 DUSANPETKOVIC/ISTOCK/GETTY IMAGES PLUS
DUSANPETKOVIC/ISTOCK/GETTY IMAGES PLUS
Visual Acuity and Ergonomic Health
Maintaining visual acuity helps clinicians support ergonomic health.
Ergonomics is the scientific discipline that is concerned with the understanding of interactions among humans and their work.1 The desired outcome of ergonomic science is to fit the work to the worker in a manner that can help individuals achieve job performance objectives, while maintaining their health and well-being. As dental professionals strive to achieve ergonomic health, visual acuity is an important aspect to consider. Visual acuity is best described as the degree of clarity or sharpness of vision.2 How well an individual can see is dependent on many variables and will change throughout a lifetime.
Studies indicate a high number of oral health professionals experience some degree of musculoskeletal pain related to their occupation.3,4 While there are many causes of such pain, an individual’s visual acuity may play a role. Optimal visual acuity is vital to the assessment of tissue conditions, evaluating radiographs, and delivering operative care. When visual acuity is compromised, clinicians may compensate in a way that could lead to musculoskeletal disorders.1,3,4
Researchers have hypothesized that many in the field of dentistry are unaware of the level of their visual acuity.5 In an attempt to create an accessible way to measure the degree of near vision, researchers developed a unique test for practicing dentists and dental students to evaluate visual acuity using a $5 bill.5 In this test, research participants were asked to read the first five words of each line in the Lincoln Memorial frieze printed on the bill under a dental operating light at a distance of 300 mm, or approximately 12 inches. The ability to read six or more words in the memorial frieze indicated that visual acuity was within the average range of clinicians. If none of the words could be read, concurrent vision tests verified the individual’s visual acuity was lower than the median score of the research participants. The authors concluded this was an easy way to determine if additional aids were required for practice.5
Oral health professionals commonly report pain in the neck and shoulders.1,2,6 While many variables contribute to this, bending the head closer to the patient to obtain better vision could be a contributing factor.1,2 Studies have confirmed that tilting the head forward greater than 20° for the majority of a workday leads to an increased risk of neck pain.6 The forward head posture that clinicians commonly adopt can cause the muscles, ligaments and soft tissue to permanently adapt to this posture, leading to postural deformity. The cervical spine can also be affected by this forward head posture.7 Providers need to be aware of the recommended positioning during treatment, which is a head tilt between 0° and a maximum of 20°.1,7 It is also important to attempt to maintain this neutral posture for the majority of the workday.6,7
Another aspect of visual acuity is the effect of aging. As we age, the lens of the eye becomes thinner and less flexible, which makes it difficult to focus on nearby objects. This is referred to as presbyopia.8 In addition to changes in near vision, many individuals find that presbyopia causes an increased need for light and a heightened sensitivity to glare.8 A study placed dentists in a simulated dental environment to determine their near visual acuity. The results indicated a wide disparity in the quality of near vision among the research participants, with increasing age playing a major factor in the loss of visual acuity.9 This loss of vision may contribute to headaches and eyestrain. Additionally, clinicians tend to compensate by adopting unhealthy working postures.1,2
STRATEGIES FOR IMPROVING VISION
Research indicates that magnification aids are useful in enhancing visual acuity.9–11 A study examined the visual acuity of dental hygienists and dental hygiene students in clinical settings.10 Visual acuity was measured with and without magnification. The authors concluded that magnification should be used by all operators to improve visual acuity, and is especially important for those older than 40.10 Other studies indicate that many dental professionals with visual deficiencies are not aware of the magnitude of their loss. These studies concluded that the use of magnification improved visual acuity and helped minimize the effects of aging.11 It was recommended that dental professionals schedule eye exams every two years to track any changes in vision.12
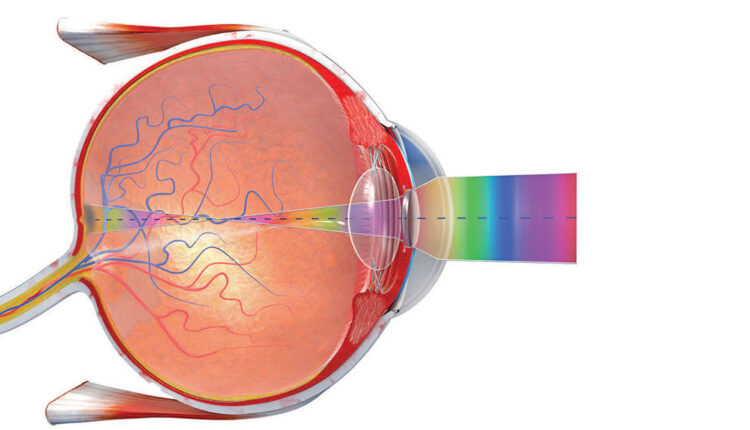
While illumination can be used to improve visual acuity,13,14 the consensus is that over-illumination can be as harmful to the human eye as inadequate lighting. When evaluating products for ergonomic design, it is helpful to review how light affects vision. As light enters the eye through the cornea, the iris dilates or constricts, controlling the amount of light that enters the pupil. The light is refracted to the back of the eye, where the image is focused. Adequate light makes it easier for the eye to focus, which improves visual acuity.13 However, if too much light is present, the eye’s natural defenses can no longer block the additional incoming light, and glare results. This leads to eye discomfort and could be harmful for clinicians in the long term.13
Many items are available that enhance visibility by introducing illumination to the oral cavity. Light sources have been attached to handpieces, mirrors and suction devices, although these should be evaluated to ensure they do not create additional glare. The use of retraction and isolation devices offers enhanced access and allows more light to illuminate the field of operation. The use of retraction devices and mirrors, combined with high-evacuation suction, is helpful in practice. Another useful product is the high-definition dental mirror.
Often, clinicians find the addition of light-emitting diode (LED) headlights to magnification frames enhances illumination and improves ergonomics.13 The most common headlights are coaxial LED systems that direct a beam of light to the working area, following the head position of the operator to eliminate shadowing.13,14 These products can vary considerably in quality, however, and should be carefully evaluated before purchasing. A generous trial period by the manufacturer and customer follow-up are essential. When investigating various products, clinicians should be aware of several factors that will help achieve the desired outcome.
For example, it is important to evaluate the intensity of the light produced and ensure it can be adjusted to compensate for operator preference. The light must be uniform and clear at the operator’s working distance. Lights that emit a beam with a hazy outline are not recommended. Color temperature, which is the color of light produced, is another important consideration. Light sources close in color to neutral sunlight are considered the safest options.13,14 Batteries that control the light source can be corded or attached to the headlight. For ease of use, the power switches on the batteries should be easy to access.14 In order to minimize cross contamination, a good solution is to purchase lights that can be activated by motion sensors or through fabric.
CONCLUSION
Maintaining visual acuity and improving body mechanics will help practitioners maintain ergonomic health and provide effective care. When investigating products designed enhance vision, clinicians need to evaluate whether these products improve vision without causing undue eye damage. Oral health professionals should also develop an awareness of how vision changes throughout their career, and make accommodations as necessary to maintain optimal clinical performance.
REFERENCES
- Murphy DC, ed. Ergonomics and the Dental Care Worker. Washington, DC: American Public Health Association; 1998:56.
- American Optometric Association: Visual Acuity: What is 20/20 Vision? Available at: https://www.aoa.org/patients-and-public/eye-and-vision-problems/glossary-of-eye-and-vision-conditions/visual-acuity. Accessed August 11, 2020.
- Hayes M, Smith DR, Cockrell D. An international review of musculoskeletal disorders in the dental hygiene profession. Int J Dent Hyg. 2010;60:343–352.
- Morse T, Bruneau H, Michalak-Turcotte C, et al. Musculoskeletal disorders of the neck and shoulder in dental hygienists and dental hygiene students. J Dent Hyg. 2007;81:3.
- Perrin P, Eichenberger M, Neuhaus KW, Lussi A. A near visual acuity test for dentists. Oper Dent. 2017;42:581–586.
- Ariens GA, Bongers PM, Douwes M, et al. Are neck flexion, neck rotation, and sitting at work risk factors for neck pain? Results of a prospective cohort study. Occup Environ Med. 2001;58:200–207.
- Valachi BS. Practicing Dentistry Pain-Free: Evidence Based Ergonomic Strategies to Prevent and Extend Your Career. Portland: Posturdontics Press; 2008:56,64.
- Merck Manual. Eye Disorders. Available at: merckmanuals.com/professional/ SearchResults?query=eye+disorders. Accessed August 11, 2020.
- Eichenberger M, Perrin P, Neuhaus K, Bringolf U, Lussi A. Visual acuity of dentists under simulated clinical conditions. Clin Oral Invest. 2013;17:725–729.
- Eichenberger M, Perrin P, Sieber KR, Lussi A. Near visual acuity of dental hygienists with and without magnification. Int J Dent Hyg. 2018;16:357–361.
- Eichenberger M, Perrin P, Neuhaus K, Bringolf U, Lussi A. Influence of loupes and age on the near visual acuity of practicing dentists. J Biomed Opt. 2011;16:035003.
- Burton JF, Bridgman GF. Presbyopia and the dentist: the effect of age on clinical vision. Int Dent J. 1990;40:303–312.
- Chang BJ. Ergonomic benefits of surgical telescope systems: selection guidelines. J Calif Dent Assoc. 2002;30:161–169.
- Holt E, Hoebeke R. Shine a light. Dimensions of Dental Hygiene. 2012;10(9):25–27.
The author has no commercial conflicts of interest to disclose.
From Decisions in Dentistry. September 2020;6(8):24-25.


