 ANGELIKA-ANGELIKA / ISTOCK / GETTY IMAGES PLUS
ANGELIKA-ANGELIKA / ISTOCK / GETTY IMAGES PLUS
Airflow Engineering Controls for the Dental Setting
A multidimensional approach is key to creating a safe practice environment.
This course was published in the November 2022 issue and expires November 2025. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
AGD Subject Code: 148
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss concerns over the risk of pathogenic transmission in dental settings and agencies or organizations that provide research and guidelines to help ensure a safe work environment.
- Describe the hierarchy of controls established by the U.S. Centers for Disease Control and Prevention and National Institute for Occupational Safety and Health.
- Explain engineering controls that mitigate the risk of cross-transmission in oral healthcare settings, including those posed by dental aerosols.
With the emergence of the SARS-CoV-2 pathogen, the risks posed by dental aerosols have become top of mind for oral health professionals. Fortunately, dentistry has a long history of incorporating infection prevention measures to create a safe environment for patients and practitioners. The low incidence of COVID-19 transmission in dental settings is a testament to an effective combination of educational programing, policies and procedures, as well as the dedication of dental team members in maintaining stringent protocols to limit the risk of cross-contamination.
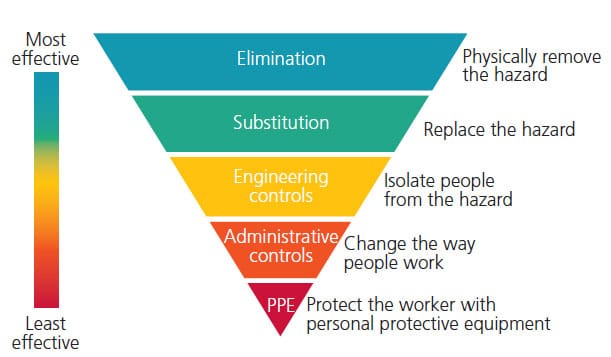
Multiple agencies, including the U.S. Centers for Disease Control and Prevention (CDC), Occupational Safety and Health Administration, National Institute for Occupational Safety and Health (NIOSH), and Organization for Safety, Asepsis and Prevention (OSAP), provide current scientific research and information to assist oral health professionals in creating a healthy and safe work environment. The COVID-19 pandemic has forced dentistry to reevaluate infection prevention measures with a focus on the hierarchy of controls that includes elimination and substitution, along with engineering and administrative controls, as well as the use of personal protective equipment (PPE).1 This paper will focus chiefly on engineering controls aimed at reducing the risk from dental aerosols.
The CDC and NIOSH established a hierarchy of controls to identify and mitigate exposure to hazards before workers are exposed (Figure 1).1 Effective controls strive to eliminate or reduce risks to promote worker safety. While eliminating hazards is the most effective control, this is not always feasible in the dental setting. Attention to eliminating hazards in the design or early stages of any development makes this a more attainable and less expensive goal.1
Substitution involves replacing a hazard with nonhazardous options. An example of substitution is replacing radiographic film requiring chemical processing with digital radiography. Elimination and substitution have not been an option during the COVID-19 pandemic because the virus and variants continue to circulate across the globe. Theoretically, the virus could be eliminated if a vaccine was effective against all variants and everyone worldwide developed immunity.
ENGINEERING CONTROLS
Engineering controls do not eliminate hazards; rather, they isolate people from a hazard. Examples include installing physical barriers and use of high-volume evacuation, dental dams, instrument cassettes, needle recapping devices and sharps containers. During the pandemic, the CDC published the following recommendations for dental facilities to prevent the spread of airborne pathogens:2
- Space dental chairs at least six feet apart
- Place easy-to-clean physical barriers between patient chairs
- Orient operatories parallel with the direction of airflow
- The patient’s head should be positioned near return air vents, away from corridors, and toward a rear wall when feasible
High-efficiency heating, ventilation and air conditioning (HVAC) systems with high-efficiency particulate air (HEPA) filters enhance air quality throughout the office. Well-designed engineering controls can effectively boost productivity and worker comfort, as well as safety. Because it is not always possible to remove or reduce all hazards through elimination or substitution, engineering controls and administrative controls serve as the next level in the hierarchy.3
Administrative controls are thought to be less effective than other controls because they require additional effort by workers to adjust their work habits.1 Examples include preprocedural mouthrinsing, predispensing single-use items, avoiding aerosol-producing procedures, developing written policies and operating procedures, personnel training, immunization tracking, and adhering to a respiratory protection program.4
A primary example of a respiratory protection program is fit testing N95 masks or a reusable elastomeric half-mask respirator for each dental team member. Clinicians using N95 respirators should be fit tested annually. A fit test measures for any leakage to ensure a tight seal between the respirator and facial structure for each specific mask manufacturer, model and size.5 When purchasing N95 respirators, NIOSH certification indicates they have undergone rigorous testing and are a “legitimate particulate respirator.”5,6
Many oral health professionals are not aware the last line of defense in the hierarchy of controls is PPE, which is used to protect clinicians when other controls in the hierarchy cannot eliminate or mitigate hazards.1 Gowns, masks or N95 respirators, eye protection (such as goggles or face shields), and gloves should be used appropriately for the specific procedure(s) performed.2
CONTROLLING AIR FLOW AND VENTILATION
While the quality of ambient air is not readily observable, it is critical in preventing the spread of viruses and disease. Increasing outside air flow and ventilation are important in minimizing exposure to aerosols and contaminants in the dental setting. The American Institute of Architects established guidelines to address indoor air-quality standards.7 As new dental facilities are built and older ones renovated, engineering controls are needed to mitigate dental aerosols. A primary control is regulating outside airflow and reducing aerosols through air filtration devices.7
The amount of time viruses remain airborne varies depending on their particle size, with smaller nano-sized particles staying airborne for up to 40 hours.8 Airborne particles are influenced by air currents created by fans, human movement, humidity and HVAC units.8 The primary types of air filtration are built-in HVAC systems and freestanding units that provide additional air filtration. The need for freestanding units is based on the efficacy of the HVAC system, room size and occupancy.9
The HVAC system consists of the building’s central heating and cooling equipment. As air is circulated within the system, it runs through a filter to remove contaminants from the air before recirculating into the building. This system serves as the principal mover of air within a building.9 Installing a high-efficiency filter within the HVAC system may provide a sufficient level of protection to negate the need for freestanding air filtration units. Airflow within buildings is affected by numerous factors, including furniture and walls, people moving, and open windows and doors, all of which create areas of higher and lower pressure.9 All air filtration systems should be evaluated for the cubic feet of air the system can process (also referred to as the air exchange rate), and the rating of the specific air filter. Even if the HVAC system is capable of providing quality environmental air, the addition of freestanding air purification systems can greatly reduce the time it takes to clear a room of potentially infectious aerosols.2
In February 2022, the CDC released updated infection control recommendations for healthcare professionals that included using physical barriers and improving ventilation systems.2 Complementing these recommendations, the U.S. Environmental Protection Agency has identified steps to control indoor pollutants.9 Most dental professionals are familiar with the concept of source control and reducing aerosols with the use of high-volume evacuation. The other two recommendations may be less familiar: ventilation and air cleaning.
Two types of air filter ratings are used in HVAC and freestanding filtration systems: minimum efficiency reporting value (MERV) and HEPA.10 A MERV rating is based on testing developed by the American Society of Heating, Refrigerating, and Air-Conditioning Engineers, and describes the ability of a filter to collect particles between 10 microns down to 0.3 microns.9,10 In this system, a higher MERV rating correlates with improved air filtration. Particles of 0.3 microns are the most penetrating particle size.10
A common misconception is that particles smaller than 0.3 microns, such as SARS-CoV-2 at 0.125 microns, are not filtered as effectively. This is not necessarily true for several reasons. First, particles of 0.3 microns are the most challenging to filter, while particles both larger and smaller are filtered at much higher rates.10 In addition to their size, the ability to trap particles is influenced by how they move in the air. Smaller particles bounce around in the air in an irregular zigzag pattern known as Brownian motion.11 Second, for viruses to remain airborne, they must attach to a larger dust particle or water droplet, which can then be trapped in an air filter.
Recommended by the CDC, HEPA filtration is another fairly simple yet effective environmental control.2 These filters consist of a “mat of randomly aligned fibers, made from either glass or synthetic materials.”12 They are effective in removing 99.97% of most particles, including viruses and bacteria, but not gases such as nitrous or carbon dioxide (CO2).12 A HEPA filter’s MERV rating is 17 or higher.13 Both HVAC filtration and freestanding air purifiers reduce the volume of aerosolized pathogens. Initially, when turned on, air purifiers create substantial airflow disturbances and movement of nano-sized aggregates. However, continuous use can significantly reduce the overall concentration of respiratory droplets in the air.14 Running air purifiers and ventilation systems during working hours and up to two hours at the end of the business day is recommended.15
CARBON DIOXIDE MONITORING
Through processes such as simple respiration, CO2 can build up in a room, and higher CO2 levels indicate poor ventilation and/or an overcrowded room. High CO2 levels can result in pathogen-laden aerosols that negatively impact health.16 Measuring adequate ventilation in dental operatories can be accomplished with a consumer-grade CO2 monitor. Normal atmospheric CO2 levels are approximately 400 parts per million (ppm), whereas exhaled air might be as high as 40,000 ppm.16 A dental operatory with good ventilation should mirror outdoor CO2 levels. A recent study by Zemouri et al17 notes that “CO2 levels were found to play the most important role in the risk of disease transmission.” Levels at or above 1135 ppm potentially increase the risk of pathogen transmission.17 Therefore, monitoring CO2 levels in a dental office can help identify spaces that would benefit from increasing outdoor air flow or incorporating an adjunctive air treatment system.16,17
Inspired by the COVID-19 pandemic, OSAP’s 2020 infection control guidelines recommend proper ventilation and air filtration controls.15 The simplest way to enhance ventilation is to change the setting of the HVAC thermostat from “auto” to “on,” which keeps the air circulating through the HVAC filtration system throughout the day.18
UPPER-ROOM ULTRAVIOLET GERMICIDAL IRRADIATION
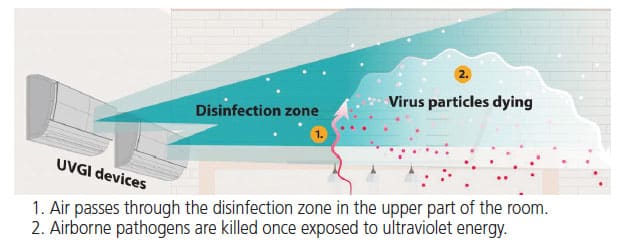
Upper-room ultraviolet germicidal irradiation (UR-UVGI) systems use ultraviolet energy to create a zone that kills airborne pathogens. These systems have a long history of substantial germicidal and tuberculocidal effects and eliminate pathogens as they enter the irradiated area in the upper portion of dental operatories. Ultraviolet-C irradiation has a short wavelength that breaks the bonds that hold a microorganism’s DNA and RNA strands together, thus destroying viral and bacterial pathogens, including SARS-CoV-2. Because ultraviolet-C irradiation can be dangerous to humans, the UR-UVGI system is installed within HVAC ducts or along the upper wall or ceiling of a room (Figure 2). This directs the ultraviolet-C energy toward the upper part of a room, ensuring occupants receive ultraviolet doses well below current safe exposure levels and preventing eye and skin damage.19,20
The COVID-19 pandemic has created an environment of innovation for multiple new air treatment options. Ideas such as ionization, dry hydrogen peroxide, and chemical fogging disinfection have emerged to combat the spread of the virus.15 Guidelines issued by OSAP recommend that oral health professionals exercise caution when using these new air treatment options, as the evidence related to efficacy and safety is not yet fully understood.15 Consulting a knowledgeable professional is recommended when installing and maintaining these engineering controls.
CONCLUSION
Creating a safe indoor environment requires a multidimensional approach. While it is not feasible to eliminate all airborne contaminants and hazards in the dental setting, disease transmission can be minimized by incorporating as many aspects of the hierarchy of controls as possible. This includes the use of high-efficiency HVAC systems with HEPA filters and/or freestanding air filtration units designed to mitigate the risks posed by dental aerosols.
REFERENCES
- The National Institute for Occupational Safety and Health. Hierarchy of Controls. Available at: https://www.cdc.gov/niosh/topics/hierarchy/default.html. Accessed September 28, 2022.
- U.S. Centers for Disease Control and Prevention. Interim Infection Prevention and Control Recommendations for Healthcare Personnel During the Coronavirus Disease 2019 (COVID-19) Pandemic. Available at: https://www.cdc.gov/coronavirus/떓-ncov/hcp/infection-control-recommendations.html. Accessed September 28, 2022.
- The National Institute for Occupational Safety and Health. Indoor Environmental Quality. Available at: https://www.cdc.gov/niosh/topics/indoorenv/buildingventilation.html. Accessed September 28, 2022.
- Occupational Safety and Health Administration. Respiratory Protection. Available at: https://www.osha.gov/respiratory-protection. Accessed September 28, 2022.
- U.S. Centers for Disease Control and Prevention. The Respiratory Protection Information Trusted Source. Available at: https://www.cdc.gov/niosh/npptl/topics/respirators/disp_part/respsource.html. Accessed September 28, 2022.
- OSHA Review. OSHA Requirements for Occupational Use of N95 Respirators in Healthcare. Available at: https://oshareview.com/떔/葐/osha-requirements-for-occupational-use-of-n95-respirators-in-healthcare/. Accessed September 28, 2022.
- U.S. Centers for Disease Control and Prevention. Environmental Infection Control Guidelines. Available at: https://www.cdc.gov/infectioncontrol/guidelines/environmental/index.html. Accessed September 28, 2022.
- Kumar PS, Subramanian K. Demystifying the mist: Sources of microbial bioload in dental aerosols. J Periodontol. 2020;91:1113–1122.
- U.S. Environmental Protection Agency. Building Air Quality Guide: A Guide for Building Owners and Facility Managers. Available at: https://www.epa.gov/indoor-air-quality-iaq/building-air-quality-guide-guide-building-owners-and-facility-managers. Accessed September 28, 2022.
- U.S. Environmental Protection Agency. What is a MERV rating? Available at: https://www.epa.gov/indoor-air-quality-iaq/what-merv-rating. Accessed September 28, 2022.
- Gustafsson O, Gustafsson S, Manukyan L, Mihranyan A. Significance of Brownian motion for nanoparticle and virus capture in nanocellulose-based filter paper. Membranes (Basel). 2018;8:90.
- Robertson P. What are HEPA filters and how do they work? Available at: https://smartairfilters.com/en/blog/what-is-hepa-filter-how-hepa-air-filter-work/. Accessed September 28, 2022.
- Henry Schein Dental. Air Management and Infection Control in the Dental Office Post COVID-19. Available at: https://henryscheinequipmentcatalog.com/content-library/air-management-infection-control. Accessed September 28, 2022.
- Heo KJ, Park I, Lee G, et al. Effects of air purifiers on the spread of simulated respiratory droplet nuclei and virus aggregates. Int J Environ Res Public Health. 2021;18:8426.
- Organization for Safety, Asepsis and Prevention. OSAP/CareQuest Institute Best Practices for Infection Control in Dental Clinics During the COVID-19 Pandemic. Available at: https://www.osap.org/best-practices-for-infection-control-in-dental-clinics-during-the-covid-19-pandemic. Accessed September 28, 2022.
- Huang Q, Marzouk T, Cirligeanu R, Malmstrom H, Eliav E, Ren YF. Ventilation assessment by carbon dioxide levels in dental treatment rooms. J Dent Res. 2021;100:810–816.
- Zemouri C, Awad SF, Volgenant CMC, Crielaard W, LaheiJ AMGA, de Soet JJ. Modeling of the transmission of coronaviruses, measles virus, influenza virus, Mycobacterium tuberculosis, and Legionella pneumophila in dental clinics. J Dent Res. 2020;99:1192–1198.
- U.S. Centers for Disease Control and Prevention. Ventilation in Buildings: Summary of Recent Changes. Available at: https://www.cdc.gov/coronavirus/떓-ncov/community/ventilation.html. Accessed September 28, 2022.
- U.S. Centers for Disease Control and Prevention. Upper-Room Ultraviolet Germicidal Irradiation (UVGI). Available at: https://www.cdc.gov/coronavirus/떓-ncov/community/ventilation/UVGI.html. Accessed September 28, 2022.
- Nunayon SS, Zhang HH, Lai ACK. Comparison of disinfection performance of UVC-LED and conventional upper-room UVGI systems. Indoor Air. 2020;30:180–191.
From Decisions in Dentistry. November 2022;8(11)40-43.




