Passive Space Management in Children
An essential part of pediatric dental care, understanding the concept of space management is critical in managing the developing dentition.
The significance of healthy primary dentition is often overlooked by health care providers, parents and caregivers due to the belief that primary teeth will eventually be replaced by permanent teeth and will not cause any issues if lost prematurely. In one study, it was reported that more than 40% of parents/caregivers felt it was unnecessary to spend time and money on a tooth that is going to shed.1 The impact of loss of deciduous teeth would not be realized until later, and could lead to costly and complicated orthodontic and/or surgical treatment. Therefore, the importance of preserving the primary dentition should be emphasized by dental professionals. The concept of space management is critical in managing the developing dentition and is essential knowledge for any dental provider who cares for children.

ectopic eruption due to crowding and
space loss.
One of the functions of the primary dentition is to preserve space for the succedaneous teeth. Teeth have a tendency to drift into edentulous space. Without intervention, premature loss or reduction in tooth mass (due to factors such as interproximal dental caries in deciduous teeth) could lead to inadequate space for erupting permanent teeth. Hence, maintenance of a healthy primary dentition and its existing space is paramount in preserving arch length and space for the erupting permanent dentition, and preventing complications leading to malocclusion, ectopic eruption, crowding, impaction, super-eruption, and tipping and drifting of teeth (Figure 1).
Spacing between primary teeth is generally beneficial and doesn’t need to be closed. It not only provides ease of cleansing and reduces caries incidence, but, most importantly, provides leverage to accommodate and offset the tooth size discrepancy between primary and permanent dentitions. It also alleviates minor crowding of permanent teeth.2 Baume described two distinct types of arch form in primary dentition, and approximately two-thirds of the primary dentition exhibited generalized spacing known as Baume Type I. Those without spacing or with closed proximal contacts were termed Baume Type II. Studies have shown a correlation between amount of spacing in the primary dentition and severity of crowding in the permanent dentition.3,4 If the child has more than 6 mm of spacing, crowding is less likely to be observed in permanent dentition. If the spacing is between 3 to 6 mm, there would be approximately a 20% chance that crowding will occur in the permanent dentition. For those with less than 3 mm of spacing, the possibility of crowding increased to 50%. If a child has no space in the deciduous teeth, crowding of the permanent dentition would be highly likely (more than a 66% chance). With existing crowding in the primary dentition, it would be almost certain that the child will have crowding in the succedaneous dentition.

between primary teeth.
To predict space availability, various space analysis methods have been utilized — such as Tanaka and Johnston, Nance, Hixon and Oldfather Mixed Dentition Analyses, and the Moyer’s method — that are based on prediction tables, dental casts and/or radiographs. Determinants and variables that may affect available arch space and lead to space issues include tooth size discrepancy, supernumerary teeth, ectopic eruption of teeth, congenitally missing teeth, sequence and timing of tooth eruption, premature loss of teeth, arch development, and interproximal dental caries.
Developmental spaces have been identified in developing dentitions of children, and were distinctive and categorized based on the anatomical position in the arch (Figure 2). Primate space is a naturally occurring spacing between deciduous teeth. In the mandibular arch, the primate space is observed between primary canine and first molar. The primate space in the maxillary arch is located between primary lateral incisor and canine. Other generalized spacing mesial to the primary canine and in between incisors is termed physiological space.4 The leeway space involves posterior primary teeth and accounts for tooth size difference between primary and permanent dentitions. It is the space to be preserved when primary teeth are lost prematurely. The realization of leeway space occurs during the process of exfoliation and eruption of succedaneous teeth in the mixed dentition and may relieve some crowding in the permanent dentition.5 The amount of available space is calculated based on the difference between the sum of width of primary canine, primary first molar, and primary second molar and the sum of widths of their succedaneous teeth; or (C+D+E) – (3+4+5) = leeway space. The leeway space derives from larger mesial-distal anatomical dimension of primary molars compared to their permanent successors or premolars (Figure 3), and stays the same from time of eruption of the second deciduous molars until that tooth is lost. It is either saved via space maintenance or lost due to mesial drifting of the first permanent molar. The leeway space serves as the basis in the concept of passive space management in the developing occlusion.

leeway space.
MECHANISMS FOR PRESERVING SPACE
The best space maintenance is the one provided by natural teeth and is one of the many functions of the primary dentition. Good oral hygiene practices, dietary habits, and an effective caries prevention protocol are the fundamental and most efficient, cost-effective methods of preserving the arch length and space. Hence, parental education about the critical role that primary dentition plays and its effect on permanent dentition should serve as a priority and basic element in space management.
immediately following tooth extraction.
Early recognition and timely intervention of dental disease and interproximal dental caries can prevent space loss, as teeth have a tendency to drift into edentulous spaces and into damaged, lost dental structure. Previous studies have reported that the arch length could be reduced due to carious breakdown of dental structure, even in absence of premature loss of teeth.6,7 It was evident that the mesial-distal width of teeth is reduced due to extensive proximal caries and compromised by drifting of adjacent teeth, and subsequent restorative procedures would be altered and modified. The placement of a stainless steel crown, for example, in such a situation may require significant adjustment, such as squeezing the mesial-distal dimension of the prefabricated crown and reducing the mesial-distal width of the crown, which otherwise would have fit nicely on a prepared tooth without significant adjustment. Shape of the restored interproximal surface of an intracoronal restoration may not follow the physiological contour and may be concave due to chronic drifting of adjacent teeth into the previous caries lesions. Restoring a primary tooth with dental caries not only serves to restore the esthetic and physiologic form, it also prevents space loss and preserves arch length.
The relationship between premature loss of primary teeth and space loss with reduction in arch length has been well documented in the literature.6,8 The amount of space loss accelerated and increased during the active eruption phase of permanent first molars. If the deciduous tooth is extracted before 6 years of age, the loss is more significant than those extracted after the eruption of the first permanent molar, with the effect more significant in the maxillary arch.9 Therefore, an appliance to maintain space for the extracted primary teeth is crucial and should be placed in a timely manner. If the leeway space is not preserved promptly, the consequence could be costly and require orthodontic treatment to open and create space for succedaneous teeth to erupt.

loop appliance.
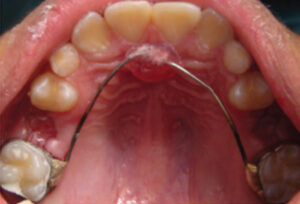
Management and preservation of space can be easily accomplished with a passive appliance. For children, a fixed appliance is preferred due to treatment compliance. A variety of space maintainers is available, and each appliance comes with specific indications (Table 1) and limitations. A space maintainer should be placed as soon as a tooth is lost or extracted (Figure 4). A lengthy wait between tooth extraction and final cementation of the appliance may lead to tipping and drifting of adjacent teeth, space loss, poor fit, and remaking of the appliance. If feasible, consideration should be given to fabrication of the appliance prior to tooth extraction. The tooth to be extracted, if asymptomatic, could serve as a natural space maintainer until the extraction can be performed. With the space maintainer available, the extraction could be performed immediately prior to cementation of the space maintainer with glass ionomer cement. As a precaution for the cementation of the appliance (especially when working with children), a piece of dental floss should be attached to the space maintainer to prevent possible aspiration of the appliance.
COMMON SPACE MAINTAINERS
The most common space maintainer is the band and loop appliance, which held space for single extracted tooth (Figure 5). Custom fabrication of a band and loop appliance is a durable and precise means of preventing adjacent teeth from drifting and tipping into the space. The band should fit tightly, present some degree of difficulty to remove with digital pressure, and the occlusal portion of the band should be placed below the marginal ridge of the anchor tooth to prevent interference with occlusion. The loop is made with 0.036-inch orthodontic wire bent into shape with three-prong plier and is extended and in direct contact with the proximal surface of tooth adjacent to the space. The anchor tooth with band is usually the first permanent molar or the tooth distal to the empty space. However, if the permanent molar is partially erupted and a band cannot be fitted, a reverse band and loop appliance could be an alternative option, with the band placed on the primary first molar and the loop extended distally. The band and loop appliance is also available in a prefabricated form (Figure 6).
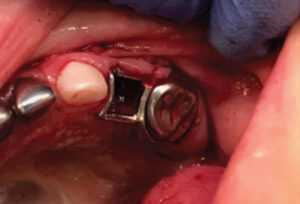
In a situation in which the primary second molar is extracted and permanent first molar has not erupted adequately to serve as the anchor tooth, a distal shoe is indicated for space maintenance and guidance of the unerupted permanent first molar into proper position in the arch (Figure 7). The blade of distal shoe would extend through the gingiva to engage the mesial surface of the unerupted permanent first molar. The distal shoe appliance is also available in a prefabricated form; however, the wire attachment may easily be dislodged upon mastication. A chairside modification with an electric spot welder has been shown to improve the clinical performance of the prefabricated distal shoe appliance.10 A radiograph should be taken to verify the position and proper engagement of the distal shoe blade prior to final cementation (Figure 8). The distal shoe appliance may not be appropriate and is contraindicated in children who are medically compromised or have systemic diseases, such as diabetes mellitus, hemophilia, a compromised immune system, or cardiac anomalies requiring antibiotic prophylaxis.11

appliance.
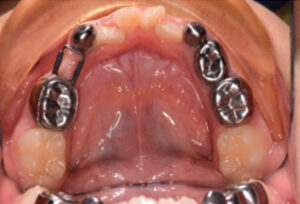
When multiple primary teeth are extracted or lost prematurely, a bilateral fixed appliance is the treatment of choice and provides arch stability and space preservation. A lower lingual holding arch appliance can maintain arch length in the mandible (Figure 9). The design consists of bands placed on the permanent first molars bilaterally and connected by a heavy lingual wire circumferentially, resting on the cingulae of incisors above the gingival margin. Omega loops near the posterior section of the lingual wire are frequently incorporated bilaterally into the appliance design for adjustment and minor activation, if needed. One criterion that should be met prior to fabrication of a lower lingual holding arch appliance is that the permanent incisors and permanent first molars must be adequately erupted. As the mandibular permanent incisors erupted lingual to the deciduous teeth, an inappropriately placed appliance may hinder the eruption of permanent incisors, trap the incisors ectopically, and pose as a potential obstacle if it is placed prior to the eruption of permanent incisors. In this case, two band and loop appliances may be the most appropriate treatment option.
For the maxillary arch, a Nance appliance and transpalatal arch appliance present two options for bilateral fixed appliances in children. The clinical indications for a Nance appliance is similar to that of the lower lingual holding arch appliance, but the eruption of incisors is not a factor to consider with a Nance appliance (Figure 10). An acrylic button is incorporated anteriorly to provide contact with palate and stabilization, as opposed to resting on the teeth. Although hygiene and cleansing may be an issue, the Nance appliance is most effective in case of tooth loss bilaterally in the maxillary arch. The transpalatal arch appliance presents a hygienic alternative. Bands cemented to the maxillary first permanent molars are connected by a single heavy wire across the posterior palate (sometimes with an omega loop incorporated into the midline portion of the wire) without contacting soft tissue The appliance can prevent mesio-palatal rotation of the maxillary permanent first molar. However, it has limited efficacy in preventing mesial tipping of molars. Therefore, a transpalatal arch appliance should not be considered as the first option for patients with bilateral tooth loss in the maxilla.
Not all the cases of premature loss of primary tooth require placement of an appliance to preserve arch length. Space maintainers may not be indicated when imminent eruption of a succedaneous tooth is preceded by primary tooth exfoliation. When the primary incisors are lost prematurely, no space maintainer is indicated, and any appliance fabricated to replace deciduous anterior teeth is mainly for esthetics. If the first permanent molar is completely erupted and in stable occlusion, the loss of deciduous first molar may not warrant placement of a space maintainer. Park et al12 reported minimal change in available space for erupting succedaneous premolars after premature loss of primary first molars, provided the permanent first molars have already erupted and are in Class I molar relationship. Conversely, if a deciduous second molar is lost prematurely, a space maintainer appliance should be placed, regardless the state of permanent first molars.
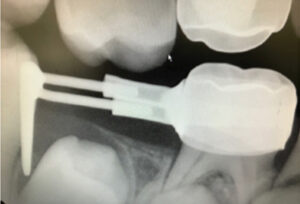
position and engagement of distal shoe
blade prior to final cementation.
FOLLOW-UP MANAGEMENT
Once a space maintainer is placed, continuous follow-up and monitoring are required. Detailed instructions should be presented to the parent/caregiver at the insertion visit in order to avoid miscommunication and noncompliance. The need to return for periodic evaluation and assessment of treatment should be emphasized. If the appliance is defective or lost, a decision must be made to either repair or replace it, or discontinue the appliance based on assessment and the state of dental development and eruption of the permanent dentition. It is critical to inform parents/caregivers that space maintainers should be evaluated at routine intervals, and that appliance removal is necessary upon eruption of the appropriate permanent tooth or teeth. The consequence of prolonged retention of space maintainers may lead to undesirable complications, such as ectopic eruption of permanent teeth. Finally, if a space has been held by a distal shoe appliance, replacement with a band and loop appliance may be indicated in the future, following the eruption of permanent molars.
Daily oral hygiene practice may present a significant challenge at times, as cleaning is difficult around the bands and wires — but it is absolutely essential to maintain good oral hygiene and healthy hard and soft tissues. Risks and benefits, potential complications, and alternative treatment options should be discussed with parents/caregivers prior to fabrication and placement of an appliance, especially if the child has a debilitating medical condition, combative or cognitive issue, or special needs.
SUMMARY
The primary dentition maintains arch length and space for permanent teeth. Restoration of carious primary teeth can prevent drifting and tipping of adjacent teeth and space loss. Premature loss of a deciduous tooth may warrant placement of a space maintainer appliance. Once the appliance is placed, clinical management is not finished, and periodic evaluation and assessment are required until the eruption of the permanent succedaneous tooth and removal of the appliance.
KEY TAKEAWAYS
- One of the functions of the primary dentition is to preserve space for the succedaneous teeth.
- Leeway space involves posterior primary teeth and accounts for tooth size difference between primary and permanent dentitions. It is the space to be preserved when primary teeth are lost prematurely.
- Good oral hygiene practices, dietary habits, and an effective caries prevention protocol are the fundamental and most efficient methods of preserving the arch length and space.
- Space preservation can be easily accomplished through the use of passive appliances.
- Parental education about the critical role that primary dentition plays and its effect on permanent dentition should serve as a priority and basic element in space management.
REFERENCES
- Setty JV, Srinivasan I. Knowledge and awareness of primary teeth and their importance among parents in Bengaluru City, India. Int J Clin Pediatr Dent. 2016;9:56–61.
- Vinay S, Keshav V, Sankalecha S. Prevalence of spaced and closed dentition and its relation to malocclusion in primary and permanent dentition. Int J Clin Pediatr Dent. 2012;5:98–100.
- Leighton BC. The early signs of malocclusion. Eur J Orthod. 2007;29:i89–i95.
- Baume LJ. Physiological tooth migration and its significance for the development of occlusion. I. The biogenetic course of the deciduous dentition. J Dent Res. 1950;29:123–132.
- Gianelly AA. Leeway space and the resolution of crowding in the mixed dentition. Semin Orthod. 1995;1:188–194.
- Northway WM, Wainright RL, Demirjian A. Effects of premature loss of deciduous molars. Angle Orthod. 1984;54:295-329.
- Northway WM, Wainright RW. D E Space–a realistic measure of changes in arch morphology: space loss due to unattended caries. J Dental Res. 1980;59:1577–1580.
- Seward FS. Natural closure of the deciduous molar extraction spaces. Angle Orthod. 1965;35:85–94.
- Luzzi V, Fabbrizi M, Coloni C, et al. Experience of dental caries and its effects on early dental occlusion: a descriptive study. Ann Stomatol (Roma). 2011;2:13–18.
- Brill WA. The distal shoe space maintainer chairside fabrication and clinical performance. Pediatr Dent. 2002;24:561–565.
- Hicks EP. Treatment planning for the distal shoe space mainitainer. Dent Clin North Am. 1973;17:135–150.
- Park K, Jung DW, Kim JY. Three-dimensional space changes after premature loss of a maxillary primary first molar. Int J Paediatr Dent. 2009;19:383–389.
Featured image by REANAS/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. July 2018;4(7):13–14,17–18.