
Oral Health Implications of a Patient With Albinism and Bilateral Maxillary Paramolars
This case presentation is believed to be the first literature report of the dental management of a patient with oculocutaneous albinism and supernumerary maxillary paramolars.
Oculocutaneous albinism (OCA) is an autosomal recessive genetic disorder caused by a disruption of biosynthesis of the tyrosinase enzyme that results in the absence or reduction of melanin pigmentation in the skin, hair and eyes. Melanin is a photoprotective pigment found in the basal layer of the epidermis that prevents skin damage by absorbing ultraviolet light from the sun. According to the National Organization of Albinism and Hypopigmentation, seven genotype forms of OCA are now recognized based on the distinct genetic mutation.
The first type, OCA1, is the most common subtype in Caucasians and accounts for half of all albinism globally.1 The second, OCA2, is primarily found in African Americans and some Native American groups, and occurs in one in 1000 individuals in sub-Saharan Africa populations.1,2 With albinism occurring in people of every race and nationality throughout the world, it is crucial that dental professionals are aware of this disorder. There is very limited information on the oral manifestations of patients with albinism. This case report is believed to be the first in the literature reporting on the dental management of a patient with OCA2 and extremely rare supernumerary maxillary paramolars.
CASE REPORT
A 25-year-old male reported to the clinic at Midwestern University College of Dental Medicine in Glendale, Arizona, for routine dental care. A medical review revealed the patient had undergone a genetic sequence analysis that confirmed OCA2. He presented with photophobia, nystagmus rapid eye movements and decreased visual acuity. His family is from Nigeria, a sub-Saharan Africa country and the family history revealed his two older sisters also have albinism. The patient reported no other known health conditions and was not on medications.
An intraoral examination revealed generalized gingivitis and moderate localized periodontitis. There was a full complement of 32 teeth, in addition to two ectopically erupted paramolars, or maxillary supernumerary teeth. Paramolars are considered to be smaller, more rudimentary supernumerary molars commonly found buccally or palatally to molars. Ectopic paramolars are considered a developmental dental anomaly. Though etiology is still unknown, according to Nayak et al,3 multiple supernumerary development is thought to be influenced by both genetic and environmental factors.
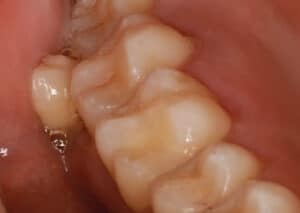
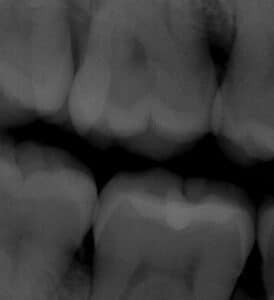
The two paramolars were located bilaterally between the second and third maxillary molars and eruption was displaced buccally (Figure 1 and Figure 2). The paramolars had conical-shaped crowns and were vertically oriented. The supernumerary teeth were visualized clinically but were difficult to ascertain radiographically because of their buccal position (Figure 3). The patient was unaware of having hyperdontia and the paramolars were asymptomatic. Due to microstomia, the patient reported difficulty reaching the posterior teeth for effective oral self-care. Periodontal and restorative treatment was provided. The removal of both paramolars was advised due to possible food pack, dental caries, and the increased risk of continued periodontal disease. Since there are possible suspected bleeding time disorders associated with albinism,1 the patient was advised to obtain hematological testing prior to any oral surgery.

DISCUSSION
Albinism is a congenital condition apparent from birth. Considered an autosomal recessive genetic disorder, each parent carries one copy of the mutated OCA gene, but they themselves do not show signs or symptoms of albinism. More than 80 gene mutations have been found in OCA2. These mutations disrupt tyrosine, the essential substrate of the tyrosinase enzyme, and this interferes with melanin production, causing hypopigmentation in the hair, skin and eyes. The most common OCA2 mutation is a large gene deficiency found in people of sub-Saharan African heritage,4 such as this patient.
Individuals with OCA2 exhibit white or blond hair, very pale to creamy colored skin, and light-colored irises at birth. In African or African Americans with OCA2, the skin and hair remain light throughout their lifetime and the skin has no tanning potential. A further subtype of OCA2 is the Brown OCA specific to African heritage. These individuals are born with light brown skin and hair and gray irises. In Caucasian populations with OCA2, pigmentation may increase with age to include nevi or freckles, and the hair may also darken. Even visual acuity may improve. Due to the low pigmentation in the iris and retina, visual problems include myopia, photosensitivity and functional blindness.2,4 Patients with OCA are photophobic, so the use of tinted safety eyewear during dental treatment may help reduce light sensitivity2,5 from the operatory light or operator loupes. Due to myopia and other visual problems, many individuals with OCA use vision aids, but they may also benefit from large-print postoperative instructions and educational pamphlets.
ORAL MANIFESTATIONS
Dental manifestations reported to occur with OCA include severe halitosis,1 gingivitis, gingival bleeding, ulcerations of oral mucosa (such as Sutton’s recurrent aphthous ulcers on the tongue and hard palate),1 and chronic periodontal diseases.2 In addition, because of sun exposure damage, patients with OCA may experience extreme dry lips1 and angular cheilitis. Due to microstomia and limited opening, pediatric-sized handpieces may prove beneficial. Oral self-care may be difficult due to microstomia, so patients are advised to try child-sized toothbrushes, flossers with handles, and oral irrigators. Frequent recare visits and fluorides for caries prevention should also be stressed. Oral hygiene counseling and patient education introduced at an early age may prevent the need for more invasive future dental procedures.
Due to lower skin pigmentation, patients with albinism are highly susceptible to sun exposure and skin damage. They risk solar ultraviolet radiation-related skin erythema, blistering and cutaneous cancers, such as melanoma.1 Dentists can play an important role in addressing these issues during the head and neck oral cancer examination, which is advisable at every dental visit, along with referral to a dermatologist if appropriate.2
Since some types of OCA are associated with other syndromes, such as Hermansky-Pudlak (a genetic platelet deficiency found primarily in Puerto Rican albinism populations), most physicians advise a bleeding time test for all patients with albinism. Patients with this additional syndrome have bruising, frequent nose bleeds, and report excessive bleeding after surgery or tissue trauma after dental work.4 Young patients with albinism may have never had any type of surgery, and wisdom teeth extraction may be their first surgical experience. To prevent surprises of these possibly undiagnosed syndromes associated with albinism, a referral to a hematologist for hematologic and genetic testing may be prudent.2,4,5
HYPERDONTIA PREVALENCE
Hyperdontia is considered quite rare, with an incidence rate of only 0.04% to 2.7%.6 In a review of the literature, supernumerary teeth have been found to occur more often in Asian populations,3 American Blacks and males.7 They also tend to present in the maxilla.6 The most accredited theory for how hyperdontia teeth develop, per Nayak et al,3 is through a combination of genetic and environmental factors called the unified etiology explanation. There may be a hereditary trait with low dominant autosomal transmission, so the presence of supernumerary teeth in the family of patients with this dental anomaly indicates that some generations will be affected, but others will not be predisposed.3
Supernumerary teeth are classified according to syndrome and non-syndrome relationship, chronology, morphology, topography and orientation. Paramolars fall into the topographic category, and most commonly occur in the interproximal space buccal to the second and third molars.3,6 A non-tubercle paramolar’s shape is classified as rudimentary or dysmorphic, and may cause damage to the buccal mucosa with traumatic biting due to its buccal position. There is a wide variation in the statistics and figures of supernumerary teeth, but, in the last 50 years, very few cases of paramolars have been reported in the literature — and even fewer were maxillary or bilateral presentations.3,6
Few dental anomalies have been reported in the literature for OCA; these include febrile induced molar-incisor enamel hypoplasia and a type 2 dens invaginatus of the maxillary lateral incisors.2,5 To the authors’ knowledge, no supernumerary teeth — or, specifically, bilateral maxillary paramolars — have been reported in patients with albinism (other than this case presentation of this rare occurrence).
Removal of any supernumerary teeth must be carefully considered, as their position may cause pathological changes or disruption of bone or tooth alignment, gingival inflammation or periodontal disease, pericoronitis, or root resorption of adjacent teeth.3 If the hyperdont is not extracted, the condition must be closely monitored with frequent radiographs. For patients with albinism requiring third molar or other extractions, this surgical decision must consider periodontal and functional concerns versus surgical complications. A consultation with an oral surgeon and radiologist for a cone beam computed tomography scan and a hematologist for bleeding time evaluation may be required for patient safety.
CONCLUSION
Albinism is a worldwide genetic disorder. It requires a multidisciplinary approach in which dental professionals play a key role in the management of both dental and medical concerns. In conjunction with the physician, hematologist, ophthalmologist and dermatologist, the dentist should establish a comprehensive preventive program that addresses the multifactorial oral issues that can present in patients with OCA.
In addition, supernumerary teeth may cause not only functional and occlusal problems, but also esthetic, mucosal and medical challenges. As part of the interdisciplinary team, dentists should be aware of the various types of supernumerary teeth so they are able to establish an early diagnosis and appropriate treatment plan for these rare, but important, dental anomalies.
KEY TAKEAWAYS
- Seven genotype forms of oculocutaneous albinism (OCA) are now recognized based on the distinct genetic mutation.
- The first type, OCA1, is the most common subtype in Caucasians and accounts for half of all albinism cases.1 The second, OCA2, is primarily found in African Americans and some Native American groups.1,2
- Oral manifestations reported to occur in OCA include severe halitosis,1 gingivitis, gingival bleeding, ulcerations of oral mucosa, and chronic periodontal disease.2
- There is very limited information on dental implications or oral manifestations of patients with albinism, and this case report is believed to be the first in the literature reporting on the dental management of a patient with OCA2 and extremely rare supernumerary maxillary paramolars.
- The removal of both paramolars was advised due to possible food pack, caries, and the increased risk of continued periodontal disease.
- For patients with albinism requiring third molar or other extractions, the surgical decision must consider periodontal and functional concerns versus surgical complications.
- Prior to surgery, consulting with an oral surgeon, a radiologist for cone beam imaging, and a hematologist for a bleeding time evaluation may be required for patient safety.
ACKNOWLEDGMENT: This care report was approved by the Midwestern University Office of Research and Sponsored Programs Institutional Review Board AZCS-211.
References
- Sharma D, Jhingta PK, Bhardwaj VK, Rasila D, Negi N, Vaid S. Oculocutaneous albinism and the oral manifestation in a 14-year-old boy — A case report and review of literature. J Dent Allied Sci. 2017;6:93–97.
- Murthy V, Yuvraj V, Thomas S, Nair P. Prosthodontic management of an albinism patient — dental implications and management. BMJ Case Rep. 2013;2013:bcr2012008004.
- Nayak G, Shetty S, Singh I, Pitalia D. Paramolar — A supernumerary molar: A case report and an overview. Dent Res J (Isfahan). 2012;9:797–803.
- Feliciano NZ, Rivera E, Agrait E, Rodriguez K. Hermansky-Pudlak syndrome: dental management considerations. J Dent Child (Chic). 2006;73:51–56.
- Suprabha BS. Premolarized double dens in dente in albinism — a case report. J Indian Soc Pedod Prev Dent. 2005;23:156–158.
- Arandi NZ. Hyperdontia: Exploring the develpmental abnormality. J Pre-Clin Clin Res. 2020;14:178–183.
- Harris EF, Clark LL. An epidemiological study of hyperdontia in American blacks and whites. Angle Orthod. 2008;78:460–465.
From Decisions in Dentistry. September 2022;8(9)14-16.


