Evolution of Caries Diagnosis
Identifying the presence of carious lesions and determining their activity are essential to effective treatment.
This course was published in the February 2018 issue and expires February 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
OBJECTIVES
- Explain key factors affecting caries detection, assessment and treatment.
- Describe classification systems and tools that aid lesion diagnosis and management.
- Discuss various new technologies for caries detection.
A greater understanding of dental caries has led to a paradigm shift in its management. Traditionally, surgical intervention was viewed as the initial course of treatment, but evidence now indicates that prevention is a better first step.1 Because caries is most effectively treated when caught early, accurate diagnosis of initial lesions is essential. Clinicians cannot rely on symptoms alone to aid in caries diagnosis because many are only apparent in the latter stages of caries progression.2 As the caries process continues, symptoms — such as pain and sensitivity to cold, hot or sweet substances — develop; however, without additional information, the mere presence of symptoms is not indicative of an active, ongoing caries process. An accurate diagnosis relies on identifying the presence of lesions, assessing lesion activity, and performing caries risk assessment.1,4–8 These components will help determine the best treatment approach.1,3
Large lesions are usually easier to diagnose because of the presence of obvious visual or radiological signs; conversely, initial lesions are more challenging to diagnose because uncertainty exists about their activity status. Indeed, they are often in a dynamic state, which varies from activity (demineralization or remineralization) to inactivity (arrested).2
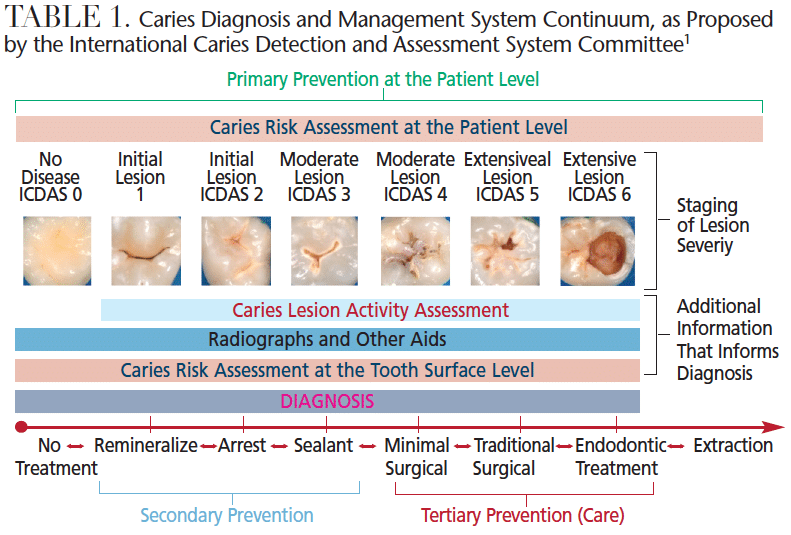
Systems that can support this new paradigm in dental caries management have garnered significant interest. The International Caries Detection and Assessment System (ICDAS) and American Dental Association Caries Classification System are evidence-based tools for assessing the severity of caries.4,5,9,10 They are based on direct visual examination of clean tooth surfaces. The ICDAS has seven categories (0 to 6) for every tooth surface (Table 1, page 44). Initial and moderate enamel carious lesions make up a significant portion of these criteria (categories 1 to 4). For these changes to be visible, tooth surfaces must be free of plaque and examined both wet and dry.
Until such time that an initial lesion is clinically (or radiographically) visible, clinicians must rely on the presence of caries risk factors, such as a carbohydrate-rich diet or lack of saliva, to indicate the risk of future caries development. However, because the risk indicator that is the best predictor of future caries is past caries experience (particularly in the last 12 to 24 months), identifying the presence of initial lesions is critical to accurate risk assessment.1,11 In the presence of cariogenic risk indicators, preventive interventions, such as topical fluorides and sealants, should be used to prevent lesion development or progression.1
As the caries process progresses, initial signs of the disease become identifiable when the surface is dried for a few seconds (ICDAS 1). These early lesions (initial, incipient or white spot lesions) can be seen more clearly when dried because they are more porous than sound enamel. When the enamel is dried, the water that fills the voids is replaced by air. Due to the difference in refractive indexes of air and water, the lesion is revealed as a white spot.12 If a tooth was examined under a microscope, these lesions would appear limited to the outer half of the enamel (Table 2, page 45).13
As the caries process continues, demineralization progresses through the entire thickness of the enamel, sometimes affecting the outer surface of the dentin (ICDAS 2).13 These changes are more distinct, making them visible even when the surface is wet or covered in saliva (Table 2). At this stage, the dentin-pulp complex responds by increasing the activity of odontoblasts, which deposit a tertiary dentin matrix (i.e., reactionary dentin). The underlying dentin may acquire a brown tint.
With further progression, the continuity of the enamel is compromised and microcavitations are formed (Table 2). However, nonsurgical treatment is still feasible.1 Once the dentin is exposed, pathogens can invade the dentin expeditiously and the lesion will spread along the dentinoenamel junction and destroy the mantle dentin, which, in turn, provides less support for the overlying enamel.14 When the enamel surface collapses, exposing the dentin (ICDAS 5 and 6), the cavitation fills with food debris, saliva and bacteria (Table 2).14 The bacteria then come in direct contact with the dentin, demineralize it, and expose the extracellular matrix, which is subsequently degraded by matrix metalloproteinases found in saliva and the dentin itself.15,16 At this stage, pulpal involvement is a significant concern.
ACTIVITY ASSESSMENT AND DIAGNOSIS
As noted, once a lesion has been detected, its activity status must be assessed. Visual-based caries activity assessment tools have been proposed, including the ICDAS activity criteria and Nyvad criteria.10,17 Clinical data suggest these visual activity assessment criteria are feasible and likely to help operators predict lesion activity.3,10,17
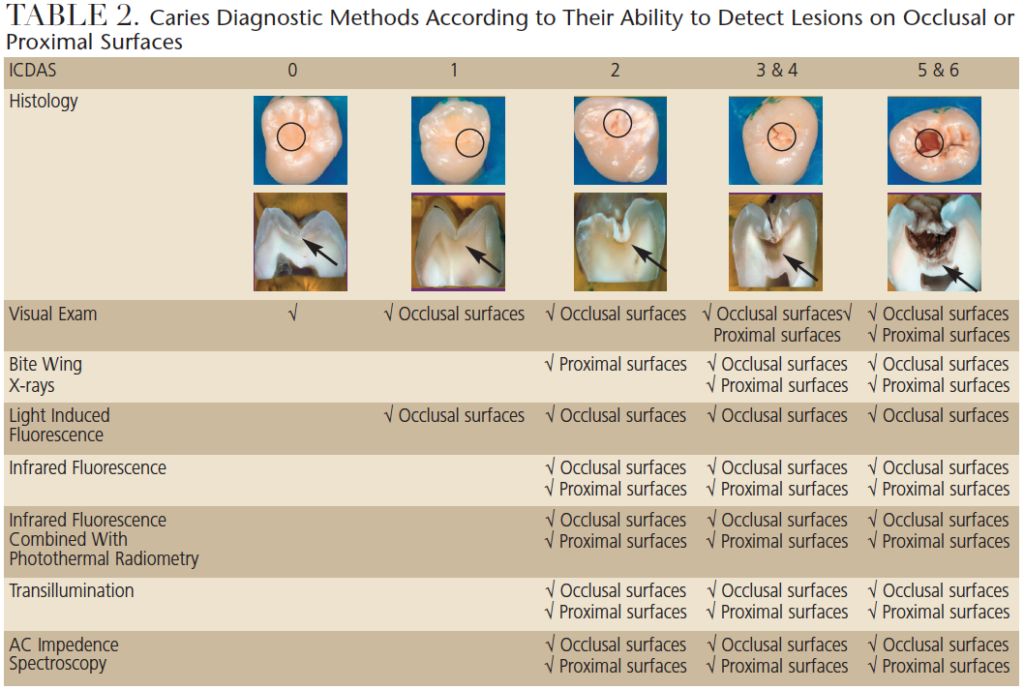
Both assessment systems are based on severity of the lesions and characteristics of the surface, such as color, location in plaque stagnation area, surface texture17 and hardness.10 Table 3 provides a correlation between severity status and characteristics of active/arrested lesions in enamel and dentin. Once lesion activity is assessed, the information is compiled with the caries risk assessment to achieve the best treatment decision.1
Diagnosis can be a subjective process. Under- or over-diagnosis both provide negative outcomes: the former resulting in additional tooth destruction,1 while the latter leads to unnecessary restorative treatment.18 However, caries progression is usually slow, and, in cases of uncertainty, delaying surgical intervention in favor of prevention is in the patient’s best interest.
Although visual examination alone is highly specific and helpful for determining if surfaces are sound, it lacks sensitivity, particularly in the early stages of lesions on proximal surfaces. Bitewing radiographs improve sensitivity for detection on proximal surfaces.19 Because the X-ray beam must pass through the entire tooth, it will only detect a caries lesion when at least one-third to one-half of the hard tissue is affected. Thus, only more advanced lesions (ICDAS 2 to 6 on proximal surfaces, and ICDAS 4 to 6 on occlusal surfaces) are detected via radiographs (Table 2).14 Early lesions do not provide enough contrast to be clearly visible on radiographs.20 Consequently, new technologies have been developed to aid in caries detection and diagnosis.4
NEW DETECTION TECHNOLOGIES
New methods of caries detection are especially suitable for diagnosing early to moderate-stage lesions (ICDAS 1 to 4). Table 2 illustrates the ability of each method to detect lesions on occlusal and proximal surfaces. Many of these new technologies work by measuring various optical characteristics of enamel that are affected by demineralization. Most use some form of light — from the blue green region to near-infrared region of the light spectrum. Some measure reflectance (the amount of light reflected by the tooth surface in relation to the amount of incidental light), while others measure a combination of luminescence (the level of glow) and heat generated after a laser is shined on a tooth. Additional tools measure differences in light transmission. Several technologies measure differences in fluorescence, which is a type of luminescence. One option uses electrical impedance to determine tooth health.
Varying degrees of evidence support the use of these technologies.3,4,21 The methods based on fluorescence in the blue range are highly sensitive and can detect most initial lesions — however, this sensitivity can lead to an increased rate of false positives.21 Combining this approach with a visual method might be a viable clinical alternative.22 Fluorescence in the infrared range has greater sensitivity for more severe lesions (ICDAS 2 to 4),23 but it is not as effective in diagnosing caries around restorations.24
While limited data show the tools that measure changes in reflectance from sound enamel to demineralized enamel can detect very early lesions (ICDAS 2 to 4), they may offer advantages that include minimal dilution of the light signal and insensitivity to the presence of bacteria.25
Analyses of luminescence (glow) and thermal behavior (heat) from the tooth are the basis of one technology. Some evidence indicates this system performs well in detecting enamel caries on occlusal surfaces and underneath sealants.26
Methods that use transmission of light through the tooth structures perform similarly to bitewing radiographs in detecting approximal and occlusal caries when the lesions extend into dentin (ICDAS 3 and 4).26 These methods place a light on one surface and observe the area from a different surface.
As noted, another method uses electrical impedance that examines electrical resistance or lack of resistance. It is able to detect lesions on approximal surfaces and occlusal surfaces,27 but limited data support the effectiveness of this device.28 Other technologies, such as optical coherence tomography, show promise, but are not yet commercially available.29
All of these devices can aid in diagnosing dental caries.4 They have the potential to improve the sensitivity of visual methods of detecting early lesions, and assist in the diagnosis of questionable surfaces.
TECHNOLOGICAL ADVANTAGES
Although no perfect caries detection device yet exists, adopting a technological approach has advantages. Because several technology-based detection devices have moved to a camera system, they are able to record images of the lesion over time. These can be analyzed, and the severity of the lesion quantified. This allows providers to monitor lesion progression and evaluate if it has been remineralizing, demineralizing or arrested. It is especially advantageous when dealing with early lesions that are difficult to quantity with visual criteria.
Furthermore, this approach offers the dentist another tool with which to assess whether a preventive treatment has been successful. This allows clinicians to adjust the treatment more rapidly, which could be beneficial because treatment is most effective when lesions are small or in their early stages.2
Showing patients quantitative data about caries lesions could help motivate them to improve their oral hygiene. These devices could therefore improve patient education and, ultimately, case acceptance.
Traditionally, interproximal lesions have been diagnosed with X-rays. Yet in certain situations, such as routine screenings, technology-based caries detection devices may reduce the need for radiography. While several studies have shown a correlation between diagnosis using technology-based devices or X-rays,30–32 radiographs offer additional information not provided by other caries detection devices, such as visualization of the pulp chamber or periapical region.
Ultimately, technology-based devices allow a less subjective detection and quantification of initial lesions. By monitoring lesion progression with these devices, the effectiveness of preventive measures can be assessed in shorter intervals, and modifications implemented as needed. There are disadvantages to a technology-based approach, too. Besides cost, all methods have a learning curve, and none will be equally effective on all surfaces and lesion severity stages. And while there is a recently approved American Dental Association CDT code (D0600) associated with use of these technologies, few, if any, insurance plans cover the costs.
CONCLUSION
As in other areas of practice, these new caries detection modalities should be viewed as additional clinical tools and not as replacements for sound professional judgment. In the best possible scenario, high-risk individuals would be identified before the caries process begins. At this time, however, none of the risk assessment tools offers sufficient accuracy to identify patients who will develop new lesions.33 Because the best predictor of disease is past caries history,1,11 early identification of initial caries lesions can be a valuable tool for management. All patients should benefit from primary preventive measures, including oral hygiene instruction, dietary advice, and recommendations to use fluoridated dentifrice twice per day.1 In addition, identifying lesions is a requisite for managing patients via secondary preventive measures (such as topical fluorides and sealants), rather than resorting to surgical intervention.
REFERENCES
- Zero DT, Zandona AF, Vail MM, Spolnik KJ. Dental caries and pulpal disease. Dent Clin North Am. 2011;55:29–46.
- Nyvad B. Diagnosis versus detection of caries. Caries Res. 2004;38:192–198.
- Braga MM, Ekstrand KR, Martignon S, Imparato JC, Ricketts DN, Mendes FM. Clinical performance of two visual scoring systems in detecting and assessing activity status of occlusal caries in primary teeth. Caries Res. 2010;44:300–308.
- Zandoná AF, Zero DT. Diagnostic tools for early caries detection. J Am Dent Assoc. 2006;137:1675–1684.
- Pitts NN. Modern concepts of caries measurement. J Dent Res. 2004;83(Spec No C):C43–C47.
- Nyvad B, Fejerskov O. Assessing the stage of caries lesion activity on the basis of clinical and microbiological examination. Community Dent Oral Epidemiol. 1997;25:69–75.
- Zero DT. Dental caries process. Dent Clin North Am. 1999;43:635–664.
- Ekstrand K, Zero D, Martignon S, Pitts N. Lesion activity assessment. In: Pitts N, ed. Detection, Assessment, Diagnosis and Monitoring of Caries. Basel, Switzerland: Karger; 2009:63–90.
- Ismail A, Sohn W, Tellez M, et al. The International Caries Detection and Assessment System (ICDAS): an integrated system for measuring dental caries. Community Dent Oral Epidemiol. 2007;35:170–178.
- Nyvad B, Machiulskiene V, Baelum V. Reliability of a new caries diagnostic system differentiating between active and inactive caries lesions. Caries Res. 1999;33:252–260.
- Disney JA, Graves RC, Stamm JW, et al. The University of North Carolina caries risk assessment study: further developments in caries risk prediction. Community Dent Oral Epidemiol. 1992;20:64–75.
- Kidd E, Fejerskov O. What constitutes dental caries? Histopathology of carious enamel and dentin related to the action of cariogenic biofilms. J Dent Res. 2004;83(Spec No C):35–38.
- Ekstrand KR, Ricketts DN, Kidd EA. Reproducibility and accuracy of three methods for assessment of demineralization depth of the occlusal surface: an in vitro examination. Caries Res. 1997;31:224–231.
- Ekstrand K, Ricketts D, Kidd E. Occlusal caries: pathology, diagnosis and logical management. Dental Update. 2001;28:380–387.
- Chaussain-Miller C, Fioretti F, Goldberg M, Menashi S. The role of matrix metalloproteinases (MMPs) in human caries. J Dent Res. 2006;85:22–32.
- Tjäderhane L, Larjava H, Sorsa T, Uitto VJ, Larmas M, Salo T. The activation and function of host matrix metalloproteinases in dentin matrix breakdown in caries lesions. J Dent Res. 1998;77:1622–1629.
- Ekstrand KR, Martignon S, Ricketts DJ, Qvist V. Detection and activity assessment of primary coronal caries lesions: a methodologic study. Oper Dent. 2007;32:225–235.
- Elderton RJ. Clinical studies concerning rerestoration of teeth. Adv Dent Res. 1990;4:4–9.
- Dove SB. Radiographic diagnosis of dental caries. J Dent Educ. 2001;65:985–990.
- Ko AC-T, Hewko M, Sowa MG, Dong CC,Cleghorn B, Choo-Smith LP. Early dental caries detection using a fibre-optic coupled polarization-resolved Raman spectroscopic system. Optics Express 2008;16:6274–6284.
- Pretty IA. Caries detection and diagnosis: novel technologies. J Dent. 2006;34:727–739.
- Zandona AF, Santiago E, Eckert G, Fontana M, Ando M, Zero DT. Use of ICDAS combined with quantitative light-induced fluorescence as a caries detection method. Caries Res. 2010;44:317–322.
- Costa AM, de Paula LM, Bezerra ACB. Use of Diagnodent for diagnosis of noncavitated occlusal dentin caries. J Appl Oral Sci. 2008;16:18–23.
- Bamzahim M, Aljehani A, Shi XQ. Clinical performance of Diagnodent in the detection of secondary carious lesions. Acta Odontol Scand. 2005;63:26–30.
- Amaechi BT. Emerging technologies for diagnosis of dental caries: the road so far. J Applied Phys. 2009;105:102047.
- Silvertown JD, Wong BP, Abrams SH, Sivagurunathan KS, Mathews SM, Amaechi BT. Comparison of The Canary System and Diagnodent for the in vitro detection of caries under opaque dental sealants. J Investig Clin Dent. 2017;8.
- Huysmans M-C, Longbottom C, Pitts NB, Los P, Bruce PG. Impedance spectroscopy of teeth with and without approximal caries lesions — an in vitro study. J Dent Res. 1996;75:1871–1878.
- Longbottom C, Hall A, Czajczynska-Waszkiewicz A, et al. Caries detection by optimal clinical visual, radiographic, laser fluorescence and AC-impedance spectroscopy techniques. Caries Res. 2007;41:297.
- Louie T, Lee C, Hsu D, et al. Clinical assessment of early tooth demineralization using polarization sensitive optical coherence tomography. Lasers Surg Med. 2010;42:898–905.
- Abogazalah N, Eckert GJ, Ando M. In vitro performance of near infrared light transillumination at 780-nm and digital radiography for detection of non-cavitated approximal caries. J Dent. 2017;63:44–50.
- Söchtig F, Hickel R, Kühnisch J. Caries detection and diagnostics with near-infrared light transillumination: clinical experiences. Quintessence Int. 2014;45:531–538.
- Marinova-Takorova M, Anastasova R, Panov VE, Yanakiev S. Comparative evaluation of the effectiveness of three methods for proximal caries diagnosis — a clinical study. J IMAB. 2014;20:514–516.
- Hausen H, Kärkkäinen S, Seppä L. Application of the high-risk strategy to control dental caries. Community Dent Oral Epidemiol. 2000;28:26–34.
The authors have no commercial conflicts of interest to disclose.
FEATURED IMAGE BY YOH4NN/E+/GETTY IMAGES PLUS
From Decisions in Dentistry. February 2018;4(2):43-46.




