Perspective on Bioactive Restoratives
Bioactive materials are taking restorative dentistry one step further by helping to prevent demineralization, promote remineralization, and, when used as a liner or pulp-capping agent, stimulate the formation of dentin.
Bioactive materials are taking restorative dentistry one step further by helping to prevent demineralization, promote remineralization, and, when used as a liner or pulp-capping agent, stimulate the formation of dentin. But before clinicians can decide if a caries-fighting bioactive restorative is appropriate for their case, they need perspective on what these materials do, and how they differ from traditional restoratives.
“It is difficult to define a bioactive material without first classifying what type of material it is,” notes Nathaniel Lawson, DMD, PhD, director of the Division of Biomaterials at the University of Alabama at Birmingham School of Dentistry. Lawson, who has a PhD in biomedical engineering, classifies bioactive restorative materials as either liners/pulp capping agents, or restoratives and cements.
“For example, a bioactive material that is a liner/pulp capping agent would initiate the formation of reparative dentin in the pulp chamber,” he says. A bioactive restorative or cement, on the other hand, offers clinical benefits to tooth structure associated with the restoration. “If a material releases fluoride, calcium or phosphate, it may help prevent demineralization of the tooth and surrounding dentition,” he explains. “This release of ions may also help remineralize any demineralized dentin left at the bottom of a caries preparation. Such a material may also form hydroxyapatite — which, if formed at the interface of the material and tooth, may help seal the restoration. Finally, a bioactive restorative may be antibacterial, as well.”
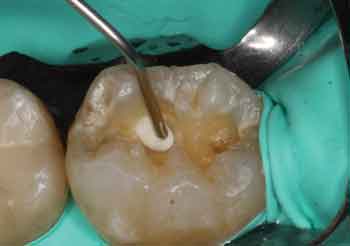 When choosing pulp capping agents, it wouldn’t make sense to use a material that is not bioactive, Lawson asserts. “When the pulp is exposed or nearly exposed, a material should be placed that will stimulate the formation of reparative dentin — which is an obvious indication for a bioactive pulp capping material,” he says. In cases that don’t involve exposure or near exposure, he believes it is up to the clinician’s discretion to choose a bioactive liner. “The disadvantage of a bioactive liner in this situation,” he explains, “is that it may not bond as strongly to the preparation as a layer of resin composite.”
When choosing pulp capping agents, it wouldn’t make sense to use a material that is not bioactive, Lawson asserts. “When the pulp is exposed or nearly exposed, a material should be placed that will stimulate the formation of reparative dentin — which is an obvious indication for a bioactive pulp capping material,” he says. In cases that don’t involve exposure or near exposure, he believes it is up to the clinician’s discretion to choose a bioactive liner. “The disadvantage of a bioactive liner in this situation,” he explains, “is that it may not bond as strongly to the preparation as a layer of resin composite.”
In Lawson’s view, a comparison of the clinical advantages that are gained or lost through the addition of bioactivity helps steer the choice of restorative materials and cements. “For instance, glass ionomers and resin-modified glass ionomers offer high levels of fluoride release, but at the cost of esthetic and mechanical properties,” he notes. “Conversely, some of the resin-based bioactive restoratives provide less ion release, but feature mechanical properties closer to resin composites.”
Recent advances in bioactive restoratives are taking these materials to the next level. One example is a new concept that incorporates bioactive glass into a dental adhesive. “Testing in our laboratory showed that incorporating ion release into the restorative material is more critical than incorporating it into the adhesive; however, combining ion release from the adhesive and restorative is more effective than using either individually,” he explains. “Another new concept is the addition of charged molecules into restorative materials that can break down bacterial walls, which means these materials will resist plaque accumulation.”
When asked what properties he would like to see introduced, Lawson says he looks for a material that interacts favorably with soft tissue. “Clinicians are plagued by carious cervical lesions that extend subgingivally, because restoring these lesions with composite leads to gingival recession,” he says. “A true innovation would be a bioactive restorative that would allow the attachment of soft tissue while also promoting other bioactive benefits.”
From Decisions in Dentistry. September 2021;7(9):46.


