
Accurate Diagnosis in Endodontic Therapy
A careful evaluation of the patient’s clinical presentation and pathosis is key to establishing a sound endodontic diagnosis.
First in a two-part series: The material in this multipart series was adapted from a white paper published in 2017 by the American Association of Endodontists. Appearing in a future issue, Part 2 will focus on competence in treatment planning and prognosis of endodontic therapy.
The American Association of Endodontists (AAE) offers this information as a means of outlining and defining the skills required of all dentists who perform endodontic diagnosis and treatment. These guidelines are meant to establish context regarding the knowledge and skill that should provide a standard for all practitioners who undertake the responsibility to diagnose, treatment plan, and provide prognoses for the endodontic care of patients. When deciding whether to provide treatment or refer a case, clinicians should consider that general dentists are bound to the same standard of care as endodontic specialists. Only if practitioners are confident they can meet this standard should treatment be rendered.
In the diagnosis of endodontic pathosis:
- The practicing dentist should be able to manage a patient with pathosis of pulpal and/or periapical origin. The first step in this management is the diagnosis of the problem. The dentist should be able to assimilate the necessary subjective, objective and radiographic information to establish a pulpal and/or periapical diagnosis. Appropriate treatment or referral can only occur if the patient’s signs and symptoms are properly diagnosed and understood as a biologic departure from health.
- A dentist should be able to provide/manage urgent/emergent care to patients experiencing signs and symptoms of pulpal and/or periapical pathoses, which can lead to pain and/or swelling. This includes consultation and/or the provision of immediate referral, if indicated.
- Clinicians should be able to evaluate, diagnose, provide emergency care, or refer patients presenting with traumatic injuries. Providers are expected to know the traumatic dental injury protocols and recommendations published by the AAE and the International Association of Dental Traumatology.

As the most critical step in dental treatment, developing a diagnosis is the process of gathering information and applying the data to the individual patient. This information is correlated from the patient’s history of treatment, pain, trauma or restorative procedures, clinical examinations, results of clinical tests, and radiographic examination of the teeth and surrounding tissues. By definition, diagnosis is both the process of identifying the presence of disease and naming the disease itself. In endodontics, a multitude of pathologic entities exist that are distinguished in the diagnostic process, and establishing the correct diagnosis permits the implementation of an appropriate treatment regimen. The basic endodontic diseases are associated with pathoses of the pulpal and/or periapical tissues and their related inflammatory processes.
The diagnostic process begins with a patient interview and review of the medical history, dental history and pain history. A thorough patient and pain assessment interview will often enable the clinician to differentiate between odontogenic and nonodontogenic pain. The latter can often become chronic and debilitating in nature. Furthermore, this pain can be exacerbated by incorrect or unnecessary treatments that may result in the establishment of chronic pain pathways. When symptoms don’t make sense, or do not correlate with normal odontogenic descriptors of pain, the clinician becomes obligated to seek opinions from specialist colleagues before initiating endodontic treatment.
An accurate diagnosis is crucial for the development of a comprehensive treatment plan, including alternative options — such as no treatment, vital pulp treatment, nonsurgical root canal treatment, surgical root canal treatment, extraction or referral. Pulpal and periapical testing should always be conducted to establish an accurate diagnosis. After making an endodontic diagnosis, the clinician must answer two critical questions before progressing to treatment or referral to a specialist:
- Can the tooth be properly restored?
- Do the supporting structures provide a reasonable prognosis?
Endodontic diagnoses always include both a pulpal and a periapical diagnosis, and treatment should not be initiated without at least a tentative diagnosis and patient consent. In the majority of situations, a diagnosis can be reached that is sufficiently certain for treatment to proceed. In some cases, however, where there is conflicting evidence or referred pain with unknown etiology, it is better to let some time pass for the condition to clarify than to make an incorrect diagnosis or start unnecessary or inappropriate treatment. Without a diagnosis, there can be no treatment plan.
KEY TAKEAWAYS
- These guidelines detail the knowledge and skill necessary for any practitioner who undertakes the responsibility to diagnose, treatment plan, and provide prognoses for endodontic care.
- When deciding whether to provide treatment or refer a patient, clinicians should consider that general dentists are bound to the same standard of care as endodontic specialists.
- The clinician should be able to assimilate the necessary subjective, objective and radiographic information to establish a pulpal and/or periapical diagnoses.
- Keeping detailed clinical records is critical to effective endodontic care. Records are also a fundamental means of communication should the patient be referred for continued or follow-up care.
- In endodontics, a multitude of pathologic entities exist that are distinguished in the diagnostic process, and establishing the correct diagnosis permits the implementation of an appropriate treatment plan.
THE PATIENT INTERVIEW
There are several critical aspects to the patient interview, including the chief complaint, history of the chief complaint, medical history and dental history. Only a recent myocardial infarct, uncontrolled hypertension and uncontrolled diabetes have been identified as systemic contraindications for endodontic treatment. However, a thorough and current medical history is mandatory before any dental treatment can begin. The medical history is vital in order to determine whether medical consultation with the patient’s physician may be necessary, or how systemic conditions might impact healing or prognosis. It is important to confirm the patient’s health status to coordinate treatment and evaluate if premedication is necessary before diagnostic examination or clinical treatment can be undertaken. While some patients may require premedication with systemic antibiotics prior to treatment, others can present with allergies requiring an alternate medication or drug. The potential effect of electrically powered instruments — such as ultrasonic units or electrosurgical instruments — on a patient’s pacemaker function or cochlear ear implants must be carefully evaluated prior to treatment.
The dental history can help direct a diagnosis, and it is important to inquire if a patient has had any recent dental treatment or injuries. A fractured tooth as a result of caries can frequently result in a near or actual pulp exposure and often leads to an uncomplicated diagnosis. Evaluating radiographs and recognizing the extensive nature of restorations, and looking at the quality, depth and structural impact of past restorations, can provide meaningful clues to the possibility of irreversible pulpal inflammation. To obtain all essential facts, the art of careful listening and acting in a caring manner cannot be overemphasized. Treatment decisions must be made considering all patient treatment modifiers, such as oral health and hygiene, finances, esthetics, expectations of therapy, and function.
A chief complaint is often the reason a patient seeks care, and it is important for the individual to express this in his or her own words, which should be noted in the treatment record. A clear understanding of a patient’s motivation for seeking care and of his or her expectations will help alleviate misperceptions and improve communication in the dentist-patient relationship. Important considerations for the patient interview include:
- The character of the complaint
- The location and inception of the complaint, as well as provoking or attenuating factors
- Frequency, intensity and duration, and whether the pain is spontaneous or stimulated
- Is the pain getting better or worse?
A majority of endodontists will rely on a judgment of irreversible inflammation when the pain has two major characteristics: Complaints of spontaneity and intensity are fundamental descriptors that link the biology of irreversible pulpal inflammation to symptoms. It is important to realize that pain of endodontic origin can, at times, be intense and debilitating. Inception of symptoms is typically of short duration — as opposed to the months or years noted in chronic pain syndromes. Pulpal/periradicular pain will characteristically become focused on a particular tooth or dissipate, only to return at a later date.

ASSESSING TRAUMATIC DENTAL INJURIES
A clinician’s ability to assess, diagnose and treatment plan for traumatic dental injuries and known sequelae, such as mineralization and root resorption, places additional requirements for competence in this area of care. All dental practitioners should be able to evaluate, diagnose and provide emergency care in instances of dental trauma, as well as develop a comprehensive treatment plan. Providers are expected to learn fundamental protocols and recommendations published by the International Association of Dental Traumatology and the American Association of Endodontists. Diagnosis and appropriate treatment of root resorption is complex, and, in complying with contemporary standards of practice, requires three-dimensional imaging. The clinician should be able to make a differential diagnosis of the different types of root resorption and provide the proper management or appropriate referral to a specialist.
TRAUMATIC DENTAL INJURIES
Traumatic dental injuries must be assessed carefully because treatment immediately after injury has a major influence on future prognosis. Generally, treatment can be accomplished without significant difficulty; however, it can also be complicated and require specialty expertise. A primary diagnosis based on an accurate assessment must be carried out competently following established guidelines.
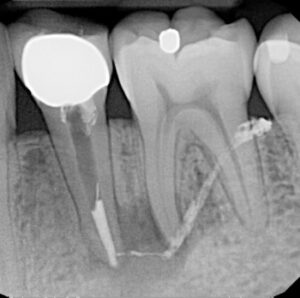
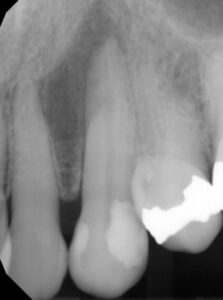
Most practitioners consider all diagnoses as the art and science of identifying departure from health and its cause. Inherent in this process is the identification of all conditions that may produce the same signs and symptoms. Because testing for health or disease of pulpal circulation encased in a mineralized exterior can be challenging, all information must be interpreted indirectly from the patient response to stimulus placed externally on the tooth. This is subjective and varies between patients, and within patients as they age. By and large, pulpal testing is more valid in determining that teeth are free of disease, and less accurate in identifying teeth with pulpal pathoses. However, diagnostic tests that include thermal and electric pulp testing, palpation, percussion, periodontal probing, a bite test, and radiographic examination and interpretation (Figure 1, Figure 2 and Figure 3) will provide multiple confirmations that can build confidence in a diagnosis. Signs and symptoms of odontogenic pain include constant pain, prolonged sensitivity to temperature changes, an extruded feeling in the tooth, tenderness to biting pressure, impaired mouth opening, tooth mobility, and tenderness to palpation in the apical area. These signs and symptoms in various combinations are highly accurate predictors of odontogenic disease.
IMPORTANCE OF TREATMENT RECORDS
In determining the quality of endodontic records and the clinician’s responsibility for those records, a statement that should define any practitioner of endodontics is simply that “good clinicians keep good records.” The dental record of endodontic treatment serves as important documentation to guide the clinician’s objective data through the correct diagnostic and treatment path. Documentation is essential to attaining an accurate log of events and decision-making, as endodontic diagnosis is a clinical diagnosis based on the database gathered. Over time, the database may change as more information is obtained, possibly indicating a different diagnostic classification.
The dental record must contain sufficient information to identify the patient, support the diagnosis, justify the treatment, and document the course and result of treatment that is designed to protect the patient’s welfare. Records are also a fundamental means of communication among health care professionals should the patient be referred for continued or follow-up care. A systematic and complete record should contain:
- A thorough review of the patient’s medical and dental history
- Chief complaint(s), including onset, duration, frequency, type and intensity of any pain
- Pulpal and periodontal diagnostic tests performed
- Objective clinical examination findings
- Differential diagnoses and definitive diagnosis
- Radiographs of diagnostic quality
- The treatment plan, alternative options and prognosis
- Documentation of the course of treatment
These are essential components of a quality record that supports the doctor-patient interaction. When other factors affect the prognosis of any tooth diagnosed for endodontic treatment — such as the tooth’s strategic value, restorability, supporting structures, or the tooth’s proximity to vital structures — prior to initiating endodontic treatment the clinician should consider further consultation with an endodontist or other specialist, including a prosthodontist, periodontist, pediatric dentist, oral pathologist, or radiologist with advanced imaging capability.

IMAGING AND DIAGNOSIS
The collection and collation of pertinent information is central to the establishment of an appropriate and accurate diagnosis. Radiographs are prescribed only after the clinical examination to ensure the proper projections are obtained. Preoperative radiographs are an indispensable part of diagnostic procedures in root canal treatment. A simple bitewing radiograph will always yield the truest projection of the pulp chamber and its depth, along with the depth of interproximal caries and prior restorations. Bitewing radiographs provide additional information about the teeth of the opposing arch, as well as the arch under investigation, and frequently can direct the clinician’s eye to a possible problem on an opposing tooth that might be overlooked with periapical films alone.
That noted, recognition and diagnosis of periapical disease on conventional radiographs can be challenging. Well-angulated periapical films should be taken with the cone directed straight on, mesio-oblique, and disto-oblique. This technique often reveals and clarifies the three-dimensional (3D) morphology of the tooth and identifies anatomic complexities. Digital radiography and other imaging technologies offer an enhanced variety of software features that significantly augment radiographic diagnostics when identifying anatomical complexities. The clarity, color, contrast and brightness of a digital image can be easily modified, affording greater capability in interpreting hidden, mineralized or untreated canals.

When a radiographic examination is performed or required, the practitioner assumes the responsibility to make accurate interpretations from images of diagnostic quality (Figure 4, Figure 5 and Figure 6). It is common understanding that pathoses, as well as anatomic entities, are often missed in two-dimensional radiographic surveys, both by the operator and the limitations of the technology when encountering differences in anatomic variation. Advanced 3D imaging, such as cone beam computed tomography (CBCT), can image periapical lesions and other anatomical structures in horizontal, vertical and sagittal sections. The scanning devices responsible for these “limited field” 3D images have greatly advanced our understanding of the anatomic complexities in any given case, elucidating preoperative intricacies and unseen pathoses and canal complications. When their utilization is indicated, the field of view can be limited to several teeth and the resulting CBCT scans can produce images with excellent contrast and clarity — and with limited radiation. One of the greatest causes of poor outcomes in molar endodontics is failure to locate and treat all parts of the canal system. The appropriate radiographic techniques (periapical and/or CBCT imaging) will provide the information to address these shortcomings.
In difficult instances of diagnosis — such as internal or external resorption, which often superimposes itself over pulpal anatomy — a 3D image accurately defines the extent of the disease and the amount of resorptive invasion. Assessment of periradicular lesions in multirooted teeth and differentiating these lesions from nonodontogenic pathoses, as well as understanding size and distances, are now predictably possible with limited field cone beam imaging. In addition to spatial relationships of root apices to anatomical structures, accessory canals, location of root canals and canal obstructions can be viewed. Utilizing these approaches, the healing and repair of pathoses after nonsurgical and surgical endodontics can be observed in a far more predictable manner, which can dramatically aid clinicians in treatment planning and predicting prognosis.
IN SUMMARY
An accurate diagnosis is the cornerstone of effective treatment planning and therapy. As noted at the outset, when considering endodontic treatment, the general dentist is bound to the same standard of care as the endodontist. Consequently, referral should be considered when appropriate. For example, in a recently published study of retention outcomes on endodontically treated molars, complex teeth showed a 10-year survival rate that was statistically and significantly better when treatment was performed by endodontists. Regardless of the provider, however, clinicians have a responsibility to deliver the best care possible. In that light, these guidelines detail the knowledge and skills necessary to establish a diagnosis that permits implementation of an appropriate treatment plan. Toward that goal, the next installment in this two-part series will explore clinical competence in endodontic treatment planning and prognosis.
SUGGESTED BIBLIOGRAPHY
Standards of Practice, Case Assessment, Initial Treatment, Cost Effectiveness
- American Association of Endodontists. Endodontic Case Difficulty Assessment and Referral. Chicago, IL: 2005;1–4.
- American Association of Endodontists. The standard of practice in contemporary endodontics. ENDODONTICS: Colleagues for Excellence. Chicago, IL. 2014;1–12
- American Association of Endodontists and American Academy of Oral and Maxillofacial Radiology. Joint Position Statement: Use of Cone Beam Computed Tomography in Endodontics 2015 Update.
- American Association of Endodontists. Recommended Guidelines for the Treatment of Traumatic Injuries. 2013; aae.org.
- Canadian Academy of Endodontics. Standards of Practice. Copyright 1998 Canadian Academy of Endodontics; revised 2015. Winnipeg, MB.
- Stedman’s Medical Dictionary, 28th ed. Philadelphia: Lippincott Williams & Wilkins. 2006.
- Ricucci D, Loghin S, Siqueira JF, Jr. Correlation between clinical and histologic pulp diagnoses. J Endod. 2014;40:1932–1939.
- Levin LG, Law AS, Holland GR, Abbott PV, Roda RS. Identify and define all diagnostic terms for pulpal health and disease states. J Endod. 2009;35:1645–1657.
- Jaeger B, Reyes MR. Non-odontogenic Toothache and Chronic Head and Neck Pain. In: Ingle JI, Bakland LK, Baumgartner C, eds. Ingle’s Endodontics. 6th ed. Ontario, Canada: BC Decker; 2008:392–467.
- von Eckardstein KL, Keil M, Rohde V. Unnecessary dental procedures as a consequence of trigeminal neuralgia. Neurosurg Rev. 2015;38:355–360.
- Newton CW, Hoen MM, Goodis HE, Johnson BR, McClanahan SB. Identify and determine the metrics, hierarchy, and predictive value of all the parameters and/or methods used during endodontic diagnosis. J Endod. 2009;35:1635–1644.
- Siedberg BH. The Law and Endodontics. In: Ingle JI, Bakland LK, Baumgartner C, eds. Ingle’s Endodontics. 6th ed. Ontario, Canada: BC Decker; 2008:86–104.
- Ng YL, Mann V, Gulabivala K. Tooth survival following non-surgical root canal treatment: a systematic review of the literature. Int Endod J. 2010;43:171–189.
- Ng YL, Mann V, Rahbaran S, Lewsey J, Gulabivala K. Outcome of primary root canal treatment: systematic review of the literature — Part 2. Influence of clinical factors. Int Endod J. 2008;41:6–31.
- Ricucci, Mannocci F, Ford TR. A study of periapical lesions correlating the presence of a radiopaque lamina with histological findings. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:389–394.
- Todd R. Cone beam computed tomography updated technology for endodontic diagnosis. Dent Clin North Am. 2014;58:523–543.
Featured image by DUSANMANIC/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. April 2018;4(4):12-14,16.


