
Safety Protocols Using Implant Checklists
Incorporating implant safety checklists into clinical practice can help reduce the risk of error and improve outcomes.
can help reduce the risk of error and improve outcomes.
In 1999, the U.S. Institute of Medicine published a report, “To Err Is Human,” which revealed that more Americans die annually due to medical errors than traffic accidents.1 This report, among others, led to the new discipline of patient safety, and helped galvanize efforts to promote a culture of safe practice among the health care professions. While many of these patient safety-related efforts have been focused on medicine, dentistry, by comparison, has been a relative latecomer to the concept of a safety-based practice.2 Using implant checklists as an example, this article will examine how patient safety can be addressed in dental settings to help raise the level of care provided.
Yamalik and Perea Pérez2 discussed several “peculiarities of patient safety in dentistry” that serve as barriers for development of a safety culture. For one, iatrogenic injury to patients is typically milder in dentistry compared to medicine because dental procedures tend to be less invasive. Deaths related to dental procedures are relatively rare. In addition, dental care is largely unstructured and often provided by dentists who practice in relative isolation. This structure limits the dissemination of knowledge regarding adverse events, as well as their analysis. Lastly, dentists have no incentive to report adverse events, considering that most dental procedures take place in private practice settings. This is particularly true when the event may reflect a professional error and/or have negative financial consequences.
There are few statistics available on patient safety incidents (PSI) — such as near misses or adverse events — occurring in dental practice. A large portion of the available information on PSI stems from case studies, which range from less severe events, such as local allergy to dental materials, to life-threatening events, such as airway obstruction or even death.3,4
In terms of dental implants, recent advances in site development and placement techniques have made the practice of implant dentistry more effective, but also more dangerous.5,6 The American Academy of Implant Dentistry estimates that approximately 3 million Americans have implants, and this number is growing by 500,000 annually.7 Despite the rapid expansion, several safety and quality-of-care issues need to be addressed to reduce the associated risks.8
Experience in placing implants varies widely among clinicians.9–14 In terms of quality of care, implant survival rates are relatively well documented.15,16 For example, a meta-analysis by Pjetturson et al15 revealed that although dental implants placed by experienced surgeons had a 95% survival rate within five years of placement, 39% of these surviving implants were associated with at least one complication. Common problems, such as those involving prosthetics, may become more serious when clinician experience is limited.16 For example, implants placed by inexperienced surgeons were shown to be twice as likely to fail as those placed by experienced surgeons.17 When clinicians make iatrogenic errors — especially those leading to patient morbidity and mortality — they face loss of licensure and other legal ramifications.18 In 2012, 11% of medical malpractice payments were against dentists.19,20
Understanding how errors occur is paramount to patient safety, and several models have been proposed to conceptualize this. Reason’s “Swiss cheese” model focuses on built-in preventive mechanisms that may act as barriers to errors.21 In actual practice, each barrier is more like a slice of Swiss cheese, meaning that while there may be holes, collectively, they help prevent errors. Nevertheless, when several minor errors occur in concert, they can trigger an adverse event.
Another way to think about errors is to consider the buildup of risks that eventually leads to a PSI. Sometimes failures in organizational systems can result in human errors — such as structure that is too complex, inappropriate automation, reliance on memory for optimizing information systems, lack of physical/engineering constraints, and the effects of change on systems.22
PUT A PLAN IN PLACE
Developing a patient-centered safety climate is critical to preventing PSI.23 The goal is not to identify individuals to blame, but to find system mistakes and prevent errors from occurring.2 Yamalik and Perea Pérez2 proposed the adoption of steps to encourage an effective safety culture. Table 1 provides a list of these steps.2
 The World Health Organization (WHO) published a surgical safety checklist (available HERE). This checklist was developed to reduce human error during surgical procedures and is modeled after the airline industry’s in-flight safety checklists.24–26 It includes three phases: sign in before induction of anesthesia; time out before skin incision; and sign out before the patient leaves the operating room. The operating team checks off each item before proceeding to the next phase.
The World Health Organization (WHO) published a surgical safety checklist (available HERE). This checklist was developed to reduce human error during surgical procedures and is modeled after the airline industry’s in-flight safety checklists.24–26 It includes three phases: sign in before induction of anesthesia; time out before skin incision; and sign out before the patient leaves the operating room. The operating team checks off each item before proceeding to the next phase.
With complex clinical decision-making systems, health care practitioners face two main challenges: fallibility of memory and attention, and the inadvertent skipping of clinical steps.24,27 Despite receiving extensive training, some clinicians assume that certain steps may not always be essential.24 This is why making key procedures explicitly routine is critical. In addition, checklists provide clinicians with clear reminders of the minimum steps necessary for the procedure, with the aim of avoiding or catching any significant procedural errors.24
Checklists provide clinicians with clear reminders of the minimum steps necessary for the procedure, with the aim of avoiding … procedural errors
key takeaways
- Developing a patient-centered safety culture is critical to preventing patient safety incidents.23 The goal is to prevent errors.2
- Dental professionals face two main challenges with complex clinical decision-making systems: fallibility of memory and attention, and the inadvertent skipping of clinical steps.24,27 This is why making key procedures explicitly routine is critical.
- Checklists provide clinicians with reminders of the minimum steps necessary during implant procedures.
- An expert panel notes 20 items as essential elements of an implant safety checklist; these items are arranged in three phases: treatment planning, intraoperative and postoperative.
- Customizing the checklist to fit the practice setting is one key to success. Testing the checklist on a small scale and then making further modifications is another helpful approach.
- The expert panel also recommends the use of appropriate diagnostic aids in implant cases — such as radiographs and cone beam computed tomography — to help identify key anatomical structures.
- Obtaining signed consent from patients for any proposed treatment will help protect clinicians in case of possible legal action.
DENTAL IMPLANT CHECKLIST
As dental implant placement is more akin to medical surgical procedures than routine dental procedures, Christman et al34 created a preliminary surgical safety checklist for dental implant placement.34–36 The expectation was that dental practitioners could then customize the framework based on individual practice needs. In the following sections, the process by which the checklist was created will be briefly discussed, and key findings will be summarized.
The process involved obtaining consensus from a panel of experts to create a checklist that would provide a preliminary framework for minimizing risks. The authors administered the survey to 24 board-certified periodontists, who came to a consensus on the appropriate clinical steps for the successful restoration of edentulous areas with dental implants. The panel ultimately determined that 20 items were essential to the checklist, and arranged them in three phases: treatment planning, intraoperative and postoperative (Table 2). The broad consensus among the panelists was:
- In preparing treatment plans for patients, clinicians should verify periodontal stability, conduct a proper diagnostic workup, and engage in effective communication with restorative partners.
- Important steps include thoroughly reviewing the patient’s medical and dental history before placing implants, and using safety checklists.
- Postoperative care should include appropriate communication with patients and restorative partners.
In terms of treatment planning, the panelists note that verification of patients’ periodontal stability is critical, and they emphasize the need for thorough clinical and radiographic evaluation to establish this stability. The experts also encourage the use of appropriate diagnostic aids — such as radiographs and cone beam computed tomography — to help identify key anatomical structures. The consequences of failing to identify and protect such structures are documented extensively in the literature. In a meta-analysis of complications related to implant placement, the most common surgical problems were associated with hemorrhage.12 In addition, the incidence of persistent or long-term altered sensation of the mental nerve after implant surgery varies from 1% to 43%.37,38
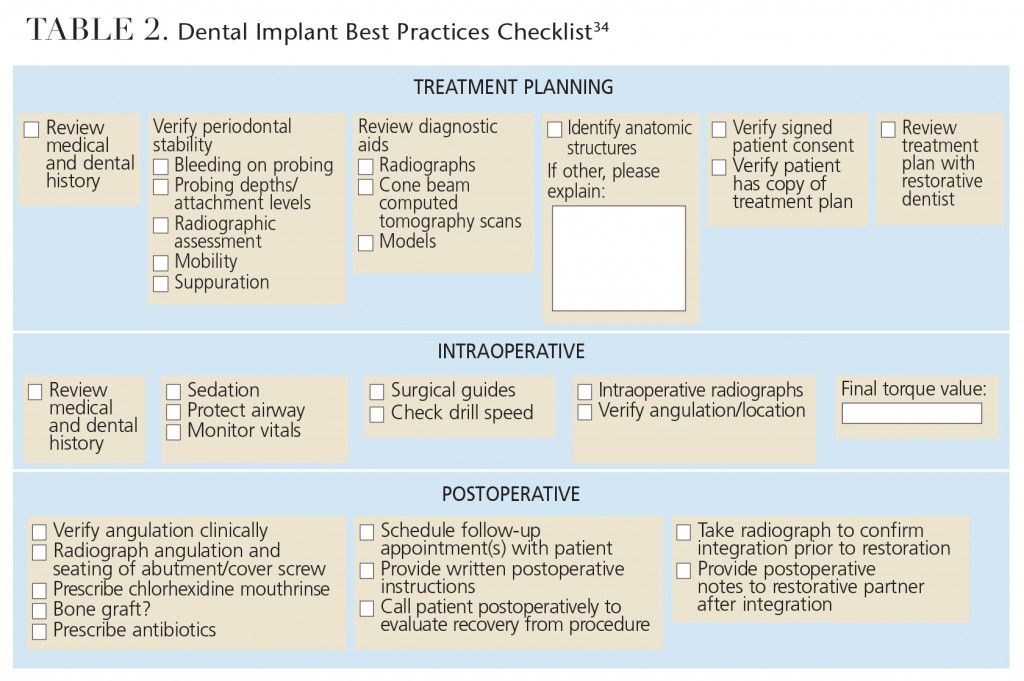
The panel points out that reviewing the patient’s medical and dental history is critical to preventing medical emergencies, and it emphasizes the need to identify relative or absolute contraindications to implant placement. The panelists also suggest that formal treatment plans should be determined for complex cases, and recommend obtaining signed consent from patients for any proposed treatment in order to protect clinicians in case of possible legal action.
Following a prescribed, standardized safety checklist may prove useful in reducing errors associated with implant placement
In terms of intraoperative steps, all panelists concur that a review of current medications and an exploration of any changes to the patient’s dental or medical history must be done on the day of surgery. They assert that protecting the airway is critical, but offer the caveat that achieving this goal may be difficult due to space restrictions. The dental literature contains reports of sporadic occurrences of surgical instrument aspiration and associated life-threatening complications.14,39 Consequently, the expert panel advocates the use of safety measures, such as placing gauze at the back of the throat, and emphasizes the importance of monitoring vital signs during administration of conscious sedation.
Consistent with Greenstein and colleagues,40 several experts suggest that sound clinical judgment and evaluation of bone quality are the most important factors in determining drill speeds and torque values, but the panel did not reach consensus on these points. Reported causes of initial integration failures include high heat levels due to drilling, and excessive pressure at the implant-bone interface (i.e., greater torque values) at the time of implant insertion, which may result in retrograde peri-implantitis lesions.41
The panelists agree on the essential need for intraoperative radiographs in areas where space is limited due to anatomical constraints. They also suggest that verifying implant angulation and positioning with the help of a qualified assistant, and obtaining final radiographs after implant placement are wise clinical practices.
Tarnow et al42 reported that improper mesio-distal angulation and positioning of implants can lead to lateral bone loss, as well as unacceptable esthetic results. Invasion of the periodontal ligament space and devitalization of adjacent teeth due to improper angulation and positioning are additional concerns related to improper implant placement.43
In terms of postoperative steps, the panelists advocate prescribing chlorhexidine mouthrinses, providing patients with written postoperative instructions, communicating after surgery with restorative partners, making follow-up calls to patients, and scheduling follow-up appointments as essential clinical practices.8,40 Reported postoperative infection rates are low, but such conditions can lead to serious adverse events beyond the oral cavity.8 Consequently, following a prescribed, standardized safety checklist may prove useful in reducing errors associated with implant placement.
While the medical field is making tremendous strides in promoting a safety culture, dentistry still needs to ramp up its efforts
CONCLUSION
While the medical field is making tremendous strides in promoting a safety culture, dentistry still needs to ramp up its efforts. Some of the factors that are instrumental to initiating a safety culture in the dental setting include:
- Creating strategies that promote group orientation and reduce influence of hierarchy.
- Providing and promoting multidisciplinary training as part of dental education and continuing education programs.
- Developing quality improvement tools to gather databases of PSIs, as well as further development, improvement and implementation of checklists.
- Customizing checklists and encouraging ownership by all members of the dental team.
Christman et al34 made the first attempt to design a standardized safety checklist for dental implant surgeries. Further research is needed to evaluate improvements in outcomes. Unique implementation challenges related to dentistry need to be identified. While adverse events may occur less frequently in dentistry than medicine, they can still exert serious consequences on patient health and quality of life. A culture of safety and the use of implant checklists will not only benefit patients, but practitioners, as well.
References
- Kohn LT, Corrigan JM, Donaldson MS. To Err Is Human: Building a Safer Health System. Washington, DC: National Academies Press; 2000.
- Yamalik N, Perea Pérez B. Patient safety and dentistry: what do we need to know? Fundamentals of patient safety, the safety culture and implementation of patient safety measures in dental practice. Int Dent J. 2012;62:189–196.
- Kalenderian E, Walji MF, Tavares A, Ramoni RB. An adverse event trigger tool in dentistry: a new methodology for measuring harm in the dental office. J Am Dent Assoc. 2013;144:808–814.
- Hiivala N, Mussalo-Rauhamaa H, Murtomaa H. Patient safety incidents reported by Finnish dentists; results from an internet-based survey. Acta Odontol Scand. 2013;71:1370–1377.
- Chantler C. The role and education of doctors in the delivery of health care. Lancet. 1999;353:1178–1181.
- Zitzmann NU, Hagmann E, Weiger R. What is the prevalence of various types of prosthetic dental restorations in Europe? Clin Oral Implant Res. 2007;18:20–33.
- American Academy of Implant Dentistry. Dental Implant Facts and Figures. Available at: aaid.com/about/press_room/dental_implants_faq.html. Accessed September 14, 2015.
- Greenstein G, Cavallaro J, Romanos G, Tarnow D. Clinical recommendations for avoiding and managing surgical complications associated with implant dentistry: a review. J Periodontol. 2008;79:1317–1329.
- Stillman N, Douglass CW. The developing market for dental implants. J Am Dent Assoc. 1993;124:51–56.
- Vasak C, Fiederer R, Watzek G. Current state of training for implant dentistry in Europe: a questionnaire-based survey. Clin Oral Implants Res. 2007;18:668.
- Melo MD, McGann G, Obeid G. Survey of implant training in oral and maxillofacial surgery residency programs in the United States. J Oral Maxillofac Surg. 2007;65:2554–2558.
- Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications with implants and implant prostheses. J Prosthet Dent. 2003;90:121–132.
- Bartling R, Freeman K, Kraut RA. The incidence of altered sensation of the mental nerve after mandibular implant placement. J Oral Maxillofac Surg. 1999;57:1408–1410.
- Bergermann M, Donald PJ, àWengen DF. Screwdriver aspiration: a complication of dental implant placement. Int J Oral Maxillofac Surg. 1992;21:339–341.
- Pjetursson BE, Brägger U, Lang NP, Zwahlen M. Comparison of survival and complication rates of tooth-supported fixed dental prostheses (FDPs) and implant-supported FDPs and single crowns (SCs). Clin Oral Implant Res. 2007;18:97–113.
- Kourtis SG, Sotiriadou S, Voliotis S, Challas A. Private practice results of dental implants. Part i: survival and evaluation of risk factors-part ii: surgical and prosthetic complications. Implant Dent. 2004;13:373–385.
- Lambert PM, Morris HF, Ochi S. Positive effect of surgical experience with implants on second-stage implant survival. J Oral Maxillofac Surg. 1997;55(Suppl 5):12–18.
- Edwards A. Dentist sued after tools fall in patient. The Orlando Sentinel. July 19, 2009.
- U.S. Department of Health and Human Services. Data Bank Annual Report: 2002. Available at: npdb.hrsa.gov/resources/annualRpt.jsp. Accessed September 14, 2015.
- Givol N, Taicher S, Halamish-Shani T, Chaushu G. Risk management aspects of implant dentistry. Int J Oral Maxillofac Implant. 2002;17:258–262.
- Reason J. Human error: models and management. BMJ. 2000;320:768–770.
- Bailey E, Tickle M, Campbell S. Patient safety in primary care dentistry: where are we now? Br Dent J. 2014;217:339–344.
- Milne JK, Bendaly N, Bendaly L, Worsley J, Fitzgerald J, Nisker J. A measurement tool to assess culture change regarding patient safety in hospital obstetrical units. J Obstet Gynaecol Can. 2010;32:590–597.
- Gawande A. The Checklist Manifesto: How to Get Things Right. New York: Metropolitan Books; 2010.
- Semel ME, Resch S, Haynes AB, et al. Adopting a surgical safety checklist could save money and improve the quality of care in US hospitals. Health Aff. 2010;29:1593–1599.
- Haynes AB, Weiser TG, Berry WR, et al. A surgical safety checklist to reduce morbidity and mortality in a global population. New Engl J Med. 2009;360:491–499.
- Gawande AA, Thomas EJ, Zinner MJ, Brennan TA. The incidence and nature of surgical adverse events in Colorado and Utah in 1992. Surgery. 1999;126:66–75.
- Van Klei WA, Hoff RG, Van Aarnhem EEHL, et al. Effects of the introduction of the WHO “Surgical Safety Checklist” on in-hospital mortality: a cohort study. Ann Surg. 2012;25:44–49.
- De Vries EN, Prins HA, Crolla RM, et al. Effect of a comprehensive surgical safety system on patient outcomes. New Engl J Med. 2010;363:1928–1937.
- Neily J, Mills PD, Young-Xu Y, et al. Association between implementation of a medical team training program and surgical mortality. JAMA. 2010;304:1693–1700.
- Urbach DR, Govindarajan A, Saskin R, Wilton AS, Baxter NN. Introduction of surgical safety checklists in Ontario, Canada. New Engl J Med. 2014;370:1029–1038.
- Haugen AS, Søfteland E, Almeland SK, et al. Effect of the World Health Organization checklist on patient outcomes. Ann Surg. 2015;261:821–828.
- Pinsky HM, Taichman RS, Sarment DP. Adaptation of airline crew resource management principles to dentistry. J Am Dent Assoc. 2010;141:1010–1018.
- Christman A, Schrader S, John V, Zunt S, Maupome G, Prakasam S. Designing a safety checklist for dental implant placement: A Delphi study. J Am Dent Assoc. 2014;145:131–140.
- Whittle JG, Grant AA, Sarll DW, Worthington HV. The Delphi technique: its use in dental health services research assessed in a study to improve care for elderly mentally ill patients. Community Dent Health. 1987;4:205–214.
- Cramer CK, Klasser GD, Epstein JB, Sheps SB. The Delphi process in dental research. J Evid Based Dent Pract. 2008;8:211–220.
- Ellies LG, Hawker PB. The prevalence of altered sensation associated with implant surgery. Int J Oral Maxillofac Implants. 1993;8:674–679.
- Wismeijer D, Van Waas MAJ, Vermeeren J, Kalk W. Patients’ perception of sensory disturbances of the mental nerve before and after implant surgery: a prospective study of 110 patients. Br J Oral Maxillofac Surg. 1997;35:254–259.
- Worthington P. Ingested foreign body associated with oral implant treatment: report of a case. Int J Oral Maxillofac Implant. 1996;11:679–681.
- Greenstein G, Cavallaro JS Jr, Tarnow DP. Clinical pearls for surgical implant dentistry: Part I. Dent Today. 2010;29:124–127.
- Quirynen M, Mraiwa N, Van Steenberghe D, Jacobs R. Morphology and dimensions of the mandibular jaw bone in the interforaminal region in patients requiring implants in the distal areas. Clin Oral Implant Res. 2003;14:280–285.
- Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71:546–549.
- Sussman HI. Tooth devitalization via implant placement: a case report. Periodontal Clin Investig. 1998;20:22–24.


