
Treating Patients With Extreme Body Modifications
These insights will help clinicians provide effective care and recommendations designed to support oral health in this patient population.
This course was published in the April 2018 issue and expires April 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
OBJECTIVES
- Discuss the prevalence of body modifications in the United States, in addition to their historical and cultural significance.
- Identify the types of extreme body modifications and their risks.
- Explain the role of oral health professionals in treating this patient population.
Humans have used body modifications, such as tattoos, piercings and branding/scarification, for thousands of years. While acceptance of these practices varied in different cultures, their social acceptance has been growing globally and in the United States.1 In 2016, approximately one in three Americans had a tattoo — a 20% increase from 2012.2 Nearly four in 10 millennials had at least one tattoo, and one in four had a piercing in a place other than earlobes, according to a 2010 Pew Research Center report.3 The majority of Americans feel comfortable with seeing individuals with tattoos in various professional roles.2 A number of more extreme trends, such as skin scarification, sclera tattooing and tongue bifurcation, have emerged. While few studies have been conducted on the effects of these modifications, media reports, case studies and personal accounts offer evidence of complications. Oral health professionals should be familiar with these body modifications and understand their possible local and general complications. They should also understand the implications for patient assessment and treatment, and strategies to minimize risks.
Body modifications are associated with cultural expression in religious, social, punitive, sexual, esthetic and medical contexts.1,4,5 One of the oldest human specimens with tattoos was dated at more than 5200 years old. The markings were found on the lower spine, wrists, knee and ankle joints, and it is speculated that they were made for therapeutic purposes.5–7 Egyptians used tattoos to signify social or religious status, and tattoos on the abdomen and thighs were used to ward off evil during birthing.7 Slaves and prisoners were known to be permanently marked in early Greek and Roman societies, and South Pacific cultures have long used ornamental tattoos.6
Body piercings of the lips, ears and tongue trace back 4000 to 5000 years and were popular esthetic and tribal adornments in ancient Africa. Nobility in ancient Egypt pierced their navels, while Roman soldiers pierced their nipples to demonstrate virility.8
Scarification, the purposeful manipulation of healing to create markings on the skin, has ancient roots in some cultures. It is believed to have originated in the Australian Aborigines as early as 60,000 BC.5 While currently prevalent in some communities as a method of cultural self-expression and identification, as well as for medicinal purposes by placing herbs into the cuts for the prevention of snake bites and various diseases,5 there are no studies on the rates of this practice in the U.S.1 This more extreme body art practice emerged in San Francisco in the 1980s and increased in popularity in the 1990s.5,9
LAWS AND REGULATIONS
The Association of Professional Piercers states its support for “the right for all adults to adorn or modify their bodies in a safe, informed, and consensual manner when performed by a qualified practitioner under appropriate asepsis.”10 The association and the Alliance of Professional Tattooists11 offer detailed information on safe practices, dangers, and complications and their prevention, as well as links to the state legislatures that regulate various body art forms. In the absence of federal regulations, all states except Nevada have adopted laws addressing body art to ensure safety, protection of minors, and to prevent conflict with the scope of practice of medical and dental professionals.12 However, most regulations address body art limited to tattooing and piercings, with several states including branding/scarification, sub-/transdermal implants, and tongue bifurcation.12 Scarification is not addressed in 19 states, while other states’ legislation ranges from prohibition of the practice to some degree of regulation.1 Currently, Oklahoma is the only state that bans sclera tattooing, although the Indiana legislature is considering it.13
TYPES OF MODIFICATIONS
Sclera Tattooing: Eyeball tattooing, specifically corneal tattooing, is an ancient practice that has specific medical indications for patients with congenital eye defects, such as aniridia (absence of the iris), cataracts, and scars due to traumatic injury to the eye.14 This complex surgical procedure can be safely performed by trained ophthalmologists and can result in improved appearance, although ocular function is not restored. By comparison, cosmetic sclera tattooing is performed by self-taught tattoo artists without anesthesia in a nonmedical environment.15 Luna Cobra, the inventor of cosmetic sclera tattooing, claims to have refined the technique, but admits there are risks.16 The American Academy of Ophthalmology emphasizes that cosmetic sclera tattooing has not been studied and strongly advises against the practice, warning of serious risks, including infection from injection or ink, decreased vision, complete blindness, and potential loss of the eye.17 A video case report of a 24-year-old patient demonstrates that despite surgical intervention and removal of some of the black tattoo ink, followed by antibiotic treatment, the patient’s eye was subsequently removed due to intractable pain.18
Published cases describe individuals seeking professional medical care several days19,20 to several weeks15 after sclera tattooing. Their chief complaints ranged from conjunctival lumps/nodules without reported pain,15,19 to pain, photophobia, decreased vision and eyelid edema.19 Different mixtures of tattoo dyes19 resulted in various coloration of patients’ scleras. In these cases, following appropriate treatment — including corticosteroids and antibiotics — the patients’ conditions improved;19 however, long-term complications, such as secondary glaucoma20 and conjunctival granulomas that can lead to scleral thinning or malignancy, are possible.15,19 Risks during the procedure performed by untrained personnel and without the use of a surgical microscope can result in globe penetration,15,20 traumatic cataract, retinal detachment and endophtalmatis.15 Because the tattoo ink acts as a foreign body, it can cause ocular inflammatory and allergic reactions to the metallic elements, such as nickel, cobalt, copper, chromium and iron.19 Until recently, sclera tattooing has been relatively unknown outside of a small group of practitioners and their clients — as well as the medical professionals who treat the resulting complications.15,17–20
Scarification: This is the practice of creating permanent scars by cutting, burning or branding images, words or patterns in the skin.1,5 It can be performed by cutting with scalpel or knife, hot or cold branding (using liquid nitrogen), thermo- and electrocautery, and moxibustion (placing incense on the skin and allowing it to burn until it is extinguished in the underlying layers).1,5 Strips of skin can be removed to produce larger patterns, and wounds can be irritated by chemicals (e.g., iodine or citrus juice) and scraping off scabs to enhance scar formation.1,21 Regardless of the method, results can be inconsistent due to unpredictable healing and possible complications, such as infections and keloid formation.1 Performed without anesthesia and with intentionally prolonged healing time, undergoing this procedure requires remarkable pain tolerance.
Scarification and other more dramatic and intense body modifications can be a sign of a nonsuicidal self-injury syndrome (NSSI), a disorder associated with mental health conditions, such as psychotic, personality and anxiety disorders. The prevalence of NSSI in adolescents is estimated at 14% to 24%.1 Careful, nonjudgmental interviewing by a health care professional observing these body modifications can help determine the intent. Clinicians need to distinguish between normal body modifications and self-injurious behaviors that can be a symptom of underlying mental health disorders, and help identify individuals at risk for greater self-harm, including suicide;1,4,21 because many body modifications, including scarification, involve the head, neck or face, oral health professionals may play an important role in this regard.
Tongue Bifurcation: Also known as tongue splitting, forking or bifid tongue, this modification involves separating the tongue anteriorly into two parts to resemble a snake’s tongue. This procedure can be done by cutting with a scalpel or laser along the midline and cauterizing or suturing the edges to prevent reattachment.21,22 Tongue bifurcation has also been reported as an unwanted complication of an infected tongue piercing that successfully healed after a surgical intervention.23 Tongue splitting is an extremely painful procedure, which is typically done by medically untrained artists with inadequate or no anesthesia.21,22,24 It can result in infection, inflammation, blood loss due to high vascularization of the tongue, and nerve damage that can persist even in a well-healed bifid tongue.22,24 With training, individuals can learn to control the two parts of their tongue independently and the effects on speech may be unnoticeable.21,22 The American Dental Association (ADA) advises against tongue bifurcation as an invasive and dangerous procedure performed for nonmedical reasons.25
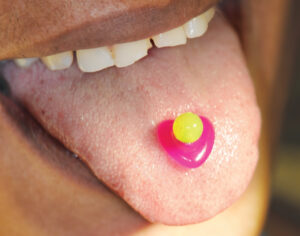
Tongue piercings can precede or accompany tongue bifurcation, and can have serious complications and implications for oral health care (Figure 1). More frequent in women, tongue piercing is the most prevalent oral/perioral piercing (5.6%).8 It has been associated with rare, but serious, complications — including cerebellar abscess,26 infective endocarditis,27 local infections, and increased incidence of tooth injuries, such as enamel fissures, fractures and gingival recession, especially in the mandibular lingual incisor area.28 Unfortunately, surveys of piercers29 and clients with oral piercings30,31 demonstrate low awareness of the associated local and systemic risks, including possibility of transmission of blood-borne diseases, bacterial infections, temporary and permanent paralysis due to possible nerve damage, and local complications. Piercers also demonstrated poor knowledge of oral cavity and tongue anatomy,29 and postprocedural care recommendations were limited to using mouthrinse, while follow-up visits with piercing specialists or medical professionals were recommended only rarely.30,31
Clinical cONSIDERATIONS
Assessment and documentation of the status of orofacial modifications should be performed as part of the comprehensive intra- and extraoral examination and include the location, description and condition of sites and surrounding hard and soft tissues. Photographic documentation is advisable for future comparison. Familiarity of the oral health professional with typical postprocedural healing time and potential adverse reactions ensure safety and create an environment of respect and candor in the dental setting.4
The routine removal of all metal objects and jewelry in the field of view of a diagnostic image is essential. In panoramic imaging, a metal object obscures anatomy and potential pathology in its own location, and creates an enlarged ghost image on the contralateral side. The complexity of cone beam computed tomography causes artifacts when imaging dense metals that obscure anatomical structures adjacent to the metal object, and create multiple light/dark bands across the image layers. Many software programs can reduce these effects from dental materials in the dentoalveolar area, but may be less able to eliminate these effects in perioral and facial piercings.32,33
In magnetic resonance imaging (MRI), minor burns have been associated with tattoos,7 although a recent study with a new MRI machine showed safety and effectiveness, with no side effects associated with tattooed regions.34 Artifacts on MRIs, however, have been discovered from even small tattoos, such as permanent eye liner.7
During dental procedures, facial, perioral and mucosal piercings need not be removed unless they directly interfere with the treatment site, affect asepsis, or limit the use of isolation or suction devices. Removed hardware may be cleaned and disinfected as needed, and vulnerable openings maintained with nonmetallic instruments.4,35,36
Oral health professionals should assess patient awareness of hard and soft tissue risks and proper care of tongue and lip piercings — with the tongue being the most common, and problematic site.28,30 Healing time for tongue piercing and bifurcation procedures is estimated at four to six weeks and the lips at six to eight weeks.4 Common acute complications of tongue piercing include hypersensitive reactions to metal, swelling, pain and, less commonly, increased salivary flow, severe infection, airway obstruction, severe bleeding, embedding of the object, and nerve damage. Trauma to teeth may include chips, fractures, pulpal damage and gingival recession. Localized hyperplastic growth is not uncommon.25,30
Although the ADA and American Academy of Pediatric Dentistry strongly discourage intraoral piercings, both recognize the oral health professional’s role in assessment, care and education.25,37 Patients should be informed about the need to maintain excellent oral hygiene after piercing procedures, and be able to recognize abnormal swelling, prolonged bleeding, pain and exudate.25
CONCLUSION
Discussions regarding the care and complications associated with body modifications that may affect health or treatment are essential to effective patient education. Knowledgeable oral health professionals who can offer recommendations about modifications are able to build trust. For young patients, anticipatory guidance may prevent future issues and even influence decisions — which have been shown to be often made in haste and without adult input. Discussions may focus on the individual’s motivation and permanency of the procedure, associated risks, difficulty of removal, need for asepsis, and choice of a qualified professional to perform the procedure.38 Especially dangerous procedures, such as sclera tattooing and tongue bifurcation, should be discouraged. For adolescents and young adults, in particular, information on the care and complications associated with various body modifications delivered objectively from a knowledgeable provider may be received with openness.
All forms of body modification are growing in prevalence and social acceptability, which increases the likelihood that dental professionals will encounter patients exhibiting these phenomena and their associated risks and complications. Being knowledgeable about extreme body modifications and skilled in communicating with these patients will allow clinicians to help this population maintain optimal oral health.
References
- Breuner CC, Levine DA; Committee On Adolescence. Adolescent and young adult tattooing, piercing, and scarification. Pediatrics. 2017;140:e20163494.
- The Harris Poll. Tattoo Takeover: Three in Ten Americans Have Tattoos, and Most Don’t Stop at Just One. Available at: theharrispoll.com/health-and-life/Tattoo_Takeover.html. Accessed March 6, 2018.
- Pew Research Center. Millennials: A Portrait of Generation Next Confident. Connected. Open to Change. Available at: pewsocialtrends.org/2010/02/24/millennials-confident-connected-open-to-change/. Accessed March 6, 2018.
- Dunn D. Body art and the perioperative process. AORN J. 2016;104:326–340.
- Perper M, Aldahan AS, Tsatalis JP, Nouri K. Modifications of body surface: piercings, tattoos, and scarification. Int J Dermatol. 2017;56:351–353.
- Lineberry C. Tattoos: the ancient and mysterious history. Available at: smithsonianmag.com/history/tattoos-144038580/. Accessed March 6, 2018.
- Durkin SE. Tattoos, body piercing, and healthcare concerns. J Radiol Nurs. 2012;31:20–25.
- Hennequin-Hoenderdos N, Slot D, Van der Weijden G. The prevalence of oral and peri-oral piercings in young adults: a systematic review. Int J Dent Hyg. 2012;10:223–228.
- Guynup, S. Scarification: ancient body art leaving new marks. Available at: news.nationalgeographic.com/news/2004/07/0728_040728_tvtabooscars.html. Accessed March 6, 2018.
- Association of Professional Piercers. Safe Piercing. Available at: safepiercing.org/safe_piercing.php#mods. Accessed March 6, 2018.
- Alliance of Professional Tattooists. About Us. Available at: safe-tattoos.com/about.html. Accessed March 6, 2018.
- National Conference of State Legislatures. Tattooing and Body Piercing. State Laws, Statutes and Regulations. Available at: ncsl.org/ research/health/tattooing-and-body-piercing.aspx. Accessed March 6, 2018.
- Rudavsky S. Eyeball tattoos? Here’s why Indiana lawmaker wants to ban them. Indianapolis Star. January 8, 2018.
- Pitz S, Jahn R, Frisch L, Duis A, Pfeiffer N. Corneal tattooing: an alternative treatment for disfiguring corneal scars. Br J Ophthalmol. 2002;86:397–399.
- Brodie J, El Galhud H, Bates A. A case of episcleral tattooing — an emerging body modification trend. BMC Ophthalmol. 2015;8:15.
- Cobra L. Eyeball tattooing. Available at: http://lunacobra.net/services/eyeball-tattooing. Accessed March 6, 2018.
- Gudgel D. Eyeball tattoos are even worse than they sound. Available at: aao.org/eye-health/news/eyeball-tattoos-are-even-worse-than-they-sound. Accessed March 6, 2018.
- Freund PR, Greve M. Scleral tattoo gone wrong. Available at: aao.org/clinical-video/scleral-tattoo-gone-wrong. Accessed March 6, 2018.
- Duarte G, Cheja R, Pachón D, Ramírez C, Arellanes L. Case series: Two cases of eyeball tattoos with short-term complications. Am J Ophthalmology Case Reports. 2017;5:26–28.20.
- Cruz NF, Santos KS, Farah ML, Felberg S. Conjunctival tattoo with inadvertent globe penetration and associated complications. Cornea. 2017;36:625–627.
- Benecke M. First report of nonpsychotic self-cannibalism (autophagy), tongue splitting, and scar patterns (scarification) as an extreme form of cultural body modification in a Western civilization. Am J Forensic Med Pathol. 1999;20:281.
- Bressmann T. Speech adaptation to a self-inflicted cosmetic tongue split: perceptual and ultrasonographic analysis. Clin Linguist Phon. 2006;20:205–210.
- Fleming PS, Flood TR. Bifid tongue — a complication of tongue piercing. Br Dent J. 2005;198:265.
- Aga F, Harris R. Cosmetic tongue split. Br Dent J. 2013;214:275.
- American Dental Association. Intraoral/Perioral Piercing and Tongue Splitting. Available at: ada.org/en/member-center/oral-health-topics/oral-piercing. Accessed March 6, 2018.
- Martinello RA, Cooney EL. Cerebellar brain abscess associated with tongue piercing. Clin Infect Dis. 2003;36:e32–e34.
- Tronel H, Chaudemanche H, Pechier N, Doutrelant L, Hoen B. Endocarditis due to Neisseria mucosa after tongue piercing. Clin Microbiol Infect Off Publ Eur Soc Clin Microbiol Infect Dis. 2001;7:275–276.
- Hennequin-Hoenderdos N, Slot D, Van der Weijden G. The incidence of complications associated with lip and/or tongue piercings: a systematic review. Int J Dent Hyg. 2016;14:62–73.
- Vozza I, Fusco F, Bove E, Ripari F, Corridore D, Ottolenghi L. Awareness of risks related to oral piercing in Italian piercers. Pilot study in Lazio Region. Ann Stomatol (Roma). 2015;5:128–130.
- De Moor RJG, De Witte AMJC, Delmé KIM, De Bruyne MA, Hommez GMG, Goyvaerts D. Dental and oral complications of lip and tongue piercings. Br Dent J. 2005;199:506–509.
- Vozza I, Fusco F, Corridore D, Ottolenghi L. Awareness of complications and maintenance mode of oral piercing in a group of adolescents and young Italian adults with intraoral piercing. Med Oral Patol Oral Cirugia Bucal. 2015;20:e413–e418.
- Liang H, Flint D, Benson B. Why should we insist patients remove all jewellery? Dentomaxillofacial Radiol. 2011;40:328–330.
- Schulze R, Heil U, Gross D, Bruellmann DD, et al. Artefacts in CBCT: a review. Dentomaxillofacial Radiol. 2011;40:265–273.
- Noureddine Y, Bitz AK, Ladd ME, et al. Experience with magnetic resonance imaging of human subjects with passive implants and tattoos at 7 T: a retrospective study. Magma N Y N. 2015;28:577–590.
- Smith FD. Caring for surgical patients with piercings. AORN J. 2016;103:583–596.
- Maspero C, Farronato G, Giannini L, Kairyte L, Pisani L, Galbiati G. The complication of oral piercing and the role of dentist in their prevention: a literature review. Stomatologija. 2014;16:118–124.
- Policy on intraoral/perioral piercing and oral jewelry/accessories. Pediatr Dent. 2017;39:83–84.
- Montgomery DF, Parks D. Tattoos: Counseling the adolescent. J Pediatr Health Care. 2001;15:14–19.
Featured image by HTTPS://COMMONS.WIKIMEDIA.ORG/WIKI/FILE%3ATONGUE-SPLIT.JPG BY IOERROR (HTTPS://WWW.FLICKR.COM/PHOTOS/IOERROR/30201729/) [CC BY-SA 2.0 (HTTPS://CREATIVECOMMONS.ORG/LICENSES/BY-SA/2.0)], VIA WIKIMEDIA COMMONS FROM WIKIMEDIA COMMONS
From Decisions in Dentistry. April 2018;4(4):53-56.




