 FLY VIEW PRODUCTIONS/E+/GETTY IMAGES PLUS
FLY VIEW PRODUCTIONS/E+/GETTY IMAGES PLUS
Nonspecific Oral Ulcerations in Infants
This case illustrates a nonspecific ulcer in an infant with a history of aerodigestive tract trauma, and the process of establishing a differential diagnosis.
This course was published in the January 2022 issue and expires January 2025. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Describe the presentations, potential etiology and treatment of nonspecific oral ulcerations in infants.
- Explain the effects these ulcers can have on infant development.
- Discuss clinical considerations when diagnosing these lesions.
Nonspecific oral ulceration occurring in the infant population often lead to consultations with medical and dental professionals. Although these conditions are not uncommon, there are very few reports in the dental literature regarding their etiology, clinical features and treatment. Thus, it is important for oral health providers to be able to recognize and diagnose the lesion or lesions based upon common clinical features. Collaboration between dentists, dental specialists, pediatricians and parents/caregivers helps in the early recognition of these ulcers, as well as when planning treatment that is most beneficial to the infant. Efficient resolution will allow minimal disruption in nutritional intake, and overall improved growth and development.
This paper presents a case report of a six-week-old infant with a nonspecific, unilateral ulceration of the palate, and the application of a differential diagnosis of Mikulicz minor aphthous ulcers (MMAU), Bednar’s ulcers (or pterygoid aphthae [BPA]), and necrotizing sialometaplasia-like changes (NSMLC).1 All three differential diagnoses have a self-limiting nature and complete resolution within two to 12 weeks without scarring.1–4 There is usually no recurrence or requirement for surgical biopsy if complete healing takes place within the accepted healing period.2
Distinct, shallow, round ulcers with a white or yellow pseudo-membrane and erythematous halo, MMAUs are usually found on nonkeratinized mucosa and heal within seven to 14 days.3 They are uncommon in children younger than age 4 and very rare in infants. Their etiology remains unconfirmed, but associated factors include a range of triggers, including underlying systemic disease (e.g., celiac disease or cyclic neutropenia), nutritional deficiencies (including iron, zinc and vitamin B), local trauma allergies, and genetics.2
First described in 1850 by Bednar,5 BPAs are reported as smooth, shallow ulcers, with a central region of white or grey ulceration and erythematous borders typically ranging from a few millimeters to 1 centimeter. They can be bilateral or unilateral and are confined to the posterior palate approximating the tonsillar region and pterygoid pillars. Reportedly occurring in 15% of infants, the ulcers are painful, but self-limiting, and total resolution is thought to occur within six weeks.6 The exact etiology remains unclear, but positive correlations have been made to trauma from increased sucking action of the infant and size of the nipple.7 Recent studies propose the location of these bilateral lesions near the lymphatic area may be an inductive site for stimulation of lymphocytes as an immune response in infants fed with formula.4,7,8
Acute necrotizing sialometaplasia (NSM) was first reported by Abrams et al9 in 1973, and is described as a benign, self-limiting inflammatory pattern of salivary ischemia and unilateral necrosis of the minor salivary gland lobules or acinary cells.10 Healing may be protracted, with reports ranging from four to 12 weeks.1,9–12 This condition is thought to be extremely rare in infants, with only one published case report of a 2-year-old developing this lesion three months after an adenoidectomy.13 The common causes of ischemia of the salivary gland tissues are infarction,2,13 medications,11 or physical trauma (e.g., intubation),12 and recent research points to the role of gastric acid secretion.1,10,14–18 Braxton et al1 describe this acid refluxate-induced pathology as NSM-like changes (i.e., NSMLC).
CASE REPORT
An eight-week-old infant was seen by a pediatrician after presenting with a chief complaint, expressed by the mother, of the presence of an ulcer on the maxillary left posterior palate. The mother stated the infant was having pain that limited milk intake. The ulcer had been present for approximately 10 days prior to the visit. The mother reported no trauma, vesicles or redness of the location prior to the appearance of the ulcer.
The patient’s history showed no associated pyrexia or reports of ulcers or rashes at other locations. No other clinical or systemic signs were noted, such as lymphadenopathy, at this visit. The infant was alert and responsive during the examination.
The medical history was positive for aerodigestive tract trauma and low birth weight (in the 2nd percentile for gestational birth weight). Aerodigestive problems are a group of conditions that affect the airway, swallowing, feeding and growth.19 The mother reported a pregnancy complication of intrauterine growth restriction, with a total gestation period of 37 weeks and caesarian section delivery. The infant was designated a premature status due to the low birth weight. A feeding and nutritional history revealed that, following birth, the infant had been breastfed, but supplemented with a nutritional-based formula from a bottle to address the low birth weight. Just prior to the appearance of the oral ulceration, breastfeeding was completely stopped, and milk intake was exclusively from bottle-feeding with the nutritional-based formula. Gastric reflux was experienced by the infant since birth and was observed to continue after being exclusively bottle-fed.
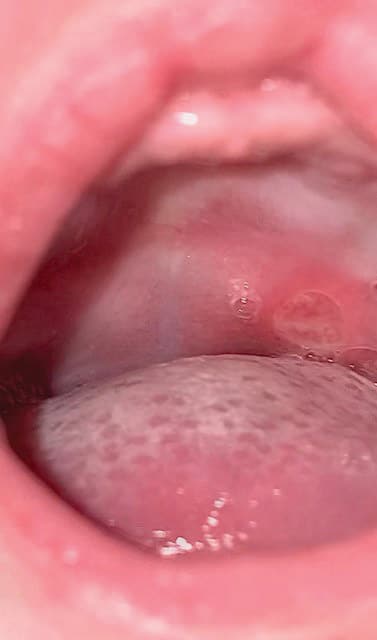
The mother reported there had been no change in the size or appearance of the ulcer since its initial presentation at the junction of the hard and soft palate. On visual examination, a single, round-to-oval ulcer approximately 1 centimeter in diameter was noted (Figure 1). The lesion had a white-to-gray colored center, with a diffuse, smooth erythematous bed. The pediatrician made a diagnosis of nonspecific oral ulceration. Viral, fungal or bacterial infections were not suspected, and blood or smear tests were not advised. Palliative management was discussed consisting of a change to a pro-sensitive formula (a specifically designed formula alternative for infants with gastrointestinal symptoms), and uprighting the feeding position to address the symptoms of gastric reflux — and possibly the ulceration. A low-birth infant can have a shorter and narrower esophagus, and the immature lower esophageal sphincter may relax and be displaced, allowing for milk to be pulled into the gastroesophageal junction, with reflux resulting. Supine feeding positions cause the reflux to worsen.20 The use of the analgesic acetaminophen was suggested to provide symptomatic relief from the pain so that feeding would improve.
PROVISIONAL DIAGNOSIS
The lesion had been present for more than three weeks from its initial presentation, with very little changes in its clinical appearance. The infant continued to have difficulty feeding, so the mother contacted Midwestern University School of Dental Medicine, Arizona. A provisional diagnosis was made by the authors from the clinical features of the presenting lesion. A referral to an oral surgeon for surgical biopsy and definitive diagnosis was provided as a treatment option. The mother’s preference was to monitor the lesion due to the self-limiting nature of the differentials presented, and to continue with the recommendations of the pediatrician with regard to feeding practices. Continued surveillance was recommended and immediate follow-up if symptoms or the appearance of the lesion worsened. This allowed for the most conservative of treatment approaches.
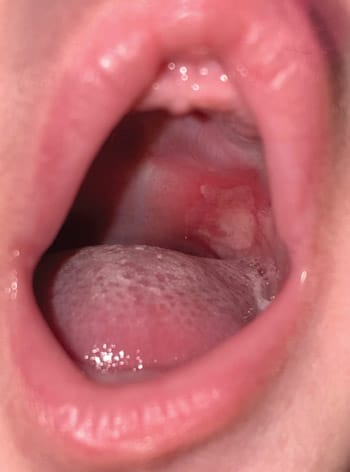
The continued presence of the lesion was reported by the mother on a weekly basis, with healing commencing at approximately five weeks (Figure 2). Acetaminophen had been discontinued due to concerns of constipation. Bottle-feeding continued with difficultly. Changes were made to feeding practices in accordance with pediatrician recommendations, including a change in the type of formula, an increased upright positioning of the infant during and after feeding, a change in both nipple and aperture size, and using a higher pH water for formula reconstitution. The infant also seemed to prefer a bottle with a vent system that removed air from the milk to aid digestion. Shortly after the implementation of the new practices, gastric reflux improved slowly and the area of ulceration also started healing, but resolution was relatively slow compared to literature reports for all the differentials considered.
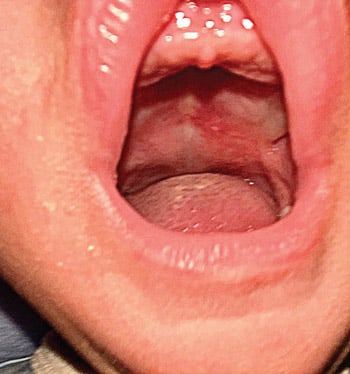
This may have been due to continued presence of gastric reflux, which may have acted as an irritant, preventing normal healing of the epithelial surface. Another possible cause could be the immature immune system of the premature infant. At nine weeks, an erythematous irritation of the palatal mucosa could still be visualized (Figure 3). At approximately 12 weeks after the initial observation, reflux was minimal and the ulceration was reported to have completely healed.
DISCUSSION
An ulcer has been defined as a breach in the continuity of the oral epithelium associated with molecular degeneration.8 Oral ulcerations can result from thermal, chemical or mechanical trauma. They can also arise from a multifactorial etiology,2 as described in this case. The three main differential diagnoses considered were based upon the clinical appearance of the ulcer, anatomical location, and local contributory factors, such as bottle-feeding with an inappropriately sized nipple and a more supine feeding position. Additional considerations in this case included the significant medical history of the infant’s aerodigestive tract trauma, gastric reflux and low birth weight, which could be associated with gastrointestinal tract and immunological immaturity.
Current literature indicates that systemic disease and nutritional deficiencies can be possible etiological causes for MMAU,3 while nutritional deficiencies — as well as immune responses to formula — have also been suggested in the development of BPA.6,8 In addition, NSMLC was considered in the differential diagnosis because of possible ischemic effects of the gastric reflux fluid, and due to the location of lesion in an area that has salivary gland tissue. The prolonged healing time of the ulcer was also consistent with NSMLC.1 Protracted infantile reflux can have serious complications of apnea, bradycardia, bronchopulmonary dysplasia lung aspiration, esophagitis, and failure to thrive. Infants with persistent reflux should receive additional medical care and observation.19 Low birth weight and premature infants, often fed a nutritional-based formula, are reported to have immunological mediated responses with continued use.6,7,21
It is important to recognize the etiology of oral ulcerations in infants and need to address underlying medical conditions that can have contributory effects.2 This knowledge of clinical features, causative factors, and known healing times can help in reaching a confident diagnosis, thus avoiding invasive and unwarranted medical or surgical investigations and interventions.
Establishing the correct diagnosis can also assist educational efforts for parents/caregivers concerning strategies to improve feeding practices. It will also help promote accelerated healing of the ulcer. Such targeted therapies include the use of correctly sized feeding bottle nipples, correctly sized nipple apertures, and using orthopedic nipples and pacifiers.8 These strategies will serve to decrease direct trauma from the bottle nipple and indirect trauma from the excessive sucking pressure. These changes decrease the risk of trauma to the already fragile infant mucosa.20 Altering the position of the infant from horizontal to a 45-degree upright position can be beneficial.19,20 The ultimate goal is to promote a more natural sucking motion of the tongue and musculature of the jaws,6 and decrease excessive sucking actions. A lactation specialist can often provide practical support and review for ankylosis, and offer recommendations for a multidisciplinary approach for parents/caregivers and treatment teams.
For clinicians treating this patient group, the literature has also suggested modalities aimed at pain relief and accelerated healing, such as the use of a coating agent (e.g., glycerin)6 and intra-lesional triamcinolone.2 Caution should be used with this approach to prevent potential overdose due to the low body weight of infants and inadvertent swallowing of these agents.
CONCLUSION
This case report illustrates an example of a nonspecific oral ulcerative lesion with atypical features of an aphthae in an age group in which such lesions are not commonly observed. The differential diagnosis was reached through comprehensive history taking, evaluating the clinical features of the presenting lesion, and utilizing previously reported literature. The most probable cause for the ulceration in the presented case was from trauma associated with either the size of the nipple, or the size of the nipple hole of the feeding bottle. The medical contributory effects from the aerodigestive trauma, gastric reflux, and possible immunologic reaction to nutritional formula point to MMAU, BPA and NSMLC as the differential diagnosis.
This case also highlights the importance of dental professionals, especially general dentists, as primary care dental providers in recognizing the clinical features of such lesions in infants. General dentists are usually the main resource when families and other care providers — such as pediatricians, lactation specialists and nurse practitioners — have questions about oral conditions. It is relevant for both dental and medical professionals to understand the relationship between infant feeding practices and oral ulcerations, and to emphasize the value of collaboration between various healthcare disciplines to provide parents/caregivers with reassurance and conservative therapeutic measures. Educating parents/caregivers about the self-limiting nature of these lesions can reduce anxiety and prevent unnecessary investigations and surgical intervention.
Acknowledgement: This case report was approved by the Midwestern University Office of Research and Sponsored Programs Institutional Review Board AZCS-150. We wish to thank Ruzanna Balyan, DMD.
References
- Braxton DR, Nickleach DC, Liu Y, Farris AB 3rd. Necrotizing sialometaplasia-like change of the esophageal submucosal glands is associated with Barrett’s esophagus. Virchows Arch. 2014;465:135–143.
- Legeret C, Furlano R. Oral ulcers in children — a clinical narrative overview. Ital J Pediatr. 2021;47:144.
- Messadi DV, Younai F. Aphthous ulcers. Dermatol Ther. 2010;23:281–290.
- Nebgen S, Kasper HU, Schafer D, Christ H, Roth B. Bednar’s aphthae in neonates: incidence and associated factors. Neonatology. 2010;98:208–211.
- Madurapperuma SW, Jayaweera A, Jayasinghe RD. Spontaneously regressing neonatal oral aphthous ulceration of the palate. Case Rep Pediatr. 2021;2021:6660302.
- Chaudhry A, Saluja P. Nostalgia of neonatal Bednar’s aphthae. J Clin Neonatol. 2019;8:1–4.
- Tricarico A, Molteni G, Mattioli F, et al. Nipple trauma in infants? Bednar aphthae. Am J Otolaryng. 2012;33:756–757.
- Chaudhry A. Infantile Bednar’s aphthae. J Paediatr Child Health. 2021;57:1720.
- Abrams AM, Melrose RJ, Howell FV. Necrotizing sialometaplasia. A disease simulating malignancy. Cancer. 1973;32:130–135.
- Carlson DL. Necrotizing sialometaplasia: a practical approach to the diagnosis. Arch Pathol Lab Med. 2009;133:692–698.
- Gatti A, Broccardo E, Poglio G, Benech A. Necrotizing sialometaplasia of the hard palate in a patient treated with topical nonsteroidal anti-inflammatory drug. Case Rep Dent. 2016;2016:9545861.
- Fernandes PM, Pedroso EG, Santos-Silva AR, Vargas PA, Lopes MA. Non-ulcerated necrotizing sialometaplasia may mimic a salivary gland tumor. Autops Case Rep. 2021;11:e2021244.
- Ylikontiola L, Siponen M, Salo T, Sandor GK. Sialometaplasia of the soft palate in a 2-year-old girl. J Can Dent Assoc. 2007;73:333–336.
- Solomon LW, Merzianu M, Sullivan M, Rigual NR. Necrotizing sialometaplasia associated with bulimia: case report and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103:e39–e42.
- Salvado F, Nobre MA, Gomes J, Maia P. Necrotizing sialometaplasia and bulimia: A case report. Medicina (Kaunas). 2020;56:188.
- Rushinek H, Keshet N, Maly A, Aframian DJ. Necrotizing sialometaplasia related to vomiting and silastic ring vertical gastroplasty. Quintessence Int. 2016;47:147–150.
- Scully C, Eveson J. Sialosis and necrotising sialometaplasia in bulimia; a case report. Int J Oral Maxillofac Surg. 2004;33:808–810.
- Lombardi T, Samson J, Kuffer R. Subacute necrotizing sialadenitis: a form of necrotizing sialometaplasia? Arch Otolaryngol Head Neck Surg. 2003;129:972–975.
- Ringley T. Reflux in preemies: a very common condition in premature babies. Available at: https://www.verywellhealth.com/reflux-in-preemies-2748637. Accessed November 30, 2021.
- Bird C. Formula feeding your preemie. Available at: https://www.verywellfamily.com/how-long-should-my-baby-use-preemie-formula-2748587. Accessed November 30, 2021.
- Nam SW, Ahn SH, Shin SM, Jeong G. Clinical features of Bednar’s aphthae in infants. Korean J Pediatr. 2016;59:30–34.
From Decisions in Dentistry. January 2022;8(1):40-43.




