 DRAZEN_/E+/GETTY IMAGES PLUS
DRAZEN_/E+/GETTY IMAGES PLUS
Principles of Endodontic Diagnosis
Proper examination and testing will lead to an accurate endodontic diagnosis, allowing clinicians to deliver appropriate treatment.
Proper and accurate diagnosis is paramount for successful treatment in medicine and dentistry. In endodontics, an accurate diagnosis is imperative to identify the offending tooth that is causing the patient’s symptoms and/or disease. Furthermore, the type of diagnosis can affect the success rate. Endodontic cases diagnosed with pulpal necrosis and an associated periapical radiolucency have roughly a 10% decreased success rate compared to cases of pulpitis or necrotic cases that do not yet have a periapical radiolucency.1–3
A thorough medical and dental history should be taken before examining the patient. The patient’s chief complaint, if there is one, should also be documented. When performed on the offending tooth, the objective tests discussed in this article should replicate the patient’s chief complaint. Extraoral and intraoral examinations, along with periodontal and radiographic assessments, are also part of the overall diagnostic process. This article will focus on the objective pulpal sensibility and periapical tests.
While myriad pulpal and periapical diagnoses exist for cases, they can generally be separated into three broad categories: the pulp tissue is either normal, inflamed or infected. Even though these broad categories exist, endodontic disease is a progression of a single disease — one that progresses in a coronal to apical direction over time. Depending on when a patient seeks treatment along this timeline, there will be a specific set of diagnoses. If no treatment is performed, the pulp will move from an inflamed to a necrotic state.4
Endodontic testing is divided into two main components, pulp sensibility and periapical tests. Pulp tests involve methods used to determine the vitality of the pulp; ideally, this would be accomplished by detecting a vascular supply to the pulp. While some methods are able to accomplish this (such as pulse oximetry or laser doppler flowmetry), their use is neither widespread nor practical in dentistry. Traditional pulp tests assess the neural response of the pulp, either directly or indirectly. These tests include electric, cold and heat tests. Each has their strengths, weaknesses and common errors.5,6
It is prudent to first test a control tooth, or teeth, and the suspect tooth last. This allows the patient and clinician to understand what a normal response is, so when the offending tooth is tested, an abnormal response can be differentiated from a normal response or lack of response.
ELECTRIC PULP TESTING
The electric test is performed with an electric pulp tester (EPT). This monopolar device flows high-frequency electrical current from the probe tip through the tooth. While the current is flowing through the tooth, viable A-delta nociceptive fibers will be stimulated, resulting in a tingling or “zinging” sensation to the patient.
Performing the electric test accurately requires a well-dried and isolated tooth. It is recommended to dry the tooth with gauze and place a cotton roll in the vestibule to isolate. One should not dry the tooth with an air syringe because if the tooth is very sensitive, as in cases of pulpitis, it will cause the patient unnecessary pain. The probe tip is coated with a contact medium, such as petroleum jelly, topical anesthetic or toothpaste.7 According to Bender et al,8 the optimal placement of the tip is on the incisal third for anterior teeth. However, placement of the tip on sound tooth structure anywhere on the clinical crown will yield an accurate result (Figure 1).
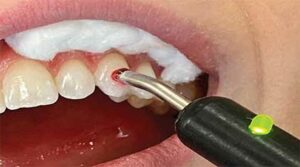
Depending on the EPT used to complete the electrical circuit, a lip clip is placed on the patient, or the patient will holds the metal handle. The latter has the benefit of having the patient in charge of the test by letting go of the handle if a sensation is felt. This will lessen any potential anxiety.9 If a full coverage restoration is present, a bridging technique can be utilized. A fine tip of an explorer or file can be used to contact tooth structure cervical to the crown margin, and the EPT probe tip contacts the instrument (Figure 2).10 Alternatively, a micro-EPT that is thin (like an explorer tip) can also be used.
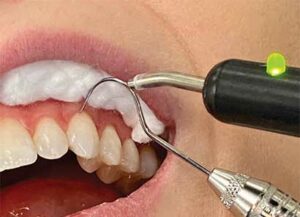
A positive response (meaning the patient felt a sensation) indicates vital pulp tissue, more specifically, viable A-delta fibers. It should be noted this does not indicate pulpal health. A negative response or lack of response indicates necrosis of the pulp (assuming the proper contact was made). The number of the reading is usually of little significance and the test result should be recorded as present or absent. However, a positive response at a high reading that is close to the maximum range of the unit is usually a false positive result.
Errors in the EPT that yield false positive or negative results can occur. The most common error for a false positive is inadequate tooth isolation. Dry tooth structure that is free from saliva is imperative for an accurate and reliable reading. Contact with metal restorations and gingival tissue should also be avoided. A false negative result can occur if the canals are extremely calcified, the teeth have been recently traumatized, and in teeth with immature apices.11,12 The reason for the latter is that A-delta fibers take five years from eruption to fully develop and grow in number.13
COLD TESTING
The cold test is one of the two thermal tests. It is now most commonly performed using a refrigerant spray. Historically, ethyl chloride, dichlorodifluoromethane (i.e., Freon), CO2 snow, and ice have also been used. The cold test indirectly stimulates viable A-delta fibers14 by movement of dentinal tubule fluid according to hydrodynamic theory.15 The cold temperature causes contraction, or an outward movement, of the dentinal tubule fluid, resulting in negative pressure. This movement physically affects the odontoblastic processes of odontoblasts that stimulate the A-delta fibers. This is termed mechanotransduction. The results of the cold test not only indicate pulpal vitality, but also the pulp’s condition.
Properly performing the cold test also involves isolating the tooth. While isolation is not as critical as with the electric test, saliva should be wiped away, as this can increase the temperature of the refrigerant spray and may lead to a false negative response. The patient should be instructed to alert the clinician (by raising a hand, for example) only if a sensation is felt. A control tooth should be tested first so the patient knows what a normal sensation feels like. A small cotton pellet on forceps should be generously saturated and applied to the tooth (Figure 3). Compared to a cotton pellet, a cotton swab has less surface area; therefore, it does not adequately transfer cold and should not be used. The intensity and duration of the response should be recorded. Bear in mind that whatever the response was for the control tooth (even if exaggerated), it is considered normal for that patient.
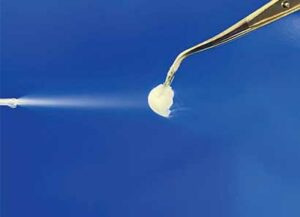
refrigerant spray. Cotton pellets have more surface
area to retain the spray than cotton swabs.
The response of the suspect tooth is compared to the control tooth to determine the intensity (normal, moderate or severe) and duration (lingering or not). Also keep in mind that thermal tests can be completed on teeth with full-coverage restorations.16,17 While metal restorations are conductive and porcelain restorations are insulative, thermal tests can be attempted on both. A positive response indicates vitality. A negative response does not necessarily indicate pulpal necrosis and could be a false negative.
While the cold test is considered an accurate test,18–20 false results can still occur — the most common being a false negative on a tooth that has a calcified or receded pulp chamber. This can occur in heavily restored teeth or as patients age.21 In cases of the latter, the patient would most likely not feel a sensation on the control tooth, as well. The radiographs can be observed to evaluate the size and position of the pulp chamber to see if a negative response would be expected.
Other reasons for a false negative include an immature apex and recent trauma (for the same reasons as stated previously). A false positive is much less common, but can result from an overly anxious patient. This again is why it is imperative to test a control tooth first to set expectations. Also, in a tooth with an inflamed periodontal ligament, an intense sensation could be felt just by touching the tooth with a cotton pellet, not because it is cold. This can be ruled out by touching the tooth with a cotton pellet before spraying the pellet. Finally, ensure the cotton pellet is small enough that it does not contact more than one tooth.
HEAT TESTING
The other thermal test is the heat test, which is not routinely performed. Like the cold test, the heat test indirectly stimulates viable A-delta fibers14 by movement of dentinal tubule fluid via hydrodynamic theory.22,23 Unlike the cold test, the heat test causes expansion, or an inward movement, of the dentinal tubule fluid, resulting in positive pressure and a similar mechanotransduction phenomenon. Compared to the cold test, the nerve response, and thus the patient response, is much lower. As demonstrated by Vongsavan and Matthews,24 the negative pressure created by the cold test results in significantly more nerve impulses than the positive pressure created the heat test. One thing the heat test offers that cold testing does not is that it can also activate C fibers,25 which is why some regard the heat test as the ultimate test.
There are a few ways to perform the heat test. An easy method is to use a dry prophy cup on the tooth, with the friction creating heat on the tooth. Another way is to isolate an individual tooth with a rubber dam and bathe the tooth with warm water. The most common way is to heat gutta-percha and apply it to the tooth. White gutta-percha stopping sticks can be heated and applied to the tooth (Figure 4). A light coat of petroleum jelly should be applied to the tooth to avoid gutta-percha adhering to dentition. Heat tests can also be done with heating devices used in the warm vertical compaction method of obturation. Special tips and settings are used to perform the heat test in this manner. Like the cold test, intensity and duration should be recorded. The reasons for false negative and false positive results with the heat test are similar to the cold test, with a calcified or receded pulp chamber being the most common reason for a false negative.
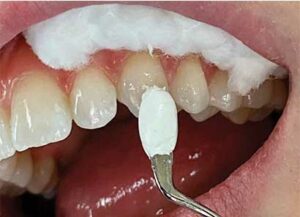
to a metal instrument used for a heat test;
care must be taken not to burn soft tissue.
VARYING SENSITIVITIES
All three of these pulpal sensibility tests have varying sensitivities, specificities and accuracies. Studies show cold testing is most accurate (ranging from 84% to 86%),19,20 followed closely by the electric test (81% to 82%), with the heat test being the least accurate (70%). Clinicians should be cognizant that even though cold testing is considered most accurate, if the pulp chambers of the teeth being tested appear calcified radiographically, a negative result in itself does not necessarily indicate pulpal necrosis. Two tests should be performed to confirm pulpal necrosis.
PERIAPICAL TESTING
The periapical tests include percussion and palpation. Although these tests do not provide information about the pulp, such as vitality or necrosis, they indicate whether there is inflammation in the periapical tissues. The percussion test is accurate in identifying and localizing the offending tooth. However, this can only be achieved if the disease has progressed apically to affect the periodontal ligament. The pulp lacks proprioceptors which are needed to localize pain. Therefore, early in the endodontic disease process, patients have a difficult time localizing the source of pain. The periodontal ligament has proprioceptors, the A-beta fibers, which, when activated via percussion or mastication, transmit a signal to the mesencephalic nucleus in the central nervous system. There, a synapse occurs with a second order neuron that crosses to the contralateral side to reach the thalamus and cerebral cortex for interpretation and localization.
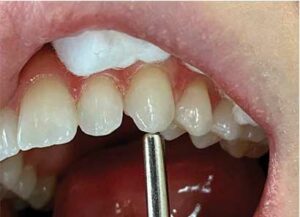
tapping gently along the long-axis of the
tooth with a blunt instrument.
The percussion test can be performed by tapping gently on the incisal or occlusal surface of teeth with a gloved finger, or, more commonly, the blunt end of an instrument, such as a mirror handle (Figure 5). Only gentle force is needed and the patient should be instructed beforehand to inform the dentist of any sensitivity or differences between the control teeth and tooth or teeth in question. A positive response (i.e., pain) does not in itself indicate endodontic disease. Trauma, such as concussive injuries (primary occlusal trauma), and periodontal disease can result in percussion sensitivity. Percussion testing should be performed vertically with the long axis, as well as horizontally. If the patient has more sensitivity to horizontal percussion than vertical, and in the absence of other signs or symptoms that would indicate endodontic disease, the issue may be periodontal in origin.26
Clinicians use palpation to test for periapical inflammation or infection. A gloved index finger and firm digital pressure is applied to the mucosa overlying the root apices from the facial/buccal and lingual aspects (Figure 6). A positive response can be sensitivity, swelling, bony expansion, or a break in the cortical plate. The contralateral side should also be palpated for comparison.
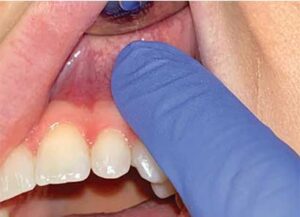
finger to check for sensitivity, swelling,
expansion, or a break in the cortical plate.
CONCLUSION
These diagnostic objective tests, along with the patient’s subjective symptoms, will lead to a pulpal and apical diagnosis. While not described in this article, the current endodontic diagnostic terms historically have not correlated with the histopathologic condition of the pulp.27,28 However, a more recent study has shown that when defined criteria are used, there can be a strong correlation.29
In closing, proper examination and testing will lead to an accurate diagnosis, resulting in appropriate treatment to alleviate a patient’s symptoms and disease.
KEY TAKEAWAYS
- A proper endodontic diagnosis is imperative to identify the offending tooth that is causing the patient’s symptoms and/or disease.
- Extraoral and intraoral examinations, along with periodontal and radiographic assessments, are key steps in the overall diagnostic process.
- When performed on the offending tooth, the objective tests discussed in this article should replicate the patient’s chief complaint.
- Endodontic testing is divided into two main components, pulp sensibility and periapical tests.
- Pulp tests, such as electric pulp testing and thermal tests, involve methods used to determine the vitality of the pulp.
- Periapical tests include percussion and palpation. While these tests do not provide information about the pulp, they indicate whether there is inflammation in the periapical tissues.
- These diagnostic, objective tests, along with the patient’s subjective symptoms, will lead to an accurate pulpal and apical diagnosis.
REFERENCES
- Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors affecting the long-term results of endodontic treatment. J Endodon. 1990;16:498–504.
- De Chevigny C, Dao TT, Basrani BR, et al. Treatment outcome in endodontics: the Toronto study — phase 4: initial treatment. J Endod. 2008;34:258–263.
- Ricucci D, Siqueira JF. Recurrent apical periodontitis and late endodontic treatment failure related to coronal leakage: a case report. J Endod. 2011;37:1171–1175.
- Walton RE, Garnick JJ. The histology of periapical inflammatory lesions in permanent molars in monkeys. J Endod. 1986;12:49–53.
- Jafarzadeh H, Abbott PV. Review of pulp sensibility tests. Part I: general information and thermal tests. Int Endod J. 2010;43:738–762.
- Jafarzadeh H, Abbott PV. Review of pulp sensibility tests. Part ΙΙ: electric pulp tests and test cavities. Int Endod J. 2010;43:945–958.
- Martin H, Ferris C, Mazzella W. An evaluation of media used in electric pulp testing. Oral Surg Oral Med Oral Pathol. 1969;27:374–378.
- Bender I, Landau M, Fonsecca S, Trowbridge H. The optimum placement-site of the electrode in electric pulp testing of the 12 anterior teeth. J Am Dent Assoc. 1989;118:305–310.
- Anderson RW, Pantera EA Jr. Influence of a barrier technique on electric pulp testing. J Endod. 1988;14:179–180.
- Pantera EA Jr, Anderson RW, Pantera CT. Use of dental instruments for bridging during electric pulp testing. J Endod. 1992;18:37–38.
- Fulling HJ, Andreasen JO. Influence of maturation status and tooth type of permanent teeth upon electrometric and thermal pulp testing. Scand J Dent Res. 1976;84:286–290.
- Fuss Z, Trowbridge H, Bender IB, Rickoff B, Sorin S. Assessment of reliability of electrical and thermal pulp testing agents. J Endod. 1986;12:301–305.
- Johnsen DC, Harshbarger J, Rymer HD. Quantitative assessment of neural development in human premolars. Anat Rec. 1983;205:421–429.
- Narhi M, Jyväsjärvi E, Virtanen A, Huopaniemi T, Ngassapa D, Hirvonen T. Role of intradental A- and C-type nerve fibres in dental pain mechanisms. Proc Finn Dent Soc. 1992;88(Suppl 1):507–516.
- Brannstrom M, Astrom A. The hydrodynamics of dentine: its possible relationship to dentinal pain. Int Dent J. 1972;22:219–227.
- Jones VR, Rivera EM, Walton RE. Comparison of carbon dioxide versus refrigerant spray to determine pulpal responsiveness. J Endod. 2002;28:531–533.
- Miller SO, Johnson JD, Allemang JD, Strother JM. Cold testing through full-coverage restorations. J Endod. 2004;30:695–700.
- Peters DD, Baumgartner JC, Lorton L. Adult pulpal diagnosis. I. Evaluation of the positive and negative responses to cold and electrical pulp tests. J Endod. 1994;20:506–511.
- Petersson K, Soderstrom C, Kiani-Anaraki M, Levy G. Evaluation of the ability of thermal and electrical tests to register pulp vitality. Endod Dent Traumatol. 1999;15:127–131.
- Mainkar A, Kim SG. Diagnostic accuracy of 5 dental pulp tests: a systematic review and meta-analysis. J Endod. 2018;44:694–702.
- Bernick S, Nedelman C. Effect of aging on the human pulp. J Endod. 1975;1:88–94.
- Brännström M, Åström A. A study on the mechanism of pain elicited from the dentin. J Dent Res. 1964;43:619–625.
- Brännström M. The hydrodynamic theory of dentinal pain: sensation in preparations, caries, and the dentinal crack syndrome. J Endod. 1986;12:453–457.
- Vongsavan N, Matthews B. The relationship between the discharge of intradental nerves and the rate of fluid flow through dentine in the cat. Arch Oral Biol. 2007;52:640–647.
- Narhi M, Yamamoto H, Ngassapa D, Hirvoven T. The neurophysiological basis and the role of inflammatory reactions in dentine hypersensitivity. Arch Oral Biol. 1994;Suppl:23s–30s.
- Pantera E. Diagnosing endodontic-periodontal disease. Periodontal Insights. 1994;1:5.
- Seltzer S, Bender IB, Ziontz M. The Interrelationship of pulp and periodontal disease. Oral Surg Oral Med Oral Pathol. 1963;16:1474–1490.
- Seltzer S, Bender IB, Ziontz M. The dynamics of pulp inflammation: correlations between diagnostic data and actual histologic findings in the pulp. Oral Surg Oral Med Oral Pathol 1963;16:969–977.
- Ricucci D, Loghin S, Siqueira JF Jr. Correlation between clinical and histologic pulp diagnoses. J Endod. 2014;40:1932–1939.
The authors have no commercial conflicts of interest to disclose
From Decisions in Dentistry. April 2020;6(4):9–10,12–13.


