 CASARSAGURU/E+/GETTY IMAGES PLUS
CASARSAGURU/E+/GETTY IMAGES PLUS
Prevention Over Prevalence: Importance of Interdental Cleaning
Informed clinicians can help tailor individualized, patient-specific recommendations for effective interdental cleaning.
This course was published in the August 2020 issue and expires August 2023. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Describe the prevalence of periodontal disease in the United States, and the basic structure of the American Academy of Periodontology’s (AAP) disease classification system.
- Explain various approaches to interdental cleaning, and how the AAP classifications can be used to develop patient-specific oral hygiene recommendations.
- Discuss clinical strategies to help improve the efficacy of patients’ self-care regimens.
Preventing and treating oral diseases is the focus of oral healthcare. Periodontal disease and caries, while largely preventable, are pervasive. In most cases, they can be prevented by controlling plaque biofilm via toothbrushing, interdental cleaning, and modifying lifestyle-based risk factors (such as smoking, metabolic control and dietary choices). These risk factors impact the host inflammatory response, and it is each patient’s individual response that contributes to periodontal health or tissue destruction.1 When prevention predominates, disease is less prevalent. Yet, it is apparent that prevention has not adequately impacted prevalence.
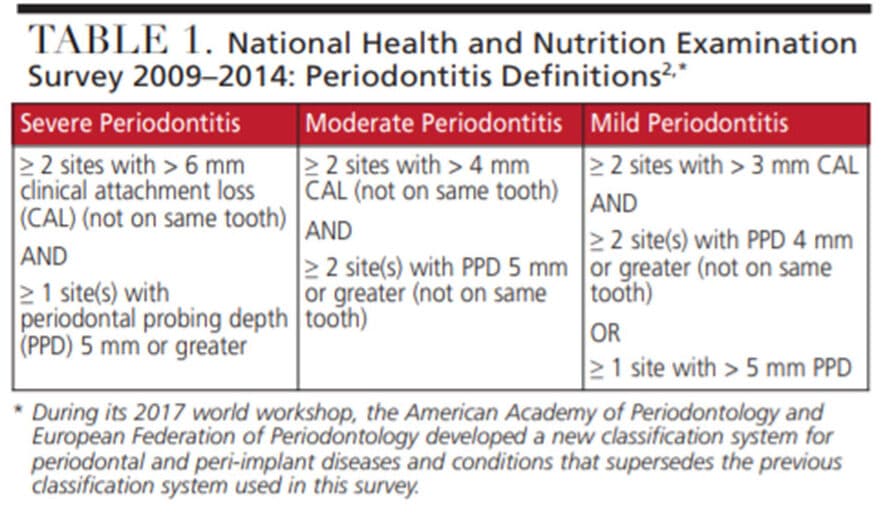
A large-scale study that collected comprehensive data regarding the prevalence of periodontal disease in the United States paints a discouraging scenario. Based upon clinical examinations conducted on more than 10,000 individuals, nearly half (42.2%) of adults over 30 had periodontitis.2 According to the disease classifications in use when the study was conducted, the disease was severe for 7.8% of that group, while it was mild or moderate for more than a third (34.4%) of the subjects.2 In this study, clinical attachment level (CAL) at each interproximal site was measured by calibrated clinicians for all teeth except third molars. Despite this rigorous approach, the researchers stated that disease prevalence figures may have been even higher if buccal and lingual CAL were also measured. However, these were not included due to the potential for zealous toothbrushing as the cause of recession at these sites. The severity of periodontal disease as defined for this study is seen in Table 1.
It is unlikely these prevalence results would surprise oral health professionals, as it is well established that plaque accumulation is requisite to the development of periodontal and peri-implant disease.3,4 Considering that daily oral hygiene takes five to six minutes (twice daily brushing for two minutes each time, and interproximal plaque removal taking one to two minutes), disease prevention is largely within reach for most patients — and clinicians can support periodontal health by providing education on effective brushing and interdental cleaning methods.
PERIODONTAL CLASSIFICATIONS
The periodontal disease classification system recently developed through a joint effort of the American Academy of Periodontology (AAP) and European Federation of Periodontology is based upon the amount of damaged or destroyed tissue.5 The current classification system uses four stages and three grades to describe disease status. The stages are based upon the severity (as determined by the loss of the interdental clinical attachment, radiographic loss of bone, and/or loss of teeth), complexity of management, and extent/distribution of disease (assessed as localized, generalized, or a molar/incisor pattern).
Practitioners can objectively identify when a patient’s disease process has a low rate of progression and the potential for arrest (Stage I and Grade A). Patients may be familiar with the process of staging and grading disease, as a similar system is used for classifying cancer severity and prognosis. Consequently, if patients know a stage and grade designation for their periodontal disease, it may help them understand the severity — potentially allowing education and prevention to gain traction.
Home-based plaque control suggestions can be personalized utilizing the patient’s specific stage and grade status, plus other factors, such as dexterity, patient preference and motivation. Toothbrushing with a dentifrice is nearly a universal practice.3 Conversely, daily interruption of biofilm from interproximal surfaces (usually by flossing) is not universal, and this practice has consistently shown low compliance.6
IMPORTANCE OF BIOFILM REMOVAL
Periodontal and peri-implant involvement has been described as microbially associated, host-mediated inflammation resulting in loss of attachment.5 With the interdental gingiva at the embrasure between teeth apical to the contact area, biofilm accumulates at these sites, matures, and increases the pathogenic potential of the bacterial load — thus favoring the development of periodontal disease. Daily interproximal biofilm disruption can reduce inflammation and disease, and consequently improve clinical outcomes.7–10
A randomized controlled trial to evaluate the effects of interproximal devices on oral disease cannot be conducted since it would be unethical to withhold interproximal cleaning from a study group. However, a recent cross-sectional investigation provided information in this regard. With nearly 7000 Americans over 30 years of age surveyed, regular interproximal cleaning (using dental floss or any other device) was found to be associated with less periodontal disease, decreased caries rates and fewer missing teeth. Moreover, interdental cleaning four to seven times per week was associated with less interproximal periodontal disease than in individuals who cleaned interdentally one to three times per week.11
DENTAL FLOSS
Effective and regular interproximal biofilm control is critical to disease prevention.10 In fact, interdental CAL is key to the periodontitis case definition and the first criterion in the grading category of the new classification system.5 Patients often associate interproximal oral hygiene with dental floss. When done properly, flossing takes minimal time, yet mastering the technique can elude some patients, leading to frustration and even abandonment of flossing. While some clinicians believe effective use of floss is generally tenable only for motivated patients, flossing is still the approach that receives the most attention and clinical recommendations.
Additionally, incorrect flossing can be detrimental, as both soft tissue clefts and bone loss have been associated with improper technique.12,13 Provider expectations of regular flossing can lead noncompliant patients to lie about compliance.14 Flossing can be efficacious when done correctly, which underscores the value of educating patients about proper technique. In fact, the benefits of flossing are best demonstrated in research designs where flossing is professionally supervised or performed by professionals.15 Studies in which subjects use interproximal devices themselves are more realistic, however, as research findings based on professional flossing protocols are not necessarily comparable to real-life scenarios.16
As noted, two challenges to flossing efficacy are improper technique and inconsistent use. The challenge of inconsistent use impacts a majority of patients, as evidenced by a study of more than 9000 individuals over 30 years of age which revealed that about one-third floss daily, one-third floss less than that, and one-third never floss.17
Flossing is just one of several options for interdental cleaning. It should be noted that floss is most advantageous in sites where healthy papillae fill embrasure spaces; open embrasures that often accompany tissue loss are likely better served by other devices, such as the interdental brush.10 To be effective, any interproximal device must be used properly; thus, there is need for quality research studies with comparable methodology to evaluate the effectiveness of floss and other interproximal devices in reducing gingival inflammation.10,18
ALTERNATIVE BIOFILM CONTROL MEASURES
The Cochrane Database of Systematic Reviews recently summarized the research on interdental biofilm control devices for self-care that impact periodontal disease and caries. The authors described most evidence as “low to very low certainty,” and cautioned there were weaknesses in most studies, such as small populations and low levels of disease at baseline, that make applying these findings to all populations difficult. Keeping these limitations in mind, key findings include:19
- Floss combined with toothbrushing may reduce gingivitis in the short term (30 days) and medium term (three months)
- A rubber or elastomer tip may reduce plaque, but not gingivitis, in the short term
- An interdental brush may reduce gingivitis and plaque in the short term
- Interdental brushes may be better at reducing gingivitis than flossing in the short and medium term
- Oral irrigators (commonly referred to as water flossers) may reduce gingivitis, and may be better than flossing for reducing gingivitis in the short term
- Wooden cleaning sticks may be better than toothbrushing for reducing gingivitis in the medium term
One classic sign of the inflammation associated with gingivitis is bleeding.20 With effective control of pathogenic biofilm, a decrease in bleeding can be evident to patients — although these changes can take up to a week to occur.21 By then, discouragement by not seeing tangible improvement could impact compliance with interdental cleaning. For those with “floss frustration,” it can be refreshing when a device other than floss is recommended. A patient may pay special attention when they hear clinicians suggest an alternative approach for interproximal biofilm control.
DISRUPTING INTERDENTAL BIOFILM
The availability of a user-friendly interdental cleaning device with a large body of evidence documenting its effectiveness in combatting inflammation would be advantageous for individuals diagnosed in various stages/grades of the AAP disease classification system. No single device or approach has been demonstrated in studies as unequivocally superior. Rather, limited (and largely low-quality) research suggests various interproximal oral hygiene devices may be of value, depending on factors related to patient parameters.19 When personalizing self-care recommendations, providers should consider the dexterity and preferences of the individual, along with the patient’s overall oral condition and AAP periodontal classification.
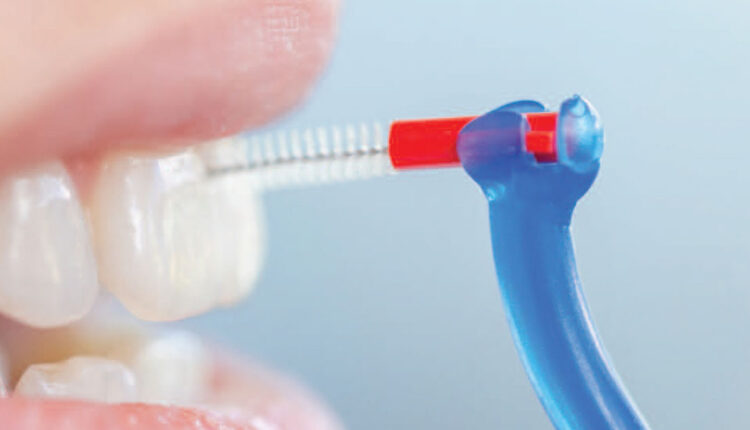
The use of interdental brushes is well accepted by patients and associated with higher plaque removal levels than flossing or use of wood sticks,22 although direct comparisons with water flossers are limited.9 With interdental conditions in which the papillae does not fill the embrasure spaces, interdental brushes have been suggested as the best interproximal cleaning device;22 however, when used at healthy sites with no attachment loss, soft tissue trauma is possible.10 Although evidence indicates interdental brushes remove interdental plaque efficiently, direct evidence documenting their effects on gingival health is currently lacking.22
There is limited data from which to draw conclusions about gingival benefits with the use of wood sticks. A systematic review concluded that while wood sticks do not necessarily demonstrate visible biofilm removal, improvements were documented in gingival health.23 One explanation may be that with sufficient interdental space, a wood stick can adequately disturb subgingival biofilm by displacing soft tissue. This subgingival area would not be visible with a disclosing solution often used in research studies.
Devices that use bursts of either air and/or water to help clean interproximal areas are available. While studies of water flossers document improved clinical signs of gingivitis,22,24,25 corresponding biofilm removal is not as strongly demonstrable. One possible explanation is that water under pressure can disrupt and alter pathogenic bacteria, rendering it less pathogenic, yet not visibly change biofilm amounts when viewed with a disclosing solution. More sophisticated analysis, such as scanning electron microscopy, shows that hydraulic shear forces allow water flossers to disrupt up to 99.9% of the biofilm, although the authors drew no conclusions as to efficacy in reducing the clinical signs of disease.26 Improvements in gingivitis could also be due to selective modulation of inflammatory mediators.27
With a long research history, the water flosser was the first powered interdental cleaning device to earn the American Dental Association’s (ADA) Seal of Acceptance for biofilm removal along the gingival margin and between teeth, and for preventing and reducing gingivitis.28 It is also safe to use.29,30 Recently, a power toothbrush combined with an irrigator function also received the ADA Seal of Acceptance, allowing simultaneous brushing and interproximal debridement. With demonstrated efficacy,24,25,31–33 both technologies require only average dexterity, presenting a possible advantage over floss.
PERIODONTAL PROBING DEPTH
Probing depth is a critical criterion of the AAP classification system for staging periodontitis. Stage I is defined as maximum probing depths of < 4 mm, Stage II by maximum probing depths < 5 mm, and stages III and IV by probing depths > 6 mm.5 These parameters suggest personalized care recommendations for patients in stages III and IV should consider an interdental cleaner’s ability to safely reach deep into periodontal pockets. While there is no clear data on pocket depth reached by floss or most other devices, one in vivo study suggests water flossers can disrupt bacteria up to 6 mm.34
MARRIAGE OF JUDGEMENT AND EVIDENCE
As noted, while there are many types of interdental cleaning devices, a meta-review of interdental mechanical plaque control in managing gingivitis concluded that no single device is superior for all patients.22 Combined with available scientific evidence, clinicians must carefully consider oral care recommendations based on patients’ abilities, lifestyle and preferences. Sharing the extent of a patient’s disease process (per the AAP staging and grading criteria) can help convey the importance of effective and consistent biofilm disruption via brushing and use of an interdental cleaning device.
In review, periodontal disease and caries, although largely preventable, are still too common. By utilizing the AAP classification system to inform and educate,5 clinicians and patients can develop personalized self-care approaches that, with time, may positively impact the prevalence of these conditions.
REFERENCES
- Meyle J, Chapple I. Molecular aspects of the pathogenesis of periodontitis. Periodontol 2000. 2015;69:7–17.
- Eke PI, Thornton-Evans G, Wei L, Borgnakke WS, Dye BA, Genco RJ. Periodontitis in U.S. adults: National Health and Nutrition Examination Survey 2009–2014. J Am Dent Assoc. 2018;149:576–588.
- Murakami S, Mealey BL, Mariotti A, Chapple IL. Dental plaque-induced gingival conditions. J Clin Periodontol. 2018;45(Suppl 20):S17–S27.
- Kinane DF, Attstrom R. Advances in the pathogenesis of periodontitis. J Clin Periodontol. 2005;32(Suppl 6):130–131.
- Tonetti MS, Greenwell H, Korman KS. Staging and grading of periodontitis: framework and proposal of a new classification and case definition. J Periodontol. 2018;89(Suppl 1):S159–S172.
- Asadoorian J. Flossing:CDHA Position Paper. Available at: https://www.cdha.ca/pdfs/Profession/Resources/Flossing_Position_Paper.pdf. Accessed June 15, 2020.
- Christou V, Timmerman MF, van der Velden U, van der Weijden FA. Comparison of different approaches of interdental oral hygiene: Interdental brushes versus dental floss. J Periodontol. 1998;69:759–763.
- Jackson MA, Kellett M, Worthington HV, Clerehugh V. Comparison of interdental cleaning methods: a randomized controlled trial. J Clin Periodontol. 2006;77:1421–1429.
- Salzer S, Slot DE, Van der Weijden FA, Dorfer CE. Efficacy of inter-dental mechanical plaque control in managing gingivitis — a meta-review. J Clin Periodontol. 2015;42(Suppl 16):S92–S105.
- Chapple IL, Van der Weijden F, Doerfer C, et al. Primary prevention of periodontitis: managing gingivitis. J Clin Periodontol. 2015;42(Suppl 16):S71–S76.
- Marchesan JT, Morelli T, Moss K, et al. Interdental cleaning is associated with decreased oral disease prevalence. J Dent Res. 2018;97:773–778.
- Hallmon WW, Waldrop TC, Houston GD, Hawkins BF. Flossing clefts. Clinical and histologic observations. J Periodontol. 1986;57:501–504.
- Walters JD, Chang EI. Periodontal bone loss associated with an improper flossing technique: a case report. Int J Dent Hyg. 2003;1:115–119.
- More than a quarter of U.S. adults are dishonest about how often they floss their teeth. Available at: https://www.perio.org/consumer/quarter-of-adults-dishonest-with-dentists. Accessed June 15, 2020.
- Graves, RC, Disney JA, Stamm JW. Comparative effectiveness of flossing and brushing in reducing interproximal bleeding. J Periodontol. 1989;60:243–247.
- Hujoel PP, Cunha-Cruz J, Banting DW, Loesche WJ. Dental flossing and interproximal caries: a systematic review. J Dent Res. 2;85:298–305.
- Fleming EB, Nguyen D, Woods PD. Prevalence of daily flossing among adults by selected risk factors for periodontal disease — United States 2011–2014. J Periodontal. 2018;89:933–939.
- Slot DE, Dörfer CE, Van der Weijden GA. The efficacy of interdental brushes on plaque and parameters of periodontal inflammation: a systematic review. Int J Dent Hyg. 2008;6:253–264.
- Worthington HV, MacDonald L, Pericic TP, et al. Home use of interdental cleaning devices, in addition to toothbrushing, for preventing and controlling periodontal diseases and dental caries. Cochrane Database Syst Rev. 2019;4:CD012018.
- Lang NP, Bartold PM. Periodontal health. J Clin Periodontol. 2018;45(Suppl 20):S9–S16.
- Loe H, Theilade E, Jensen SB, Schiott C. Experimental gingivitis in man. 3. Influence of antibiotics on gingival plaque development. J Periodontol. 1965;36:177–187.
- Sälzer S, Slot DE, Van der Weijden FA, Dörfer CE. Efficacy of inter-dental mechanical plaque control in managing gingivitis: a meta-review. J Clin Periodontol. 2015;42(Suppl 16):S92–S105.
- Hoenderdos NL, Slot DE, Paraskevas S, Van der Weijden GA. The efficacy of woodsticks on plaque and gingival inflammation: a systematic review. Int J Dent Hyg. 2008:6;280–289.
- Lyle DM, Qaqish JG, Goyal CR, Schuller R. Efficacy of the use of a water flosser in addition to an electric toothbrush on clinical signs of inflammation: 4-week randomized controlled trial. Compend Cont Edu Dent. 2020; 41:170–177.
- Husseini A, Slot DE, Van der Weijden GA. The efficacy of oral irrigation in addition to a toothbrush on plaque and the clinical parameters of periodontal inflammation: a systematic review. Int J Dent Hyg. 2008;6:304–314.
- Cobb CM, Rodgers RL, Kilroy WJ. Ultrastructural examination of human periodontal pockets following the use of an oral irrigation device in vivo. J Periodontol. 1988;59:155–163.
- Cutler CW, Stanford TW, Abraham C, Cederberg RA, Boardman TJ, Ross C. Clinical benefits of oral irrigation for periodontitis are related to reduction of pro-inflammatory cytokine levels and plaque. J Clin Periodontol. 2000;27:134–143.
- American Dental Association. Waterpik Becomes First Powered Interdental Cleaner to Receive ADA Seal of Acceptance. Available at: https://www.waterpik.com/news-press/waterpik-receives-ADA-seal-of-acceptance/. Accessed June 30, 2020.
- Jolkovsky DL, Lyle DM. Safety of a water flosser: a literature review. Compend Cont Educ Dent. 2015;36:146–149.
- Goyal CR, Qaquish JG, Schuller R, Lyle DM. Evaluation of the safety of a water flosser on gingival and epithelial tissue at different pressure settings. Compend Cont Educ Dent. 2018;39:8–13.
- Barnes CM, Russell CM, Reinhardt RA, Payne JB, Lyle DM. Comparison of irrigation to floss as an adjunct to tooth brushing: effect on bleeding, gingivitis and supragingival plaque. J Clin Dent. 2005;16:71–77.
- Goyal CR, Qaqish JG, Schuller R, Lyle DM. Comparison of a novel sonic toothbrush to a traditional sonic toothbrush and manual brushing and flossing on plaque, gingival bleeding, and inflammation: a randomized controlled clinical trial. Compend Contin Educ Dent. 2018;39(Special Issues):14–22.
- Goyal CR, Lyle DM, Qaqish JG, Schuller R. The addition of a water flosser to power tooth brushing: Effect on bleeding, gingivitis, and plaque. J Clin Dent. 2012;23:57–63.
- Gorur A, Lyle DM, Schaudinn C, Costerton JW. Biofilm removal with a dental water jet. Compend Cont Educ Dent. 2009;30(Special issue 1):1–6.
From Decisions in Dentistry. July/August 2020;6(7):40-43.