Diagnosis and Prognosis for Dark Tooth Bleaching
Due to multiple possible etiologies, the following case reports help illustrate variations in the diagnosis and treatment of a dark tooth.
Bleaching teeth can involve all the teeth, a single dark tooth, or clinically unique situations. While rare, there are also some unusual black discolorations that dentists should carefully evaluate prior to bleaching, whether the treatment plan is to use internal or external bleaching.
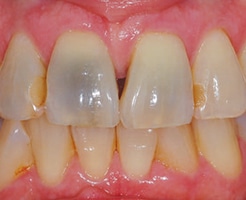
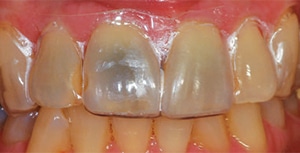
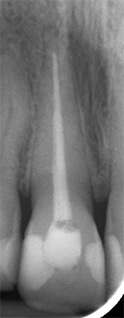
There are a number of possible diagnoses for a black area on an anterior tooth. The first concern is the possibility of internal resorption, which may manifest in a black or darkened discoloration (Figure 1). There could also be remaining materials in the pulp chamber or pulp horns of an endodontically treated tooth. Additionally, the tooth may have previously had amalgam placed (with or without endodontic therapy), and the discoloration is an amalgam stain. Other possibilities include caries, a dark restoration, or a leaking restoration that is showing through to the facial (Figure 2). Even some tetracycline antibiotics can cause a dark black or grey stain in one location of the tooth.
The following case reports demonstrate some variations in the diagnosis and treatment of blackened discolorations.
endodontically treated right central incisor resulted from internal resorption, which had to be cleaned out by going inside the tooth.
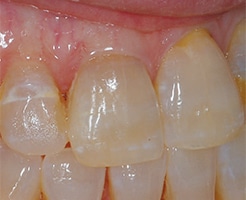
endodontically treated right central
incisor was due to a leaking lingual
composite restoration. The issue was
resolved by replacing the restoration.
CASE 1
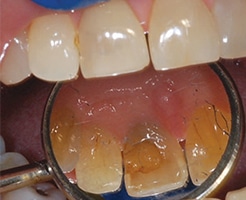
A 69-year old female presented with two large black areas on her maxillary central incisors (Figure 3). An examination revealed two lingual composite restorations, with staining on the adjacent tooth structure consistent with amalgam staining (Figure 4). The patient reported a previous dentist had removed the amalgams in an attempt to change the color, but with no success. However, it is always best to remove old amalgams with staining prior to bleaching, as previous reports have indicated the tooth can turn green around the old amalgam during bleaching.1 A periapical radiograph revealed neither tooth had received endodontic therapy, nor were there any indications of pathology.
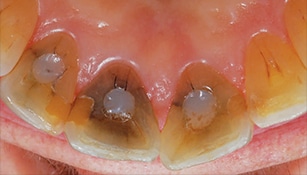
Photographs were taken on facial and lingual. A maxillary alginate impression was made and a subsequent cast generated. The cast was trimmed from the base to a horseshoe shape, with no vestibule and the central incisors perpendicular to the base. A variation of single-tooth bleaching tray was used to cover only the central incisors.2 The tray was fabricated from a thin, soft material and allowed to sag 1 inch in the vacuum former before applying the vacuum. Reservoirs or spacers were not used, as they are not required to bleach teeth when using a low concentration of 10% carbamide peroxide (CP). When fabricating a single-tooth bleaching tray, the tray should extend 2 to 4 mm onto the attached gingival, rather than scalloped to follow the free gingival margin. Scalloping or trimming the tray to the free gingival margin will not allow the tray to remain intact for the fabrication of a single-tooth tray.3 If a full tray is fabricated, the response to bleaching for the single tooth may not coincide with the adjacent teeth, so the smile will still have a single dark tooth, except that all the teeth will be lighter.
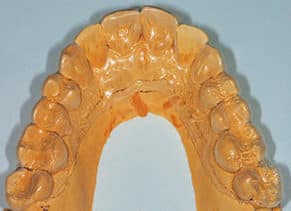
extends onto the tissue on palate and facial
in a nonscalloped, no-reservoir design.
The tray should be trimmed such that it extends further onto the palate than a typical bleaching tray to allow adjacent tooth mold removal without sectioning the tray. Next, the teeth molds on either side of the two single dark teeth were removed so the bleaching material will only be in contact with the treated teeth (Figure 5). A normal single dark tooth usually takes at least eight weeks of bleaching with 10% CP to see a final result.3 The patient was informed that her other restorations would not change color, and if the dark spots were not removed by bleaching, the dark spots will become more noticeable as remainder of tooth becomes lighter. Other options would include composite restorations, porcelain veneers, or crowns to cover the discoloration. However, in each case it would be easier to create natural-looking esthetics when the teeth are lighter, with less darkness to block out.
PATIENT PREFERENCE
The patient preferred to attempt bleaching first, understanding the poor prognosis. She was given the custom bleaching tray and 12 syringes of 10% CP, as well as an instruction sheet. A 10% formulation works well with a nonscalloped, no reservoir tray because 10% CP is designed to contact tissue (Figure 6). Since the teeth were vital, the patient was also given instructions for treating any possible sensitivity. The best approach for potential sensitivity is to use 5% potassium nitrate toothpaste for brushing two weeks prior to bleaching;4 the dentifrice can also be used directly in the bleaching tray5 for 10 to 30 minutes.
When applied in a tray, 5% potassium nitrate penetrates the enamel and dentin in approximately 30 minutes; it will also reduces the excitability of the nerve.6 The patient was instructed to brush with the 5% potassium nitrate toothpaste throughout treatment, as well as place it in the tray for 30 minutes instead of the bleaching material if the teeth became sensitive.
The patient bleached nightly for approximately six months until the teeth no longer were changing color. There were no episodes of sensitivity. The two central incisors bleached lighter, but the black areas remained (Figure 7). Due to the excellent response of the nonstained areas of the central incisors, the patient requested to bleach all of her teeth. The same cast was used to generate a full-mouth, nonscalloped, no-reservoir tray to bleach the remaining teeth. There was no need to remove any tooth molds in the tray because the central incisors had already reached their maximum lightness.
A smile analysis revealed a chipped mesio-incisal on tooth #10, and a large composite on #7. The proposed treatment was to replace those, and, when replacing the distal of #8, to remove the previous composite restoration to determine if any further stain removal could be accomplished before considering restorative therapy. The patient was not able to return for further treatment, however.
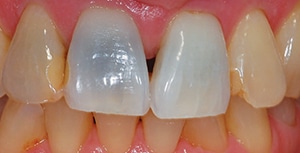
the tooth structure was significantly lightened.
This case demonstrates the difficulty in removing amalgam stains. As some of the older amalgams remain in a tooth, the tin, silver and copper tend to diffuse into the tooth, rather than mercury.7 The only historical reference from the 1800s for removing amalgam stains involves the use of cyanide of potassium, but that treatment was applied to a nonvital tooth that had received endodontic therapy.8 It is unknown at this time whether that caustic, poisonous material can still be used, or whether it would work on vital teeth from the outside in.
CASE 2
The patient’s chief complaint was a single blackened anterior tooth that had received endodontic therapy approximately 20 years ago in another country (Figure 8). A radiograph did not reveal any pathology (Figure 9), however, the gutta-percha extended occlusally into the pulp chamber. Because the tooth was endodontically treated and the contents of the pulp chamber were unknown, the first option was to remove the composite restoration and explore the pulp chamber due to the possibility that internal resorption was causing the discoloration. The patient chose not to have any anesthesia. Isolation was achieved through a rubber dam placed from teeth #6 to #11.
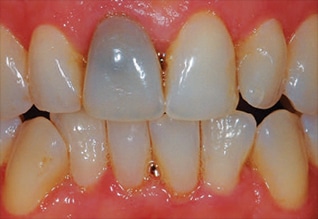
the extent of the blackened area.
Upon removal of the previous composite restoration and exploration of the endodontic access, staining was apparent in small amounts on mesial and distal composite restorations, and along the internal walls of the endodontic access (Figure 10). It was hypothesized the sealer used in the previous endodontic therapy contained silver nitrate or some compound that resulted in the discoloration. Approximately 4 mm of gutta-percha was removed until the gutta-percha was 2 mm below the cementoenamel junction, and the internal walls were cleaned with a #6 Gates-Glidden bur.
the extent of the blackened area.
The gutta-percha remaining in the floor of the pulp chamber was sealed with a layer of glass ionomer. The reason for sealing the remaining gutta-percha is that previous cases of resorption reported in the literature involving bleaching with 35% hydrogen peroxide (HP) noted the gutta-percha had not been sealed.9 At present, that step is a standard approach to internal bleaching, regardless of the bleaching material used. A single drop of 20% CP was placed in the depth of the chamber without contacting the margins of the opening, and covered with a large cotton pellet. As a bleaching agent, CP has been shown to be as effective as sodium perborate,10 and avoids the use of the caustic 35% HP previously used in bleaching anterior teeth (and that has been associated with resorption). Using CP has also been shown to elevate the pH due to the urea.11 Low pH is another factor cited in resorption cases, and HP has a pH of approximately 5. The chamber was closed by restoring with a resin-modified glass ionomer. Normally the use of the chosen glass ionomer requires a mild acid conditioner to achieve maximum bond strength and seal. However, cavity conditioner was not used in this “walking bleach technique” due to the temporary nature of the restoration and plans for removal later. If any leakage occurs, the material would not be caustic to the oral cavity because it is often used for tray bleaching. The restoration was adjusted for smoothness and checked for occlusion.
COST AND TIME EFFICIENCIES
Upon completion of the pulp chamber cleaning, the patient reported being satisfied with the initial result (Figure 11), as there was a drastic color difference noted after removal of the old sealer. The patient was informed the results of this further bleaching treatment were as yet unknown. If the internal bleaching did not achieve lightening of the gingival third of the tooth as desired, the next step would be the use of a single-tooth bleaching tray. An alternative option if tray fabrication was not desired would be to continue to change the CP weekly for several appointments. However, the unknown number of subsequent appointments (up to six) often creates difficulty for the patient and dentist in both time and cost, so having the patient continue bleaching with the tray is more time-efficient and cost-efficient for both parties.
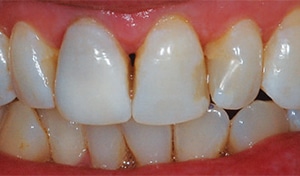
The patient returned for evaluation after the first internal bleaching treatment (Figure 12). The patient was pleased with the color of the tooth, so a decision was made to restore the tooth with no further bleaching. Should the tooth become slightly darker in time, a single-tooth bleaching tray could be used externally to attempt to further lightening. The removal of the black area also highlighted the discoloration of the interproximal composite restorations, and the patient agreed to their replacement for optimal esthetics.
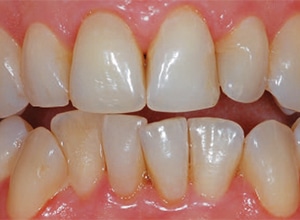
The teeth were cleaned of any surface stains, isolated with a rubber dam, and the temporary restoration was removed on tooth #8. The preparation was extended to the mesial aspect of the tooth once the older composite was removed (Figure 13). There was a connection between the endodontic opening and disto-lingual (DL) restoration on #8, but the decision was made not to replace the DL since it was a reasonable restoration. After etching the tooth with 37% phosphoric acid, a primer and adhesive were applied and the tooth restored with an opaque composite B1 shade. The patient reported being pleased with the final look and feel of the restoration (Figure 14). The patient was told the color might change as the teeth rehydrate, and if the color change was significantly darker, external bleaching would be initiated.
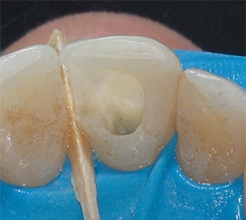
composite restoration, as well as a
proximal composite restoration, shows
clean dentin in the pulp chamber from
the bleaching procedure.
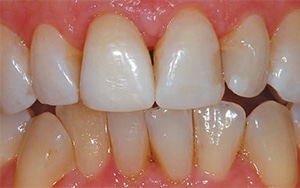
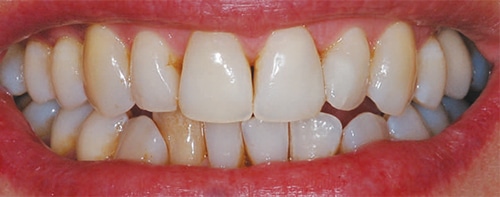
After one week, the patient returned and was pleased with the stabilized shade (Figure 15). At this time, the decision was made not to bleach externally unless the tooth later darkened. Once the inside of the pulp chamber had been cleaned, there was no need to reenter the chamber, but the tooth could be rebleached from the “outside-in” using a single-tooth tray.
DISCUSSION
These two cases represent very different outcomes from similar black stains. Amalgam stains have historically been the most difficult to treat, with the only literature reference to their removal involving the use of potassium cyanide in a nonvital anterior tooth.8 However, the patient in Case 1 presented with a vital tooth, and the potassium cyanide technique is unclear in the literature.
The endodontically treated tooth in Case 2 involved material discolorations of unknown origin, so the prognosis was unknown. However, the ability to explore the pulp chamber and remove discolored materials — in addition to bleaching — aids in a better prognosis. A screening radiograph should be included for any bleaching procedure, whether on vital or nonvital teeth.12 Even with a poor prognosis from the unknown response of the teeth, the relatively low cost and safety make bleaching the first choice after removal of the discolored materials.
CONCLUSIONS
Black areas on teeth can be the result of internal resorption, caries, leaking restorations, amalgam stains, or incomplete debridement of a root canal pulp chamber. Some tetracycline staining can also present as blackish-gray discoloration. Black and gray are the most difficult stains to remove with bleaching. Amalgam stains cannot be removed at this time by any known means, while other stains from dental materials or diseases may be successfully resolved.
Photographs should always be taken to establish a baseline and determine the progress of therapy. Often, combination treatments of bleaching or additional restorations may be required for a successful outcome. Use of a screening radiograph to help determine of the cause of the discoloration, a careful diagnosis, and providing patients with reasonable expectations are key elements of bleaching examinations and treatment planning.
KEY TAKEAWAYS
- There are a number of possible etiologies for a black area on an anterior tooth, which underscores the need for a careful examination, diagnosis and treatment planning.
- Possible causes for dark areas include internal resorption, decay, leaking restorations, amalgam stains, incomplete debridement of a root canal pulp chamber, and even staining from certain tetracycline antibiotics.
- Amalgam stains cannot be removed at this time by any known means, while other stains from dental materials or diseases may be successfully resolved.
- Photographs should always be taken to establish a baseline and determine the progress of therapy.
- Often, combination treatments of bleaching or additional restorations may be required for a successful outcome.
REFERENCES
- Haywood VB. Greening of the tooth-amalgam interface during extended 10% carbamide peroxide bleaching of tetracycline-stained teeth: a case report. J Esthet Restor Dent. 2002;14:12–17.
- Haywood VB. Current status of nightguard vital bleaching. Compend Contin Educ Dent Suppl. 2000;28:S10–S17;quiz S48.
- Haywood VB, DiAngelis AJ. Bleaching the single dark tooth. Inside Dentistry. 2010;6:42–52.
- Browning WD. Haywood VB. Hughes N, Cordero R. Prebrushing with a potassium nitrate dentifrice to reduce tooth sensitivity during bleaching evaluated in a practice-based setting. Compend Contin Educ Dent. 2010;31:220–225.
- Pashley DH, Tay FR, Haywood VB, Collins MA, Drisko CL. Consensus-based recommendations for the diagnosis and management of dentin hypersensitivity. Comp Contin Edu Dent. 2008;29(Spec Iss):1–35.
- Kwon SR, Dawson DV, Wertz PW. Time course of potassium nitrate penetration into the pulp cavity and the effect of penetration levels on tooth whitening efficacy. J Esthet Restor Dent. 2016;28:S14–S22.
- Wei SH, Ingram MJ. Analyses of the amalgam-tooth interface using the electron microprobe. J Dent Res. 1969;48:317–320.
- Kingsbury CA. Discoloration of dentine. The Dental Cosmos. 1861;3:57–60
- Nutting EB, Poe GS. Chemical bleaching of discolored endodontically treated teeth. Dent Clin North Am. 1967;Nov:655–662.
- Carneiro MV, Camargo CH, Carvalho CA, de Oliveira LD, Camargo SE, Rodrigues CM. Effectiveness of carbamide peroxide and sodium perborate in non-vital discolored teeth. J Appl Oral Sci. 2009;17:254–261.
- Leonard RH Jr, Austin SM, Haywood VB, Bentley CD. Change in pH of plaque and 10% carbamide peroxide during nightguard vital bleaching. Quintessence Int. 1994;25:819–823.
- Haywood VB. Pre-bleaching examination vital for optimum whitening. Compend Cont Edu Dent. 2012;33:76–77.
Van B. Haywood, DMD, has received research, grants and other financial or material support from Ultradent Products. Leigh Anne Fortney, BS, has nothing to disclose.
Featured image by BILL OXFORD/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. March 2019;5(3):10—12,14.