 ALEKSANDARGEORGIEV / E+ / GETTY IMAGES PLUS
ALEKSANDARGEORGIEV / E+ / GETTY IMAGES PLUS
Developments in Dental Magnification Technologies
An examination of advances in magnification that may prompt clinicians to upgrade their current setups.
Because the mouth is a confined and narrow space, and much dental treatment is irreversible, dentistry is a visually demanding profession. General dentists need optimal visual acuity to evaluate intra- and extraoral tissues for disease, conduct thorough periodontal assessments, and perform restorative procedures and other clinical tasks. Whether in general or specialty practice, the use of magnification enhances clinicians’ ability to ensure proper decision-making in regard to diagnosis and treatment planning. While providing care, magnification also helps dental professionals maintain a neutral posture that decreases eyestrain and preserves musculoskeletal health.1–4
Although many general and specialty dentists already utilize some type of magnification, not all give due consideration to when it is time to upgrade their current magnification system. This article will examine factors related to visual acuity and musculoskeletal health, and explore developments in magnification that may prompt providers to consider upgrading this helpful adjunct to clinical practice.
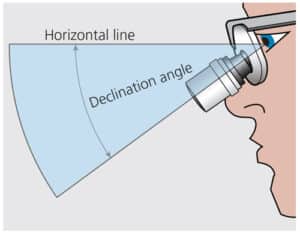
Loupes are the most widely used magnification system among dental professionals and must be properly fitted in order for operators to work ergonomically and efficiently. In addition to working distance, depth of field and coaxial alignment, declination angle is a crucial factor to consider when fitting loupes to the dentist and his or her line of vision.5–7
Declination angle is the downward angle between the support line connecting the loupe earpiece to the clinician’s head (specifically, the corner of the eyes) and the individual’s line of sight (Figure 1).5 The steeper the declination angle, the less a clinician has to tilt his or her head. An ideal declination angle for dentists is ≥ 40o; unfortunately, many early through-the-lens loupes could not attain a declination angle greater than 30˚.
Inadequate declination angle increases eye, head, back and neck strain. Moreover, it may cause loupes to be out of coaxial alignment, further contributing to visual deviations and musculoskeletal issues.8 It is recommended that dental professionals reassess their current magnification systems to ensure an adequate declination angle, as newer ergonomic loupes provide up to a 55˚ declination angle.
CONSIDERATIONS WHEN UPGRADING LOUPES
With proper maintenance and care, loupes may last for the duration of a dentist’s career. However, operators should not ignore signs and symptoms that may indicate the need for a magnification upgrade. Proper magnification promotes ergonomics while preventing eyestrain, fatigue and musculoskeletal issues.9 The higher the magnification, the smaller the field of view. Thus, the lowest-needed magnification is recommended for first-time loupes users. This is typically a 2.5X magnification. As visual acuity changes over time, the dentist may lean closer to the patient, causing musculoskeletal stress, especially in the neck and back. Increased pain is a good indication the magnification in an existing set of loupes may not be strong enough.
Today’s dental offices are widely incorporating digital technology. Digital eyestrain is more prevalent with these modernizations and can lead to blurred vision and headaches.4 These are additional signs the current loupe magnification may no longer be adequate.
The American Optometric Association recommends adults age 18 to 64 have their eyes examined at least every two years, with annual exams for those age 65 and older.9 If there is a change in the clinician’s eye prescription, loupe measurements should be reassessed to ensure optimal visual acuity and proper ergonomics. Any visual changes or unclear optics, such as the blurring of viewed structures, especially the edges of teeth, may also warrant a magnification update.
A 2020 survey revealed U.S. dentists found magnification to be a significant technological advancement in the provision of care.10 Despite this, some are still apprehensive to utilize loupes. Clinicians report one of the disadvantages to wearing loupes is fixed magnification.11 Dentists often complete procedures needing various magnification levels and may not have the time or ability to switch between various loupes. To address these concerns, the industry has created a three-in-one variable-magnification loupe that allows operators to easily switch between 3x, 4x and 5x magnification. A potential downside to this design is its additional weight, which may increase pressure on the nasal bridge, temples and neck, possibly contributing to neck and back pain.3
The average age of a working dentist in 2020 was 49.3, while the average age of retirement was 68.2.12 Since many providers are practicing longer, ergonomic health has become an even greater concern as clinicians rely on musculoskeletal health to prolong their careers.1,3,13 Dentists often experience neck pain while wearing loupes because many still operate at an inadequate declination angle and with their neck held at angles of 20˚ to 30˚.14
Loupe manufactures are now offering more ergonomic options to improve musculoskeletal health while providing the needed optical tools for restorative and surgical treatment. Ergonomic loupes help clinicians maintain a head tilt of less than 20˚, which enables the spine to remain properly aligned. Modern lightweight ergonomic loupes are designed to allow operators to have a 0˚ tilt, meaning the chin is up, the neck is straight, and the eyes are forward. This helps users maintain a steeper declination angle and upright positioning while viewing the oral cavity. Such loupes are offered in various magnification levels and some manufactures even provide ergo-fit nose pads to match facial features for added comfort.
INFECTION CONTROL IN MAGNIFICATION
The SARS-CoV-2 virus has escalated clinicians’ concerns regarding dental aerosols and infection prevention protocols. Dentists are now looking for ways to incorporate high-level eye protection while having the ability to use magnification and maintain visual acuity. To address this issue, operators can now choose aerosol-protection loupes fitted with silicone eyecups that help prevent transmission from aerosols and spatter. The eyecups provide a protective seal around the orbit and are removable for disinfection purposes.
In addition to protective eyewear, federal guidelines suggest the use of a face shield.15 Fortunately, a variety of easily accessible face shields fit over a clinician’s loupe-and-light systems. Certain shields fully cover the face and have an optional cutout allowing the clinician’s light to pass through the shield. The cutout decreases the amount of heat created by the light.
ADVANCES IN HEADLIGHTS AND LASER EYE PROTECTION
Along with loupes, the use of LED coaxial illumination further aids the dental professional’s ability to work in the dark, cramped confines of the oral cavity. Coaxial illumination may aid caries detection while still allowing operators to maintain a neutral posture.16 Initially, many headlights were corded and heavy. In the height of the SARS-CoV-2 pandemic, cross-contamination was a heightened concern as dentists had to manually turn their headlights on and off. Manufactures now offer touch-free headlights activated by the clinician’s head movement to eliminate this cross-contamination risk. These touchless light systems clip into the loupes and do not have a heavy cord or battery pack to wear. Instead, they come with three power pods and a charging unit. Newer headlight technology also uses color-neutral LED lights that emit the lowest blue light for eye protection and unsurpassed color accuracy.
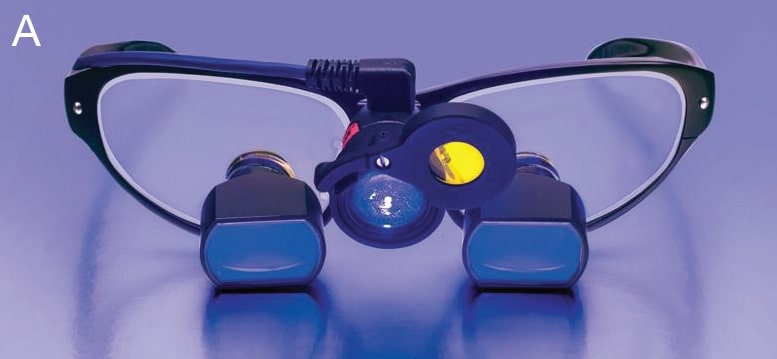
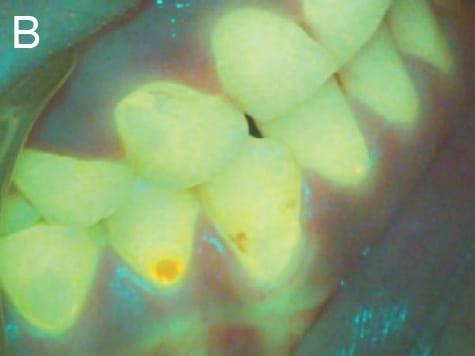
A recent advance in dental illumination is the use of fluorescence activating headlights. When combined with filtered loupes, these headlights help support minimally invasive restorative treatment by allowing clinicians to actively visualize and differentiate diseased and non-diseased tooth tissue (Figure 2A).17 In addition, the hands-free system allows dentists to easily identify resin degradation, enamel demineralization and bacterial contamination, detect supra- and subgingival calculus, and identify accumulations of active periodontal bacteria around teeth and implants (Figure 2B).17 Also available are wireless integrated multiwavelength LED headlights that allow operators to easily switch between daylight, violet light and fluorescent illumination.
With increased use of hard and soft tissue laser procedures in both general and specialized dental practice, maintaining appropriate laser eye protection while using necessary magnification is a valid concern. Manufacturers provide shield inserts compatible with most dental loupes. These protection filters are available for curing filter wavelengths, as well. The shields slip securely behind the clinician’s loupes and are easier to use than traditional laser protective goggles or clip-in filters.
DENTAL OPERATING MICROSCOPES
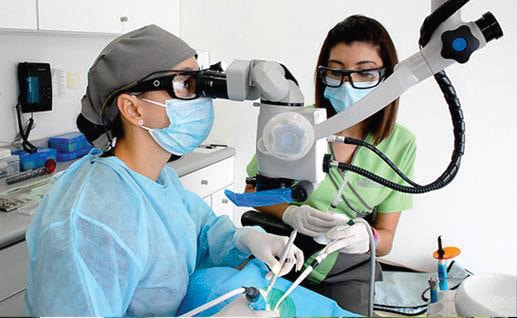
As noted, advances in loupes and headlights offer dentists more options for providing optimal care while maintaining musculoskeletal health. However, limitations still exist — including a lack of fixed position and magnification power. Additionally, even though many loupes and light systems are now lightweight, any added weight to the head throughout the day can contribute to neck and back pain.11 As a result, the dental operating microscope (DOM) is becoming more popular with general dentists and periodontists, as it addresses many of the existing limitations (Figure 3).
Since its introduction, the DOM has primarily been used by endodontists.18 This technology allows clinicians to utilize multiple magnification levels while maintaining the appropriate amount of shadow-free illumination needed for higher magnifications. It also limits the need for clinicians to adjust their posture.11 The illumination is superior to a headlight because the coaxial path of light is parallel to the path of vison.11 In addition, the DOM supports optimal working posture. The clinician is measured seated in an ideal ergonomic position, referred to as the home position; therefore, unlike loupes, the clinician is automatically seated at an upright position prior to and during treatment.19
Dentists claim to have less eyestrain and an overall decrease in musculoskeletal stress while using the DOM.11 Another benefit is its ability to take photos and videos during procedures with the use of a beam splitter. This capability improves patient/provider communication and results in greater treatment acceptance rates. The video stream also facilitates efficiency in four-handed dentistry.11 Because of the superior magnification and illumination of DOMs, dentists are able to perform procedures with greater precision.11
In addition to a beam splitter, accessory upgrades make the DOM even more effective. These include binocular extenders and rotation rings, curing light and laser filters, and multifocal lenses for offices that have more than one operator.11 Disadvantages include cost, the size of the device, and the associated learning curve.
SUMMARY
Ongoing advances in magnification and illumination will continue to support ergonomic practice, which, in turn, helps clinicians extend their careers. Today’s technologies enhance visual acuity, enabling dentists to diagnose, plan and provide optimal treatment. The result is increased productivity and greater patient satisfaction.
Due to improvements in magnification, coupled with vision changes that are part of the aging process, oral health professionals are encouraged to evaluate their current magnification aids at least every two years to determine if an upgrade may be advantageous to their health and productivity.
KEY TAKEAWAYS
- Due to improvements in magnification, coupled with vision changes that are part of the aging process, oral health professionals are encouraged to evaluate their current magnification aids at least every two years to determine if an upgrade may be advantageous.
- The use of magnification enhances clinicians’ ability during diagnosis and treatment planning.
- Magnification also helps dental professionals maintain a neutral posture in clinical practice, which decreases eyestrain and supports musculoskeletal health.1–4
- Newer headlight technology uses color-neutral LED lights that emit the lowest blue light for eye protection and unsurpassed color accuracy.
- A recent advance in dental illumination is the use of fluorescence activating headlights.
REFERENCES
- Arnett M, Eagle I. Enhance vision and ergonomics with loupes and lights. Decisions in Dentistry. 2021;7(12):22–24.
- Arnett MC, Gwozdek AE, Ahmed S, Beaubien HD, Yaw KB, Eagle IT. Assessing the use of loupes and lights in dental hygiene educational programs. J Dent Hyg. 2017;91:15–20.
- Lietz J, Ulusoy N, Nienhaus A. Prevention of musculoskeletal diseases and pain among dental professionals through ergonomic interventions: a systematic literature review. Int J Environ Res Public Health. 2020;17:3482.
- Auffret É, Gomart G, Bourcier T, Gaucher D, Speeg-Schatz C, Sauer A. Digital eye strain. Symptoms, prevalence, pathophysiology, and management. J Fr Ophtalmol. 2021;44:1605–1610.
- Rucker LM, Beattie C, McGregor C, Sunell S, Ito Y. Declination angle and its role in selecting surgical telescopes. J Am Dent Assoc. 1999;130:1096–1100.
- Valachi B. Neck health: the three ergonomic criteria for loupes selection. Available at: dentaleconomics.c/m/articles/print/volume-98/issue-9/columns/preventing-pain-in-dentistry/neck-health-the-three-ergonomic-criteria-for-loupes-selection.html. Accessed September 6, 2022.
- Wen WM. An investigation in the prevalence of co-axial misalignment of surgical loupes amongst BC dental professionals. Available at: open.library.ubc.ca/cIRcle/collections/ubctheses/葤/items/䁯.0228864. Accessed September 6, 2022.
- Wen W, Zul K, Laronde D, et al. Out of the loupe: The prevalence of coaxial misalignment of surgical loupes among dental professionals. J Am Dent Assoc. 2019;150:49–57.
- American Optometric Association. Comprehensive Eye Exams. Available at: https://www.aoa.org/healthy-eyes/caring-for-your-eyes/eye-exams?sso=y. Accessed September 6, 2022.
- Heft MW, Fox CH, Duncan RP. Assessing the translation of research and innovation into dental practice. JDR Clin Trans Res. 2020;5:262–270.
- Bud M, Jitaru S, Lucaciu O, et al. The advantages of the dental operative microscope in restorative dentistry. Med Pharm Rep. 2021;94:22–27.
- American Dental Association. The dentist workforce. Available at: https://www.ada.org/resources/research/health-policy-institute/dentist-workforce. Accessed September 6, 2022.
- Roll SC, Tung KD, Chang H, et al. Prevention and rehabilitation of musculoskeletal disorders in oral health care professionals: A systematic review. J Am Dent Assoc. 2019;150:489–502.
- Marklin RW, Cherney K. Working postures of dentists and dental hygienists. J Calif Dent Assoc. 2005;33:133–136.
- U.S. Department of Labor. Occupational Safety and Health Administration. Dentistry workers and employers. Available at: https://www.osha.gov/coronavirus/control-prevention/dentistry#:~:text=OSHA%20recommends%20using%20a%20combination,areas%20with%20ongoing%20community%20transmission. Accessed September 6, 2022.
- Ari T, Ari N. The performance of ICDAS-II using low-powered magnification with light-emitting diode headlight and alternating current impedance spectroscopy device for detection of occlusal caries on primary molars. ISRN Dent. 2013;2013:276070.
- Steier L, Figueiredo JAP, Blatz MB. Fluorescence-enhanced theragnosis: a novel approach to visualize, detect, and remove caries. Compend Contin Educ Dent. 2021;42:460–465.
- Gutmann JL. historical perspectives on the use of microscopes in dentistry. J Hist Dent. 2017;65:20–27.
- Javed F, Habib S, Ghafoor R. Surgical endodontics under the microscope: Principles and practice. Dent Update. 2022;49:416–422.
From Decisions in Dentistry. October 2022;8(10):8,10,13.


