
Role of Chemical and Biological Indicators in Infection Prevention
Proper sterilization monitoring requires a combination approach using mechanical, chemical and biological indicators.
This course was published in the September 2021 issue and expires September 2024. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the regulatory and guidance agencies for infection control in dentistry.
- Describe the instrument processing cycle, as well as the types of sterilizers and monitoring processes used.
- Explain best practices for use of chemical and biological indicators.
While oral health professionals acquire baseline knowledge and meet clinical competencies related to infection prevention during their formal education, continuing education is critical to providing safe care. In today’s practice setting, safe dental visits encompass new COVID-19 protocols, as well as existing infection prevention measures — including verification of sterile instruments. While the U.S. Centers for Disease Control and Prevention (CDC) recommends verifying dental instrument sterility, the Occupational Safety and Health Administration (OSHA) formally requires it. Proper sterilization monitoring includes using a combination of mechanical monitoring, chemical indicators (CI) and biological indicators (BI).1,2 This paper focuses on sterilization processes, including the effective use of CIs and BIs.
As a division of the U.S. Department of Labor, OSHA has been protecting workers since 1971 with the use of mandatory regulations. Employers are legally required to comply with these standards. The Bloodborne Pathogens (BBP) Standard CFR 1910.1030 (exposure to BBP, such as hepatitis B and C and human immunodeficiency virus), Hazard Communication (HAZCOM) Standard CFR 1910.1200 (safety with chemicals), and the Respiratory Protection Standard CFR 1910.134 are the most commonly used and cited OSHA standards in dentistry.3,4 Considered a federal regulatory body, OSHA can investigate and impose fines for lack of compliance with standards.5,6 In 2020, the two most commonly violated OSHA standards in dentistry were the BBP and Respiratory Protection standards, which accounted for 68% of all cited standards.7
The 2003 CDC Guidelines for Infection Control in Dental Health-Care Settings are the most comprehensive guidance for the safe provision of dental treatment.1 An updated summary with checklists was released in March 2016.8 The CDC is an advisory body that provides evidence-based recommendations, but cannot impose fines or enforce its own guidelines (unless specific state boards adopt CDC guidelines, which then become state law). However, CDC recommendations can be enforced when they are related or connected to an OSHA regulatory standard, such as the BBP Standard.
Interim guidance from the CDC was published in response to the COVID-19 pandemic in May 2020 to supplement the 2003 guidelines, and has been updated multiple times since.9 Major highlights or procedural changes/recommendations for dentistry include social distancing, universal source control, prescreening protocols, personal protective equipment, aerosol reduction, and environmental controls.9
The CDC has not issued any new guidance regarding the instrument processing cycle.9 As OSHA standards and CDC guidance remain the same for instrument processing, bear in mind these are the minimal requirements for safe practice.
INSTRUMENT PROCESSING CYCLE
A proper sequence of instrument processing should be followed, as outlined by the CDC, including safe transportation; receiving, cleaning and decontamination; preparation and packaging; sterilization; and storage.1 The CDC recommends safely transporting instruments from the operatory to the sterilization area in a hard-walled container to avoid percutaneous injuries.1 Instrument processing is a multistep procedure that includes cleaning (via an ultrasonic unit, washer, or washer/disinfector — including rinsing and drying); packaging (use of pouches with built-in CIs or placement of CIs inside wrapped cassettes); sterilization; and storage.1
The CDC recommends heat sterilization for all critical and semi-critical items in compliance with the OSHA BBP Standard.1,2 Monitoring the sterilization process using physical means (e.g., watching gauges for time, temperature and pressure), chemical methods (such as color changes on pouches or internal indicators to verify all sterilization parameters are met), and biological monitoring (e.g., regular spore testing with BIs) as suggested by CDC, is critical to ensure proper sterilization parameters are achieved.1
An effective infection prevention protocol requires weekly spore testing.1 Again, CDC recommendations are considered the minimal standard. Best practices may include performing biological monitoring more frequently based on practice needs; for example, high-volume clinics may need to perform biological monitoring more frequently. New ultra-rapid systems that offers 20-minute in-office BI monitoring technology may help clinicians exceed minimal standards. Performing daily monitoring in-office could be time efficient and would exceed current BI monitoring standards.
REGULATORY GUIDANCE FOR STERILIZATION
As noted, effective sterilization monitoring requires a multifaceted approach using mechanical monitoring, as well as CIs and BIs. Several infection control recommendations related to CIs and BIs are outlined in the comprehensive 2003 CDC guidelines, which remain the gold standard in dentistry.1 The CDC guidance is broad and allows for flexibility in the implementation of its recommendations. Dental practices implement these recommendations in myriad ways, as CDC does not provide specific instructions as to how to carry out infection controls tasks. However, this flexibility results in little standardization in dentistry as compared to medicine. There is very little oversight unless infection control breaches are reported.
For healthcare facilities, the Association for the Advancement of Medical Instrumentation (AAMI) provides comprehensive guidance for instrument processing and steam sterilization activities, regardless of the size of the sterilizer or facility. This is a handy resource for all personnel who use steam sterilization.10 In practice, AAMI ST79 represents a comprehensive guidance document used in healthcare facilities and provides standardization and oversight for infection control tasks. It also offers guidance for the operation of sterilizers; standards for decontamination and instrument processing; criteria for steam sterilization; physical standards for instrument processing areas — including sterile storage, staff qualifications, and step-by-step processing guidance; and care and maintenance of all types of steam sterilizers, including for the small tabletop sterilizers frequently used in dentistry.10
Ensuring that sterilizers are functioning properly is critical for safe practice and eliminating the spread of disease. External accrediting bodies in healthcare use AAMI ST79 to ensure standardization of sterilization procedures, as it provides a means for external oversight and reporting. Although AAMI ST79 is not required in dentistry, it is an excellent supplement to OSHA and CDC guidance.

TYPES OF STERILIZERS
Autoclaves are U.S. Food and Drug Administration (FDA)-cleared medical devices that use steam under pressure, and they are the most common sterilizers in dental practice. There are two common types of autoclaves: gravity displacement (Class N) and dynamic air removal (class S or B).1 Gravity displacement units are the most frequently used in dentistry. These sterilizers admit air at the top or side of the chamber and, because steam is lighter than air, gravity forces the heavier air out, exiting through the bottom drain. This passive method requires more drying time. Trapped air or cool pockets can be problematic with gravity displacement sterilizers, so placement of the BI is critical.
Dynamic air removal sterilizers — such as Class S and Class B — use a vacuum pump to remove air from the chamber before steam is emitted. The advantages include nearly instantaneous steam penetration, shorter drying time, and the ability to fully penetrate even the smallest hollow tubing of medical instruments. No matter which type of sterilizer is used, it is critical to let the load cool and dry fully to avoid wicking microorganism into the contents. Wicking is a process that allows bacteria or other contaminants to penetrate the inside contents of a sterilization pouch or pack.
Widely used in Europe and Canada, the European Standard EN 13060 is a strict guideline that defines requirements for small steam sterilizers. Class B sterilizers meet this standard. Although the CDC does not require Class B autoclaves, these units provide high levels of sterility assurance that meet the EN 13060 hollow tube test.10 Manufacturers offer a wide range of autoclaves for clinicians seeking to enhance their infection control practices by using Class B technology.
Some of the latest sterilization technology includes autoclaves that provide the following benefits: upgradeable from a Class S to a Class B with a simple software upgrade, fast cycles completed in 32 minutes, a variety of documentation and traceability options and barcodes, and smart technology. Class B autoclave meets high standards of sterilization. Additional new technology includes a Class B autoclave with a pretreatment cycle that addresses the air in the chamber before the preliminary air removal stage, ensuring the air released back into the ambient air is free from microorganisms and viruses. This technology might provide additional peace of mind. Manufacturers have produced autoclaves that allow faster cycles that deliver dry instruments without wicking. This technology provides closed-door drying (instruments dry without having to monitor and open the door) — allowing more cycles throughout the day — and features an automatic safety shutoff.
STERILIZATION MONITORING
Guidance from CDC and OSHA requires the use of chemical and biological monitoring to ensure sterilization parameters are achieved.1,2 Chemical monitoring is based on the use of indicators. For example, CIs use sensitive material to detect physical conditions, such as exposure time and temperature. These can be external or internal indicators that might change color when exposed to the sterilization process. During the preparation and packaging phase (prior to sterilization), CIs are added to monitor a variety of internal and external parameters to determine if steam has reached the contents inside.10
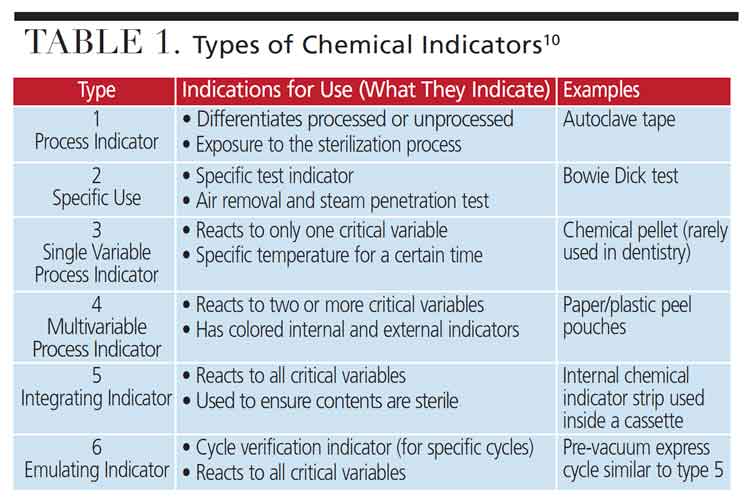
There are six types of CIs according to AAMI ST79 (Table 1).10 Type 1 is the most basic and demonstrates that the item has been exposed to one sterilization process (such as heat) and distinguishes between processed and unprocessed items. Type 1 CIs, such as autoclave tape used to secure wrapped cassettes, measure a single parameter.
Type 2 is a specialty indicator used for specific tests, such as the Bowie Dick test, which measures the air-removal performance in prevacuum steam sterilizers. These indicators test for the presence of air in the steam sterilizing chamber. A positive test indicates air leakage, which inhibits the conditions necessary for sterilization. This test is performed at the start of the day to ensure the autoclave is functioning optimally.
Type 3 is a single parameter indicator designed to respond to only one variable of the sterilization process, such as time or temperature. The FDA does not recognize this type.
Type 4 indicators are more accurate. They react to two or more critical parameters of the sterilization process (such as time and temperature) and indicate exposure to the sterilization cycle. Pouches are a great example of Type 4, as they have internal and external markers that change color when exposed to sterilization parameters. Pouches must be examined after sterilization to ensure the parameters were met (e.g., color change). There is debate whether to place the pouch’s paper side or plastic side up in the autoclave. It is ideal to stack pouches side to side in a pouch rack for better steam penetration,1,10 but it is always best to consult the manufacturer’s instructions on proper placement without a rack.
Type 5 integrating indicators are designed to react to all of the critical variables of the specific sterilization process (time, temperature and pressure). They are similar to BIs, but the Type 5 integrating indicator does not contain live bacterial spores and should not be used as a substitute for a BI. Integrating indicators may be used as internal CIs, and can also be employed as process challenge devices to monitor and release nonimplant loads. In certain situations, the results of the Type 5 can be used to release an implant before the BI result is available. Type 5 integrators are used inside a cassette to ensure the contents inside are sterile.
Type 6 emulating indicators are designed to react to all critical variables of a specified sterilization cycle. They should only be used in the specific cycle for which they are labeled. For example, one of the available Type 6 CIs is labeled for use in a prevacuum, express cycle. This indicator can be used only in that cycle. Type 6 CIs do not contain spores and are not substitutes for BIs. They can be used to release implant loads while waiting for a biological spore test.10
Best practices with CIs depend on the type of packaging used. With pouches, they should meet the following requirements:1 Type 4, compatible with the autoclave, and visibly labeled with nontoxic ink or pencil on the nonporous side with the date of sterilization, sterilizer number, and the cycle number to facilitate traceability. If cassettes are used, Type 5 integrating indicators must be inside each cassette, wrapped using FDA-approved wrap, and secured with Type 1 tape.1 Logging all activity related to sterilization is another important consideration. The CDC recommends keeping a log that contains information related to mechanical, chemical and biological monitoring (Table 2).1
BIOLOGICAL INDICATORS
Also known as spore tests, BIs are used to monitor the functioning of autoclaves by testing for the inactivation of highly resistant microorganisms.1 An inactivated BI indicates pathogens in the load have been killed, thus verifying sterilization. In fact, BI testing is the only way to ensure that sterility has been achieved.1
Two methods of BI testing are available: in-office incubation and mail-in services.1 Mail-in services are easy to use and inexpensive. A BI strip is placed in an autoclave cycle and sent by mail for incubation and results. Correct placement of the BI in the autoclave is critical to ensure steam has penetrated the most challenging area of the sterilizer. It is best to place the BI in the center of the load, as this is where cool air pockets exist in gravity displacement sterilizers.1,10 However, it is best to place the BI near the door in Class S or Class B units (dynamic air removal sterilizers).10
A potential downside with mail-in BI testing is that notification of failed tests might be delayed due to mail delivery issues. By the time the practice receives a failed spore test notification, several loads of instruments may have been run and may not be sterile. Tracking and retrieval of these instruments might prove difficult.
In-office incubation methods of BI may be preferred to ensure verification of sterility in a timelier manner (less than 24 hours); however, the up-front cost may be higher. In this process, a test vial is placed in a regular autoclave cycle. Next, the vial is incubated for a specified period before comparing the color change. If a test fails, a new test must be completed. Most BI test failures are due to operator error, such as overloading the sterilizer, improperly loading cassettes and pouches, and incorrect BI placement. Truly failed spore tests can be quicker to flag, retrieve, and log with in-office incubation methods. Table 3 outlines troubleshooting tips for BI testing.
Advantages of in-office incubation include the rapid nature of testing, a printout of the results, ability to test several vials at a time from different types of autoclaves, and the capacity to test more frequently than CDC recommendations (which is at least weekly).1 The risks of performing BI testing on a minimal weekly basis include the potential for disease transmission and inability to retrieve potentially unsterile instruments in a timely fashion. Best practice may include performing BI more frequently, such as daily or multiple times per day, depending on the practice volume and types of loads.
BEST PRACTICES
Guidance from the CDC and OSHA dictates the use of chemical and biological monitoring to ensure sterilization parameters are achieved.1,2 The importance of regular BI testing is critical to safe care. Oral health professionals can ensure safe dental visits by adhering to current infection control guidance. Exceeding minimal standards may be considered best practice.
As one example, high-volume practices may consider performing BI testing more frequently. Dentistry has had to adapt to evolving infection control challenges during the COVID-19 pandemic. Oversight mechanisms in the medical profession — such as the use of AAMI ST79 by external accrediting bodies to ensure infection prevention measures are in place — may need to be considered for dentistry.
References
- Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection control in dental health-care settings — 2003. MMWR Recomm Rep. 2003;52:1–66.
- Occupational Safety and Health Administration. Bloodborne Pathogens Standard 1910.1030. Available at: osha.gov/pls/oshaweb/owadisp.show_document?p_table=standards&p_id=10051. Accessed August 3, 2021.
- Occupational Health and Safety Administration. Hazard Communication 1910.1200 Standard. Available at: osha.gov/laws-regs/regulations/standardnumber/1910/1910.1200. Accessed August 3, 2021.
- Occupational Health and Safety Administration. Respiratory Protection Standard 1910.134. Available at: osha.gov/laws-regs/regulations/standardnumber/1910/1910.134. Accessed August 3, 2021.
- Occupational Safety and Health Administration Enforcement. Available at: osha.gov/dep/index.html. Accessed August 3, 2021.
- Occupational Safety and Health Administration. Fine Fact Sheet. Available at: osha.gov/OshDoc/data_General_Facts/factsheet-inspections.pdf. Accessed August 3, 2021.
- Occupational Safety and Health Administration. Commonly Cited Standards. Available at: osha.gov/pls/imis/citedstandard.naics?p_esize=&p_state=FEFederal&p_naics=621210. Accessed August 3, 2021.
- U.S. Centers for Disease Control and Prevention. Summary of Infection Prevention Practices in Dental Settings: Basic Expectations for Safe Care. Available at: cdc.gov/oralhealth/infectioncontrol/summary-infection-prevention-practices/index.html. Accessed August 3, 2021.
- U.S. Centers for Disease Control and Prevention. Guidance for Dental Settings. Interim Infection Prevention and Control Guidance for Dental Settings During the COVID-19 Response. Available at: cdc.gov/coronavirus/2019-ncov/hcp/dental-settings.html Accessed August 3, 2021.
- Association for the Advancement of Medical Instrumentation. ANSI/AAMI ST79. Comprehensive Guide to Steam Sterilization and Sterility Assurance in Health Care Facilities. Available at: aami.org/detail-pages/press-release/updated-steam-sterilization-standard-for-healthcare-facilities-st79-now-available. Accessed August 3, 2021.
From Decisions in Dentistry. September 2021;7(9):40-43.





