Pediatric Sedation Principles
These clinical insights into sedation and general anesthesia will facilitate the treatment of children who have low tolerance to dental care.
This course was published in the May 2016 issue and expires 05/31/19. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
OBJECTIVES
After reading this course, the participant should be able to:
- Define the continuum of sedation and anesthesia.
- Identify the methods used to provide sedation and general anesthesia.
- Discuss the clinical guidelines for administering sedation and anesthesia.
- List the most common agents used to achieve sedation.
Some patients, particularly children, may require sedation before dental treatment.1 The goals of sedation include patient comfort and reduced anxiety. In addition, the use of appropriate sedation techniques will not only facilitate the provision of high-quality dental care, it may also encourage a positive view of dental treatment from otherwise fearful patients.2,3 Dentists who wish to provide sedation must undergo specific and extensive training, and also be certified by the state in which they practice.
Sedation and general anesthesia can be conceptualized as a continuous spectrum of nervous system depression. At one end of the spectrum is local anesthesia, wherein sensory impulses are blocked in a fully conscious patient. At the other extreme is general anesthesia. In between are varying levels of sedation, which are classified by level of consciousness, response to command, airway patency, ventilation, and cardiovascular function. For dental procedures, local anesthesia is usually combined with sedation, and is often used even if general anesthesia is planned.
Minimal Sedation — Patients respond normally to verbal commands during this drug-induced state; although cognitive function and coordination may be impaired, ventilatory and cardiovascular functions are unaffected.4–6
Moderate Sedation — During this drug-induced depression of consciousness, patients respond purposefully to verbal commands, either alone or accompanied by light tactile stimulation. Medications and techniques should carry a margin of safety that’s wide enough to make unintended loss of consciousness unlikely. With this modality, no interventions are required to maintain a patent airway, and spontaneous ventilation is adequate. In addition, cardiovascular function is usually maintained.4–6 Purposeful response varies according to the patient’s chronological and developmental age; for example, older patients may respond to “squeeze my hand,” whereas younger children may only cry at times. What is not considered purposeful, however, is reflex withdrawal from a painful stimulus without any other reaction.5
Deep Sedation — During this drug-induced depression of consciousness, patients cannot be easily aroused, but respond purposefully following repeated or painful stimulations. A patient’s ability to independently maintain ventilatory function may be impaired; what’s more, the individual may require assistance in maintaining a patent airway, and spontaneous ventilation may be inadequate. Cardiovascular function is usually normal, however.4–6
General Anesthesia — During this drug-induced loss of consciousness, patients are not arousable, even by painful stimulation. The ability to independently maintain ventilatory functions is often impaired. Patients frequently require assistance in maintaining a patent airway, and positive pressure ventilation may be required due to depressed spontaneous ventilation or drug-induced depression of neuromuscular function. In addition, cardiovascular function may be impaired.4–6
MODES OF SEDATION
There are numerous methods in which to administer medications to produce sedation and anesthesia, and any route of administration can lead to any level of sedation along the continuum. Routes of drug administration are generally categorized as enteral or parenteral. Enteral refers to administration via the gastrointestinal tract, and consists of oral and rectal routes. Parenteral routes involve the direct delivery of the drug into the systemic circulation and do not involve the gastrointestinal tract. These include administration into veins (intravenous, or IV), muscles (intramuscular, or IM), tissues between the skin and muscles (subcutaneous), the nose (intranasal), or via other routes, such as into bone marrow (intraosseous). The parenteral route also comprises drugs that are absorbed into the vasculature after being inhaled.
The oral route is the most common, and is often the most acceptable to patients. It is convenient, noninvasive and economical. Oral medications are subject to metabolism in the gut and liver before reaching the systemic circulation. Known as first-pass metabolism, this means that less of the drug reaches the circulation than is consumed, and there is a lag time between administration and action. Furthermore, the amount of medication actually absorbed varies between individuals, and food and other medications can interact to increase or decrease the drug’s availability for systemic circulation.7 Because a drug’s influence is difficult to foresee, the lowest effective dose should be administered and adequate time allowed after dosing, so drug effects and any side effects can be observed.8
The IV route is also a common pathway for drug administration. Medications given in this manner avoid first-pass metabolism, and action can be rapid. Pharmacological effects are easier to predict in terms of onset, maximum effect and duration, which enhances the ability to titrate the drug.7 Titration allows for a more individualized approach to sedation, and may also increase safety and effectiveness. However, IV medications are subject to drug interactions during metabolism that may decrease or prolong a drug’s action; in addition, the IV route is invasive, may be painful, and requires extra training on the part of the practitioner.
The IM route is frequently used in sedation and general anesthesia. In pediatric patients, the medication is generally injected into the thigh (vastus lateralis) or shoulder (deltoid) muscles. First-pass metabolism is avoided, and the drug is absorbed into the vasculature in a fairly predictable and uniform manner. Onset of action is less rapid than IV injection, and the absorption is spread out, so the duration of action tends to be longer.7 The IM route may require less technical skill on the part of the practitioner than IV cannulation. This route can be painful and locally irritating, and only a certain volume of medication can be injected at each site, depending on the size of the musculature. It is not advisable to attempt titration via the IM route; in addition, some drugs are not appropriate for IM injection.
The inhalation mode depends on absorption of the gas into the vasculature of the respiratory system. First-pass metabolism is avoided, and onset is rapid. As gases are minimally metabolized in general, the cessation of action occurs by redistribution of the gases out of the blood and into the lungs for exhalation.9 When delivered by nasal hood or face mask, the administration of gases by inhalation can be diluted if the equipment is poorly fitting or the patient will not tolerate it.9 During general anesthesia, gases are typically delivered more directly to the lungs via an endotracheal tube or supraglottic device.
CLINICAL GUIDELINES
As the popularity of office-based sedation and general anesthesia increases, so, too, do instances of tragic outcomes. Children are particularly vulnerable to sedative depressant effects on airway patency, protective reflexes and respiratory effort.5 Respiratory distress can quickly lead to cardiac compromise. The key to minimizing risk is careful and thorough preparation.
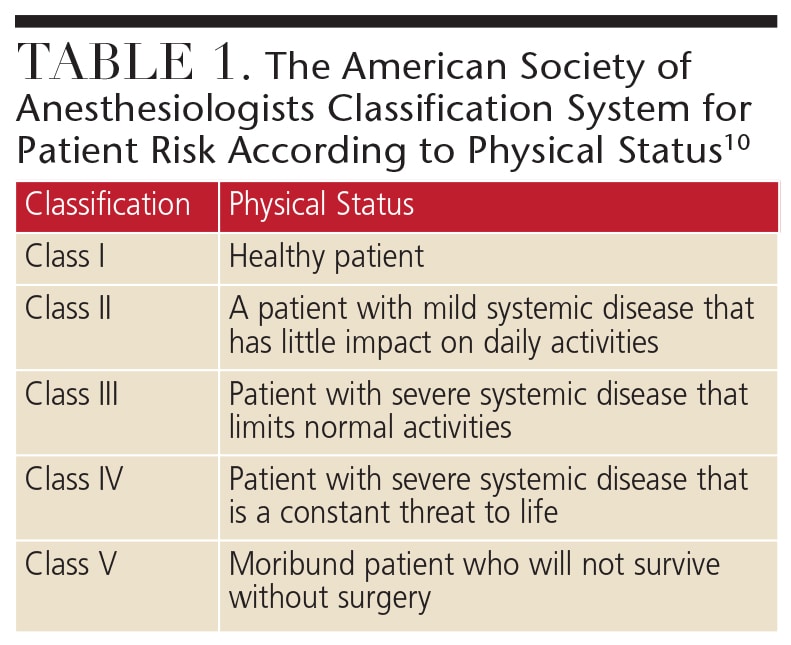
For any level of sedation, preparation begins with a complete evaluation that takes into account a patient’s age and weight, allergies and medication usage; medical history (including surgeries/anesthesia); family medical history; baseline vital signs; a physical examination focused on the heart, lungs and airway; and appropriate consultations with primary care physicians and specialists based on the patient’s underlying medical conditions. This evaluation will help determine whether the patient is a suitable candidate for sedation. The American Society of Anesthesiologists created a useful tool for categorizing patient risk according to physical status (Table 1).10 In the case of office-based sedation for children, patients in classes I and II are generally considered appropriate candidates, whereas Class III patients require additional medical consultation and health improvements prior to considering sedation.

Diet is an important aspect of presedation preparation. Sedative medications have the potential to impede protective airway reflexes, especially as the patient moves deeper along the anesthesia continuum. If a child vomits and is unable to protect his or her airway, the vomitus can be aspirated into the lungs. This is a potentially serious, or even deadly, complication that can require prolonged hospitalization. To help minimize this risk, certain dietary guidelines should be followed to prevent patients from presenting for sedation with full stomachs. For healthy patients, the recommendations for minimum time before sedation are as follows: clear liquids are acceptable up to two hours before sedation; breast milk, four hours; formula and cow’s milk, six hours; and solid food, eight hours.5
The dental office must be adequately prepared for emergencies, according to the scope of their practice and training. This includes size-appropriate tools for managing the airway, IV catheters and fluids, suction devices, and rescue medications. An oxygen delivery system capable of positive pressure ventilation and an automated external defibrillator must be available.5 An emergency protocol should be in place and periodically reviewed. During an adverse event, the sedation team is responsible for stabilizing the patient until emergency medical help arrives.
The majority of emergencies in healthy children undergoing sedation are airway related. When a patient is sedated, the muscles responsible for maintaining airway tone relax, and the soft tissues surrounding the airway can collapse, causing airway obstruction. Children are more susceptible than adults due to the orientation and size of their airways. Airway obstruction can often be treated by providing a chin lift or a mandible thrust while administering supplemental oxygen. If ineffectual, an airway adjunct can be promptly placed orally or nasally to splint open the airway. In pure airway obstruction, the patient will continue to make respiratory effort but needs help opening the airway to allow airflow. In this way, airway obstruction is distinct from respiratory depression. The latter occurs as a result of medication effects on the respiratory drive. Simply opening the airway will not treat respiratory depression; rather, if a patient is not ventilating adequately, the provider must manage the patient’s breathing. This is where positive pressure ventilation becomes especially relevant. Often, positive pressure ventilation is provided by a face mask attached to a self-inflating bag via a one-way valve connected to an oxygen source.11 Obstruction and respiratory depression can occur together, so if positive pressure ventilation is required, it is wise to concurrently open the airway. If the patient still cannot be ventilated, more advanced airway management is required in the form of a supraglottic device or endotracheal tube. While changes to ventilation and airway patency, by definition, should not occur during minimal or moderate sedation, patients can easily slip into more profound levels of sedation than anticipated. Furthermore, airway obstruction can occur as the patient relaxes or if the patient’s posture changes, including the position of the mandible.8 Providers must be able to manage patients who move beyond the planned level of sedation.
During sedation, the patient’s physiological condition must be observed constantly. For example, patients under moderate sedation should have their oxygen saturation, heart rate, response to sedation, respiratory rate, and blood pressure closely monitored. During deep sedation or general anesthesia, continuous measurements of exhaled carbon dioxide levels, heart function via electrocardiogram (EKG), and core body temperature are required.4–6 Because changes in exhaled carbon dioxide (as monitored through capnography, for example) can signal respiratory compromise before a pulse oximeter can, monitoring carbon dioxide levels is also encouraged during moderate sedation. Similarly, EKG monitoring is helpful when treating patients with cardiovascular disease undergoing any level of sedation. All vitals should be documented in a time-oriented sedation record, which should also include the names, routes, dosages, and administration times of all medications used, including oxygen and inhaled agents.4–6
Once the dental procedure is completed, the patient enters a period of recovery. The recovery area requires immediate access to equipment for positive pressure ventilation and suction. Blood pressure, heart rate, oxygenation, and level of consciousness should be continually monitored until the patient has met the criteria for discharge. At discharge, the patient should be awake and back to the presedation level of cognition and activity. Cardiopulmonary function should be at baseline, and airway patency should be maintained.4–6 Postoperative pain, nausea and vomiting, and bleeding need to be controlled.6
COMMON SEDATIVE AGENTS
Numerous medications are available for dental sedation. The differences between the drugs in terms of onset, duration and side-effect profile help determine which regimen is best suited for each patient. Sedatives may decrease fear and anxiety, for example, but they do not diminish pain. For this reason, adequate local anesthesia is still an integral part of the dental plan when using sedation. As local anesthetics are nervous system depressants, they can potentiate the sedative and respiratory depressant actions provided by sedation medications, which can have catastrophic consequences in pediatric patients undergoing sedation. It is therefore prudent to keep dosages of local anesthetics below the recommended maximums.
Chloral hydrate is a central nervous system (CNS) depressant that was historically popular for pediatric sedation. Because chloral hydrate has many adverse effects and is no longer commercially available as a prepared drug, benzodiazepines have widely supplanted it as the agents of choice for pediatric sedation. They have a high therapeutic index, meaning there is a large margin of safety between the effective dose and toxic dose. Benzodiazepines work by potentiating the action of the inhibitory neurotransmitter, gamma-aminobutyric acid (GABA).12,13 They produce anxiolytic, hypnotic, muscle relaxant and amnesic effects, but, unfortunately, occasionally cause increased activity and agitation in children who are negatively stimulated. At doses used for moderate and deeper sedation, it is possible for this class of drug to depress respiration, promote airway obstruction, and decrease blood pressure, especially when used in combination with other sedatives or opioids.12 An advantage to using benzodiazepines is the existence of a reversal agent. Flumazenil antagonizes benzodiazepine action at the GABA receptor, and can be given in the event of an unresponsive patient. It is best administered via the IV route.
Opioids are effective analgesics, making them a useful adjunct when a dental procedure is expected to be particularly painful or stimulating. They act as agonists to the mu, kappa and delta receptors in the nervous system, and are similar to substances the body naturally produces.12,14 Opioids also possess somewhat unpredictable sedative actions, and combination with other agents can produce profound sedation. Opioids depress brain respiratory centers and usually lead to a net decrease in ventilation. This respiratory depression may be synergistic when benzodiazepines and opioids are used together. Opioids are considered to be heart safe secondary to their ability to decrease sympathetic responses; this is beneficial in patients whose cardiovascular systems cannot tolerate the stimulation produced by uncomfortable dental procedures.12 While opioids tend to reduce heart rate, overall, they are thought to produce hemodynamic stability.14 Opioids can cause nausea and vomiting and should be avoided in patients who are prone to these conditions.15 Like benzodiazepines, there is a reversal agent for opioids. Naloxone antagonizes opioid receptors, effectively undoing opioid actions, and may be given by the IV, IM or subcutaneous route.
Antihistamines work by antagonizing histamine and acetylcholine receptors, abolishing the excitatory impact these neurotransmitters usually have within the CNS. They are sleep inducing and have antinausea actions, rendering their use helpful in combination with other medications. They are less effective than benzodiazepines when used alone, but they can potentiate the sedative effect of other agents when used in combination. Antihistamines have minimal depressant influence on the respiratory and cardiovascular systems, but can cause anticholinergic side effects.12 These side effects — which can prove quite bothersome to some patients — include xerostomia, dizziness, urinary retention, blurred vision, increased heart rate and constipation.
Nitrous oxide is widely used in dental offices to promote relaxation and analgesia. It is a colorless, nonirritating and mildly sweet-smelling gas. Its onset and conclusion of action are rapid, as nitrous oxide has low blood and tissue solubility and is not metabolized.9,16 It has minimal effect on physiological parameters. When nitrous oxide is combined with other sedatives or opioids, however, respiratory and/or cardiovascular depression can be synergistically produced.9 Nitrous oxide quickly enters gas-filled spaces, and can cause dangerous increases in volume and pressure when such areas are closed or noncompliant. It is therefore contraindicated in patients with obstructions in spaces like the middle ear or sinuses.9,16 It can also promote nausea and vomiting. Chronic exposure to nitrous oxide has been linked to reproductive issues, neurological deficits and blood cell abnormalities. Such risk is minimized by the use of scavenging systems. Short-term use of nitrous oxide in healthy patients appears to be safe.9 Used alone, the gas typically produces minimal to moderate levels of sedation.
CONCLUSION
Sedative regimens are chosen based on a number of factors, such as the patient’s age, medical history and temperament. Surgical factors include the planned length of the procedure and amount of intraoperative and postoperative discomfort anticipated. The pharmacological profile of the various sedative agents is then matched to the patient and treatment plan. As no single medication is ideal, combinations of drugs are often used to achieve the desired effects. When combinations are used, the sedative and respiratory depressant actions of each are intensified. Using combinations does, however, allow for lower doses of each individual medication, which can decrease the risk of side effects. In pediatric oral sedation, midazolam (a benzodiazepine), hydroxyzine (an antihistamine), and meperidine (an opioid) are commonly used together. If the goal is longer duration of action, diazepam may be used to replace the midazolam. If a patient is easily nauseated, the opioid may be avoided. In addition to these drugs, the level of sedation can be titrated and operative time may be extended by administering a nitrous oxide/oxygen mix.12
Dental patients present with different capacities for coping and compliance, and varying levels of anxiety and medical complexity. In some patients, minimal sedation is adequate, while others may need moderate to deep sedation in order for dental care to be delivered in a secure and compassionate manner.2 A patient’s well-being is paramount, and every member of the sedation team must be well trained and vigilant to ensure patient safety.
References
- American Academy of Pediatric Dentistry Ad Hoc Committee on Sedation and Anesthesia. Policy on the use of deep sedation and general anesthesia in the pediatric dental office. Pediatr Dent. 2012;37:86–87.
- American Academy of Pediatric Dentistry Clinical Affairs Committee, Sedation and General Anesthesia Subcommittee. Guideline on use of anesthesia personnel in the administration of office-based deep sedation/general anesthesia to the pediatric dental patient. Pediatr Dent. 2012:37:228–231.
- American Dental Association. Policy Statement: The Use of Sedation and General Anesthesia by Dentists. Available at: http://www.ada.org/~/media/ADA/ About%20the%20ADA/Files/anesthesia_ policy_statement.pdf?la=en. Accessed April 5, 2016.
- American Dental Association. Guidelines for the Use of Sedation and General Anesthesia by Dentists. Available at: http://www.ada.org/~/media/ADA/ Advocacy/Files/%20anesthesia_use_guide lines.ashx. Accessed April 5, 2016.
- American Academy of Pediatrics and the American Academy of Pediatric Dentistry. Guidelines for Monitoring and Management of Pediatric Patients During and After Sedation for Diagnostic and Therapeutic Procedures. Available at: aapd.org/media/policies_guidelines/g_sed ation.pdf. Accessed April 5, 2016.
- The American Society of Dentist Anesthesiologists. Parameters of Care. Available at: asdahq.org/Parameters ofCare. Accessed April 5, 2016.
- Becker DE. Pharmacokinetic considerations for moderate and deep sedation. Anesth Prog. 2011;58:166–173.
- Donaldson M, Gizzarelli G, Changpong B. Oral Sedation: A primer on anxiolysis for the adult patient. Anesth Prog. 2007;54:118–129.
- Becker DE, Rosenberg M. Nitrous oxide and the inhalation anesthetics. Anesth Prog. 2008;55:124–131.
- Kramer K, Treasure T, Kates C, Klene C, Bennett J. History and physical evaluation. In: Bosack RC, Lieblich S, eds. Anesthesia Complications in the Dental Office. Ames, Iowa: Wiley Blackwell; 2015:9–13.
- Becker DE, Rosenberg M, Phero J. Essentials of airway management, oxygenation, and ventilation: part 1: basic equipment and devices. Anesth Prog. 2014;61:78–83.
- Becker DE. Pharmacodynamic considerations for moderate and deep sedation. Anesth Prog. 2012;59:28–42.
- Struyk BP, Tyler DC, Motoyama EK. Safety and outcome in pediatric anesthesia. In: Davis PJ, Cladis FP, Motoyama EK, eds. Smith’s Anesthesia for Infants and Children. 8th ed. Philadelphia: Elsevier Mosby; 2011:1273–1293.
- Robert RC. Parenteral anesthetic agents. In: Bosack RC, Lieblich S, eds. Anesthesia Complications in the Dental Office. Ames, Iowa: Wiley Blackwell; 2015:135–141.
- Becker DE. Adverse drug interactions. Anesth Prog. 2011;58:31–41.
- Kates C, Anderson D, Shamo R, Bosack R. Inhalation anesthetic agents. In: Bosack RC, Lieblich S, eds. Anesthesia Complications in the Dental Office. Ames, Iowa: Wiley Blackwell; 2015:143–149.




