Improving the Oral Health of Pregnant Patients
Researchers now better understand how quickly gingivitis may develop in pregnant women.
Researchers now better understand how quickly gingivitis may develop in pregnant women. Conventional wisdom held that gingivitis progressed steadily during pregnancy, but new research from a team led by Michael Reddy, DMD, of the University of Alabama at Birmingham has found that by the end of the first trimester, a woman can have up to three times more bleeding-on-probing sites than she had before becoming pregnant. Instead of being a slowly worsening condition, pregnancy-related gingivitis can advance quickly and last throughout pregnancy and the postpartum period.1 This poses health risks to the mother and child, as Han2 cites numerous studies that have found a correlation between maternal periodontal infection and adverse pregnancy outcomes, such as premature and low-birthweight infants. 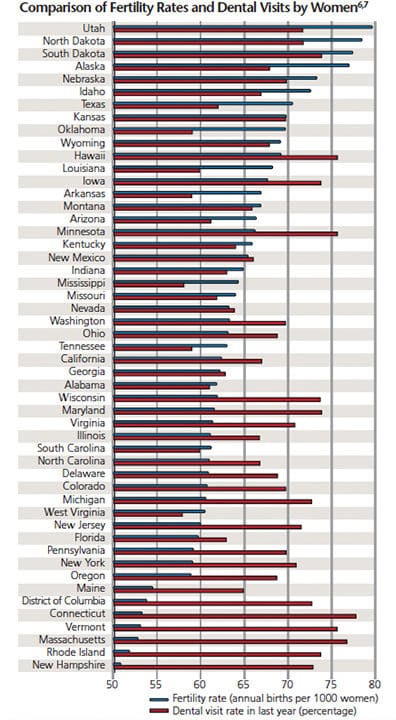
What can be done to improve this situation? According to the American College of Obstetrics and Gynecology (ACOG) position statement on dental care, “pregnancy is a ‘teachable’ moment when women are motivated to adopt healthy behavior.”3 And indeed, prenatal counseling about oral health care correlates highly with oral hygiene during pregnancy.4 Yet in a study of patient and provider attitudes toward oral health in pregnancy, 80% of obstetricians did not use ACOG-recommended oral health screening questions during prenatal visits, even though a majority acknowledged a need for oral health care during pregnancy. Furthermore, 94% of obstetricians did not routinely refer all patients to a dentist.5
Clearly, dental teams have an opportunity to improve the oral health of pregnant women by getting the message out about the importance of oral care, particularly when pregnant. To gain insight into where the greatest opportunities for outreach from dentists to medical professionals and patients may lie, we have combined U.S. Centers for Disease Control and Prevention (CDC) statistics on state fertility rates6 with a Kaiser Family Foundation analysis of the CDC’s data on percentage of women in each state who reported visiting a dentist for any reason in the past year.7 States in which the fertility rate is high, but the percentage of women visiting the dentist is low — such as Alaska, Texas, Oklahoma, Louisiana, Arkansas and Mississippi — represent areas in which the need to improve outreach to pregnant women is greatest.
REFERENCES
- Reddy M. Gingivitis during the first/second trimesters of pregnancy. International Association for Dental Research General Session. Seoul, Republic of Korea. June 23, 2016.
- Han YW. Oral health and adverse pregnancy outcomes — What’s next? J Dent Res. 2011;90:289–293.
- American College of Obstetrics and Gynecology Committee on Health Care for Underserved Women. Oral Health Care During Pregnancy and Through the Lifespan. Available at: acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-Health-Care-for-Underserved-Women/Oral-Health-Care-During-Pregnancy-and-Through-the-Lifespan. Accessed November 16, 2016.
- Thompson TA, Cheng D, Strobino D. Dental cleaning before and during pregnancy among Maryland mothers. Matern Child Health J. 2013;17:110–118.
- Strafford KE, Shellhaas C, Hade EM. Provider and patient perceptions about dental care during pregnancy. J Matern Fetal Neonatal Med. 2008;21:63–71.
- U.S. Centers for Disease Control and Prevention. National Center for Health Statistics State and Territorial Data. Available at: cdc.gov/nchs/fastats/state-and-territorial-data.htm. Accessed November 16, 2016.
- Kaiser Family Foundation. State Health Facts: Percent of Women Who Visited a Dentist or Dental Clinic Within the Past Year. Available at: kff.org/womens-health-policy/state-indicator/percent-of-women-who-had-dental-visit. Accessed November 16, 2016.
From Decisions in Dentistry. December 2016;2(12):54


