 ROSSHELEN/ISTOCK/GETTY IMAGES PLUS
ROSSHELEN/ISTOCK/GETTY IMAGES PLUS
Developments in Modern Endodontics
Yaara Berdan, DDS, provides insights into advances in endodontic therapy and today’s thinking about the armamentarium available for root canal treatment.
Advances in technology are contributing to more predictable outcomes in endodontic therapy. From developments in endodontic instruments to improved visualization that aids diagnosis and treatment, today’s clinicians can harness a powerful armamentarium that supports optimal care. To gain a better understanding of today’s clinical options and how they factor into treatment, we asked YAARA BERDAN, DDS, director of predoctoral endodontics for the Herman Ostrow School of Dentistry at the University of Southern California, for insights into the state of today’s endodontic care.
The advent of new tools and technologies for endodontic therapy has contributed to more predictable outcomes. Please briefly recap some of the more notable advances that help support improved care.
A major advance was introduction of nickel-titanium instruments, as this resulted in improved root canal preparation by both endodontists and general dentists. These files’ flexibility, combined with unique blade and taper designs, allow for improved shaping of root canal systems while minimizing procedural errors.
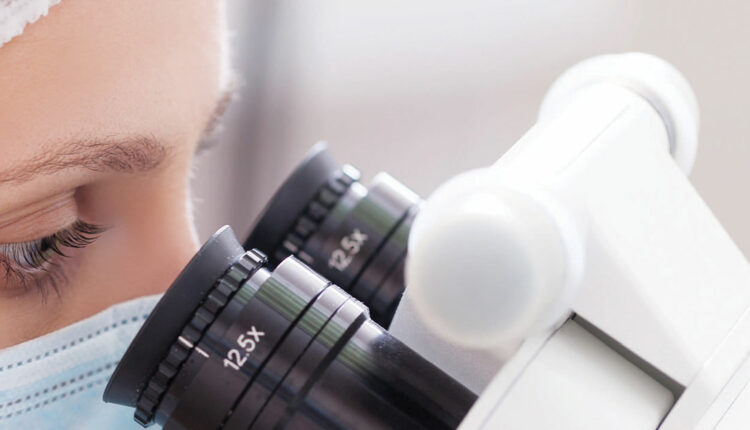
Enhanced visualization is critical to successful outcomes, and the dental/surgical operating microscope greatly enhances magnification and illumination of the operating field. It increases the clinician’s ability to visualize details, such as the anatomy of the pulp chamber floor, location of canals, and fractures or cracks along the dentinal walls and pulp chamber. The surgical microscope is also a significant help when removing foreign objects from the root canal, and it facilitates the use of ultrasonics for both orthograde and surgical endodontics.
Electronic apex locators have evolved and now provide accurate and reliable readings of root canal length. Together with radiography, working length can be determined in a predictable manner. The use of an electronic apex locator also reduces the number of radiographs needed for treatment, thereby reducing radiation exposure and treatment time.
Cone beam computed tomography (CBCT) is a significant breakthrough in endodontic therapy. It allows the visualization of the third dimension, aiding in the diagnosis of pathoses, differential diagnosis, treatment decision-making, assessment of root canal anatomy, endodontic retreatment and endodontic microsurgery. Utilization of CBCT imaging greatly enhances the endodontist’s ability to diagnose, evaluate and treat — which, in turn, supports improved patient care.
Finally, regenerative endodontics allows immature necrotic teeth to continue to develop. This cutting-edge approach uses the concept of tissue engineering to retain teeth that otherwise would have been candidates for extraction.
While important to endodontic therapy, radiographs are only one facet of the diagnostic and treatment processes. What are the value and limitations of radiographs in endodontics?
A conventional radiograph is a two-dimensional image of a three-dimensional structure. While a powerful diagnostic tool in endodontics, the final diagnosis should not be based on radiographs alone. Pathoses may go undetected when the cortical bone has not yet been affected; in addition, the full extent of resorptive lesions may be difficult to evaluate. Another key consideration is that pulp status cannot be determined radiographically; it is not apparent solely from the radiograph whether the pulp is normal, inflamed or necrotic. Misinterpretations may also occur due to image distortion, such as elongation or foreshortening. Therefore, radiographic interpretation should always be combined with patient assessment and careful clinical examinations.
Please discuss the importance of case selection, especially for general practitioners who may elect to refer some patients to endodontists.
One of the primary determinants of successful outcomes is case selection. Although a high proportion of endodontic treatment is provided appropriately by general dentists, when difficulties or risks are identified, it is in the best interest of the patient and dentist to refer to a specialist. There are many factors that influence the degree of difficulty and risk of endodontic treatment. The American Association of Endodontists’ Case Difficulty Form provides an objective assessment of the level of difficulty and associated risks with treatment. Recognition of these factors prior to the initiation of treatment will help support optimal outcomes. Referral before treatment begins is much better than after a procedural problem has occurred, because the prognosis for the tooth may be compromised by the procedural error and correction may be difficult or impossible.
The decision to refer is based on the provider’s skill and experience. A dentist should not undertake treatment unless he or she is prepared to manage the extent of pathology in the root canal system and any complications that may arise from treatment. A good principle to follow is to consider what you would do for a friend or family member: refer or treat.
In light of the overuse and abuse of opioids, what is the current thinking regarding pain management and medications for endodontic procedures?
Nonsteroidal anti-inflammatory drugs (NSAIDS) are usually the medicament of choice when treating pain of endodontic origin due to the inflammatory etiology of the pain. Understanding the cause enables clinicians to treat pain appropriately. Studies have shown that 800 mg of ibuprofen is more effective than Percocet in managing endodontic pain. This is not surprising, as Percocet has no anti-inflammatory properties.
Some patients cannot tolerate NSAIDS, however. If acetaminophen alone is not effective, tramadol or the addition of a narcotic to acetaminophen is usually effective for pain management. Another sound strategy is combining acetaminophen and ibuprofen. This combination has a synergistic effect and is extremely effective for pain management.
Pain of endodontic origin usually subsides after three to five days if the source of the inflammation is addressed (e.g., initiation of root canal therapy). If the patient still requires high doses of analgesics for pain control, the patient should be reevaluated to verify that healing is progressing normally and there is no other cause for the pain.
Patients present with different sets of symptoms and medical considerations. Pain management is a necessary and compassionate element of care, and all patients deserve a personalized approach addressing their specific needs. When narcotics are necessary to control pain, a three- to five-day supply should be sufficient. Narcotics should be used judiciously and not as the first line of treatment, however, as there are much more effective pain medications that carry less risk.
What is the modern approach to working length, and when should it be established? What role do electronic apex locators play in this part of treatment?
Working length should be established after the coronal portion of the root canal has been prepared. This will result in less chance of a change in the working length and easier access to the apical portion of the canal — and with less probability for errors. In more curved canals, working length may need to be established after a more significant portion of the canal has been shaped. This is due to slight straightening of the canal as shaping takes places.
Electronic apex locators play an important role when determining working length. The combined use of electronic apex locators and radiographs will result in greater accuracy. This approach will also provide essential information about tooth anatomy, canal morphology, additional canals, missed canals or procedural errors.
How important is the use of CBCT to successful endodontic treatment?
As noted, CBCT is transforming clinicians’ ability to improve patient care by facilitating treatment planning and outcome assessment. Although its use should be considered on a case-by-case basis, it has been critical in many cases of retreatment or endodontic microsurgery. In addition, it can help solve challenging diagnostic cases or assist in treatment of complex morphology. It is used routinely for presurgical treatment planning, and allows for detailed evaluation of the extension of periapical lesions and localization of root apex/apices and their proximity to adjacent anatomical structures. The use of CBCT is also recommended for evaluation of traumatic injuries and localization and differentiation of fractures and resorptive defects.
Together with additional developments in the armamentarium, the use of advanced technologies such as CBCT — along with careful case selection — will support successful endodontic outcomes.
From Decisions in Dentistry. July/August 2019;5(7):48–50,.


