Bonded Functional Esthetic Prototype as a Diagnostic Aid
An exploration of using a bonded prototype as a diagnostic aid in cases requiring adjustment of the occlusal vertical dimension.
Dentists who take on the complexity of increasing occlusal vertical dimension (OVD), while esthetically redesigning a smile, must address a multitude of issues before confidently moving forward with treatment. This article describes a long-term provisional technique called the bonded functional esthetic prototype (BFEP) that allows dentists and patients to work together to enhance the outcome of therapy. Increasing OVD is often a necessary, yet complex, step that calls for a conservative approach to treatment planning.1 Factors to consider include the magnitude of OVD loss, facial esthetics, temporomandibular joint (TMJ) status, remaining tooth structure and occlusion.2 Given that these factors must be addressed for adequate prognosis, diagnostic wax-ups and articulated mounted study casts are essential tools to provide necessary information for predictable outcomes.1,3 One literature review concluded there is limited evidence due to the lack of randomization, appropriate controls, and long-term follow-up to suggest that increasing OVD might cause temporomandibular disorders (TMD). In addition, of those studies that qualified in the reviewers’ parameters, the results do not suggest that a moderate increase of OVD (< 5 mm) correlates with significant TMD symptoms.4 A separate review supports this and states that a 5-mm alteration is feasible, and that OVD increases greater than this are rarely indicated clinically.2

Many patients present with mild to moderate anterior attrition that has resulted in a decreased OVD. Traditionally, when increasing OVD, a clinician would provide either a splint or provisional restoration to see how the patient responds to the proposed treatment before a definitive path is taken.5 However, Poyser et al6 note that mandibular anterior composites placed at an increased OVD have a success rate of 94% at 2.5 years. In addition, Hemmings et al7 report similar findings, as they note a success rate of dental composite at 89% over 30 months when placing anterior direct restorations at an increased OVD.7 The predictable nature of bonding composites to increase vertical dimension in anterior dentition6,7 allows clinicians to confidently place long-term temporary composites (< 9 months) to gather information regarding posttreatment symptoms.
The BFEP is a provisional technique in which the clinician bonds highly filled, flowable temporary restorations to untouched/minimally prepared enamel/dentin as if they were final restorations.8 A clear matrix is fabricated from the diagnostic wax-up, and the flowable composite is cured through the matrix.3,8 With this bonding technique, the patient can function for months to evaluate the phonetics, lip support and OVD, as well as the esthetics of the new smile design.2,9 This allows clinicians to evaluate how the definitive prostheses (such as veneers or crowns) will affect a patient’s occlusion, and to identify possible pitfalls that may cause the prostheses to fail.2
A flowable, highly durable composite lends itself to the BFEP technique. In order to be successful, however, the flowable material must have the strength, wear resistance and durability of a conventional composite.8 According to Baroudi and Rodrigues,10 the variety of flowable formulations means clinicians must make sure the selected material has the properties relevant to a particular clinical situation. Balos et al11 examined which nonsilica particles were added to a flowable composite. Their study showed that with the added concentration of 0.05% nanosilica particles, higher modulus of elasticity, flexural strength and microhardness were obtained compared to the control. Another study comparing success rates between conventional and highly filled flowable composites used for posterior restorations found no observable difference between the two over a 36-month period. This study concluded the highly filled composite is “comparable, but not superior” to the conventional composite.12
CLINICAL REPORT
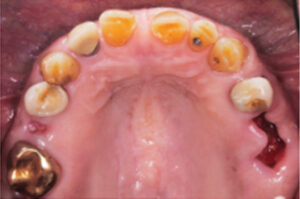
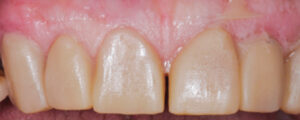
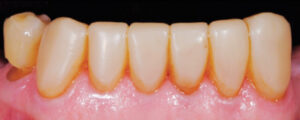
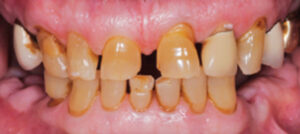
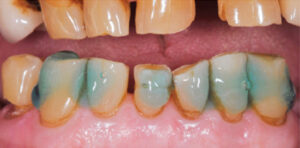
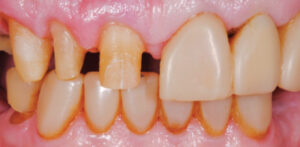
An 80-year-old male was referred to the faculty practice clinic at the Dental College of Georgia at Augusta University for a comprehensive evaluation. At the initial appointment, the patient said his teeth were “worn down” and that he did not like his smile (Figure 1). He also reported difficulty with chewing due to loss of posterior teeth (Figure 2 and Figure 3). His medical history included chronic obstructive pulmonary disorder and hypertension (both controlled with medication), prostate cancer (treated with radiation), and knee and shoulder joint replacement. An intraoral examination revealed severe generalized attrition, with no posterior support. The only existing molar was the maxillary left first molar that had been restored with a gold crown (Figure 2). A maxillary midline diastema was present, along with excessive wear of the remaining teeth, compensated by supereruption of the teeth to maintain OVD (Figure 4). A TMJ evaluation revealed no pain or tenderness to palpation of the inferior belly of the inferior lateral pterygoid muscle, and no clicking or popping of the joints. The patient’s maximum intercuspation was equal to centric relation, and he had reportedly been without posterior teeth for approximately 10 years, with the loss due to dental caries. The anterior incisors presented with attrition due to this lack of posterior support. Response to vitality testing of the remaining incisors was normal. The periodontal evaluation was within normal limits, with no bleeding on probing and normal probing depths. Preliminary impressions and a facebow were obtained, and casts were mounted in centric relation on a semi-adjustable articulator for diagnostic evaluation and treatment planning. A diagnostic wax-up of maxillary and mandibular incisors was completed, with a 4-mm increase in OVD (Figure 5).
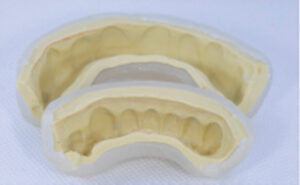
Fabrication of the clear polyvinyl siloxane (PVS) index: After completion and verification of the wax-up, the following steps were completed:
- A putty matrix impression was made of the wax-up. The thickness of the putty matrix should not exceed 2 to 3 mm (Figure 6).
- A clear, light-cure resin tray was fabricated on top of the putty matrix (Figure 6), which served as a spacer. The tray was initially polymerized with a handheld curing unit for 2 minutes. Next, it was removed from the wax-up cast and placed in the polymerization unit for 5 minutes.
- Once polymerized, the tray was removed from the unit and the clear tray was separated from the putty matrix. At this point, any undercuts in the intaglio surface of the clear tray were removed.
- Clear PVS was injected into the intaglio surface of the clear tray and seated onto the wax-up to obtain an impression (Figure 7). It is important to center the tray so the clear PVS extends 2 to 3 mm in all directions.
Fabricating the BFEP: No anesthesia is needed for this clinical protocol. A highly filled flowable composite was chosen as the restorative material. After cotton roll isolation was achieved, the restorative phase began with minor tooth preparations (elimination of unsupported enamel and sharp incisal line angles) using coarse disc or fine diamond burs. Acid etching of the enamel depends on the time the functional prototype is to be in place. For short-term use (up to 2 months), spot etching (3 mm diameter) of the enamel is enough; for long-term use (more than 6 months), etching the entire enamel surface 1 mm supragingivally is required — as was performed in this clinical report (Figure 8). A thin and uniform layer of dental adhesive was placed on all surfaces of the involved teeth. After the excess was removed with a dry microbrush, the teeth were light-cured for 20 seconds.
Fabrication of the BFEP is accomplished in the following manner:
- Clear PVS is loaded inside the clear, light-cure resin tray.
- Inject a continuous amount of the highly filled flowable composite inside the clear PVS. For this clinical case, the restorative material needed to cover all surfaces of teeth. In order to simplify final cleaning, however, avoid using excessive material.
- Seat the tray and matrix on to the teeth with gentle, but firm, pressure.
- Light-cure through the clear tray for 20 seconds per tooth.
- Remove the clear tray holding the clear PVS matrix in place. Avoid any movement of the matrix that could affect the outcome (due to lack of polymerization at this stage of the flowable composite).
- Light-cure through the clear PVS matrix for 20 seconds per tooth.
- Remove the clear PVS matrix and light-cure one more time for 20 seconds per tooth (Figure 9 and Figure 10).
Removal of excess material in the embrasure area and contouring was accomplished using a fine diamond bur and a No. 12 surgical blade. Occlusion was checked using articulating paper and adjusted using a football-shaped carbide finishing bur. Contacts in excursive movements were distributed evenly among the anterior teeth. Polishing was completed using an aluminum oxide point in combination with aluminum oxide disks. The new OVD was checked at four and eight months to verify no TMJ discomfort or chipping of the restorative material. Figure 11 and Figure 12 show the 8-month follow-up, with satisfactory function and esthetics. After this diagnostic period, the patient was referred to a periodontist for clinical crown lengthening (Figure 13) and placement of implants in the posterior.
DISCUSSION
For this patient, whose treatment plan included multiple indirect restorations requiring an increase in OVD, the BFEP served numerous purposes during the diagnostic phase. Traditionally, in cases in which OVD is being increased, a rigid, removable acrylic splint is worn for a trial period to determine if any TMD symptoms develop. The challenges with this method is that patient compliance with wearing the splint is often low,5 it may need repeated adjustment, and the opening cannot be tested during true functional and parafunctional habits. The proposed OVD can also be tested with provisional restorations, but the drawbacks to this method are that the teeth are already prepared at this stage, meaning the treatment is irreversible and the patient is already monetarily invested into the full-mouth rehabilitation. In addition, fabricating, adjusting and repairing provisional restorations can be time-consuming, especially if they need to be remade due to the development of TMD symptoms.

lengthening, with the bonded functional esthetic
prototype left in place and used as a guide during surgery.
The BFEP for this patient was completed relatively quickly. The final product was bonded in place, thus eliminating compliance issues, and it served as an accurate diagnostic tool of the increased OVD in functional movements for eight months. Although no repairs were needed in this case, the BFEP can be easily repaired. Furthermore, because no tooth preparation had been initiated, the patient was able to save for the final restorations during this diagnostic period. Following placement, the patient was shown how to clean the BFEP with interdental brushes in the gingival embrasures, as all of the teeth were bonded together.
The advantages the BFEP provided to the periodontist during the esthetic clinical crown lengthening are also significant. As discussed, a diagnostic wax-up is not only necessary to establish the desired end-result of the periodontal/restorative treatment, but a surgical guide can also be fabricated to facilitate the crown lengthening procedure. Hence, use of the surgical guide becomes essential in cases in which provisional restorations are not prepared prior to crown lengthening so the surgeon can identify the planned location of the future restoration margins, ensuring that at least 3 mm of clearance exists between the planned margins and alveolar bone crest.13 Several surgical guide designs have been proposed in the literature, including composite veneers,14 temporary smile design mock-ups,15 and computer aided design/computer aided manufacturing using a three-dimensional printer.16
Nonetheless, the periodontist in this case — who has experience with various surgical guide designs — prefers the BFEP as a surgical template for the following reasons. The BFEP provides a realistic smile design reference that becomes essential when combining gingivectomy and/or alveolectomy procedures during esthetic crown lengthening. Because the esthetic prototype is bonded, it did not have to be removed by the periodontist (as would traditional bisacryl provisional restorations), which eliminated the potential for fracturing the provisional. Additionally, no provisional restorations need to be recemented with temporary cement, which carries the risk of gingival inflammation if the excess is not thoroughly removed.
Not only was the BFEP useful during the 8-month diagnostic phase, it will also aid the restorative clinician during preparations for the final restorations. It will serve as a preparation guide, particularly during the incisal/occlusal reduction, in that the provider will be able to prepare one section through the BFEP, while the other side maintains the proposed OVD in the BFEP (Figure 14). This allows clinicians to gauge the necessary incisal/occlusal reduction from the other side, thus preventing overreduction and resulting insult to the pulp. Because the teeth are prepared through the BFEP’s bonded composite resin, reduction merely sufficient to accommodate the restorative material is needed — often making it possible to maintain enamel and existing tooth structure.17
The BFEP method proved to be a long-lasting, functional diagnostic tool for this patient in opening the OVD. It aided each of the multidisciplinary clinicians involved in this case, and provided the patient with a tangible proposal of the function and esthetics of his final restorations.
KEY TAKEAWAYS
- A long-term provisional technique called the bonded functional esthetic prototype (BFEP) allows dentists and patients to work together to enhance the outcome of therapy when increasing occlusal vertical dimension (OVD).
- Factors to consider with this therapy include the magnitude of OVD loss, facial esthetics, temporomandibular joint status, remaining tooth structure and occlusion.2
- The BFEP is a provisional technique in which the clinician bonds highly filled, flowable temporary restorations to untouched/minimally prepared enamel/dentin as if they
were final restorations.8 - With this bonding technique, the patient can function for months to evaluate phonetics, lip support and OVD, as well as the esthetics of the new smile design.2,9
- The BFEP method aided each of the multidisciplinary providers involved in this case, and provided the patient with a tangible proposal of the function and esthetics of
the planned final restorations.
ACKNOWLEDGEMENT
The authors would like to thank William W. Brackett, DDS, MSD, for his assistance in reviewing this manuscript.
REFERENCES
- Song MY, Park JM, Park EJ. Full mouth rehabilitation of the patient with severely worn dentition: a case report. J Adv Prosthodont. 2010;2:106–110.
- Abduo J, Lyons K. Clinical considerations for increasing occlusal vertical dimension: a review. Aust Dent J. 2012;57:2–10.
- McLaren E. The bonded functional esthetic prototype: part 2. Inside Dentistry. 2013;9:84–92.
- Moreno-Hay I, Okeson JP. Does altering the occlusal vertical dimension produce temporomandibular disorders? A literature review. J Oral Rehabil. 2015;42:875–882.
- Prasad S, Kuracina J, Monaco EA Jr. Altering occlusal vertical dimension provisionally with base metal onlays: a clinical report. J Prosthet Dent. 2008;100:338–342.
- Poyser NJ, Briggs PF, Chana HS, Kelleher MG, Porter RW, Patel MM. The evaluation of direct composite restorations for the worn mandibular anterior dentition – clinical performance and patient satisfaction. J Oral Rehabil. 2007;34:361–376.
- Hemmings KW, Darbar UR, Vaughan S. Tooth wear treated with direct composite restorations at an increased vertical dimension: results at 30 months. J Prosthet Dent. 2000;83:287–293.
- McLaren E, Schoenbaum T. The bonded functional esthetic prototype: part 1. Inside Dentistry. 2013;9:70–74.
- Gürel G, Bichacho N. Permanent diagnostic provisional restorations for predictable results when redesigning the smile. Pract Proced Aesthet Dent. 2006;18:281–286; quiz 88, 316–317.
- Baroudi K, Rodrigues JC. Flowable resin composites: a systematic review and clinical considerations. J Clin Diagn Res. 2015;9:ZE18–ZE24.
- Balos S, Pilić B, Petronijević B, Marković D, Mirković S, Sarcev I. Improving mechanical properties of flowable dental composite resin by adding silica nanoparticles. Vojnosanit Pregl. 2013;70:477–483.
- Kitasako Y, Sadr A, Burrow MF, Tagami J. Thirty-six month clinical evaluation of a highly filled flowable composite for direct posterior restorations. Aust Dent J. 2016;61:366–373.
- Jorgensen MG, Nowzari H. Aesthetic crown lengthening. Periodontol 2000. 2001;27:45–58.
- Walker M, Hansen P. Template for surgical crown lengthening: fabrication technique. J Prosthodont. 1998;7:265–267.
- Trushkowsky R, Arias DM, David S. Digital Smile Design concept delineates the final potential result of crown lengthening and porcelain veneers to correct a gummy smile. Int J Esthet Dent. 2016;11:338-54.
- Yin J, Liu D, Huang Y, Wu L, Tang X. CAD/CAM techniques help in the rebuilding of ideal marginal gingiva contours of anterior maxillary teeth: a case report. J Am Dent Assoc. 2017;148:834–839.e8.
- Fradeani M, Barducci G, Bacherini L, Brennan M. Esthetic rehabilitation of a severely worn dentition with minimally invasive prosthetic procedures (MIPP). Int J Periodontics Restorative Dent. 2012;32:135–147.
Featured image by CSAKITI/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. July 2018;4(7):8-10,12.