
Early Interventions to Support Pediatric Oral Health
Managing caries risk and monitoring developing dentition are key elements of an effective preventive approach to treating young patients.
Caries is a behavioral disease, and this underscores the importance of regular dental care1 in order to adequately assess the risk for disease and mitigate that risk. The foundation of early childhood oral health is disease prevention and providing information to parents and caregivers about steps necessary to avoid issues stemming from caries, periodontal disease, growth and development disorders, and other oral and systemic disease manifestations.
For more than 20 years, the American Dental Association, American Academy of Pediatric Dentistry and American Academy of Pediatrics have recommended that a child’s first visit to the dentist should be no later than the first birthday. The purpose of this initial encounter is to establish a dental home, which provides a safe place for comprehensive care and allows clinicians to develop recommendations specific to that patient’s individualized risk. A major component of the first visit, for example, is an assessment of the developing dentition and occlusion. Examination of the child during subsequent visits must assess (at minimum):2
- Growth and development
- Soft tissues (extraoral and intraoral)
- Oral hygiene practices (patient and parent/caregiver)
- Dietary analysis3
- Fluoride exposure4
- The dentition itself
- Development and status of the occlusion
- Caries risk assessment
- Behavior of the child5–7 (essential to treatment)
- Trauma prevention
- Habits (nonnutritive)
- Counseling for speech and language development
CARIES RISK ASSESSMENT
Assessing caries risk8–12 and implementing preventive strategies are critical elements of pediatric care, particularly for preschoolers and children with special health care needs. A chief clinical objective is to identify caries risk factors and present an individualized plan to mitigate risk. While clinicians can choose from a variety of risk assessment tools, caries is dependent upon local factors, so effective biofilm removal is a cornerstone of disease prevention. Even so, when treating young patients, practitioners sometimes fail to spend adequate time assessing whether the parent/caregiver has the knowledge or ability to effectively clean the child’s teeth. Clinicians should offer instruction and observe as the adult cleans the teeth, as this affords an opportunity to provide corrective action, if needed.
If a child is deemed at high risk for caries, regular dental visits and ongoing risk assessment and management become even more critical. Unfortunately, the patients who need treatment the most are often the ones least likely to establish a dental home — which may stem from the parents’/caregivers’ lack of access, or lack of knowledge about the importance of oral health.
PROPHYLAXIS AND TOPICAL FLUORIDE
Perhaps one of the most recognized components of the infant (or any childhood) examination is the prophylaxis and subsequent application of topical fluoride. While these procedures are clinically advisable, they are not nearly as important as providing education to parents/caregivers about the need for effective oral hygiene. It is not possible to manage or control caries simply via twice-yearly dental visits. The parents/caregivers must be given the means to mitigate the child’s caries risk through self-care and healthy lifestyle choices, and by working with the dental team so interventions at appropriate intervals can verify whether the risk management regimen has been effective.
Topical fluoride treatment is generally provided in the form of fluoride varnish because of the increased concentration relative to formally delivered gels, and due to the higher safety index given the low volume applied. Additionally, fluoride varnish provides substantivity — and therefore longevity — in a greater way than gels have in the past. Although fluoride varnish is sometimes applied in physicians’ and pediatricians’ offices, and by public health or school-based programs, caries prevention should not be founded on random visits in various venues. Rather, fluoride varnish should be part of an overall preventive protocol based on the dental team’s assessment of the patient’s individualized risk.13
ANTICIPATORY GUIDANCE AND DIETARY COUNSELING
Anticipatory guidance is the part of care that examines all aspects of risk, predicts what may occur in the developmental stages that lie ahead (in the case of a child), and provides information so parents/caregivers can mitigate risks — partly because they know what is expected to occur prior to the next dental visit. These discussions should include dietary habits, oral hygiene, injury prevention, nonnutritive sucking habits, and similar issues.
When discussing an infant’s or toddler’s diet, oral hygiene or fluoride regimen with parents/caregivers, a key consideration for caries risk is the frequency of fermentable carbohydrate consumption. Most parents/caregivers do not fathom that the frequency of consumption plays a much greater role in allowing lesions to develop than the quantity consumed at a given time. Thus, clinicians need to ensure that parents/caregivers have a clear understanding of the impact of frequent fermentable carbohydrate consumption in caries progression.14
EARLY CHILDHOOD CARIES
Early childhood caries (ECC) is a specific condition that results in progressive disease of the primary dentition early in life (Figure 1). In most cases, it is entirely preventable. Rarely in the manifestation of ECC has an adequate preventive protocol been implemented in advance. On the contrary, there is often a lack of understanding among parents/caregivers of the importance of oral hygiene and other mitigating factors that would otherwise prevent caries. This condition often results in the need to treat children under general anesthesia — which is not only costly, but also entails a certain level of morbidity associated with the emotional and other aspects related to being treated in a hospital setting. Surgical intervention in the form of extensive restorations, pulp treatments and extractions (in some instances) are the only possible outcomes when ECC manifests in its most virulent form (Figure 2).5,15,16

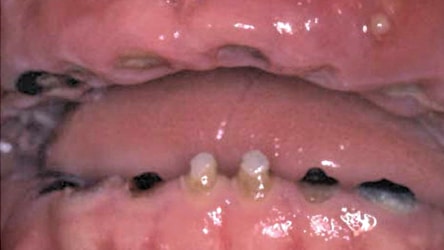
Beyond the cost of treatment, ECC poses significant risks to the child’s developing dentition; it can also affect speech, nutrition, learning, and have negative implications for quality of life that extend into adulthood.
MICROBIOME TREATMENTS
Scientific understanding of the oral microbiome is changing much about what is known concerning caries and its progression. Differences in the microbiota between individual patients — and interactions within the microbiome in each host — help determine caries risk and response to preventive and management protocols. Although it is still early in the “microbiome era,” ongoing advances in this area will likely bring positive and significant changes to therapeutic interventions.
Microbiome treatments in the form of various chemical solutions are being evaluated. For example, agents such as silver nitrate and silver diamine fluoride have been used to treat caries and avert lesion progression.1,17 In most instances, these treatments are effective in preventing the further development of lesions that have cavitated and where there is access to apply the agent. Treatments are less effective in areas where the agent cannot easily be delivered because the lesion is small or difficult to access. Consequently, clinicians must be attentive to the traditional means of using fluoride and similar remineralizing agents to mitigate the risk of developing lesions, and to reverse the course of action where possible.
New agents that are likely to be introduced in the future can be categorized in several ways:
- Treatments that might alter the biofilm and prevent acid production to prevent caries from forming initially
- Agents that prevent the formation of pathogenic biofilm
- Therapies that identify early lesions and halt their progression through remineralization or other means of altering the onset of caries
FUTURE DIRECTIONS
It is clear that the recommendations made decades ago to promote early childhood oral health by establishing a dental home before the first birthday, and providing education and preventive interventions, are crucial components of effective care. Now, as then, dental professionals play a pivotal role by assessing and monitoring the individualized risk of each pediatric patient, and applying the latest evidence-based approaches to disease prevention and treatment.18
Effective care requires a constant review the literature, ongoing assessment of the rapidly evolving understanding of the oral microbiome and its effect on caries progression, and implementing management protocols as early as possible. Beyond the clinic, however, it is equally important for dental teams to provide parents/caregivers with the knowledge and skills to make appropriate dietary and lifestyle choices for their children, while ensuring proper oral hygiene and regular dental visits. It is only through these combined efforts that oral disease can be prevented.
KEY TAKEAWAYS
- Establishing a dental home before a child’s first birthday ensures a safe place for comprehensive care and allows clinicians to develop recommendations specific to that
patient’s individualized risk. - Assessing caries risk8–12 and implementing preventive strategies are critical elements of pediatric care, particularly for preschoolers and children with special
health care needs. - Parents and caregivers must be given the means to mitigate the child’s caries risk through effective self-care and healthy lifestyle choices, and by working with dental
teams to verify whether the risk management regimen has been effective. - It is only through the combined efforts of dental professionals and parents/caregivers that oral disease can be prevented.
REFERENCES
- Berg J. Medical management of dental caries. J Calif Dent Assoc. 2014;42:442–447.
- Lai B, Tan WK, Lu QS. Clinical efficacy of a two-year oral health programme for infants and toddlers in Singapore. Singapore Med J. May 25, 2017. Epub ahead of print.
- Wright R, Casamassimo PS. Assessing attitudes and actions of pediatric dentists toward childhood obesity and sugar-sweetened beverages. J Public Health Dent. 2017;77(Suppl 1):S79–S87.
- Garcia RI, Gregorich SE, Ramos-Gomez F, et al. Absence of fluoride varnish-related adverse events in caries prevention trials in young children, United States. Prev Chronic Dis. 2017;14:E17.
- Braun PA, Widmer-Racich K, Sevick C, Starzyk EJ, Mauritson K, Hambidge SJ. Effectiveness on early childhood caries of an oral health promotion program for medical providers. Am J Public Health. 2017;107(Suppl 1):S97–S103.
- Edelstein BL. Pediatric dental-focused interprofessional interventions: rethinking early childhood oral health management. Dent Clin North Am. 2017;61:589–606.
- Sigaud CH, Santos BR, Costa P, Toriyama AT. Promoting oral care in the preschool child: effects of a playful learning intervention. Rev Bras Enferm. 2017;70:519–525.
- Kraljevic I, Filippi C, Filippi A. Risk indicators of early childhood caries (ECC) in children with high treatment needs. Swiss Dent J. 2017;127:398–410.
- Caleza-Jimenez C, Yañez-Vico R, Mendoza-Mendoza A, Palma JC, Iglesias-Linares A. Impact of delayed gratification on oral health and caries status in the primary dentition. J Dent. 2017; 63:103–108.
- Kakanur M, Nayak M, Patil SS, Thakur R, Paul ST, Tewathia N. Exploring the multitude of risk factors associated with early childhood caries. Indian J Dent Res. 2017;28:27–32.
- Fernandes IB, Pereira TS, Souza DS, Ramos-Jorge J, Marques LS, Ramos-Jorge ML. Severity of dental caries and quality of life for toddlers and their families. Pediatr Dent. 2017;39:118–123.
- Farsi NJ, El-Housseiny AA, Farsi DJ, Farsi NM. Validation of the Arabic version of the early childhood oral health impact scale (ECOHIS). BMC Oral Health. 2017;17:60.
- Croll TP, Berg JH. Use of fluoride products for young patients at high risk of dental caries. Compend Contin Educ Dent. 2014;35:602–606.
- Childers NK, Momeni SS, Whiddon J, et al. Association between early childhood caries and colonization with Streptococcus mutans genotypes from mothers. Pediatr Dent. 2017;39:130–135.
- Cidro J, Maar M, Peressini S, et al. Strategies for meaningful engagement between community-based health researchers and first nations participants. Front Public Health. 2017;5:138.
- Valdez RM, Duque C, Caiaffa KS, et al. Genotypic diversity and phenotypic traits of Streptococcus mutans isolates and their relation to severity of early childhood caries. BMC Oral Health. 2017;17:115.
- Nelson T, Scott JM, Crystal YO, Berg JH, Milgrom P. Silver diamine fluoride in pediatric dentistry training programs: survey of graduate program directors. Pediatr Dent. 2016;38:212–217.
- Berg JH, Stapleton FB. Physician and dentist: new initiatives to jointly mitigate early childhood oral disease. Clin Pediatr (Phila). 2012;51:531–537.
The author has no commercial conflicts of interest to disclose.
Featured Image by DANIELA JOVANOVSKA-HRISTOVSKA/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. September 2017;3(9):22, 24, 26.


