Head and Neck Evaluation of the Dental Patient
A comprehensive visual and tactile examination may help reveal early signs of oral or tonsillar cancer, thus aiding timely diagnosis and treatment.
This course was published in the March 2018 issue and expires March 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
OBJECTIVES
- Describe the role of the conventional visual and tactile examination in screening for oral and tonsillar cancers.
- Discuss the percentage of patients who may present with potentially malignant disorders (PMDs) or oral cancer, the number of new oral cancer cases projected in 2018, and the percent of cases diagnosed at an advanced stage.
- Explain clinical approaches to assessing, diagnosing and treating PMDs and oral cancer.
In the dental setting, the CVTE involves a standard, sequential assessment of extraoral and intraoral tissues. An essential part of this assessment is the clinician’s knowledge of head and neck anatomy, as this helps providers discriminate potentially abnormal or disease-related findings from normal landmarks or common anatomic variants. In addition to anatomy, knowledge of local and systemic pathology, and the broad categories of pathogenesis (e.g., developmental, infectious, neoplastic, inflammatory/immunologic and metabolic), are needed to develop a list of probable diagnostic considerations (the differential diagnosis), as well as the most likely diagnosis (i.e., the clinical or working diagnosis). A review of the patient’s history may provide additional information, such as symptoms, lesion recurrence, or a genetic or familial pattern of expression. For some lesions or tissue abnormalities, a confident clinical diagnosis can be assigned by CVTE and history alone, while in other cases, selective imaging may provide additional diagnostically useful information. In practice, however, a definitive final diagnosis often requires tissue biopsy, followed by histopathologic evaluation by a specialist, such as an oral and maxillofacial pathologist.
For oral health professionals, the CVTE is usually performed with nothing more than normal operatory lighting, examination gloves, a dental mirror, and cotton gauze for grasping and manipulating the tongue. A measuring device, such as a periodontal probe, may be helpful for recording the dimensions of any lesion or abnormality. It is important that each patient be examined in a standard, sequential manner that does not vary from day to day, or on the basis of patient age or potential risk factors. Similar to the approach used with infection control, assume that every patient could have a lesion — until proven otherwise through the consistent use of a standard, step-wise technique.
Extraoral patient evaluation involves inspection for superficial masses, color changes of the skin or vermilion, and evidence of ulceration, inflammation or infection. Palpation of the face and neck permits detection of deeper-seated masses, such as swollen lymph nodes or neoplasms of the parotid or submandibular salivary glands. Considering that up to 10% of dental patients may present with an oral mucosal or submucosal abnormality, early detection and the discrimination of suspicious from non-suspicious lesions is imperative.1,2 Oral PMDs or oral cancer often present in older adult male patients with a history of smoking and excessive use of alcohol, yet young adult patients without risk factors may also develop these lesions, affirming the need for a standard, consistent approach to CVTE with all adult patients.3,4
In general, the standard dental CVTE meets the definition of a screening test, as it is performed routinely on all patients, regardless of symptoms, to detect the presence of disease or tissue abnormality.5 In addition to detecting oral PMDs, CVTE can be a relatively accurate predictor of their clinical significance, with a reported specificity (85%) and sensitivity (97%) in discriminating suspicious versus non-suspicious oral lesions.6
ORAL CANCER
Although CVTE of the head and neck is used for the detection and diagnosis of any disease or tissue abnormality, dental patients are often most concerned about the possibility of oral cancer. As previously noted, the most common oral cancer is OSCC, a malignancy that arises from the surface epithelial lining of the oral cavity. As oral mucosa is generally readily accessible to direct inspection and palpation, most cases of oral cancer or PMDs can be detected early (assuming patients present for examination at regular intervals). Unfortunately, many patients don’t visit the dentist regularly, and more than 70% of oral cancers are diagnosed at an advanced stage.7
The American Cancer Society estimates there will be 33,950 new cases of oral cancer in the United States in 2018, resulting in 6800 deaths.7 Risk factors include male gender, increasing age, smoking, excessive alcohol use, immunosuppression and poor diet. While much attention has been focused on the association between human papillomavirus (HPV) infection and tonsillar/oropharyngeal cancer, such infection appears to play a minor role in cases of OSCC, including the mobile portion of the tongue (< 5% of cases).8,9 In addition, epidemiologic studies have shown the overall national incidence of OSCC has declined over the past 40 years, similar to trends in smoking.3,10 Unfortunately, the incidence of tongue cancer has increased slightly over this time, particularly among females — a trend that is not attributable to HPV or any other known risk factor.11,12 The overall 5-year survival rate in the U.S. is 64.3%, but survival is highly dependent upon the disease stage. With early (localized) oral cancer, 83.7% of patients are alive at 5 years, while patients with regional and distant metastatic spread have 64.2% and 38.5% 5-year survival, respectively. Differences have also been noted in survival based on race/ethnicity, with lower 5-year survival rates among blacks, as compared to whites, even when stratified according to stage.3,10
In addressing the issue of cancer, it should be noted that oral cancer is a relatively uncommon malignancy in the U.S.; by comparison, major U.S. cancers in 2018 will include an estimated 266,120 cases of breast cancer in women and 164,690 prostate cancers in men.7 Additional insight can be gained by comparing oral cancer with pancreatic cancer. The latter is rarely diagnosed in the early stages and will affect an estimated 55,440 Americans in 2018, with 44,330 deaths.7 These statistics can provide patients with perspective about their overall oral cancer risk, while reinforcing the need for CVTE at regular intervals to detect uncommon oral PMDs or oral cancer at the earliest stage possible.
SUSPICIOUS CLINICAL FEATURES
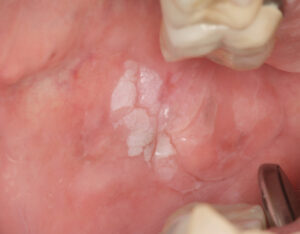
Oral PMDs are surface mucosal lesions that have an increased risk of transforming into OSCC. Most commonly, they present as leukoplakias (keratinized white patches or plaques; Figure 1), although other presentations, including erythroplakias (red patches or plaques) or mixed red/white lesions (erythroleukoplakias), may also be seen. Clinical suspicion for a given PMD may be increased based on its clinical characteristics or anatomic site — or both.3,5,13
Suspicious clinical features include:
- Sharply defined border from the surrounding mucosa
- A diameter larger than 1 cm
- Nonhomogenous surface (e.g., variations in degree of keratinization, papillations and/or clefting)
- Color variations (including erythroplakias and erythroleukoplakias)
Suspicious anatomic sites include:*
- Ventrolateral tongue
- Floor of mouth
- Anterior tonsillar pillar/retromolar area/soft palate
* These three sites combined represent 20% of the total oral mucosal surface area, yet gave rise to 75% of 209 consecutive cases of oral cancers.14
In the case of non-suspicious oral PMDs, follow-up evaluation within two to four weeks is sound clinical practice, with or without conservative therapy, and generally recommended by the American Dental Association (ADA).3 For suspicious oral PMDs or lesions that are persistent or progressive at the follow-up evaluation, tissue biopsy is recommended to establish a definitive diagnosis and guide further care.
CLINICAL FOLLOW-UP AND assessment ADJUNCTS
As noted, clinical follow-up examination is essential to routine dental practice, and its importance to the diagnosis and management of oral lesions — including PMDs — cannot be overstated. At this visit, the clinician is able to assess the impact of initial conservative therapy (if any) or the rate of physical or symptomatic changes associated with the tissue abnormality. As previously noted, even non-suspicious lesions that are merely persistent (without enlargement or progressive clinical alterations) may warrant tissue biopsy to rule out the possibility of epithelial dysplasia (the maturational disorganization of the surface epithelium seen in PMDs) or oral cancer.
Despite the relative accuracy of CVTE in detecting and discriminating between harmless and suspicious mucosal lesions, a number of adjunctive devices are available for use in primary and specialty dental care settings to assist in the detection and assessment of oral lesions — particularly oral PMDs. The ADA recently published clinical practice guidelines for these devices, as well as an updated systematic review and meta-analysis of their diagnostic accuracy and utility as triage tools and supplements to the CVTE.3,4 It is important to recognize that these adjuncts are not intended to replace a routine CVTE; rather, they can be used to supplement the examination process.
Examples of currently available adjuncts include:
- Tissue reflectance (e.g., ViziLite Plus [DenMat Holdings], Microlux DL [AdDent])
- Tissue autofluorescence (e.g., VELscope [LED Dental], Oral ID [Forward Science], Identafi [Star Dental], ViziLite Pro [DenMat Holdings], Bio/Screen [AdDent], Goccles [Pierrel Pharma])
- Salivary testing (e.g., OraRisk [Oral DNA Labs], SaliMark [PeriRx], OraMark [OncAlert Labs])
- Cytologic testing (e.g., OralCDx [OralScan Laboratories], OralCyte [ClearCyte Diagnostics], ClearPrep OC [Resolution Biomedical], CytID [Forward Science])
TISSUE REFLECTANCE
This adjunct was developed as an oral counterpart to colposcopy, an examination technique for potentially malignant and malignant lesions of cervical mucosa. Prior to evaluation of the oral mucosa, the dental patient rinses with a 1% acetic acid solution to remove superficial debris. Depending upon the manufacturer, a chemiluminescent or battery-powered light source is used to examine the oral cavity for distinctly white (acetowhite) lesions.5,13,15 In the ViziLite Plus system, tolonium chloride (toluidine blue) is provided to mark the acetowhite lesions for localization and potential biopsy once the light source is removed.
It should be noted that the extrapolation of tissue reflectance from the cervix to the oral cavity is complicated by major differences between the mucosa at these two anatomic sites. In the cervix, excess keratinization is fairly uncommon and virtually always associated with PMDs or cervical cancer. As a result, acetowhite lesions of the cervix are routinely subject to biopsy to establish a definitive diagnosis. In contrast, excess keratinization in the oral cavity is relatively common, and most often reflects reactive changes secondary to local trauma/irritation, chronic inflammation, or a superficial fungal infection. For this reason, the finding of acetowhite lesions in the oral cavity could lead to unnecessary tissue biopsies or improper patient management without careful clinical correlation. In addition, some oral PMDs (e.g., erythroplakias or erythroleuoplakias) are associated with little to no excess keratin. While these clinical features are suspicious for high-grade dysplasia or cancer, they might yield a false negative result by tissue reflectance.
TISSUE AUTOFLUORESCENCE
Tissue autofluorescence is based upon the observation that living tissues contain molecules (fluorophores) that can be stimulated by specific wavelengths of light to emit a weak light of their own. This fluorescent signal can be selectively viewed by optical filters and local tissue alterations that reduce the levels of these molecules, thus reducing the autofluorescent signal. Tissue autofluorescence has been an adjunct to bronchoscopic examination for decades after it was found that loss of fluorescence was associated with early lung cancer and PMDs of the lung and upper airways. This technology was subsequently modified for use in the oral cavity, and first became commercially available in 2006.5,13,15–17
Tissue autofluorescent examination in the oral cavity can be challenging, however, as loss of fluorescence is not specific or limited to PMDs or oral cancer. Reduced tissue autofluorescence is seen in areas of increased tissue vascularity, melanin pigmentation, and local inflammation or ulceration. As inflammation and pigmentation are quite common in the oral cavity, the potential for false positive results is substantial with this adjunct. In addition, false negative results have also been reported, warranting careful correlation with CVTE and patient follow-up examination.17,18
SALIVARY TESTING
Salivary testing is the most recently available adjunct to the CVTE. These tests analyze patient saliva for elevations in protein markers associated with oral cancer, HPV DNA, or both. While sensitive and easy to use, several potentially confounding issues have been recognized with these adjuncts. For example, a number of these tests use protein biomarkers (such as IL-1β or CD44) that are known to be elevated in patients who smoke, as well as by the presence of inflammation caused by disorders ranging from arthritis to periodontitis.19–23 As with previous adjuncts, the prevalence of these common conditions increases the likelihood of false positive results (i.e., the elevation of biomarker levels by conditions other than oral cancer), leading to unnecessary testing, additional costs and patient anxiety.
Salivary testing for HPV is even more complicated. Most oral HPV infections are transient and present with no visible surface change or lesion. As a result, the detection of HPV in saliva will often have no clinical significance. Furthermore, while clearance of the HPV infection usually occurs within six months, it may take up to two or three years, especially in males.24–27 In these patients, even repeated positive test results may not have serious or even detectable health consequences. In addition, HPV infection can develop in two ways: The viral DNA can grow and divide in the cytoplasm of epithelial cells, or the HPV DNA can become integrated into the host cell DNA, dividing and multiplying as part of the epithelial cell. Integration is a feature of “high-risk” HPV subtypes, such as HPV 16 and HPV 18, that can allow the virus to take control of host cell growth and may lead to the development of cervical cancer in women.
A similar pathogenic mechanism is thought to give rise to HPV-related tonsillar cancer in both men and women. Integration of the HPV DNA results in the overexpression of a cell marker known as p16. The association is so reliable that the finding of excess p16 production is currently used in tissue biopsy specimens to confirm HPV DNA integration in tonsillar cancer. Unfortunately, available HPV salivary tests assess only viral DNA, not p16. This limits the value of a “positive” test because it cannot distinguish between samples with integrated (potentially serious) versus nonintegrated (innocuous) HPV DNA. Finally, salivary tests are less sensitive than serum (blood) tests for detecting HPV DNA, especially in patients with tonsillar cancer. For patients concerned about their HPV status, or who worry about an undetected tonsil cancer, a serum test is preferred.
CYTOLOGIC TESTING
The previously described adjuncts are marketed as aids to the CVTE, essentially to be used as supplemental screening tests for the detection of oral PMDs and oral cancer. In contrast, cytology is only to be used when a mucosal abnormality has been identified. This makes oral cytology a case-finding test, one that is intended to either assess or diagnose a mucosal abnormality.5 Cytology testing permits the cellular (cytomorphologic) or molecular features of an oral lesion to be examined for signs of dysplasia or cancer. It is important to realize that while scalpel biopsy provides a definitive diagnosis for oral PMDs, oral cytologic testing only provides a “test result.” The result can fall into one of four categories; incomplete specimen, negative, atypical, or positive. In the case of an atypical or positive result, the company recommends a surgical biopsy of the lesional tissue to obtain a definitive diagnosis and direct appropriate treatment, if necessary. For this reason, surgical biopsy is generally preferred over cytologic testing for oral lesions — and especially those with suspicious clinical features — in order to obtain a diagnosis as soon as possible and prevent treatment delays.13,28
CLINICAL PRACTICE GUIDELINEs
In the October and November 2017 issues of the Journal of the American Dental Association, the ADA published updated guidelines for dental practitioners in the evaluation of PMDs, as well as a systematic review and meta-analysis of the pertinent scientific literature.3,4 For the clinical practice guidelines, an expert panel produced a good-practice statement and six clinical recommendations. While a brief summary is provided here, readers are directed to these manuscripts for additional details and supplemental information.
- The ADA good-practice statement notes: “Clinicians should obtain an updated medical, social and dental history, and perform an intraoral and extraoral CVTE in all adult patients.”
- Recommendation 1 suggests that clinical lesions detected on CVTE, but considered innocuous or non-suspicious for malignancy, be re-examined periodically to confirm resolution or the need for tissue biopsy.
- Recommendation 2 suggests that clinical lesions suspicious for a PMD be biopsied or referred for biopsy.
- In Recommendation 3, the panel did not recommend cytologic testing of PMDs, whether innocuous or suspicious. It was suggested that cytologic testing be reserved for patients who decline scalpel biopsy to obtain additional assessment of an oral PMD.
- In Recommendation 4, the panel did not recommend tissue reflectance or autofluorescence for the evaluation of PMDs. Although not written as part of the recommendation, both manuscripts indicated these adjuncts were not recommended as replacements for CVTE and their routine use might best be limited to secondary or tertiary settings (e.g., a specialist’s office, such as an oral and maxillofacial pathologist).
- Recommendation 5 suggests that no further action is needed (beyond normal recall visits) for patients with no symptoms or clinically evident lesions, per the CVTE.
- Recommendation 6 did not suggest the use of commercially available salivary adjuncts for the evaluation of PMDs among patients with or without either clinically evident innocuous or suspicious features. At the present time, their use should only be considered in the context of research.
SUMMARY
Patients routinely undergo a CVTE as part of their comprehensive care by dental professionals. In concert with the clinician’s training and experience, this examination is used to help detect and diagnose a broad array of diseases and abnormalities. While oral cancer is a particular concern of many patients, it is a relatively uncommon malignancy that is usually preceded by a characteristic mucosal lesion (e.g., a PMD) that is readily detectable by a CVTE. After an oral PMD has been detected, follow-up evaluation may be indicated, with or without conservative therapy.
For persistent or progressive lesions, or those with suspicious clinical features, clinicians should arrange for a biopsy to obtain a diagnosis and direct further treatment, as needed. With specialized training in anatomy and diseases of the head and neck, dental professionals are the gatekeepers of oral health. Providers are encouraged to educate patients about the importance of regular dental check-ups — including a thorough CVTE of the head and neck — as part of a comprehensive health care strategy.
References
- Bouquot JE. Common oral lesions found during a mass screening examination. J Am Dent Assoc. 1986;61:50–57.
- Christian DC. Computer-assisted analysis of oral brush biopsies at an oral cancer screening program. J Am Dent Assoc. 2002;133:357–362.
- Lingen MW, Abt E, Agrawal N, et al. Evidence-based clinical practice guideline for the evaluation of potentially malignant disorders in the oral cavity: a report of the American Dental Association. J Am Dent Assoc. 2017;148:712–727.
- Lingen MW, Tampi MP, Urquhart O, et al. Adjuncts for the evaluation of potentially malignant disorders in the oral cavity: diagnostic test accuracy systematic review and meta-analysis–a report of the American Dental Association. J Am Dent Assoc. 2017;148:797–813.
- Lingen MW, Kalmar JR, Karrison T, Speight PM. Critical evaluation of diagnostic aids for the detection of oral cancer. Oral Oncol. 2008;44:10–22.
- Downer MC, Moles DR, Palmer S, Speight PM.A systematic review of test performance in screening for oral cancer and precancer. Oral Oncol. 2004;40:264–273.
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2018. CA Cancer J Clin. 2018;68:7–30.
- Lingen MW, Xiao W, Schmitt A, et al. Low etiologic fraction for high-risk human papillomavirus in oral cavity squamous cell carcinomas. Oral Oncol. 2013;49:1–8.
- Poling JS, Ma XJ, Bui S, et al. Human papillomavirus (HPV) status of non-tobacco related squamous cell carcinomas of the lateral tongue. Oral Oncol. 2014;50:306–310.
- LeHew CW, Weatherspoon DJ, Peterson CE, et al. The health system and policy implications of changing epidemiology for oral cavity and oropharyngeal cancers in the United States from 1995 to 2016. Epidemiol Rev. 2017;39:132–147.
- Tota JE, Anderson WF, Coffey C, et al. Rising incidence of oral tongue cancer among white men and women in the United States, 1973-2012. Oral Oncol. 2017;67:146–152.
- Patel SC, Carpenter WR, Tyree S, et al. Increasing incidence of oral tongue squamous cell carcinoma in young white women, age 18 to 44 years. J Clin Oncol. 2011;29:1488–1894.
- Kalmar JR. Advances in the detection and diagnosis of oral precancerous and cancerous lesions. Oral Maxilofacial Surg Clin N Am. 2006;18:465–482.
- Moore C, Catlin D. Anatomic origins and locations of oral cancer. Am J Surg. 1967;114:510–513.
- Mehrotra R, Singh M, Thomas S, et al. A cross-sectional study evaluating chemiluminescence and autofluorescence in the detection of clinically innocuous precancerous and cancerous oral lesions. J Am Dent Assoc. 2010;141:151–156.
- Farah CS, McIntosh L, Georgiou A, McCullough MJ. Efficacy of tissue autofluorescence imaging (VELscope) in the visualization of oral mucosal lesions. Head Neck. 2012;34:856–862.
- McNamara KK, Martin BD, Evans EW, Kalmar JR. The role of direct visual fluorescent examination (VELscope) in routine screening for potentially malignant oral mucosal lesions. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;114:636–643.
- Ganga RS, Gundre D, Bansal S, Shirsat PM, Prasad P, Desai RS. Evaluation of the diagnostic efficacy and spectrum of autofluorescence of benign, dysplastic and malignant lesions of the oral cavity using VELscope. Oral Oncol. 2017;75:67–74.
- Ebersole JL, Steffen MJ, Thomas MV, Al-Sabbagh M. Smoking-related cotinine levels and host responses in chronic periodontitis. J Periodontal Res. 2014;49:642–651.
- Martin JL, Gottehrer N, Zalesin H, et al. Evaluation of salivary transcriptome markers for the early detection of oral squamous cell cancer in a prospective blinded trial. Compend Contin Educ Dent. 2015;36:365–373.
- Jaedicke KM, Preshaw PM, Taylor JJ. Salivary cytokines as biomarkers of periodontal diseases. Periodontol 2000. 2016;70:164–183.
- Ghallab N, Shaker O. Salivary-soluble CD44 levels in smokers and non-smokers with chronic periodontitis: a pilot study. J Periodontol. 2010;81:710–717.
- Zhan Y, Zhang R, Lv H, et al. Prioritization of candidate genes for periodontitis using multiple computational tools. J Periodontol. 2014;85:1059–1069.
- D’Souza, Wentz A, Kluz N, et al. Sex differences in risk factors and natural history of oral human papillomavirus infection. J Infect Dis. 2016;213:1893–1896.
- Kreimer AR, Pierce Campbell CM, Lin HY, et al. Incidence and clearance of oral human papillomavirus infection in men, the HIM cohort study. Lancet. 2013;382:877–887.
- Beachler DC, D’Souza G, Sugar EA, Xiao W, Gillison ML. Natural history of anal vs oral HPV infection in HIV-infected men and women. J Infect Dis. 2013;208:330–339.
- Beachler DC, Guo Y, Xiao W, et al. High oral human papillomavirus type 16 load predicts long-term persistence in individuals with or at risk for HIV infection. J Infect Dis. 2015;212:1588–1591.
- Rethman MP, Carpenter W, Cohen EE, et al. Evidence-based clinical recommendations regarding screening for oral squamous cell carcinomas.J Am Dent Assoc. 2010;141:509–520.
Featured image by WEBPHOTOGRAPHEER/E+/GETTY IMAGES PLUS
From Decisions in Dentistry. March 2018;4(3):45-46,49-51.





[…] To read more about oral cancer evaluation, click here: https://decisionsindentistry.com/article/head-neck-evaluation-dental/ […]