 FG TRADE/ISTOCK/GETTY IMAGES PLUS
FG TRADE/ISTOCK/GETTY IMAGES PLUS
Face Shield Use During the COVID-19 Pandemic
Face shields play an important role in clinical protection against COVID-19 transmission, particularly during dental procedures that create large particles and droplets.
This course was published in the February 2022 issue and expires February 2025. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Explain the use and benefits of face shields as adjuncts to personal protective equipment during dental care.
- List agencies that provide recommendations and standards pertaining to face shields in clinical practice.
- Describe the limitations of face shields when used during aerosol-producing dental procedures.
In early 2020, the rapid spread of the COVID-19 pandemic led to widespread awareness of the public health threat posed by the SARS-CoV-2 pathogen.1 As part of routine care, the U.S. Centers for Disease Control and Prevention (CDC) recommends the universal use of personal protective equipment (PPE) for healthcare personnel.2 Additionally, the CDC states, “Eye protection (i.e., goggles or a face shield that covers the front and sides of the face) should be worn during all patient care encounters.”2
The specter of COVID-19 has underscored the importance of protecting the eyes, nose, mouth and face from bodily fluids. While face shields are classified as PPE,3 they were not routinely worn in most dental settings prior to the pandemic. The federal Occupational Safety and Health Administration specifies that “PPE selected must be appropriate for the task.”4 The Bloodborne Pathogens standard (29 CFR 1910.1030) states, “When splashes, spray, spatter, or droplets of blood or other potentially infectious materials pose a hazard to the eyes, nose or mouth, then masks, in conjunction with eye protection (such as goggles or glasses with solid side shields) or chin-length face shields, must be worn.”4
Prior to the pandemic, the American National Standards Institute (ANSI) and International Safety Equipment Association (ISEA) did not have universal standards for design, testing, manufacturing, or performance of face and eye protection, including face shields, from biological hazards.3 The pandemic highlighted the need to develop standards for eye and face protection for high-risk occupations. As such, the recent ANSI/ISEA Z87.62-2021 standard spells out requirements regarding the safety and efficacy of face shields for protection against blood and bodily fluids.5
While face shields provide a barrier and some protection from direct splashes and spatter, they do not protect the wearer from small airborne particles.1,3 A medical/surgical face mask and eye protection must be worn in addition to a face shield during aerosol-producing dental procedures.3,4,6
EVIDENCE-BASED FINDINGS
The COVID-19 pandemic spurred interest in research on aerosols, fluid dynamics, and the effectiveness of PPE. Thus, recent studies have greatly improved the understanding of how airborne particles behave during a variety of circumstances. Should they choose to use a face shield, oral health professionals may wish to become familiar with this body of knowledge so they can select the most effective model for their circumstances.
In a simulation of a patient coughing, Lindsley et al7 found the face shields tested were able to decrease exposure of large particles by 96% immediately following a cough. When small aerosolized particles were produced, however, the face shield demonstrated 68% effectiveness. Large droplets settled more quickly than small particles because small aerosols are suspended in the air for longer periods, and the distance aerosolized particles travel reduces the level of protection provided by face shields. Based on the results, however, the researchers determined face shields can serve as an adjunct to reduce exposure to respiratory infections.
Salimnia et al8 compared the levels of protection provided by face masks and face shields by simulating talking and exhaling via an aerosol-generating system. They determined a face shield alone did not provide protection during the simulated bacterial transmission. Surgical masks alone provided what the authors characterize as “good” protection. And while the authors note the combined use of a surgical mask and face shield provided the best protection, they note the “combined protection was similar to surgical masks alone.”

Ronen et al9 investigated face shields as a substitute for surgical masks using a simulator and an airbrush diffuser to simulate a cough. As expected, researchers found higher levels of contamination to the cheek and neck regions closer to the periphery of the shield. Face shields designed with extended coverage below the chin (height = 29.5 cm) and covering the entire side of the face (width = 40.0 cm) may improve their efficacy in blocking particles.

SYSTEMATIC REVIEW
A systematic review by Samaranayake et al1 included 21 studies evaluating the effectiveness of face masks, respirators and protective eyewear. Only one of the studies involved aerosol-generating procedures in a dental setting,1,10 during which aerosol contamination was measured on blood agar plates placed around the patient chair headrest. The clinicians’ masks, gowns and head caps were also tested for microbes. The authors concluded face shields were inferior to masks in preventing penetration of aerosols due to openings around the shields.10 In Samaranayake et al’s1 research, 12 of the reviewed studies used a simulated model and/or laboratory-controlled settings — yet simulated models and lab settings do not necessarily replicate the environment or circumstances of actual dental procedures in clinical settings.
The other eight studies in the systematic review tested mask and respirator contamination, but did not include the effectiveness of face shields. Samaranayake et al1 concluded that a combination of eye protection and face shields, in addition to masks and/or respirators, provided the best protection against aerosol-generated bacterial transmission. Another consideration is that most of the studies were conducted using manikins in an upright face-to-face or side-facing position, rather than in a supine position. A supine position may significantly change the direction of air flow from a patient during dental procedures, and thus should be considered when selecting a face shield.
DESIGN AND STRUCTURE
While ANSI/ISEA sets the standards for design, performance and manufacturing in accordance with its Z87.1-2020 document for the vast majority of commercial eye and face protection used in the United States,11 there is no standard or regulation of face shields specific to dentistry (beyond the ANSI/ISEA Z87.62-2021 biological hazards standard).
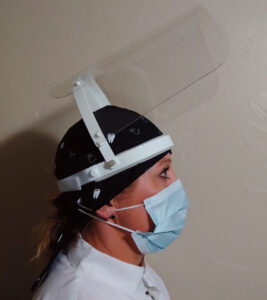
A face shield has three basic components: frame, visor, and suspension system. When choosing a frame, also referred to as headgear, several factors should be considered, including durability, weight and adjustability.3 To support comfort, a lightweight durable plastic is usually best. Some frames can be adjusted to accommodate personal eyewear, loupes and/or a headlight, and fully or partially encircle the circumference of the head (Figure 1). Some allow for detachable visors for easy replacement. In addition, frames can now be custom made to fit an individual’s head using a three-dimensional (3D) scan and 3D printer.12
Visors, or windows, are generally attached to the frame and can be removable or fixed. Made from a variety of materials — including polycarbonate, cellulose acetate, polyvinyl chloride, and polyethylene terephthalate glycol — visors come in several widths, lengths and strengths.13 Most medical and dental visors are made from acetate, as it provides the best clarity and tends to be the most scratch resistant when cleaned multiple times daily. Treating a visor with anti-glare, anti-fogging, ultraviolet light and scratch-resistant coatings can extend its longevity.
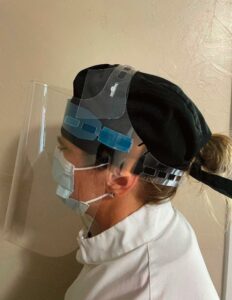
A suspension system is the mechanical interaction of springs and shock absorbers that interlock a device. A face shield’s suspension system can fully or partially encompass the head or neck. An elastic band, ratchet-adjusting plastic headband, hook-and-loop fasteners, or pin-lock systems are some of the circumferential suspension systems on the market.3 Eyeglass attachments or a neck brace may be included in partially circumferential suspension systems. On many face shield models, foam is placed on the interior forehead area for comfort and absorption (Figure 2).

SELECTION AND USE
Choosing a face shield and using it properly depend on use and the anticipated risks of the procedure. Currently, the CDC does not offer a recommendation or requirement specific to face shields in the dental office, only protective eyewear (which would include face shields, of course).2 Aerosols, splashes and spray can flow around the shield; consequently, a face shield should never function as the primary source of respiratory protection and should always be used in combination with a face mask.1 While thickness is not a major consideration, the shield’s length, design and aerodynamics are key features to evaluate. The shield should extend to the ear, below the chin, and cover the forehead to ensure maximum protection from infectious particles (Figure 2 through Figure 5).3
When choosing a face shield, airflow is an important consideration. Viola et al14 studied the airflow generated by a cough of a patient in a supine position, with the clinician in the 12 o’clock position. The team concluded that when the clinician positioned his or her hands for the procedure directly in the particle airflow, hand interference dispersed airflow upward toward the clinician’s chin. As such, a face shield would have to extend below the clinician’s chin to minimize the risk of exposure to a direct cough. Consequently, the directionality of the airflow should be a design consideration in face shield selection (Figure 6).

Suspension of air-generated particles is another key consideration. A systematic review by Innes et al15 found that particles remained in the air for two to six hours, depending on the specific aerosol-generating procedure. Therefore, a commercial, heavy-duty face shield, with coverage below the chin, over the head, and extending past the ears, will improve protection.
Roberage3 reviewed the pros and cons of face shields in relation to other PPE. The disadvantages include fogging and glare that can interfere with visual clarity, while the advantages include:
- Shields cover a larger portion of the face than standard eyewear
- Ability to wear with other eye and facial PPE
- Face shields provide protection from touching and potentially contaminating a mask and facial structures
- Ability to easily disinfect
- Relatively inexpensive
CONCLUSION
Face shields vary in design, function and efficacy. They offer a physical barrier, and may be indicated for procedures that produce large particles and droplets, but they are less effective in protecting against aerosols. Face shields serve as an adjunct and should not be used as a substitute for suitable eye and respiratory protection. Achieving the highest levels of protection against COVID-19 and other respiratory diseases necessitates wearing appropriate clinical clothing, gloves, a face mask or respirator, goggles, and/or a face shield that provide protection from the transmission of potentially infectious agents. Additional well-designed, controlled studies that mimic real-life dental procedures are needed to determine the most effective PPE to ensure oral health professionals are protected from transmissible diseases.
REFERENCES
- Samaranayake LP, Fakhuruddin KS, Ngo HC, Chang JWW, Panduwawala C. The effectiveness of respiratory protective equipment (RPE) in dentistry and other health care settings: a systematic review. Acta Odontol Scand. 2020;78:626–639.
- U.S. Centers for Disease Control and Prevention. Interim Infection Prevention and Control Recommendations for Healthcare Personnel During the Coronavirus Disease 2019 (COVID-19) Pandemic. Available at: https://www.cdc.gov/coronavirus/2019-ncov/hcp/infection-control-recommendations.html. Accessed January 10, 2022.
- Roberage RJ. Face shields for infection control: a review. J Occup Environ Hyg. 2016;13:235–242.
- U.S. Occupational Safety and Health Administration. Personal Protective Equipment (PPE) Reduces Exposure to Bloodborne Pathogens. Available at: https://www.osha.gov/sites/default/files/publications/bbfact03.pdf. Accessed January 10, 2022.
- International Safety Equipment Association. ANSI/ISEA Z87.62-2021. Available at: safetyequipment.org/ product/ansi-isea-z87-62-2021/. Accessed January 10, 2022.
- Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection control in dental health-care settings — 2003. MMWR Recomm Rep. 2003;52(RR-17):1–61.
- Lindsley WG, Noti JD, Blachere FM, Szalajda JV, Beezhold DH. Efficacy of face shields against cough aerosol droplets from a cough simulator. J Occup Environ Hyg. 2014;11:509–518.
- Salimnia H, Meyer MP, Mitchell R, et al. A laboratory model demonstrating the protective effects of surgical masks, face shields, and a combination of both in a speaking simulation. Am J Infect Control. 2021;49:409–415.
- Ronen A, Rotter H, Elisha S, et al. Investigation of the protection efficacy of face shields against aerosol cough droplets. J Occup Environ Hyg. 2021;18:72–83.
- Bentley CD, Burkhart NW, Crawford JJ. Evaluating spatter and aerosol contamination during dental procedures. J Am Dent Assoc. 1994;125:579–584.
- International Safety Equipment Association. ANSI/ISEA Z87.1-2020 Standard. Available at: https://safety equipment.org/isea-standards/ansiisea-z87-accredited-standards-committee/ansiisea-z87-1-2020standard/. Accessed January 10, 2022.
- Zhang PC, Ahmed Y, Hussein IM, Afenu E, Feasson M, Daud A. Optimization of community-led 3D printing for the production of protective face shields. 3D Print Med. 2020;6:35.
- Grainger. Face Shield Protection. Available at: grainger.com/know-how/safety/ppe-in-the-workplace/eye-face-protection/kh-face-shield-protection-373-qt. Accessed January 10, 2022.
- Viola IM, Peterson B, Pisetta G, et al. Face coverings, aerosols dispersion and mitigation of virus transmission risk. IEEE Open J Eng Med Biol. 2021;2:26–35.
- Innes N, Johnson IG, Al-Yaseen W, et al. A systematic review of droplet and aerosol generation in dentistry. J Dent. 2021;105:103556.
From Decisions in Dentistry. February 2022;8(2):36-39.




