 NALIN PRUTIMONGKOL/ISTOCK/GETTY IMAGES PLUS
NALIN PRUTIMONGKOL/ISTOCK/GETTY IMAGES PLUS
Esthetic Management of Tetracycline-Induced Staining
Thanks to advances in technology and materials, oral health professionals now have more esthetically driven treatment options for patients who present with tetracycline-induced tooth discoloration.
Tetracycline is a broad-spectrum antibiotic used to treat various bacterial infections. Examples include infections of the respiratory tract, urinary tract and skin. It is also used to treat typhus, Rocky Mountain spotted fever, certain sexually transmitted diseases, acne, anthrax, cholera and Helicobacter pylori.1 Use of this common antibiotic has multiple side effects, however — including tooth discoloration.1,2 Tooth staining caused by tetracycline use is dependent on the dose, duration of treatment, and stage of tooth development when administered.3
The mechanism of staining is tetracycline’s ability to form a complex with calcium ions in a process called chelation.4 Once these complexes are deposited into bone and teeth, the dentin becomes more susceptible to staining than enamel.5 This tetracycline-induced discoloration is presumed permanent since dentin and enamel cannot be remodeled once formed. The staining varies from yellow to grey or brown, and may present with or without banding.4 Therefore, many physicians recommend that tetracycline should not be used during the second and third trimester of pregnancy and in children under the age of 8.
Tooth discoloration from tetracycline use is not as prevalent as it once was. The medical awareness generated from the use of this antibiotic and its side effects has greatly impacted how and when providers prescribe this medication. However, there are still individuals at risk for tooth discoloration from tetracycline use. With advancing technology and enhanced dental materials, oral health professionals now have more applicable, esthetically driven treatment options for patients who present with tetracycline-induced staining.
CLINICAL CASE OVERVIEW
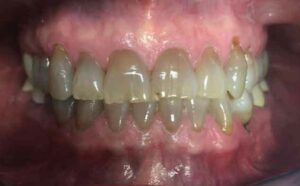
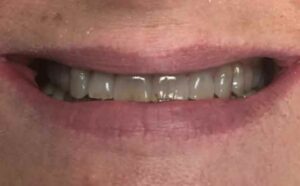
A 55-year-old female presented to the general dental clinic with the chief complaint that “my teeth are too dark, and I do not like my smile.” Due to the patient’s profession as a high school teacher, she wanted to improve her outward appearance and self-confidence. The patient was open to all options presented and was financially stable. Prior to the initiation of any restorative treatment, her medical and social histories were reviewed, and oral and radiographic evaluations performed. These revealed no significant contraindications. The patient’s dental history involved past treatment of routine crowns and direct restorations requiring maintenance. A caries risk assessment deemed her as low risk. However, findings included a few defective restorations and Class V lesions that needed attention. Slight incisal wear was noted during the hard tissue examination, but there was no evidence or complaint of dentinal hypersensitivity. The patient’s periodontal and soft tissue evaluations were within normal, healthy limits. Regular hygiene appointments were scheduled and performed prior to restoration of the tetracycline defect.
The patient had some knowledge regarding treatment options, which led to discussions of three clinical approaches: bleaching, veneers, or full coverage crowns. The advantages and disadvantages of direct tooth-colored restoration were also presented. Following the presentation, preoperative photos (Figure 1 and Figure 2) were taken, as were alginate impressions for diagnostic casts and a laboratory diagnostic wax-up. After the patient reviewed and approved the diagnostic wax-up, a decision was made to proceed with full coverage crowns as the restoration of choice. Prior to the initiation of treatment, preoperative provisional stents were made from the diagnostic casts using a vacuum-formed suck-down material. Upon discussion with the laboratory technicians, the restoration of choice for this patient was determined to be porcelain-fused-to-zirconia (PFZ) crowns with lingual zirconia occlusion for teeth #5 to 12.
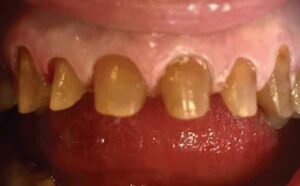
PREPARATION APPOINTMENT
Following the guidelines for zirconia, the teeth were prepared for crowns using a chamfer-tip diamond bur with a 1.5 mm facial reduction transitioning to a 1.0 mm lingual margin. Occlusal and incisal reduction of 2.0 mm were also obtained using a barrel-shaped diamond to accommodate for clearance and material thickness. It should be noted that margins were placed slightly subgingivally to avoid unesthetic darkness at the cervical areas (Figure 3). Although several methods of gingival retraction were available, an astringent retraction paste containing 15% aluminum chloride was placed into the sulcus, with special care devoted to the anterior tissue. The paste was allowed to set for two minutes in conjunction with the patient biting into stiff cotton caps for pressure. After the required time, the paste was thoroughly rinsed with an air-water syringe until clear, moisture-free margins were visible. Keeping the area as dry as possible, a light-body vinyl polysiloxane impression material was syringed carefully around the crown-prepped teeth. The full-arch impression tray filled with heavy-body vinyl polysiloxane was then positioned and held for the recommended setting time.
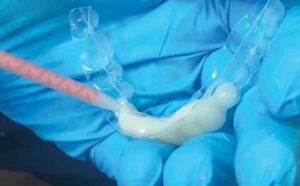
FABRICATION OF PROVISIONALS
Using the preoperative provisional stent, the tray was filled with a bisacryl dual-cure temporary material (Figure 4). After being transferred to the mouth and placed over the preparations, the material was allowed to set to a gel state before removal (Figure 5). Allowing for proper cure times, the temporaries were removed and trimmed with discs and burs to clinical satisfaction. Proper marginal fit was of utmost importance in avoiding gingival irritation or recession around the darkened preparations during the provisional phase. The teeth were air dried prior to seating the provisional crowns with a non-eugenol temporary resin cement. Following removal of the excess cement, the patient and staff chose Vita A-1 as the most appropriate shade. The patient was allowed to evaluate the provisionals for esthetic appearance and function. Postoperative and home-care instructions were issued upon dismissal.
DELIVERY AND FINAL CEMENTATION
Within approximately two weeks, the patient returned for final cementation of the PFZ restorations. Following removal of the provisional crowns, the teeth and soft tissue were cleaned of any excess cement. Cotton pellets soaked in a chlorhexidine gluconate 0.12% oral rinse were used to completely cleanse the tissue, and the preparations were cleaned with a flour of pumice paste with chlorhexidine gluconate to remove any further debris. The PFZ crowns were individually tried on each tooth to evaluate proper marginal fit. Once the fit was deemed satisfactory, all the crowns were tried in together for proper interproximal and occlusal contacts.
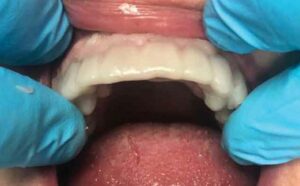
It was important for the patient, as well as her accompanying family, to approve the esthetics of the crowns prior to cementation. Upon approval, a universal cleaning paste containing sodium hydroxide was placed on the contaminated intaglio surfaces of each restoration and allowed to set for 20 seconds. The crowns were thoroughly rinsed and dried as they were prepared for the final cement. After filling the crowns with a self-adhesive universal cement, they were placed on their respective teeth. Once the cement reached a gel state, excess material was removed around the margins and the sites were flossed interproximally.
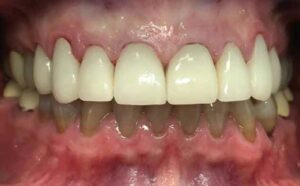
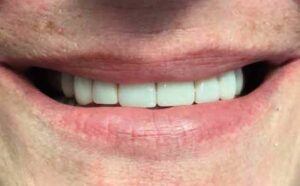
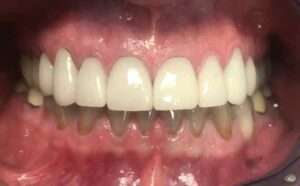
Final occlusion was once again checked for accuracy and patient comfort (Figure 6 and Figure 7). It should be noted that the gingiva around tooth #6 was inflamed. Therefore, proper self-care and hygiene instruction were emphasized to the patient to assist in achieving optimal esthetic results (Figure 8).
DISCUSSION
Severe intrinsic staining and discoloration in anterior teeth present a difficult esthetic challenge. Ultimately, the optimal therapeutic approach is chosen based on the clinical, mechanical, and cosmetic needs of the tooth being restored.6 In this case, the patient wanted a whiter smile. Due to the tetracycline defect, it was imperative the material chosen offered both superior strength and masking capabilities.
Materials are basically classified in two categories: homogeneous in composition, meaning uniform in structure throughout; or heterogeneous (i.e., nonhomogeneous), meaning they differ structurally from inside to outside. Two heterogeneous materials, zirconia and lithium disilicate, were debatable choices for this case due to their high-strength core characteristics.6 It was noted that zirconium oxide does not require as much tooth reduction as glass-based all-ceramic crowns. However, the degree of flexure and fracture strength of the monolithic material reduce the potential for chips and breakage associated with the use of veneered layered porcelain.7 In addition, the flexural moduli and strength of highly translucent zirconia materials (which offer a flexural strength of 500 to 1200 megapascals) are significantly greater than those of lithium disilicate (with a flexural strength of 350 megapascals).8
Although similar in functionality, lithium disilicate is much more translucent than zirconia. In fact, compared to lithium disilicate of the same thickness, the most translucent zirconia is only about 70% as translucent. Contrary to most anterior restorative esthetic cases, a higher translucency is not always desirable — such as in this case of severe staining from tetracycline use.
While using a lithium disilicate with medium or high opacity veneering can provide improved esthetics, the opacity of zirconia is more advantageous to gaining optimal esthetic acceptance when masking is desired.9 Although practitioners should strive to conserve natural tooth structure, such as during clinical preparation for porcelain veneers, cases will occasionally warrant deviation from this clinical concept. The severity of the tetracycline-induced staining, coupled with the patient’s esthetic demands and necessary material strength, dictated full coverage in this case — and PFZ crowns were deemed the most ideal esthetic solution.
CONCLUSION
Tetracycline-induced staining presents an esthetic challenge for the patient and clinician. However, the opportunity to achieve successful esthetic outcomes in these cases is a direct result of rapidly evolving advances in dentistry. Thus, patients presenting with tooth discoloration from tetracycline use now have many esthetically attractive choices for restoring the dentition back to its natural state.
Rational judgment regarding the fundamentals of treatment planning and restorative materials, as well as clinical knowledge and experience, are necessary to achieve an ideal outcome for the patient and practitioner.
KEY TAKEAWAYS
- While not as prevalent as it once was due to changes in prescribing practices, tooth discoloration is a well-known side effect from the use of tetracycline antibiotics.
- Tooth staining caused by tetracycline is dependent on the dose given, duration of treatment, and stage of tooth development at the time of administration.3
- Such staining varies from yellow to grey or brown, and may present with or without banding.4
- Thanks to advances in materials and technology, dentists now have more esthetically driven treatment options for patients who present with tetracycline-induced staining.
- Among the esthetic options are bleaching, veneers, full coverage crowns, or tooth-colored direct restorations.
- As demonstrated in this case report, severe intrinsic discoloration in anterior teeth presents a difficult esthetic challenge.
- Ultimately, the optimal approach to treatment is chosen based on the clinical, mechanical, and cosmetic needs of the tooth being restored.6
- In this case, the patient wanted a more esthetic smile. Due to the tetracycline defect, it was imperative that the material chosen had both superior strength and masking capabilities. Ultimately, the clinical team and patient chose porcelain-fused-to-zirconia crowns.
- Another takeaway is that contrary to most esthetic anterior restorative cases, a higher translucency material is not always desirable — such as in this patient’s case, where masking was a clinical goal.
REFERENCES
- Omudhome O, Marks J. Tetracycline. Available at: http/://www.medicinenet.com/tetracycline/article.htm. Accessed May 28, 2021.
- Huddar D, Shigli K, Sandhyarani B. Flawless smile with zirconia crowns for tetracycline stained teeth. J Dent Health Oral Disord Ther. 2016;5:346–348.
- Cohlan SQ. Tetracycline staining of teeth. Teratology. 1977;15:127–129.
- Sanchez AR, Rogers RS, Sheridan PJ. Tetracycline and other tetracycline-derivative staining of the teeth and oral cavity. Int J Dermatol. 2004;43:709–715.
- Wallman IS, Hilton HB. Teeth pigmented by tetracycline. Lancet. 1962;1:827–829.
- Spear FM. Treatment Planning Materials, Tooth Reduction, and Margin Placement for Anterior Indirect Esthetic Restorations. Available at: https://www.aegisdentalnetwork.com/id/2008/01/restorative-dentistry/treatment-planning-materials-tooth-reduction-and-margin-placement-for-anterior-indirect-esthetic-restorations. Accessed May 28, 2021.
- Church T, Jessup JP, Guillory V, Vandewalle K. Translucency and strength of high-translucency monolithic zirconium oxide materials. Gen Dent. 2017;65:48–52.
- Zarone F, Di Mauro M, Ausielli P, Ruggiero G, Sorrentino R. Current status on lithium disilicate and zirconia: a narrative review. BMC Oral Health. 2019;19:134.
- Materials Properties of Zirconia and Lithium Disilicate. Available at: https://creodental.com/materials-properties-of-zirconia-and-lithium-disilicate/. Accessed May 28, 2021.
The authors have no commercial conflicts of interest to disclose.
From Decisions in Dentistry. July 2021;7(7)12-15.


