
Fixed Retention in Orthodontics
Clinicians have many options when choosing and customizing fixed retention devices in orthodontics.
The importance of retention after orthodontic treatment is well recognized.1,2 In 1934, Oppenheim3 stated “Retention is a problem in orthodontic treatment, in fact, it is the problem.” Retention is the final phase of active orthodontic therapy, and the clinical goal is to maintain teeth in a healthy, functional and esthetic position. In orthodontics, planning for retention begins with proper diagnosis, treatment planning, sound biomechanical principles, and placing the teeth in optimal functional occlusion. It is considered inevitable that for the majority of treated cases, some degree of relapse will occur, either with or without retention.4
Among the many suggested factors that influence stability, the primary three are: (1) periodontal ligament fibers and gingival fibers affected by orthodontic tooth movement, which require time for reorganization when the appliances are removed; (2) late mandibular growth and; (3) physiologic imbalance of local extrinsic forces, such as lip, cheek and tongue pressures acting on the corrected dentition so the teeth may be in an inherently unstable position.
The method of retention is best selected at the outset of treatment and incorporated in the treatment plan for that particular case. Retention requirements are determined by the characteristics of the original malocclusion and effects of orthodontic treatment. While the type and term of a retention regimen may prove controversial, it is generally accepted in orthodontics that certain situations are best addressed by fixed retention.5,6 These include diastemas, anterior crowding, rotated teeth, maintenance of lower incisor position during late growth, maintenance of pontic or implant space, inter-canine width expansion, adult treatment, and where patient compliance is questionable (especially over long term).

stainless steel wire bonded to the maxillary incisors.
DEVICE SELECTION
In recent times, fixed retention has been an increasingly popular approach in orthodontics. Surveys in the United States and elsewhere have identified trends in the selection and duration for retainer wear.7–11 Choosing fixed retainers for the lower dental arch is most popular, with increasing use of upper vacuum-formed retainers — with or without fixed bonding to the maxillary incisors. Most orthodontists recommend removable retainers for a minimum of two years, and even up to five years or longer.
Fixed retainers may be utilized unless there are contraindications, which might include active caries or periodontal disease, poor oral hygiene, anterior deep bite for maxillary retention, atypical lingual tooth morphology, or incomplete treatment.
Potential problems and complications can occur with fixed retainers, however. For example, there can be areas of plaque accumulation — although studies do not report an increase in interproximal caries or periodontal disease.12,13 In addition, detachment of the retainer from the tooth surface can cause teeth to shift. While rare, other significant issues include torqueing of teeth (leading to tooth displacement), gingival recession and bone loss.14,15 Fixed retainers therefore require long-term maintenance and follow-up with either the orthodontist or general dentist. Self-care is also important, and use of interdental cleaning aids is advised to ensure adequate oral hygiene.
Several types of fixed retainers are available. Some can be fabricated directly in the mouth, if desired, while others are best fabricated indirectly on a stone model. A transfer tray fashioned out of vinyl polysiloxane putty can facilitate access and ease of placement on the teeth, and is highly recommended so it is passively placed. The two basic designs of lingual bonded retainers are a flexible wire bonded to each tooth in the segment, or a more rigid wire bonded only on the canines.
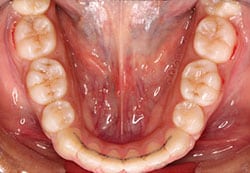
The use of flexible multistrand spiral wire for fixed retainers was first advocated by Zachrisson in the 1980s (Figure 1). Current orthodontic opinion recommends either the use of 0.0215- or 0.0195-inch multistrand wire, or a 0.030- or 0.032-inch sandblasted, rigid, round stainless steel wire.16 Five-stranded coaxial wires are suggested for use in bonded lingual retainers rather than dead soft.17 Failure rates of approximately 12% in two years have been reported.18 The most common mode of failure is loosening between the wire and adhesive, or adhesive-enamel and wire breakage caused by stress.19 The flexibility of the wire allows differential tooth movement and is particularly useful for patients who present with loss of periodontal support. It also reduces the concentration of stress within the adhesive, thus minimizing the possibility of subsequent failure. However, distortion of the wire can lead to unintentional tooth movement.
Another quick option for fabrication of a flexible retainer wire is to take two 0.010- or 0.012-inch stainless steel ligatures and tightly twist them together, double fold them, and continue twisting so that four filaments are present.

CLINICAL ALTERNATIVES
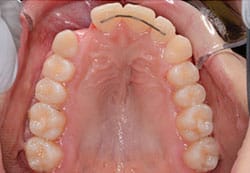
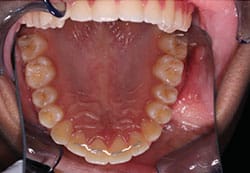
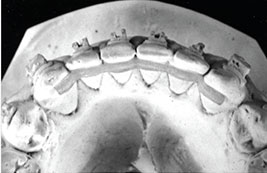
Rigid mandibular canine-to-canine retainer bars with bonding pads at the terminals are available in different sizes through various vendors. These can be used canine to canine or on two adjacent incisors to maintain closure of a diastema (Figure 2). They are excellent for maintaining inter-canine width, but less so in preventing individual tooth rotations, as they are attached only to the canines. Movement of the lower incisors can occur if the wire is not attached to them, but bonded only on the terminal teeth (the canines), especially if the wire is not intimately contacting the teeth on their entire lingual surfaces. Although bonding to all incisors remedies this problem, it can lead to bond failure at the adhesive/wire interface. This occurs as there is a natural tendency of teeth to move from the periodontal ligament (PDL), and the wire’s rigidity does not allow this. If the adhesive is applied across the entire width of the tooth and interproximally (rather than spot locations on the teeth), rigidity is improved — but the splinting of teeth does not allow physiological movement and bond failures will occur. Figure 3 shows a custom, laboratory-made lingual retainer, with bonding pads on all six anterior teeth and accessible interproximal spaces.

bonding pads on all teeth.
As a further example of clinical choices in fixed retention, the White Gold Ortho FlexTech (Reliance Orthodontic Products) (Figure 4) is fashioned from 14-karat white gold and has a low profile (0.0383 inches wide by 0.01580 inches high). It can be directly placed, and adaptation to the tooth surfaces is excellent, as it naturally forms to the lingual arch curvature and lays flat against the teeth. It also offers good mechanical retention of the adhesive and low failure rates due to “flex linkage” of the chain.
Another choice that is gaining popularity is Retainium wire (Reliance Orthodontic Products) (Figure 5), which is a rectangular 0.027×0.11-inch ribbon-form, nickel-free titanium wire that is dead soft. It is easy to configure and adapt passively, therefore minimizing inadvertent tooth movement from forces if the wire were active. Sandblasting the surface will improve the mechanical attachment with the bonding adhesive.
Fashioned using computer aided design/computer aide manufacturing (CAD/CAM) technology, Memotain (AOA Orthodontic Appliances) is a 0.016×0.016-inch nickel titanium retainer (Figure 6). Its memory-based metal helps it maintain its shape integrity and provides flexibility. These devices are electropolished to a smooth surface and the retainer’s edges are rounded for comfort. Due to the small dimensions and contoured custom fit, this may be a good choice for maxillary anterior teeth. The transfer tray makes placement easy and predictable. Even though all the teeth are bonded, the flexibility of the metal allows independent normal movement of the teeth within the PDL during mastication, without breakage or bonding failure between teeth.20
Fiber reinforced plastics (FRP) for retainers were first introduced in orthodontics in the 1990s using a two-step process from pre-impregnated, unidirectional long glass fibers in a thermoplastic resin matrix of either poly(ethylene terephthalate glycol) or polycarbonate.21 The advantages include ease of fabrication and customization of design, directional mechanical strength, good esthetics, and a nickel-free design (Figure 7). Current commercially available FRPs include Ribbond (Ribbond) and everStick ORTHO (StickTech). Due to the manner in which bonding is accomplished (with adhesive coverage across all the teeth, including interdental areas), they act as splints and prevent individual tooth movement. A potential downside is that low flexibility can induce high strain within the adhesive composite, leading to micro-cracks or weakening of the wire-adhesive and adhesive-enamel interface, leading to loosening or fracture of the wire.
Available since 1992, Ribbond reinforcement material is composed of pre-impregnated, silanized, high-molecular-weight polyethylene fibers woven in a ribbon form. This is lightly wetted with an adhesive resin consisting of methacrylate ester monomers just before placing on the teeth.22 Made from silanated continuous unidirectional glass fiber bundles in a thermoplastic polymer network structure and resin matrix of bisphenol A-glycidyl methacrylate and dimethacrylate-polymethylmethacrylate, everStick ORTHO material is light cured and adapted, and then placed directly in the mouth. Its advantages include predictable bonding and handling.23,24
With the advances in three-dimensional printing and polymer chemistry, new materials and methods are on the horizon. PEEK is a thermoplastic composite made with poly ether ketone polymer. Used in medical and dental applications, PEEK is white colored and features excellent mechanical properties.25 It can be milled to a customized shape using CAD/CAM technology and bonded using the acid etch technique. The digital design matches the patient’s individual tooth anatomy. Positioning jigs on the canines facilitate placement of the retainer. The 0.8-mm thickness of the wire offers a comfortable fit while still allowing physiological movement of the teeth — an important goal in orthodontics. In addition, it facilitates flossing because the interproximal areas are adhesive-free.
CONCLUSION
Fixed bonded retainers are preferred when long-term retention is indicated or patient compliance may be poor. Various techniques and materials for fixed bonded retainers have been described in the literature. Numerous clinical options are available, and range from direct fabrication to in-house or lab fabrication utilizing a variety of materials. They all seem to work equally well, so the final clinical approach will be determined based on the individual patient and case, as well as clinician preference.
KEY TAKEAWAYS
- Retention is the final phase of active orthodontic therapy, with a clinical goal of maintaining teeth in a healthy, functional and esthetic position.
- Planning for retention begins with proper diagnosis, treatment planning, sound biomechanical principles, and placing the teeth in optimal functional occlusion.
- Retention requirements are determined by the characteristics of the original malocclusion and effects of orthodontic treatment.
- The method of retention is best selected at the outset of treatment and incorporated in the treatment plan for that particular case.
- Fixed retainers may be utilized unless there are contraindications, which might include active caries or periodontal disease, poor oral hygiene, anterior deep bite for maxillary retention, atypical lingual tooth morphology, or incomplete treatment.
- Several types of fixed retainers are available. Some can be fabricated directly in the mouth, if desired, while others are best fabricated indirectly on a stone model.
- Ultimately, the individual case — as well as clinician preference — will determine the best clinical approach.
REFERENCES
- Nanda R, Burstone CJ. Retention and Stability in Orthodontics. Philadelphia:W.B.Saunders;1993.
- Little RM. Stability and relapse of dental arch alignment. BJ J Orthod.1990;17:235–241
- Oppenheim A. Crisis in orthodontia Part I. 2. Tissue changes during retention. Skogborg’s septomy. Int J Orthod. 1934;20:639–644.
- Johnston CD, Littlewood SJ. Retention in orthodontics. Br J Orthod. 2015;218:119–122.
- Rody WJ, Wheeler TT. Retention management decisions: a review of current evidence and emerging trends. Semin Orthod. 2017;23:221–228.
- Rossouw PE, Shaima Malik S. The retention protocol. Semin Orthod. 2017;23:237–248.
- Pratt MC, Kluemper GT, Hartsfield JK Jr, Fardo D, Nash DA. Evaluation of retention protocols among members of the American Association of Orthodontists in the United States. Am J Orthod Dentofac Orthop. 2011;140:520–526
- Padmos JA, FudaleJ PS, Renkemac AM. Epidemiologic study of orthodontic retention procedures. Am J Orthod Dentofacial Orthop. 2018;153:496–504.
- Singh P, Grammati S, Kirschen R. Orthodontic retention patterns in the United Kingdom. J Orthod. 2009;36:115–121.
- Vandevska-Radunovic V, Espeland L, Stenvik A. Retention: type, duration and need for common guidelines. A survey of Norwegian orthodontists. Orthodontics (Chic). 2013;14:e110–e117.
- Wong PM, Freer TJ. A comprehensive survey of retention procedures in Australia and New Zealand. Aust Orthod J. 2004;20:99–106.
- Artun J, Spadafora AT, Shapiro PA. A 3-year follow-up study of various types of orthodontic canine-to-canine retainers. Eur J Orthod. 1997;19:501–509.
- Booth FA, Edelman JM, Proffit WR. Twenty-year follow-up of patients with permanently bonded mandibular canine-to-canine retainers. Am J Orthod Dentofac Orthop. 2008;133:70–76.
- Shaughnessy TG, Proffit WR, Samara SA. Inadvertent tooth movement with fixed lingual retainers. Am J Orthod Dentofacial Orthop. 2016;149:277–286.
- Kučera J, Marek I. Unexpected complications associated with mandibular fixed retainers: a retrospective study. Am J Orthod Dentofacial Orthop. 2016;149:202–211.
- Zachrisson BU. Multistranded wire bonded retainers: from start to success. Am J Orthod Dentofacial Orthop. 2015;148:724–727.
- Baysal A, Uysal T, Gul N, Alan MB, Ramoglubl SI. Comparison of three different orthodontic wires for bonded lingual retainer fabrication. Korean J Orthod. 2012;42:39–46.
- Tacken MP, Cosyn J, Wilde P, De Aerts J, Govaerts E, Vannet BV. Glass fibre reinforced versus multistranded bonded orthodontic retainers: a 2-year prospective multi-centre study. Eur J Orthod. 2010;32:117–123.
- Bearn DR, McCabe JF, Gordon PH, Aird JC. Bonded orthodontic retainers: the wire-composite interface. Am J Orthod Dentofacial Orthop. 1997;111:67–74.
- Kravitz ND, Grauer D, Schumacher P, Jo YM. Memotain: a C/D/CAM nickel-titanium lingual retainer. Am J Orthod Dentofacial Orthop. 2017;151:812–815.
- Ardeshna AP. Clinical evaluation of a fiber-reinforced composite orthodontic retainer. Am J Orthod Dentofacial Orthop. 2011;139:761–767.
- Salehi P, Najafi HZ, Roeinpeikaret SM. Comparison of survival time between two types of orthodontic fixed retainer: a prospective randomized clinical trial. Progress in Orthodontics. 2013;14:25.
- Sfondrini MF, Fraticelli D, Castellazzi L, Scribante A, Gandini P. Clinical evaluation of bond failures and survival between mandibular canine-to-canine retainers made of flexible spiral wire and fiber-reinforced composite. J Clin Exp Dent. 2014;6:e145–e149.
- Annousaki O, Zinelis S, Eliades G, Eliades T. Comparative analysis of the mechanical properties of fiber and stainless steel multi stranded wires used for lingual fixed retention. Dent Mater. 2017;33:2e205–e211.
- Zachrisson P. A New Type of Fixed Retainer. Available at: https://www.orthopracticeus.com/clinical/a-new-type-of-fixed-retainer. Accessed September 30, 2019.
The author has no commercial conflicts of interest to disclose.
From Decisions in Dentistry. November/December 2019;5(10):16,18,21—22.


