7 Habits of Highly Effective Implant Clinicians – Part 2
The second installment of this series on screw-retained implants discusses the impact of occlusal forces and patient education on implant success.
Appearing in the February issue (available at decisionsindentistry.com), the first installment of this series on the seven habits of highly effective implant clinicians reviewed the high incidence of implant-abutment screw loosening, which represents the greatest prosthetic complication with single implant crowns.
Habit No. 1 discussed screw mechanics and explained why the screw should never be over-torqued or under-torqued, as either scenario will compromise the system’s optimum clamping force. In addition, the first installment defined key terminology, including torque, preload and clamping force. Habit No. 2 underscored the need to provide the specified torque by using calibrated tools (i.e., torque wrenches); it also outlined common errors when using these tools.
This installment, covering habits 3 and 4, will explain why screws tend to lose their preload over time (especially as related to occlusal forces), and the importance of patient education in implant maintenance and long-term success.
HABIT 3: BEGIN WITH THE END IN MIND
Nonaxial occlusal forces are the greatest challenge for implant-abutment screw joint stability. Even an optimally tightened, “perfect” implant screw joint can fail as a result of off-axial forces.1 Whenever possible, implant restorative occlusal surfaces, especially single restorations (where bracing from other connected implants does not exist), should be designed to transmit force through the long axis of the screw.
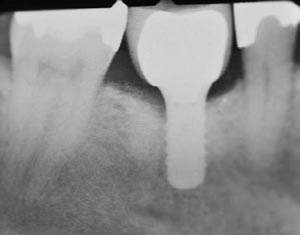
Occlusal changes and the cyclic function of mastication produce wear on implant components and the prosthetic tooth; additionally, erosion and other forces contribute to shifts in occlusion.2 While teeth have some ability for compensatory movement, implants do not. Recent evidence has shown that humans continue to experience facial and dentoalveolar growth, which again can alter the direction of occlusal forces. Thus, occlusion is dynamic, and implant restorations are less likely to absorb these forces.3–5 These changes are noted in the literature, with up to 50% of dental implants adjacent to natural teeth becoming infraocclusal within five years. What’s more, interocclusal contacts become lighter as early as three months post-implant restoration,3 and many result in open contacts (Figure 1). Bruxing, cantilevers and cyclic loading can also lead to premature screw-loosening events, especially in single-unit restorations.
Additionally, when a missing tooth is replaced with an implant, the maximum overall occlusal forces have been shown to increase within the first month of function. To reduce the risk of screw loosening, it is advisable to:
- Provide the patient with a nighttime wear retainer
- Regularly monitor and adjust the restoration, as required
- Assess open contact development and infraocclusal implant restorations, and correct as necessary
HABIT 4: PREVENTING BAD OUTCOMES
Dental implants are not without issues; for example, there is a reported 7% to 12% incidence of screw loosening over a six-year period.6 Mechanical issues, such as screw loosening, can be resolved if caught early. However, if such issues are not addressed, the screw, abutment, and even implant body can fracture. In addition, biological issues have been shown to occur due to micromovement and material wear. The biological sequalae of micromovement are peri-implant mucositis, a resolvable disease if caught early, or peri-implantitis, a permanent disease involving implant-supporting bone loss. Obviously, neither disease is desirable.
One way of maintaining healthy implant sites is to educate patients on what to expect from their dental implants. For example, the author provides a simple, concise, written handout in his practice. Patients should be informed that implant issues do occur, and thus regular evaluation of mobility and contacts is needed by both the dentist and patient.
Future installments in this series will discuss issues with measurement read errors with cantilever beam torque wrenches, the importance of using the correct implant components, and, finally, successful screw-tightening techniques.
BONUS WEB CONTENT
Dental Implants and Implant Restorations Handout

References
- Bickford JH. An Introduction to the Design and Behavior of Bolted Joints. Boca Raton, Fla: CRC Press; 1995.
- Kim YJ, Ko KH, Huh YH, Cho LR, Park CJ. Initial change in the occlusal force and occlusal contact area following single molar implant restoration. Int J Oral Maxillofac Implants. 2021;36:1139–1146.
- Varthis S, Tarnow DP, Randi A. Interproximal open contacts between implant restorations and adjacent teeth. Prevalence – causes – possible solutions. J Prosthodont. 2019;28:e806–e810.
- Bernard JP, Schatz JP, Christou P, Belser U, Kiliaridis S. Long-term vertical changes of the anterior maxillary teeth adjacent to single implants in young and mature adults. A retrospective study. J Clin Periodontol. 2004;31:1024–1028.
- Oesterle LJ, Cronin RJ Jr. Adult growth, aging, and the single-tooth implant. Int J Oral Maxillofac Implants. 2000;15:252–260.
- Goodacre BJ, Goodacre SE, Goodacre CJ. Prosthetic complications with implant prostheses (2001–2017). Eur J Oral Implantol. 2018;11(Suppl 1):S27–S36.
From Decisions in Dentistry. April 2022;8(4)20.


