HALFPOINT / ISTOCK / GETTY IMAGES PLUS
HALFPOINT / ISTOCK / GETTY IMAGES PLUS
Implementing Periodontal Surgical Checklists
The use of checklists for periodontal and other oral surgeries can help improve outcomes in clinical practice and academic settings.
Patient safety is a fundamental requirement for effective care in dental and medical settings.1 In 2008, the World Health Organization published the WHO Surgical Safety Checklist and Implementation Manual.2 Based on these guidelines, Haynes et al3 designed a surgical checklist. After its introduction, they reported the rate of complications at all sites dropped from 11.0% at baseline to 7.0%, and the total in-hospital rate of death dropped from 1.5% to 0.8%. Following this, surgical checklists have been implemented in more than 4000 hospitals worldwide.4 A systematic review by Treadwell et al5 notes that surgical checklists reduced complications and improved communication between operating staff. In another systematic review, Boyd et al6 reviewed randomized controlled trials involving checklists. The investigation pointed to their effectiveness in improving safety outcomes in hospitalized patients. The team reported significant reductions in postoperative complications and medication-related problems, as well as improved compliance with evidence-based prescribing and infection control protocols.6 In light of these results, this article proposes working examples for checklists that can be used for periodontal and other oral surgery procedures.
In dentistry, checklists have been developed for use in endodontic treatment, dental implant placement, early identification of malignancy presenting as temporomandibular disorder (TMD), and to prevent the extraction of wrong teeth. Christman et al7 designed a checklist to aid in reducing errors in the placement of dental implants especially for inexperienced practitioners, dental students, surgical residents and dental implant trainees. Similarly, Bidra8 described a perioperative surgical safety checklist that could be used by clinicians of varying experience for straightforward and/or complex implant and related surgeries in an outpatient setting, without sedation. Beddis et al9 developed a checklist for patients presenting to the TMD clinic with trismus. The team reported that use of the checklist improved early recognition of atypical features presenting with trismus, and contributed to the early diagnosis of a case of malignancy.
CHECKLISTS ENHANCE SAFETY
The mechanisms by which checklists enhance patient safety in the operating room include increasing communication among providers, improving delegation of various responsibilities to support staff, and mandating preprocedural pauses. A study by Schmitt et al10 found that implementation of a surgical safety checklist in the ambulatory clinic of an oral and maxillofacial surgery department led to a much smoother procedural flow. The incidents of instruments or materials missing or malfunctioning during surgery, and the frequency of incomplete postsurgical documentation and missing surgical consent forms, were considerably lower in the checklist group compared to the no-checklist group.
Although use of surgical checklists is widespread in medicine, the dental profession has been a slow adopter. While this may be due in part to the low morbidity and mortality data in dentistry, attitudes toward checklists may also play a role. However, it would appear that using checklists in dentistry — especially in the surgical specialties — is a wise idea. In an investigation of attitudes toward surgical safety checklists for ambulatory oral and maxillofacial surgery, Viswanath et al11 found 93% of respondents not currently using one would consider implementing checklists if available.
SAMPLE CHECKLISTS
Given this background in medical and dental settings, this article proposes sample periodontal surgical checklists that can be used by a dental student, periodontal resident, early entry clinician, and/or experienced clinicians to help remember important details that may be missed during the course of surgical treatment. The intent is to enhance safe and efficient treatment, and support better documentation of oral surgery procedures.
Presented in checklist form, these examples cover the following aspects of surgical care:
- Common checklists for all surgical procedures: patient checklist (Table 1)
- A brief instrument checklist (Table 2)
- Checklist during surgery (Table 3)
- Checklist following surgery (Table 4)
- Specific checklists for periodontal surgical procedures:
a. Guided tissue regeneration (Table 5)
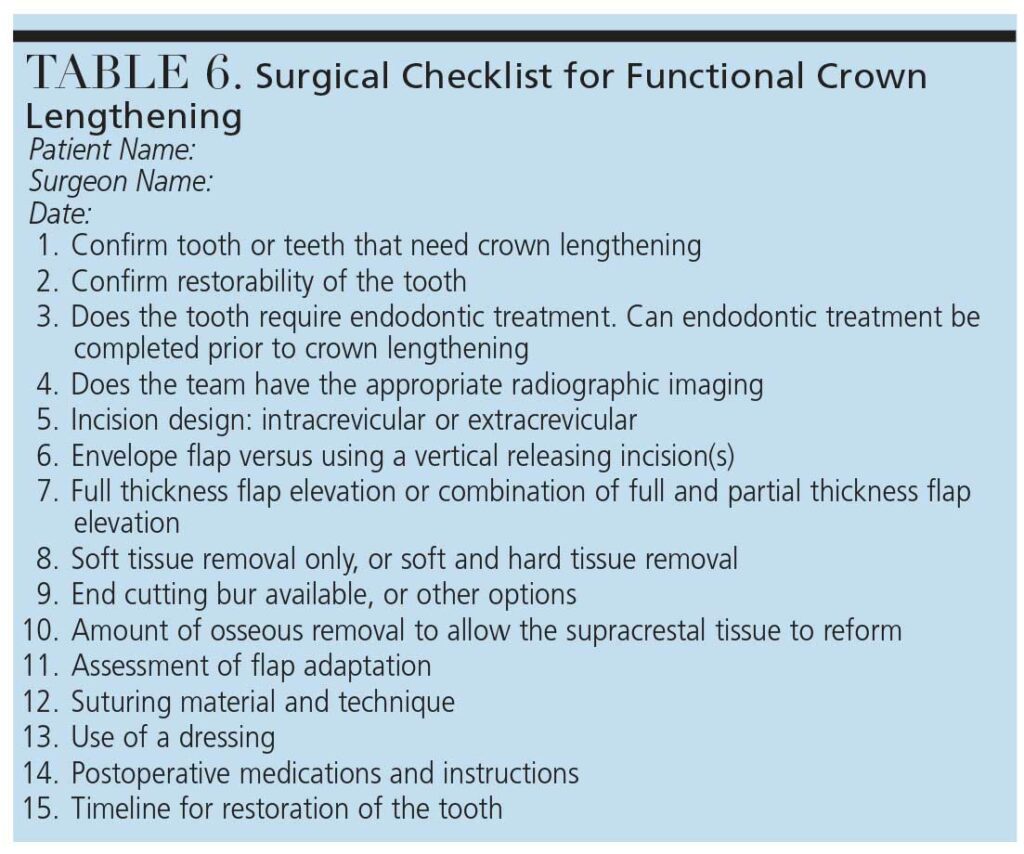
b. Functional crown lengthening (Table 6)
c. Mucogingival surgery (Table 7): Free gingival grafts (Table 8); Connective tissue grafts (Table 9); and Acellular dermal grafts (Table 10)
CONCLUSION
Among dental and medical providers, surgical checklists are becoming essential documentation and guiding tools in the provision of safe care. This paper has proposed various checklists for periodontal and other oral surgery procedures that can be used in private practice and academic settings. Oral health professionals are encouraged to implement surgical checklists — along with modifications to fit individual clinician preference — to improve the quality and safety of care.
KEY TAKEAWAYS
- Due to their efficacy, surgical checklists have been implemented in more than 4000 hospitals worldwide.4
- Investigations into the use of checklists have found significant reductions in postoperative complications and medication-related problems, as well as improved compliance with evidence-based prescribing and infection control protocols.6
- Checklists increase patient safety in dental operatories by increasing communication among providers, improving delegation of various responsibilities to support staff, and mandating preprocedural pauses.
- During a study of attitudes toward surgical safety checklists for ambulatory oral and maxillofacial surgery, Viswanath et al11 found 93% of respondents not currently using one would consider implementing checklists if available.
- In light of these results, this article proposes working examples for checklists that can be used for periodontal and other oral surgery procedures.
REFERENCES
- Campbell S, Tickle M. What is quality primary dental care? Br Dent J. 2013;215:135–139.
- World Health Organization. WHO surgical safety checklist and implementation manual. Available at: https://www.who.int/patientsafety/safesurgery/ss_checklist/en/. Accessed December 16, 2020.
- Haynes AB, Weiser TG, Berry WR, et al. A surgical safety checklist to reduce morbidity and mortality in a global population. N Engl J Med. 2009;360:491–499.
- Pugel AE, Simianu VV, Flum DR, Dellinger PE. Use of the surgical safety checklist to improve communication and reduce complications. J Infect Public Health. 2015;8:219–225.
- Treadwell JR, Lucas S, Tsou AY. Surgical checklists: a systematic review of impacts and implementation. BMJ Qual Saf. 2014;23:299–318.
- Boyd J, Wu G, Stelfox H. The impact of checklists on inpatient safety outcomes: a systematic review of randomized controlled trials. J Hosp Med. 2017;12:675–682.
- Christman A, Schrader S, John V, Zunt S, Maupome G, Prakasam S. Designing a safety checklist for dental implant placement: a Delphi study. J Am Dent Assoc. 2014;145:131–140.
- Bidra AS. Surgical safety checklist for dental implant and related surgeries. J Prosthet Dent. 2017;118:442–444.
- Beddis HP, Davies SJ, Budenberg A, Horner K, Pemberton MN. Temporomandibular disorders, trismus and malignancy: development of a checklist to improve patient safety. Br Dent J. 2014;217:351–355.
- Schmitt CM, Buchbender M, Musazada S, Bergauer B, Neukam FW. Evaluation of staff satisfaction after implementation of a surgical safety checklist in the ambulatory of an Oral and Maxillofacial Surgery Department and its impact on patient safety. J Oral Maxillofac Surg. 2018;76:1616–1639.
- Viswanath A, Balint A, Johnson III R, Rosenberg MB, Oreadi D. Surgical safety checklists are underutilized in ambulatory oral and maxillofacial surgery. J Oral Maxillofac Surg. 2018;76:267–272.
The authors have no commercial conflicts of interest to disclose.
From Decisions in Dentistry. January 2021;7(1):14–17.