 GREGORYDEAN/ISTOCK/GETTY IMAGES PLUS
GREGORYDEAN/ISTOCK/GETTY IMAGES PLUS
Caring for Children With Trisomy 21 in The Dental Setting
Treating pediatric patients with the chromosomal disorder trisomy 21 requires a thorough understanding of the condition and its implications for oral disease and dental care.
This course was published in the September 2019 issue and expires September 2022. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the prevalence of trisomy 21 in pediatric patients and the etiologies of this chromosomal disorder.
- Identify common presenting features of trisomy 21.
- Explain dental treatment strategies when caring for this patient population.
Trisomy 21, or Down syndrome, is the most common chromosomal disorder, affecting approximately one in 700 live births.1 It is characterized by an extra copy of chromosome 21, usually due to nondisjunction of the chromosome, resulting in physical and developmental disabilities. According to estimates, more than 250,000 Americans live with trisomy 21,2 and between 1979 and 2003, there was more than a 30% increase in the number of babies born with the disorder.3 Additionally, survival rates have improved over the last several decades.4,5 Due to the relatively large population of affected individuals and high frequence of occurrence (compared with other chromosomal disorders), there is an increasing need for dental providers to care for these patients. Many children with trisomy 21 can be seen in private dental settings for routine care — but in order to provide safe and effective treatment, clinicians should possess a thorough understanding of the patient’s condition.
Nondisjunction of chromosome 21 can occur in multiple ways. Most commonly, it happens on the maternal or paternal side during meiosis; however, most cases occur from the maternal chromosome set.6 Increasing maternal age is a known risk factor for nondisjunction.7 Trisomy 21 can also occur from other genetic abnormalities. For example, up to 5% of individuals with trisomy 21 have a rare form due to mosaicism, where some cells in the body have a normal chromosomal makeup, and a percentage of cells has the extra 21st chromosome.8 This happens due to abnormal cell division after fertilization. A third rare form, seen in up to 4% of affected individuals, occurs when a segment of chromosome 21 is transferred and attached to another chromosome, which is inherited along with two normal copies of chromosome 21.9 Because translocation trisomy 21 can be inherited from a parent with the translocation, families who have children with this form of trisomy 21 are at risk of passing on the abnormality in future pregnancies.9
Prenatal screening has become a routine step in diagnosing trisomy 21. The emergence of advanced, less-invasive screening techniques has led to relatively high specificity and sensitivity when screening for trisomy 21 during pregnancy.10 With the discovery of cell-free fetal DNA circulating in maternal plasma, it is now possible to screen with a false positive rate of 0.3%, compared with a false positive rate of 3.6% in standard serum biochemical assay screening.11 This screening, along with traditional screening techniques — such as amniocentesis and chorionic villus sampling — offer valuable early diagnostic tools for families.12
COMMON CHARACTERISTICS
Typical features of trisomy 21 include upslanted eyes with prominent epicanthal folds, a small chin and head, flat nasal bridge, single deep crease in the palms, Brushfield spots (small pale spots in the iris of the eyes), and hypotonia.13 This disorder is also characterized by mild to moderate levels of cognitive impairment, and, in some instances, severe impairment. The severity of symptoms and clinical manifestations vary, particularly in mosaic trisomy 21, as the extent of the manifestations depends on the proportion of abnormal to normal cells in the body.
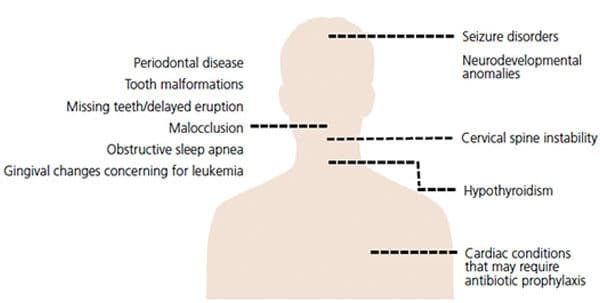
Children with trisomy 21 are at risk of other comorbidities as well (Figure 1), some of which can be fatal. For example, nearly 50% of these children are also born with congenital heart defects, most commonly atrioventricular septal defects, atrial septal defects and ventricular septal defects.14 Mortality from congenital heart defects has decreased over the years, in part due to early intervention and advancing surgical techniques — but they are still a major cause of death.14,15 Additionally, children with trisomy 21 face increased risk for developing leukemia; consequently, they must be carefully followed as they grow.16,17 Many also have some degree of hearing loss or chronic otitis media.18 This can be treated early on with interventions, such as ear tube placements.19,20 Other common comorbidities include eye disease, thyroid disease, epilepsy and obstructive sleep apnea (OSA).13,21
Trisomy 21 also presents with common orofacial findings. These include large, fissured lips, macroglossia, and a narrow, vaulted palate, which can contribute to OSA, as well as a heightened gag reflex. These patients may also have malocclusion related to an underdeveloped midface, resulting in a Class III appearance, as well as delayed eruption, congenitally missing teeth or malformations of the teeth, including conical shapes, hypoplasia and microdontia.22,23
MEDICAL CONSIDERATIONS IN ORAL HEALTH CARE
It is important for oral health professionals to account for systemic health considerations when treating a child with trisomy 21, starting with maintaining a diligent health record and coordinating consults among specialists when warranted. In children who have congenital heart defects or have had recent cardiac surgeries, dental providers should verify any current cardiac concerns, and confirm with the child’s cardiologist if antibiotic prophylaxis is recommended as a preventive measure against bacteremia-induced infective endocarditis. Of note, the American Heart Association recommends a move away from antibiotic prophylaxis for at-risk children in the dental setting, and an increasing emphasis on maintaining proper oral hygiene and oral disease prevention.24
Compared to the general population, children with trisomy 21 are at a greater risk for cervical spine instability (also known as atlantoaxial instability). This is an abnormality of the junction between the cervical vertebrae — the atlas (C1) and axis (C2) — that results in excessive mobility at the articulation of the two vertebrae. Cervical spine instability affects between 10% to 30% of children with trisomy 21.21 Most children who have the congenital abnormality, however, are asymptomatic.25 Because hyperextension or radical flexion of the hypermobile joint can result in spinal compression and neurologic injury, children with trisomy 21 may have imaging to screen for cervical spine instability, particularly if they wish to participate in sports.
Dental health care providers should be aware of any medical concerns for cervical spine instability in patients with trisomy 21, especially when considering restraint or protective stabilization for young or potentially uncooperative children during treatment. Prior to using protective stabilization, dental teams should confirm if a child’s cervical spine has been evaluated. For patients with cervical spine instability, parents and caregivers may offer valuable insight into best practices to protect the child’s spine in these situations, including utilization of pillows and management of body positioning in the dental chair.
Due to an association between trisomy 21 and hypothyroidism, many affected children are followed regularly by a pediatric endocrinologist.26,27 The American Academy of Pediatrics Committee on Genetics recommends annual thyroid screenings into adulthood for children with trisomy 21.28 If thyroid dysfunction is uncontrolled or poorly managed, practitioners should be aware of the risks of hypothyroidism-induced low blood pressure, cardiac output, and respiratory rate in the dental setting.
It is estimated that up to 13% of children with trisomy 21 also have some form of seizure disorder.29 These can vary in type and severity, and may have a neurodevelopmental effect in the growing child.30 Having a discussion with the child’s parent/caregiver regarding how a typical seizure presents, as well as their established seizure protocol, provides crucial information for clinicians in the event of seizure activity in the dental office.
OROFACIAL CONSIDERATIONS
Children with trisomy 21 can present with dental needs complicated by the physical manifestations of the chromosomal abnormality. Because these children often have some degree of developmental delay, they may have poor motor skills, resulting in an inability to brush their teeth effectively, and may be unable to chew and cleanse food from the mouth with their tongue due to generalized hypotonia. While they are still generally at lower risk for caries than individuals without trisomy 21, these children are at higher risk of developing periodontal disease.31 This may be due to generalized immunodeficiencies, malocclusion, malformed dentition, and high numbers of periodontal pathogens in their oral microbiome.32 Among this population, between 58% and 96% of patients younger than 35 have some degree of periodontal disease.33 Early intervention is important, and it can be beneficial to appoint these patients for more frequent recalls and utilize chemical adjuvants, such as chlorhexidine rinses, to improve periodontal therapeutic outcomes.34
Parents/caregivers often have questions regarding the way their child’s teeth look, as well as how they are positioned, as the adult may associate malocclusions with a negative outlook of the child’s oral health.35 Encouraging parents/caregivers to bring the child in for routine recalls as early as possible creates opportunities to provide anticipatory guidance to families. This includes discussing the possibility of missing or malformed teeth, crowding, delayed eruption and malocclusion as the child develops. Obtaining a panoramic radiograph once the child is mature enough can aid confirmation and observation of dental anomalies, and facilitate any discussions about possible orthodontic interventions.36
Craniofacial abnormalities associated with trisomy 21 play a significant role in the high prevalence of OSA in these patients. It is estimated that up to 70% of children with trisomy 21 also have OSA37 — and midface hypoplasia, macroglossia, a high and narrow palate, narrow nasopharynx and generalized hypotonia are all contributing factors. Children diagnosed with OSA are at risk of negative neurodevelopmental consequences, regardless of having a chromosomal abnormality or not.38 While utilization of continuous positive airway pressure devices to aid in treating OSA can be highly effective, it can also increase the risk of xerostomia. In light of the typical mouth-breathing habits seen in these patients and potential intake of xerostomia-inducing medications, it is important to evaluate children with trisomy 21 for adequate salivary flow to help reduce caries risk. Encouraging parents/caregivers to provide ample fluoridated water and utilize fluoridated products can help alleviate this concern.
Due to the relatively high risk of leukemia in children with trisomy 21, clinicians should also maintain awareness of common oral manifestations of leukemia and be vigilant in screening for potential symptoms in this population. The most common early manifestations of leukemia include spontaneous gingival hemorrhaging and gingival enlargement;39,40 however, this can be complicated by poor oral hygiene and other periodontal concerns in the trisomy 21 population.
ORAL HEALTH PROFESSIONALS AS ADVOCATES
Children with special needs can present challenges when providing routine dental care. Having a detailed appreciation of each child’s unique medical and orofacial considerations can help clinicians provide optimized care for children with trisomy 21. Some children may need protective stabilization to safely conduct an examination, or patients may have extensive dental needs requiring comprehensive care in a hospital setting. Others may have sensory and cognitive difficulties, resulting in challenges in tolerating dental prophylaxis and treatment, managing the gag reflex or taking dental radiographs. Yet, many of these children can eventually succeed in any environment when given the opportunity, enough time and proper encouragement.
Most children with trisomy 21 can learn to cooperate in the dental office. Behavior management techniques, such as desensitization, the tell-show-do approach, and positive reinforcement, can improve behavioral outcomes and encourage patients to practice good oral hygiene at home.23 Combined with early intervention and education involving their families and caregivers, it is possible for children with trisomy 21 to maintain a healthy dentition, as well as a positive outlook on dental care. By devoting the time and effort to work with these patients to discover their motivators, stressors, and behavioral boundaries, dental teams can establish long-lasting relationships with these children and provide a dental home for their special health care needs.
REFERENCES
- Canfield MA, Honein MA, Yuskiv N, et al. National estimates and race/ethnic-specific variation of selected birth defects in the United States, 1999–2001. Birth Defects Res A Clin Mol Teratol. 2006;76:747–756.
- Presson AP, Partyka G, Jensen KM, et al. Current estimate of Down syndrome population prevalence in the United States. J Pediatr. 2013;163:1163–1168.
- Shin M, Besser LM, Kucik JE, et al. Prevalence of Down syndrome among children and adolescents in 10 regions of the United States. Pediatrics. 2009;124:1565–1571.
- Kucik JE, Shin M, Siffel C, Marengo L, Correa A, Collaborative CAMPaS. Trends in survival among children with Down syndrome in 10 regions of the United States. Pediatrics. 2013;131:e27–e36.
- Glasson EJ, Sullivan SG, Hussain R, Petterson BA, Montgomery PD, Bittles AH. The changing survival profile of people with Down’s syndrome: implications for genetic counselling. Clin Genet. 2002;62:390–393.
- Petersen MB, Mikkelsen M. Nondisjunction in trisomy 21: origin and mechanisms. Cytogenet Cell Genet. 2000;91:199–203.
- Allen EG, Freeman SB, Druschel C, et al. Maternal age and risk for trisomy 21 assessed by the origin of chromosome nondisjunction: a report from the Atlanta and National Down Syndrome Projects. Hum Genet. 2009;125:41–52.
- Papavassiliou P, Charalsawadi C, Rafferty K, Jackson-Cook C. Mosaicism for trisomy 21: a review. Am J Med Genet A. 2015;167A:26–39.
- Kazemi M, Salehi M, Kheirollahi M. Down syndrome: current status, challenges and future perspectives. Int J Mol Cell Med. 2016;5:125–133.
- Canick J. Prenatal screening for trisomy 21: recent advances and guidelines. Clin Chem Lab Med. 2012;50:1003–1008.
- Bianchi DW, Rava RP, Sehnert AJ. DNA sequencing versus standard prenatal aneuploidy screening. N Engl J Med. 2014;371:578.
- Wulff CB, Gerds TA, Rode L, et al. Risk of fetal loss associated with invasive testing following combined first-trimester screening for Down syndrome: a national cohort of 147,987 singleton pregnancies. Ultrasound Obstet Gynecol. 2016;47:38–44.
- Bull MJ, Genetics Co. Health supervision for children with Down syndrome. Pediatrics. 2011;128:393–406.
- Bergström S, Carr H, Petersson G, et al. Trends in congenital heart defects in infants with Down syndrome. Pediatrics. 2016;138.
- Englund A, Jonsson B, Zander CS, Gustafsson J, Annerén G. Changes in mortality and causes of death in the Swedish Down syndrome population. Am J Med Genet A. 2013;161:642–649.
- Ramphul K, Mejias SG, Joynauth J. Leukemia in Down syndrome children based on national estimates. J Pediatr Hematol Oncol. Nov. 28, 2018:[Epub ahead of print].
- Mateos MK, Barbaric D, Byatt SA, Sutton R, Marshall GM. Down syndrome and leukemia: insights into leukemogenesis and translational targets. Transl Pediatr. 2015;4:76–92.
- Kreicher KL, Weir FW, Nguyen SA, Meyer TA. Characteristics and progression of hearing loss in children with Down syndrome. J Pediatr. 2018;193:27–33.
- Manickam V, Shott GS, Heithaus D, Shott SR. Hearing loss in Down syndrome revisited–15 years later. Int J Pediatr Otorhinolaryngol. 2016;88:203–207.
- Shott SR, Joseph A, Heithaus D. Hearing loss in children with Down syndrome. Int J Pediatr Otorhinolaryngol. 2001;61:199–205.
- Abanto J, Ciamponi AL, Francischini E, Murakami C, de Rezende NP, Gallottini M. Medical problems and oral care of patients with Down syndrome: a literature review. Spec Care Dentist. 2011;31:197–203.
- Desai SS. Down syndrome: a review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997;84:279–285.
- Pilcher ES. Treating the patient with Down syndrome. J Contemp Dent Pract. 2001;2:58.
- Baltimore RS, Gewitz M, Baddour LM, et al. Infective endocarditis in childhood: 2015 update: a scientific statement From the American Heart Association. Circulation. 2015;132:1487–1515.
- Pizzutillo PD, Herman MJ. Cervical spine issues in Down syndrome. J Pediatr Orthop. 2005;25:253–259.
- Cebeci AN, Güven A, Yıldız M. Profile of hypothyroidism in Down’s syndrome. J Clin Res Pediatr Endocrinol. 2013;5:116–120.
- Tüysüz B, Beker DB. Thyroid dysfunction in children with Down’s syndrome. Acta Paediatr. 2001;90:1389–1393.
- American Academy of Pediatrics Committe on Genetics. American Academy of Pediatrics: health supervision for children with Down syndrome. Pediatrics. 2001;107:442–449.
- Arya R, Kabra M, Gulati S. Epilepsy in children with Down syndrome. Epileptic Disord. 2011;13:1–7.
- Goldberg-Stern H, Strawsburg RH, Patterson B, et al. Seizure frequency and characteristics in children with Down syndrome. Brain Dev. 2001;23:375–378.
- Hennequin M, Faulks D, Veyrune JL, Bourdiol P. Significance of oral health in persons with Down syndrome: a literature review. Dev Med Child Neurol. 1999;41:275–283.
- Scalioni FA, Carrada CF, Martins CC, Ribeiro RA, Paiva SM. Periodontal disease in patients with Down syndrome: a systematic review. J Am Dent Assoc. 2018;149:628–639.
- Morgan J. Why is periodontal disease more prevalent and more severe in people with Down syndrome? Spec Care Dentist. 2007;27:196–201.
- Ferreira R, Michel RC, Greghi SL, et al. Prevention and periodontal treatment in Down syndrome patients: a systematic review. PLoS One. 2016;11:e0158339.
- Scalioni F, Carrada CF, Abreu L, Ribeiro RA, Paiva SM. Perception of parents/caregivers on the oral health of children/adolescents with Down syndrome. Spec Care Dentist. 2018;38:382–390.
- Mayoral-Trias MA, Llopis-Perez J, Puigdollers Pérez A. Comparative study of dental anomalies assessed with panoramic radiographs of Down syndrome and non-Down syndrome patients. Eur J Paediatr Dent. 2016;17:65–69.37.
- Lee CF, Lee CH, Hsueh WY, Lin MT, Kang KT. Prevalence of obstructive sleep apnea in children with Down syndrome: a meta-analysis. J Clin Sleep Med. 2018;14:867–875.
- Lin SC, Davey MJ, Horne RS, Nixon GM. Screening for obstructive sleep apnea in children with Down syndrome. J Pediatr. 2014;165:117–122.
- Sepúlveda E, Brethauer U, Fernández E, Cortés G, Mardones C. Oral manifestations as first clinical sign of acute myeloid leukemia: report of a case. Pediatr Dent. 2012;34:418–421.
- Duffy JH, Driscoll EJ. Oral manifestations of leukemia. Oral Surg Oral Med Oral Pathol. 1958;11:484–490.
From Decisions in Dentistry. September 2019;5(8):38—41.




