
Leverage Health Literacy for Better Outcomes
Assessing patients’ ability to process basic health information can help improve compliance with treatment recommendations.
PURCHASE COURSE
This course was published in the June 2017 issue and expires June 2020. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
OBJECTIVES
After reading this course, the participant should be able to:
- Define oral health literacy.
- Describe the health implications and financial impact of low oral health literacy.
- Discuss methods for assessing oral health literacy.
- Identify strategies to effectively communicate with patients who have low oral health literacy.
Determining the myriad factors that influence a patients’ systemic and oral health is no simple task. One of the factors that is increasingly linked to health care outcomes, health literacy is defined as “the degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions.”1 According to most recent national assessment of health literacy, more than one third of U.S. adults (36%) do not have the basic skills to effectively manage their health and navigate the health care system.1 In addition, individuals who have difficulty navigating the system often delay care until their disease is advanced and may opt to visit the emergency department. The cost resulting from low health literacy is estimated at $75 billion.2
In terms of dental practice, oral health literacy comprises:
Knowledge About a Specific Disease — As one example, patients, as well as medical professionals, are often unaware that dental caries is both infectious and preventable.
Interpreting Risks and Benefits of Recommended Treatment — Dental materials are frequently written at an advanced reading level. Many patients may find interpreting the proportions or ratios required to adequately understand treatment risks difficult.
Performing a Specific Task — Functional oral health literacy refers to the ability to carry out a skill, such as making dental appointments, following through with a referral for specialty care, or improving self-care technique.
Cultural Background, Societal Influences, and Familiarity with the Health Care System — Culture strongly influences how individuals think and feel about oral health. In many developing countries, for example, preventive care is rare, and seeking dental services for reasons besides acute pain is uncommon.3 Immigrants often retain similar care-seeking practices upon relocating to the United States, and these practices may be passed down to subsequent generations.
Daily demands of living, lack of insurance and difficulty locating an appropriate oral health provider are additional barriers to care. The complexity of the information presented — in addition to dental anxiety — may also impact an individual’s ability to comprehend and communicate preferences to providers.4,5
Studies show that low oral health literacy is more common among adults with less than a high school education, older adults, immigrants and refugees, racial and ethnic minorities, and low-income individuals.6–8 Although it has not been studied as extensively as health literacy, oral health literacy may be a better predictor of poor oral health outcomes than any other demographic factor.9
Compared to more knowledgeable patients, for example, individuals with low oral health literacy are less likely to exhibit oral health-related behaviors — including daily toothbrushing and flossing, seeking preventive and restorative dental care, and eating a low-cariogenic diet.10–13 Poor oral health outcomes include more severe periodontal disease, advanced caries, tooth loss and reduced quality of life.4,12,14
ASSESSING ORAL HEALTH LITERACY
Approximately 20 surveys measure oral health literacy,15 yet some are more appropriate for use in research settings than clinical practice. The Test of Functional Health Literacy in Dentistry is appropriate for use in the clinical setting. Patients read a toothpaste label and answer questions that reflect reading ability, comprehension and numeracy.16 Another assessment method used in patient care consists of four questions that can be administered independently or added to a health history. These focus on patients’ confidence in the ability to complete medical forms and read medication labels, as well as difficulties they may have learning about health topics due to limited reading comprehension.17 While most assessments are helpful in measuring reading and numeracy skills, they may be of limited use when measuring how well patients navigate the health care system or make health care decisions. Researchers continue to develop oral health literacy instruments that can be used in clinical practice. Considering that a standard tool or index has not been widely accepted for routine practice, alternative strategies — such as conducting informal individual assessments — may be more practical for clinical use.
An informal method to assess oral health literacy is to observe patients as they fill out forms. Patients who take a long time to read and sign consent forms, look confused, make excuses (such as “I forgot my glasses”), or ask for assistance may have trouble reading.18 In a recent study, oral health professionals reported asking unscripted, open-ended questions to assess oral health literacy. Through conversation, these clinicians gained a sense of patients’ oral health knowledge and interest in improving their oral health.19
Researchers have found that if clinicians ask patients to explain exactly what they understand about their conditions and instructions, they will find many gaps in knowledge, difficulties in understanding and misinterpretation.4 Due to the difficulty in assessing every patient seen in a clinical setting, using an approach similar to the universal precautions for infection control can be effective.20 The assumption that every patient may need some level of assistance to understand oral health information can help clinicians approach each patient at an appropriate level. This methodology does not assume the health literacy of individual patients; rather, it creates an environment in which patients may feel more comfortable asking questions.20 The clinical encounter may routinely include a conversational assessment to determine the patient’s educational level, readiness to learn and learning preferences, and any cultural, developmental or religious factors that might affect oral health literacy and health care decisions.4 Based on these findings, the communication can be steered to meet the requirements of evidence-based dentistry, where the most current treatments intersect with the patient’s preferences and the clinician’s expertise.21
INTERVENTIONS TO IMPROVE OUTCOMES
The extent and complexity of the oral health literacy issue requires a comprehensive solution. Toward this end, the American Dental Association has proposed three areas of intervention to improve patient oral health literacy — and, thus, oral health outcomes.22 The three areas of intervention are at the broad levels of culture and society, the educational system and health care system (Figure 1).22 While dental professionals can implement change in these areas, this article focuses on addressing oral health literacy within health care settings.
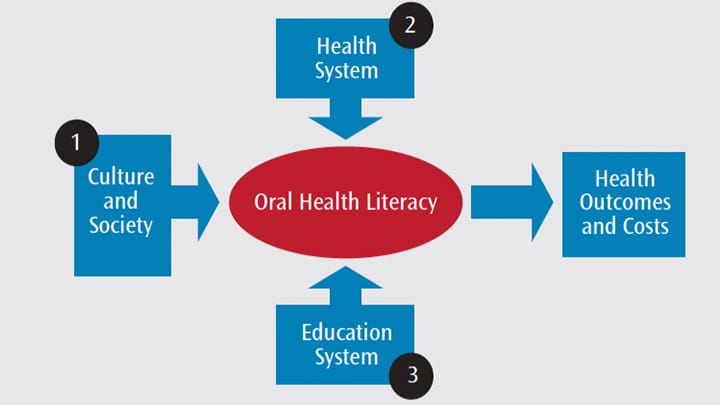
With the goal of improving patients’ understanding, health care teams can make it easier for individuals to access and understand health information. Examples include designing websites that are easy to navigate, presenting information in plain, simple terms, and providing an interactive map that can help patients find the practice. In the dental office, directional signage using pictograms aids patients with limited reading ability. Staff can review forms and written materials to ensure they are at the sixth-grade reading level. Reception areas should be welcoming and all staff members should be friendly.9,23
Oral health professionals play a significant role in bridging the gap between what is scientifically known about oral health and what patients actually understand.24 For example, a patient-provider conversation may help the patient identify a therapy or adapt behavior change that improves oral health. Communication can also have a less direct impact on patient health. If communication results in a feeling of validation, reduces fear or anxiety, improves understanding or provides social support, the patient may be more apt to comply with provider recommendations. Conversely, engaging in controlling communication laced with disagreement and directives may lead to poor compliance with directions.25 Dental professionals should bear in mind that individuals may have skills, but choose not to use them in certain settings.26 In other words, a motivated patient with low oral health literacy may be more receptive to improving his or her oral health behavior than a more informed patient who doesn’t value oral health.
MOTIVATIONAL INTERVIEWING
Understanding patients’ levels of motivation and communicating this are at the core of moving patients toward behavior change to improve oral health. Communication strategies that include the patient as an active participant (rather than the recipient of information) can help ensure that patients understand recommendations. Motivational interviewing (MI), which incorporates learning and building on patient priorities, is an effective tool to facilitate behavioral changes.27 Using MI to establish a patient’s level of engagement and priorities for care can help clinicians determine the most effective communication strategies. By asking open-ended questions about the individual’s attitudes toward oral health, barriers to making a change in self-care, and perceived benefits of making a change, clinicians can leverage these attitudes and priorities to meet the patient’s oral health goals. An open-ended question is one in which a detailed response is required (rather than a simple “yes” or “no” answer). For example, clinicians may ask, “Can you tell me about your self-care oral hygiene routine?” or “How important is it for you to keep your teeth?”
The stages of change (or transtheoretical) model is the foundation of MI and provides a framework for determining patients’ readiness for change. Individuals who have no desire or intention to make a behavioral change are in the precontemplation stage. Those thinking about making a change in the future are in the contemplation stage. Patients getting ready to make a change are in the preparation stage (meaning, they are willing to invest the time and effort to embrace new knowledge and skills). Individuals who are in the process of making a change are in the action stage; that is, they have exhibited behavior change or initiated the new skill. The maintenance stage occurs after the patient has accomplished the behavior change.28 Studies show that this approach is more effective than standard health education.29
After establishing rapport and using MI to determine if the patient is willing to participate in a discussion about oral health (i.e., the contemplation or preparation phase), specific communication strategies are recommended for use with patients exhibiting low oral health literacy. Each strategy may be used alone or in combination (Table 1).20
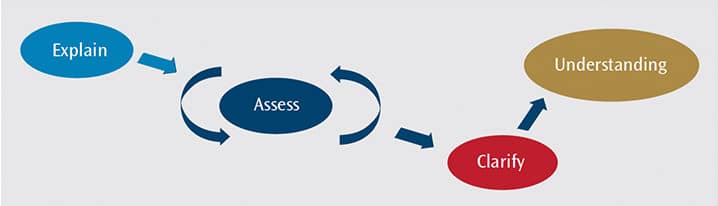
The most effective and adaptable strategy is called “teach-back” and confirms understanding by asking patients to explain information provided by clinicians (Figure 2). For example, after presenting a recommendation for a restoration, a dentist might say, “I want to make sure that I explained this correctly. Please tell me in your own words how you understand the treatment plan.” If a misunderstanding exists, the oral health professional can clarify the explanation. Ensuring both understanding and agreement about the care plan is essential to achieving patient compliance.22 Perhaps most importantly, clinicians have reported that teach-back doesn’t take more time out of their day than other forms of communication and is worth the effort when speaking with patients.30
A study of health literacy interventions reported additional strategies as being effective with low health literacy patients.31 These include presenting the most essential information first (or by itself) and adding video content to verbal descriptions. Literature and other materials should include simplified text written at the sixth-grade reading level. Numerical information is more effective if icons or pictograms are added to number displays.31
USE PLAIN LANGUAGE
The use of plain language is recommended. Traditionally, this was referred to as using “layman’s terms” and, more recently, “simple language.” Communicating in basic terms and breaking complex ideas into smaller pieces makes information easier to understand.4 Examples include using “cavities” for caries, “sticky film with germs” for biofilm, and “hard, crusty deposits” to describe calculus.
A clinician’s demeanor is also important. Studies in which practitioners provided clear explanations, appeared compassionate, and involved patients in decision-making correlated with lower blood pressure and reduced anxiety in patients.32 By comparison, clinicians who used a superior tone or talked down to patients appeared judgmental and negatively affected outcomes.31,33
Sharing information about resources available in the surrounding area is also helpful for patients with low oral health literacy. Keeping up to date on community resources in order to refer patients to additional services — such as transportation options and other health care or social service professionals — can support patients with low oral health literacy.
Appointments should conclude with an invitation for patients to ask questions. Rather than posing a “yes” or “no” question, an open-ended query — such as, “What questions do you have for me?” — is likely to provide useful information. Clinicians should determine whether a follow-up call or text might be helpful, and ask permission to check in at certain intervals. Research shows that a stronger patient-provider relationship is forged when patients feel their providers care about them.25,34
CONCLUSION
In summary, a large proportion of patients demonstrates low oral health literacy and struggles to make health care decisions. Clinicians who are armed with tools, such as MI, are well positioned to assist patients in improving their oral health. Determining whether patients are prepared to listen, learn and change behavior to enhance oral health is clinically important. Using assessment and communication strategies geared toward improving patients’ oral health literacy will not only encourage compliance with treatment recommendations, it also helps improve outcomes.
REFERENCES
- Kutner M, Greenberg E, Jin Y, Paulson C. The Health Literacy of America’s Adults: Results From the 2003 National Assessment of Adult Literacy. Washington, DC: U.S. Department of Education; 2006.
- Institute of Medicine Committee on Health Literacy. Health Literacy: A Prescription to End Confusion. Washington, DC: National Academies Press; 2004.
- Vered Y, Zini A, Livny A, Mann J, Sgan-Cohen HD. Changing dental caries and periodontal disease patterns among a cohort of Ethiopian immigrants to Israel: 1999–2005. BMC Public Health. 2008;8:345.
- New York State Department of Health, Oral Health Division. Oral Health Literacy Toolkit: 2015. Available at: static1.squarespace.com/ static/ 53bc58e3e4b060a 82ab7359d/ t/552d2c18e4b057e7ac6e3e3e/ 1429023768340/ Oral+ Health+ Literacy+Toolkit.pdf. Accessed May 8, 2017.
- Allison P, Locker D, Jokovic A, Slade G. A cross-cultural study of oral health values. J Dent Res. 1999;78:643–649.
- Jones M, Lee JY, Rozier RG, Bender D, Ruiz RE. Oral health literacy among adult patients seeking care. J Am Dent Assoc. 2007;138:1199–1208.
- McQuistan M, Qasim A, Shao C, Straub-Morarend C, Macek M. Oral health knowledge among elderly patients. J Am Dent Assoc. 2015;146:17–26.
- Maserejian NN, Trachtenberg F, Hayes C, Tavares M. Oral health disparities in children of immigrants: dental caries experience at enrollment and during follow-up in the New England Children’s Amalgam Trial. J Public Health Dent. 2008;68:14–21.
- Podschun G. National plan to improve health literacy in dentistry. J Calif Dent Assoc. 2012;40:317–320.
- Divaris K, Lee JY, Baker AD, Vann WF. Caregivers’ oral health literacy and their young children’s oral health-related quality-of-life. Acta Odontol Scand. 2012;70:390–397.
- Lee JY, Divaris K, DeWalt DA, et al. Caregivers’ health literacy and gaps in children’s Medicaid enrollment: findings from the Carolina Oral Health Literacy Study. PloS One. 2014;9:e110178.
- Miller E, Lee JY, DeWalt DA, Vann WF Jr. Impact of caregiver literacy on children’s oral health outcomes. Pediatrics. 2010;126:107–114.
- Vann WF Jr, Divaris K, Gizlice Z, Baker AD, Lee JY. Caregivers’ health literacy and their young children’s oral-health-related expenditures. J Dent Res. 2013;92:55S–62S.
- Naik A, John MT, Kohli N, Self KD, Flynn P. Validation of the English language version of the OHIP-5. J Prosthodont Res. 2016;60:85–91.
- Dickson-Swift V, Kenny A, Farmer J, Larkins S. Measuring oral health literacy: a scoping review of existing tools. BMC Oral Health. 2014;14:148.
- Gong DA, Lee JY, Rozier RG, Pahel BT, Richman JA, Vann WF, Jr. Development and testing of the Test of Functional Health Literacy in Dentistry (TOFHLiD). J Public Health Dent. 2007;67:105–112.
- Chew L, Bradley K, Boyko E. Brief questions to identify patients with inadequate health literacy. Family Med. 2004;36:588–594.
- National Institute of Dental and Craniofacial Research.The invisible barrier: literacy and its relationship with oral health. J Public Health Dent. 2005;65:174–182.
- Flynn P, VanWormer J, Schwei K, Skrzypcak K, Acharya A. Assessing dental hygienists’ communication techniques with low oral health literacy patients. J Dent Hyg. 2016;90:162–169.
- DeWalt D, Callahan L, Hawk V, et al. Health Literacy Universal Precautions Toolkit. Rockville, Maryland: The Cecil G. Sheps Center for Health Services Research, The University of North Carolina at Chapel Hill, April 2010. Report No: AHRQ Publication No. 10-0046-EF.
- Frantsve-Hawley J, Clarkson J, Slot D. Using the best evidence to enhance dental hygiene decision making. J Dent Hyg. 2015;89:35–38.
- American Dental Association Council on Access Prevention and Interprofessional Relations. Health Literacy in Dentistry Action Plan, 2010–2015. Chicago: American Dental Association; 2009.
- Horowitz AM, Kleinman DV. Creating a health literacy-based practice. J Calif Dent Assoc. 2012;40:341–350.
- Horowitz AM, Clovis JC, Wang MQ, Kleinman DV. Use of recommended communication techniques by Maryland dental hygienists. J Dent Hyg. 2013;87:212–223.
- Street RI, O’Mallley KJ, Cooper LA, Haidet P. Understanding concordance in patient-physician relationships: personal and ethnic dimensions of shared identity. Ann Fam Med. 2008;6:198–205.
- Pleasant A. Advancing health literacy measurement: a pathway to better health and health system performance. J Health Commun. 2014;19:1481–1496.
- Rollnick S, Miller W, Butler C. Motivational Interviewing in Health Care: Helping Patients Change Behavior. New York: Guilford Press; 2007.
- Norcross JC, Krebs PM, Prochaska JO. Stages of change. J Clin Psychol. 2011;67:143–154.
- Stewart J, Wolfe G, Maeder L, Hartz G. Changes in dental knowledge and self-efficacy scores following interventions to change oral hygiene behavior. Patient Educ Couns. 1996;27:269–277.
- DeWalt DA, Broucksou KA, Hawk V, et al. Developing and testing the health literacy universal precautions toolkit. Nurs Outlook. 2011;59:85–94.
- Sheridan SL, Halpern DJ, Viera AJ, Berkman ND, Donahue KE, Crotty K. Interventions for individuals with low health literacy: a systematic review. J Health Commun. 2011;16(Suppl 3):30–54.
- Street R, Makoul G, Arora N, Epstein R. How does communication heal? Pathways linking clinician-patient communication to health outcomes. Patient Educ Couns. 2009;74:295–301.
- Samuels-Kalow M, Hardy E, Rhodes K, Mollen C. “Like a dialogue:” teach-back in the emergency department. Patient Educ Couns. 2016;99:549–554.
- Waldenstrom U. Continuity of carer and satisfaction. Midwifery. 1998;14:207–213.
Featured Image by MONKEYBUSINESSIMAGES/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. June 2017;3(6):36,39—41.





