 LUCIGERMA/ISTOCK/GETTY IMAGES PLUS
LUCIGERMA/ISTOCK/GETTY IMAGES PLUS
Oral Health Impacts of the COVID-19 Pandemic on Older Adults
Acknowledging the impact of the COVID-19 pandemic on general and mental health among vulnerable groups is key to providing effective oral healthcare.
This course was published in the April 2021 issue and expires April 2024. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the relationship between the COVID-19 pandemic and social isolation, loneliness and depression.
- Discuss the effects of social isolation, loneliness and depression on general and mental health.
- Explain oral health considerations for vulnerable groups related to the global pandemic.
Never have the issues of social isolation, loneliness and depression been brought to light more poignantly and dramatically than through the COVID-19 pandemic and its ongoing public health sequelae — especially among the most vulnerable groups in the United States.1 Older adults, particularly those in long-term care facilities, have been among the hardest hit, with devastating loss of life, as well as greatly diminished connections with family and friends, leading to further isolation and reduction in quality of life.2,3
Research on the effect of epidemics, especially the consequences of social distancing, is limited. Nevertheless, the impact on the mental health of the population as a whole and its most vulnerable communities can be estimated based on the information gleaned from other large-scale calamities.1,3 Traumatic, natural and environmental disasters lead to increases in depression, post-traumatic stress disorder, and substance use issues, occurring both in the immediate aftermath and long-term.3 Awareness of the pandemic’s impact on mental, behavioral and overall health — including oral health — and the negative outcomes on quality of life for the most at-risk populations will assist dental professionals in recognizing the interconnected aspects of health decline. In turn, this will support developing immediate and long-term approaches to providing oral healthcare and preventing further disease.
IMPACT ON GENERAL AND MENTAL HEALTH
Obviously, the most devastating negative outcome of SARS-CoV-2 infection is death. Older adults, a significant number of whom have chronic diseases and comorbidities, are at much greater risk than the general population, with more than 80% of related COVID-19 fatalities occurring in those age 65 and older.2 A comparison of U.S. fatalities among people younger than 54 (1%) and older populations demonstrates a stark increase in those between ages 65 and 84 (3% to 11%), and especially those age 85 and older (10% to 27%).2 In addition to comorbidities, such as diabetes, cardiovascular disease (CVD) and chronic kidney disease, one noteworthy risk factor for SARS-CoV-2 infection is a commonly prescribed group of medications for hypertension and CVD: angiotensin converting enzyme-2 inhibitors (ACEIs) and angiotensin receptor blockers.2 These medications upregulate the ACE-2 receptors located broadly in the body, including the heart, lungs and gastrointestinal system. The SARS-CoV-2 virus uses the ACE-2 receptors to attach to the cell surface and enter the cells in the lower respiratory tract. This places patients who take these medications at higher risk for COVID-19 infection and possibly a more severe course of disease.2
Other, more indirect effects of the pandemic on systemic health may include postponement or neglect of routine medical maintenance, and preventive or elective visits, such as blood screenings, eye exams, psychotherapy and dental care. In addition, a trend in refusal of more critical medical care, including organ transplants, joint replacement, cardiovascular procedures, and even cancer care, has occurred as hospitals, surgical centers and medical offices resume scheduling postponed procedures.4
In concert, data from the U.S. Centers for Disease Control and Prevention (CDC) indicate that, compared to the previous year, emergency department visits have dropped drastically, with a 42% decrease in U.S. visits over four weeks from March to April, 2020.5 At the start of the national quarantine, emergency department visits for exposure and symptoms associated with COVID-19 infection increased by fourfold, while presentation at emergency rooms across the nation for other symptoms, such as nonspecific chest pain and acute myocardial infarction, declined. Conversely, emergency department visits for cardiac arrest and ventricular fibrillation showed an increase compared to the previous year, suggesting delays in seeking care until symptoms were more severe and outcomes were more serious.5
Some of the concerns with less urgent, ambulatory care have been mitigated by the use of critical care strategies, telehealth services, and reopening of nonhospital medical and dental facilities. A new normal is evolving in which medical and dental practitioners must follow CDC infection control protocols to the highest level, but also continue to plan and perform procedures that could expose patients and staff to the risk of COVID-19 transmission.6,7 The lessons learned during the pandemic quarantine may be valuable in treating individuals with medical complexities, cognitive impairment and/or phobias.8 In this way, enhanced patient communication, including telehealth and video conferencing, allows oral health professionals to practice forms of behavioral cognitive therapy prior to treatment to address phobias and safety concerns. This is especially true since deferred treatment suggests more involved procedures may be indicated, and the reassurance provided may aid patient cooperation and compliance.8
SOCIAL ISOLATION AND LONELINESS
Social isolation necessitated by the COVID-19 pandemic may contribute to the increase of some systemic diseases, including CVD and metabolic syndrome.9 Among community-dwelling Americans age 65 and older, approximately 24% was considered to be socially isolated before the COVID-19 pandemic, and almost half of those age 60 and older reported feeling lonely.10 While these connections and their precise mechanisms are yet to be fully understood, the experiences of loneliness and social isolation can significantly impact older adults, increasing their risk for hypertension, CVD and stroke, as well as weight gain and decreased physical activity.11 The impacts may also impair attention, cognition and sleep, and result in increased alcohol/drug use and smoking.11
While often thought of interchangeably, the terms social isolation and loneliness are related, but quite distinct. Social isolation is an objective measure of the person’s lack of relationships and contact with others, while loneliness is a subjective negative experience of lack of meaningful, or any, relationships — even in the company of others. While social isolation can be imagined as a physical barrier, loneliness is the individual’s perception.9,10,12
As nearly one-third of older Americans reported experiencing social isolation before the pandemic-associated restrictions, vulnerable groups may be at an increased risk for neglect and abuse.13,14 Social distancing and increased reliance on caregivers for daily routines, including oral hygiene, may contribute to a “multidimensional state of vulnerability” already experienced by older adults due to high rates of anxiety and depression.14 As social isolation has been indicated as the strongest predictor of elder abuse, it may only intensify during the current pandemic.14 While it is estimated that one in 10 Americans older than 60 experience some form of elder abuse, only one in 14 cases is reported.15 As healthcare providers, dental professionals should note, evaluate and report suspected cases of elder abuse or neglect, even if not mandated by law.
DEPENDENCE ON CAREGIVERS
U.S. adults age 65 and older numbered approximately 50 million (15% of the population) in 2016, and this group is expected to exceed 80 million (> 20%) by 2050.16,17 As only 2 million to 3 million older adults currently reside in assisted living and nursing home facilities, most dependent adults need assistance with activities of daily living, relying predominantly on personal healthcare aides and/or informal caregivers, such as family members.17 More than 53 million (20%) of U.S. adults are unpaid caregivers.18
DEPRESSION AND ANXIETY
Depressive disorders affect approximately 15% to 23% of U.S. older adults living in the community, and up to 40% for elders in residential care. There is evidence of underdiagnosis and treatment in both categories.19,20 Depression in this population is expressed as either a medical comorbidity (minor depressive disorder) or a unique diagnosis (major depressive disorder). Strong associations exist between systemic disease and an increased medical burden and risk of death from suicide and CVD (most notably myocardial infarction) for older adults with depression.21
While it is not possible at present to evaluate the long-term mental health effects of COVID-19-related anxiety and depressive symptoms, the aspects of sustained and enhanced social isolation and perceived loneliness among older adults have a long history of interconnectedness with depression (even though they can be experienced independent of each other). Over time, research has shown the relationship between isolation and loneliness with clinical depression is at least reciprocal, if not directly causative.10 The extended separation of many older adults from the social connections in their communities and families underscores the need for outreach strategies, even before social and healthcare systems are fully operational. The American Psychological Association issued COVID-19 practice guidelines to assist in treating existing patients and those who will need care in the aftermath of the crisis.22
There is support for adding mental health services to Medicare-funded home healthcare, and this can encompass both screening for depressive disorders, as well as treatment.23 Mental health practitioners are being more innovative in light of waivers of some regulatory barriers, and the new model of triage and even treatment using telehealth emerges again as a rational approach moving forward. This model of care meshes perfectly with CDC recommendations prior to dental visits for prescreening for COVID-19 symptoms, triage and, perhaps most importantly, human-to-human communication and trust-building.7,8
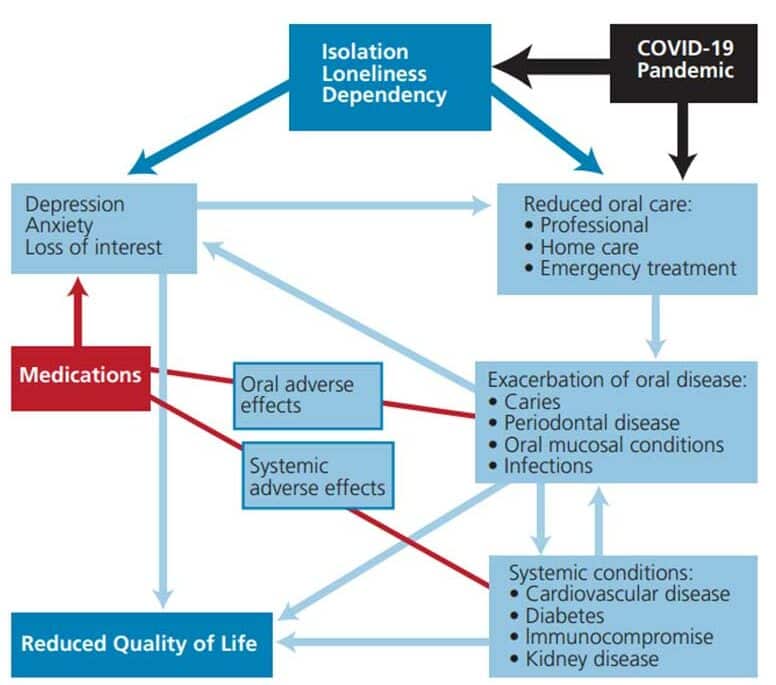
ORAL HEALTH CONSIDERATIONS
While isolation, loneliness and depression are associated with increased risk of systemic disease and mortality among elders, deleterious effects on oral health and oral health-related quality of life have also been found.24 Behavioral and biological factors play a role in oral disease among older adults, and reduced access to oral care, physical limitations, systemic disease, cognitive decline, and dependence on caregivers also contribute to its prevalence. Additionally, commonly prescribed medications in this population (especially polypharmacy) contribute to increased risk of oral disease.25
Research demonstrates an association between depressive disorders and caries, tooth loss and edentulism, and longitudinal studies show a correlation between periodontal disease and risk of depressive symptoms among elders.24 Poor oral health, including existing pain and dysfunction, reduces these patients’ quality of life. In addition, the need for assistance with oral self-care and other activities of daily living may lead to further disease and greater dependence on others.
MEDICATIONS AND ORAL HEALTH
More than 94% of adults age 65 and older use at least one prescription medication, with an average of 8.2 drugs for community-dwelling adults. This number increases to 12.7 medications in those newly admitted to nursing homes.25–27 An estimated one in four older adults take psychoactive medications, such as antidepressants, anxiolytics or sedative-hypnotics, which can have anticholinergic properties. Adverse effects include blurred vision, confusion, xerostomia or salivary gland hypofunction.25 A longitudinal study of medication exposure and salivary function revealed that almost two-thirds of participants were taking antihypertensive and other cardiac medications (predominantly diuretics, calcium channel blockers and ACEIs).27 Although this 11-year-long observation did not address the effect of polypharmacy on the incidence/prevalence and severity of xerostomia, it demonstrated a strong association of medication exposure with both prevalence and severity of the condition.27
Medication-induced salivary gland hypofunction is associated with dental caries, dysgeusia, oral mucosal soreness, and oral candidiasis; in addition, chronic xerostomia affects speech, digestion and enjoyment of food, denture wearing, and overall quality of life.27,28 A systematic review compiled a comprehensive list of medications with documented effects on salivary gland function and identified 56 medications with strong evidence of interference with salivary gland function. Of these, 36 belonged to the group of nervous system drugs that include analgesics, anti-Parkinson drugs, anxiolytics, sedatives/hypnotics and antidepressants.28 A careful review of all prescription and over-the-counter medications will help patients avoid possible adverse effects or dangerous drug interactions, which can be especially common in older adults due to polypharmacy and age-related physiological changes in drug metabolism.25,26
SARS-CoV-2-RELATED ORAL LESIONS
Dermatologic manifestations of SARS-CoV-2 infection have been widely reported. Several cases of oral-mucosal and oropharyngeal lesions (mostly in the form of herpetic-like ulcerations and erythema multiforme) affecting keratinized and nonkeratinized tissue have been documented.29 These lesions may be related to immune defense mechanisms, with etiologies in the SARS-CoV-2 infection and/or intense drug therapies, especially those that alter the oral microbiota.30 All lesions were self-limiting or resolved with the use of antimicrobial therapies. Self-reports of pain by these patients were associated with the lesions, suggesting oral manifestations may have been underdiagnosed. Consequently, intraoral examinations should be performed in suspected or confirmed SARS-CoV-2 cases.30
CONCLUSION
The direct effects of the COVID-19 crisis on the morbidity and mortality of vulnerable groups, including older adults — combined with the psychosocial impact of exacerbating existing systemic and oral health challenges — underline the need to address these concerns in a timely fashion. Older adults who have survived COVID-19’s adverse systemic effects and treatments may have lasting symptoms that require continued care.30 Additionally, postponed preventive and operative dental care should be resumed with caution and attention to patient concerns about the safety of treatment during the current pandemic.8
REFERENCES
- Torales J, O’Higgins M, Castaldelli-Maia JM, Ventriglio A. The outbreak of COVID-19 coronavirus and its impact on global mental health. Int J Soc Psychiatry. 2020;66:317–320.
- Shahid Z, Kalayanamitra R, McClafferty B, et al. COVID-19 and older adults: What we know. J Am Geriatr Soc. 2020;68:926–929.
- Galea S, Merchant RM, Lurie N. The mental health consequences of COVID-19 and physical distancing: The need for prevention and early intervention. JAMA Intern Med. 2020;180:817–818.
- Hafner K. Fear of COVID-19 leads other patients to decline critical treatment. The New York Times. May 25, 2020.
- Hartnett KP. Impact of the COVID-19 pandemic on emergency department visits — United States, January 1, 2019–May 30, 2020. MMWR Morb Mortal Wkly Rep. 2020;69.
- Chigurupati R, Panchal N, Henry AM, et al. Considerations for oral and maxillofacial surgeons in COVID-19 era: Can we sustain the solutions to keep our patients and healthcare personnel safe? J Oral Maxillofac Surg. 2020;78:1241–1256.
- U.S. Centers for Disease Control and Prevention. Interim Infection Prevention and Control Guidance for Dental Settings During the Coronavirus Disease 2019 (COVID-19) Pandemic. Available at: https://www.cdc.gov/coronavirus/2019-ncov/hcp/dental-settings.html. Accessed March 4, 2021.
- Dziedzic A. Special care dentistry and COVID-19 outbreak: What lesson should we learn? Dent J. 2020;8:46.
- Winterton A, Rødevand L, Westlye LT, Steen NE, Andreassen OA, Quintana DS. Associations of loneliness and social isolation with cardiovascular and metabolic health: a systematic review and meta-analysis protocol. Syst Rev. 2020;9:102.
- The National Academies of Sciences, Engineering, Medicine. Social Isolation and Loneliness in Older Adults: Opportunities for the Health Care System (2020). Available at: https://www.nap.edu/catalog/25663/social-isolation-and-loneliness-in-older-adults-opportunities-for-the. Accessed March 4, 2021.
- Berg-Weger M, Morley JE. Loneliness in old age: An unaddressed health problem. J Nutr Health Aging. 2020;24:243–245.
- Ong AD, Uchino BN, Wethington E. Loneliness and health in older adults: A mini-review and synthesis. Gerontology. 2016;62:443–449.
- Berg-Weger M, Morley JE. Editorial: loneliness and social isolation in older adults during the COVID-19 pandemic: Implications for gerontological social work. J Nutr Health Aging. 2020;24:456–458.
- Han SD, Mosqueda L. Elder abuse in the COVID‐19 era. J Am Geriatr Soc. 2020;68:1386–1387.
- National Council on Aging. What Is Elder Abuse? Available at: https://www.ncoa.org/public-policy-action/elder-justice/elder-abuse-facts/. Accessed March 4, 2021.
- Roberts AW, Ogunwole SU, Blakeslee L, Rabe MA. The Population 65 Years and Older in the United States: 2016. Available at: https://www.census.gov/content/dam/Census/library/publications/2018/acs/ACS-38.pdf. Accessed March 4, 2021.
- Aging & Health. Health Affairs. 2016;35:1556–1557.
- American Association of Retired Persons. Caregiving in the United States 2020. Available at: https://www.aarp.org/ppi/info-2020/caregiving-in-the-united-states.html. Accessed March 4, 2021.
- Xiang X, Danilovich MK, Tomasino KN, Jordan N. Depression prevalence and treatment among older home health services users in the United States. Arch Gerontol Geriatr. 2018;75:151–157.
- Levin CA, Wei W, Akincigil A, Lucas JA, Bilder S, Crystal S. Prevalence and treatment of diagnosed depression among elderly nursing home residents in Ohio. J Am Med Dir Assoc. 2007;8:585–594.
- Alexopoulos GS. Depression in the elderly. Lancet Lond Engl. 2005;365:1961–1970.
- Bojdani E, Rajagopalan A, Chen A, et al. COVID-19 pandemic: Impact on psychiatric care in the United States. Psychiatry Res. 2020;289:113069.
- Szanton SL, Leff B, Wolff JL, Roberts L, Gitlin LN. Home-based care program reduces disability and promotes aging in place. Health Aff (Millwood). 2016;35:1558–1563.
- Cademartori MG, Gastal MT, Nascimento GG, Demarco FF, Corrêa MB. Is depression associated with oral health outcomes in adults and elders? A systematic review and meta-analysis. Clin Oral Investig. 2018;22:2685–2702.
- Berryman SN, Jennings J, Ragsdale S, Lofton T, Huff DC, Rooker JS. Beers criteria for potentially inappropriate medication use in older adults. Medsurg Nurs. 2012;21:129–133.
- Skaar DD, O’Connor H. Potentially serious drug-drug interactions among community-dwelling older adult dental patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:153–160.
- Thomson WM, Chalmers JM, Spencer AJ, Slade GD, Carter KD. A longitudinal study of medication exposure and xerostomia among older people. Gerodontology. 2006;23:205–213.
- Wolff A, Joshi RK, Ekström J, et al. A guide to medications inducing salivary gland dysfunction, xerostomia, and subjective sialorrhea: a systematic review sponsored by the World Workshop on Oral Medicine VI. Drugs RD. 2017;17:1–28.
- Martín Carreras-Presas C, Amaro Sánchez J, López-Sánchez AF, Jané-Salas E, Somacarrera Pérez ML. Oral vesiculobullous lesions associated with SARS-CoV-2 infection. Oral Dis. 2020:10:1111.
- Dziedzic A, Wojtyczka R. The impact of coronavirus infectious disease 19 (COVID-19) on oral health. Oral Dis. 2020;10:1111.
From Decisions in Dentistry. April 2021;7(4):36–39.





The one question that needs to be asked and answered, wasn’t.
That question: What are the negative impacts of the face mask on dental health?
We’re forced into the masks 24/7. Virtually all of the elderly have been vaccinated and yet they’ve been scared to death so they’re told to keep the masks on. Fully vaccinated, yet with a mask.
So, please answer the question for all of us: What are the long term negative impacts of mask wearing on dental health?