in 1999.15 The 2012 AAE Position Statement on the Use of Microscopes and Other Magnification Techniques asserts that the microscope is integral to modern endodontic techniques. The position statement describes procedures that benefit from the use of the microscope,15 including:
- Locating canals obstructed by mineralization and/or reduced in size
- Removing materials, such as solid obturation materials (e.g., silver points and carrier-based materials), posts or separated files
- Removing canal obstructions
- Assisting in access preparation to avoid unnecessary destruction of structural dentin (Figure 2)
- Repairing perforations
- Locating cracks and fractures that are not clinically visible or palpable with an endodontic explorer
- Facilitating all aspects of endodontic surgery, particularly in root-end resection and placement of retrofilling materials
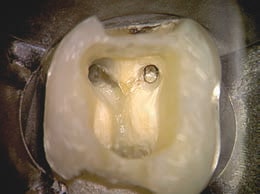
COURTESY CLIFFORD RUDDLE, DDS
In addition, the microscope allows enhanced photographic documentation and improves ergonomics for the clinician.
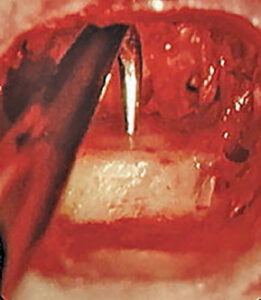
The modern approach to periradicular surgery involves magnification, illumination and microsurgery, as it is documented that prognoses are greatly improved when these techniques are employed.16 When compared with microscopes, the use of loupes or similar devices that are adequate for coronal restorative procedures may prove inadequate for apical surgery, or even conventional coronal endodontics. Microscopy provides a more detailed examination of the root apex and anatomic features, such as isthmuses, unfound and accessory canals, fractures and crazing (Figure 3).
TWO-DIMENSIONAL AND THREE-DIMENSIONAL IMAGING
Preoperative radiographs are an indispensable part of diagnostic procedures in root canal treatment. A simple bitewing radiograph will always give the most accurate two-dimensional (2D) projection of the pulp chamber and its depth. Recognition and diagnosis of periapical disease on conventional radiographs can be a challenge, however. Well-angulated periapical films should be taken with the cone directed straight-on, mesio-oblique and disto-oblique. This technique oftentimes reveals and clarifies the three-dimensional morphology of the tooth, and helps identify anatomic complexities. Digital radiography and other imaging technologies provide enhanced software features that significantly aid radiographic diagnostics and identification of anatomical complexities. The clarity, color, contrast and brightness of a digital image can be easily modified to assist clinicians in locating hidden, mineralized or untreated canals.

When a radiographic examination is performed or required, the practitioner assumes the responsibility to make accurate interpretations from discernable, diagnostic-quality images. It is a common understanding that both large and small pathoses, as well as anatomic entities, are routinely missed in 2D radiographic surveys — both by the operator and the limitations of the technology when encountering differences in anatomic variation.17 By comparison, 3D cone beam computed tomography (CBCT) can image periapical lesions and other anatomical structures in the axial (transverse), coronal (anterior-posterior) and sagittal (left-right) sections. The scanning devices responsible for these limited-field 3D images have greatly advanced our understanding of the anatomic complexities in a given case, and help reveal presurgical intricacies, and unseen pathoses and canal complications (Figure 4).
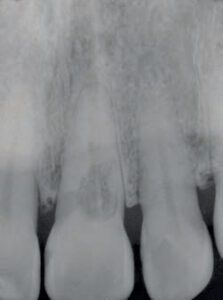
When such utilization is indicated, the field of view can be limited to several teeth, and the resulting CBCT scans can produce images with excellent contrast and clarity, while emitting relatively low radiation exposure.10,18
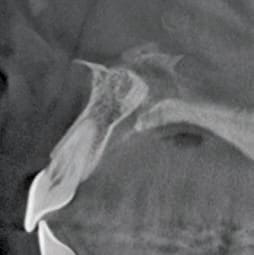
In instances of complex diagnosis, such as internal or external resorption (Figures 5A and 5B), a 3D image accurately defines the type and extent of disease. This information is critical in forming a predictable treatment plan and prognosis. Assessment of periradicular lesions in multirooted teeth, and differentiating these lesions from nonodontogenic pathoses, is greatly facilitated by the use of focused field CBCT. In addition, 3D imaging yields crucial information regarding the size and proximity of a lesion to vital structures. Besides revealing spatial relationships of root apices to anatomical structures, 3D imaging can detect accessory canals, the location of root canals, and canal obstructions. The healing and repair of pathoses after nonsurgical and surgical endodontics can be observed in a far more predictable manner with 3D technology.17
CONCLUSION
A reasonable and prudent clinician must keep current with advances that, on the basis of research and evidence, are generally accepted and embraced by endodontists. It is incumbent upon the practitioner to adopt technologies that improve the quality of endodontic care and meet currently accepted standards. Microsurgical techniques are an example of improved endodontic technology, as is CBCT imaging. Using 3D images, clinicians can accurately locate the mandibular nerve, and note the position of the mental foramen, and the relationship of the maxillary sinus to adjacent root structures. This type of imaging helps clinicians protect patients when anatomic proximity of these structures presents reasonable risk.
As endodontics evolves through science and technology, clinicians must understand how these advances will impact their own patient care. Dental professionals deservedly earn patient trust and respect by providing safe and effective care that meets the highest standards of practice.
A version of this article originally appeared in ENDODONTICS: Colleagues for Excellence, Fall 2014. Reused with permission from the American Association of Endodontists, ©2014. The AAE clinical newsletter is available at aae.org/colleagues.
REFERENCES
- Kao RT. Dentistry at the crossroads. J Calif Dent Assoc. 2014;42:91–95.
- Cooper MB. The perfect storm. J Calif Dent Assoc. 2014;42:97–100.
- Field MJ, Lohr KN. eds. Guidelines for Clinical Practice: From Development to Use. Institute of Medicine, Washington, D.C: National Academy Press, 1992.
- Kersten DD, Mines P, Sweet M. Use of the microscope in endodontics: results of a questionnaire. J Endod. 2008;34:804–807.
- Creasy JE, Mines P, Sweet M. Surgical trends among endodontists: the results of a web-based survey. J Endod. 2009;35:30–34.
- Tsesis I, Rosen E, Taschieri S, Telishevsky Strauss Y, Ceresoli V, Del Fabbro M. Outcomes of surgical endodontic treatment performed by a modern technique: an updated meta-analysis of the literature. J Endod. 2013;39:332–339.
- Parirokh M, Torabinejad M. Mineral trioxide aggregate: A comprehensive literature review — Part III: clinical applications, drawbacks, and mechanism of action. J Endod. 2010;36:400–413.
- Law AS, Withrow JC. Endodontic Case Difficulty Assessment and Referral. ENDODONTICS: Colleagues for Excellence. Spring/Summer 2005. Available at: https://www.aae.org/publications-and-research/endodontics-colleagues-for-excellence-newsletter/endodontic-case-difficulty-assessment-and-referral.aspx. Accessed April 27, 2016.
- Goldman RP. Your duty to refer. ADA Legal Adviser. 1998;2:6–7.
- Cotton TP, Geisler TM, Holden DT, Schwartz SA, Schindler WG. Endodontic applications of cone-beam volumetric tomography. J Endod. 2007;33:1121–1132.
- Zinman EJ. Endodontic records and legal responsibilities. In: Hargreaves KM, Cohen S. eds. Pathways of the Pulp. 10th ed. 2011; St. Louis; Mosby Elsevier;389–450.
- Dental Dams. Position Statement of the American Association of Endodontists 2010. Available at: https://www.aae.org/uploadedfiles/publications_and_research/guidelines_and_position_statements/dentaldamstatement.pdf. Accessed April 27, 2016.
- Vertucci FJ. Root canal morphology and its relationship to endodontic procedures. Endod Topics. 2005;10:3–29.
- Svensäter G, Bergenholtz, G. Biofilms in endodontic infections. Endod Topics. 2004;9:27–36.
- Use of Microscopes and Other Magnification Techniques. Position Statement of the American Association of Endodontists 2012. Available at: https://www.aae.org/uploadedfiles/publications_and_research/guidelines_and_position_statements/microscopesstatement.pdf. Accessed April 27, 2016.
- Tsesis I, Rosen E, Schwartz-Arad D. Retrospective evaluation of surgical endodontic treatment: traditional versus modern technique. J Endo. 2006;32:412–416.
- De Paula-Silva FWG, Wu M-K, Leonardo MR, Bezerra da Silva LA, Wesselink, PR. Accuracy of periapical radiography and cone beam computed-tomography scans in diagnosing apical periodontitis using histopathological findings as a gold standard. J Endod. 2009;35:1009–1012.
- Peters CI, Peters OA. Cone beam computed-tomography and other imaging techniques in the determination of periapical healing. Endod Topics. 2013;29:57–75.


