Implant Rehabilitation in a Patient With Recurrent Ossifying Fibroma
This case report demonstrates the multidisciplinary approach required to restore esthetics, function, and psychological well-being in a patient with partial edentulism following surgical treatment for recurrent ossifying fibroma.
This course was published in the July/August 2025 issue and expires August 2028. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
AGD Subject Code: 730
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the biological behavior and clinical management of ossifying fibroma.
- Recognize the psychological and functional implications of partial edentulism and the restorative benefits of dental implant therapy.
- Discuss the importance of interdisciplinary coordination in achieving optimal esthetic and functional outcomes in complex implant cases.
Ossifying fibromas are benign but locally aggressive bone tumors that commonly manifest in the jawbones. These lesions are characterized by the replacement of normal bone with fibrous tissue and varying amounts of calcified material.1 Patients with ossifying fibromas often experience swelling, pain, and potential displacement of teeth. As the fibroma grows, it compromises the structural integrity of the jaw, necessitating the removal of adjacent teeth to prevent further damage, while alleviating symptoms.2 Despite being benign, these tumors have a high recurrence rate, which requires ongoing checkups at regular dental visits, and imaging studies to detect and manage any recurrence.
Partial edentulism refers to a condition in which individuals have lost some, but not all of their teeth. The absence of teeth has been linked to negative feelings regarding appearance, compromised function of the mouth, and impaired psychological health.3 The most important determining factor influencing psychological well-being is self-esteem.4 A United Kingdom study conducted assessed the effects of esthetic dental treatment on oral health-related quality of life (OHRQoL). Abu-Awwad et al5 found that adults with hypodontia or those missing one or more teeth reported higher OHRQoL after completing dental treatment.
As patients age, they may become more aware of esthetics, motivating them to seek dental treatment.6 The continuous improvement of dental implant technology has provided a transformative solution for patients experiencing tooth loss. Dental implants serve as a robust and long-lasting replacement for natural teeth, offering both functional and esthetic advantages.7 The use of implants helps restore chewing efficiency and speech, significantly enhancing the patient’s quality of life. Moreover, a mouth with full dentition can greatly improve a patient’s self-confidence and social interactions. This advancement not only aids in the physical rehabilitation of the oral cavity but also contributes to the emotional well-being of patients.
Case Report
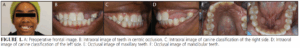
A 25-year-old nonbinary patient presented to the dental clinic in excellent health, with a chief complaint of missing teeth in the left maxillary region. (Figure 1A-F). The patient was previously diagnosed with an ossifying fibroma affecting teeth #10-12, and lost these three teeth. Following the extractions, a recurrence of the tumor required two additional alveoloplasties.
A bone graft was previously performed to optimize future prosthetic intervention. The patient disclosed a persistent numbness in the left maxillary region since the extractions. Extraoral and intraoral examination revealed sufficient interocclusal space between the vertical dimension of rest and occlusion, however, concerns lingered regarding potential anterior crossbite issues upon the delivery of the final restoration in this region.
The patient initially reported they did not want to undergo orthodontic treatment. A complete full-mouth series of periapical and bite-wing radiographs were taken. The patient had generalized moderate plaque-induced gingivitis and adequate volume of healthy bone. The patient expressed the desire for a fixed prosthesis, and they underwent an implant consultation (Figure 2). The recommendation was for implant placement at sites #11 and #12 with a delayed loading protocol. Specifically, site #11 would be designed with a cantilever of site #10. Tooth #12 would receive a single implant crown.
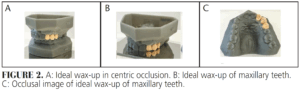
A diagnostic wax-up was crafted to delineate the occlusion based on the existing arch form. Following its completion, a prosthodontist, orthodontist, orthodontic resident, and dental student met to discuss the case. Together, they devised a strategic plan for implant placement, addressing the likelihood of the patient’s anterior crossbite. Following the collaborative meeting a revised wax-up (Figure 2A-C) was constructed to envision ideal contours of the final restorations while also outlining the optimal arch form. The efforts were to communicate tooth movement required in the opposing arch to the orthodontic department.
The International Team for Implantology’s Straightforward, Advanced, Complex (SAC) classification was performed to assess the risk and complexity of the case. The surgical and prosthodontic complexity were classified as medium. Prosthodontically, the factors contributing to the complexity were the width of the edentulous span, spanning across three units, and the gingival display at full smile. Surgically, risk factors arose from the number of implants placed in the edentulous span. Implants were then placed, and orthodontic tooth movement commenced, while allowing for the osseointegration of the implants into the maxilla. Before restoring the implants, osseointegration would be done 3 months after placement.8
The patient presented to the orthodontics clinic for an initial examination with a chief complaint of wanting to align their lower anterior dentition to provide clearance for their upper implant crowns. The patient had a Class I skeletal and hyperdivergent relationship, severe maxillary spacing (18.0 mm), mild mandibular crowding (-1.1 mm), 3.3 mm overjet, 2.4 mm overbite, and a level curve of Spee. The lower arch presented with a square-shaped arch form with a lower mandibular midline deviation 0.5 mm to the left.
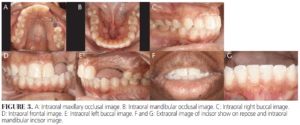
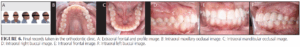
The patient exhibited an Angle’s Class I molar and canine classification on the right with Class I molar relationship on the left. Extraoral soft tissue analysis revealed a convex profile with upper and lower lips ahead of the Rickett’s esthetic line with an associated mentalis strain (Figure 3A-F). The patient elected for a limited plan focusing on the lower left alignment for opposing arch implant crown clearance.
Two clear aligner therapy plans were devised. Both plans used the upper model with restorative wax-ups provided by the dental student (Figure 2). This would ensure an accurate depiction of the estimated resulting buccal clearance following lower arch tooth movement. Both plans incorporated passive aligners on the upper arch to maintain tooth positions until delivery of permanent implant restorations. Additionally, the patient was able to utilize the pontic space in the upper passive aligners to apply temporary tooth replacement aligner trays for a temporary esthetic solution of the edentulous space. Orthodontic movements were planned for teeth #21-23.
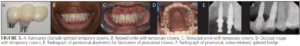
Plan 1 involved 1 mm retraction of tooth #22 with subsequent alignment of #21 and 23, resulting in 0.5 mm of interproximal reduction (IPR) in contacts distal to #21 to the mesial of #20 (Figure 4 A, C, E). Plan 2 was devised with 0.5 mm retraction of tooth #22, resulting in 0.2 mm of IPR in the same contacts (Figure 4 B, D, F). Both plans were reviewed with the prosthodontist in which plan 1 with 1 mm of canine retraction was recommended.
The patient began limited clear aligner treatment with 7-day aligner changes. Canine retraction was completed in 2 months and an intraoral scan was obtained then models printed. The progress models were reviewed with the prosthodontist who deemed adequate clearance for opposing implant restorations. Thus, no refinements were made and the patient completed orthodontic treatment. A lower lingual fixed retainer from #22-27 was bonded. Retention included the lower fixed retainer with an overlay. Total orthodontic treatment duration was 3 months and 2 weeks with 14 aligners.
After orthodontic treatment was completed, temporary crowns (Figure 5A and C) were fabricated chairside. The goal of the temporary crowns was to train the soft tissue to have an esthetic emergence profile similar to that of a natural tooth and to communicate to the patient the possible outcomes of the final restorations. The materials in the fabrication of the temporary restorations included composite resin and bis-acrylic resin.9
After 2 months of soft tissue training, the final zirconia crowns were delivered. Minor adjustments of the crowns were made to mimic the contours of contralateral natural dentition and to optimize occlusion. The patient approved of shade and function of final restorations. All involved in the treatment were happy with the outcome upon delivery (Figure 6).
Discussion
One of the most challenging aspects of executing the proposed treatment plan was achieving case acceptance. The patient was eager to proceed with the process of placing implants and restoring the edentulous space. However, they were hesitant about beginning orthodontic treatment at the age of 25. The hesitation posed a significant barrier to initially moving forward with the ideal treatment plan. To address this, the wax-up played a pivotal role in demonstrating the importance of orthodontic tooth movement. It provided a visual tool to illustrate how aligning the patient’s teeth was critical for avoiding anterior crossbite, which could potentially lead to fractures in the zirconia restorations.
An initial wax-up was carefully created and presented to the patient, which served as the basis for a comprehensive discussion. This included explaining the risks and benefits of proceeding with implant placement without first addressing the misalignment in the patient’s current dentition. During the consultation, alternative treatment options were explored; however, the clinician emphasized the potential complications associated with avoiding orthodontic treatment, particularly the heightened risk of prosthetic failure due to anterior crossbite. Ultimately, the patient gained a deeper understanding of the clinical necessity of the orthodontic treatment.
A pivotal component in achieving an effective and efficient surgical and restorative process was the use of a surgical guide. This tool ensured the accurate placement of implants according to the predetermined plan, minimizing the risk of complications. The use of the surgical guide minimized unnecessary trauma thereby increasing the chance of osseointegration and decreasing risk of marginal bone loss.10
Saline irrigation was also implemented to ensure minimal to no injury to the bone or surrounding soft tissue. Research shows that bone tissue is sensitive to heating at 47° C. Other studies have found an even greater risk of injury to tissues at 50° C and permanent damage when temperatures reach 60° C or higher.11 The importance of this finding is to strive for minimal trauma when performing surgeries to decrease likelihood of complications.
The advent of osseointegration further revolutionized the implant process, enabling a stable and durable integration of the implant.12 As described by Albrektsson,13 the osseointegration of an implant is judged in the context of a continuum of observation by looking at clinical evidence of mobility and the bone’s response radiographically. The absence or presence of a mobile implant has been proposed as clinical evidence of an integrated or nonintegrated implant respectively.
Radiographically, clinicians look for radiolucent zones around the implant, indicating a clear indication of anchorage in fibrous tissue. Albrektsson14 believes that if factors, including implant surface conditions, surgical technique, and loading conditions, are properly controlled, then osseointegration will be predictable, and implants will remain osseointegrated for decades. This is assuming the loading of the implant is of physiologic loads.
Together, the surgical guide and osseointegration not only streamlined the surgical procedure but also significantly improved the predictability and success of the restorative outcomes, underscoring the importance of prosthetically driven planning and modern techniques in dental implantology. The increased predictability and stability were particularly beneficial when initiating clear aligner treatment, as the precise placement of the implants provided an optimal foundation for the aligners to work effectively, ensuring a smooth and predictable tooth movement process without delaying the length of the treatment and without compromising the esthetic outcomes of the final restoration.
Conclusion
The treatment plan for this patient involved placing implants with a meticulous and multifaceted approach. These steps were essential in ensuring the final prostheses would be optimal in function, esthetics, and patient comfort. The extensive planning and use of interim solutions allowed the team to evaluate the fit and alignment progressively, making necessary adjustments before the final prostheses were delivered. This iterative process not only enhanced the precision of the final prostheses but also provided the patient with a visual understanding of the outcome. A multidisciplinary approach is indispensable when crafting a comprehensive treatment plan for complex cases. The success of this treatment was attributed to the patient’s cooperation and the effective communication and collaboration among multiple specialists.15
References
- Kaur T, Dhawan A, Bhullar RS, Gupta S. Cemento-ossifying fibroma in maxillofacial region: a series of 16 cases. J Maxillofac Oral Surg. 2021;20:240-245.
- Johal A, Huang Y, Toledano S. Hypodontia and its impact on a young person’s quality of life, esthetics, and self-esteem. Am J Orthod Dentofacial Orthop. 2022;161:220-227.
- MacDonald-Jankowski DS., Ossifying fibroma: a systematic review. Dentomaxillofac Radiol. 2009;38:495-513.
- Johal A, Amin M, Dean R. The impact of orthodontic treatment on a young person’s quality of life, esthetics, and self-esteem in hypodontia: a longitudinal study. Am J Orthod Dentofacial Orthop. 2023;164:813-823.e1.
- Hemmings K, Mannaa S, Gill D, Gulamali A, Petrie A. Treatment outcomes and assessment of oral health related quality of life in treated hypodontia patients. Eur J Prosthodont Restor Dent. 2017;25:49-56.
- Meaney S, Anwigi L, Ziada H, Allen F. The impact of hypodontia: a qualitative study on the experiences of patients. Eur J Orthod. 2012;34:547-552.
- Sadowsky SJ. Has zirconia made a material difference in implant prosthodontics? A review. Dent Mater. 2020;36:1-8.
- Fraulob M, Vayron R, Le Cann S, et al. Quantitative ultrasound assessment of the influence of roughness and healing time on osseointegration phenomena. Sci Rep. 2020;10:21962.
- Spyropoulou PE, Razzoog M, Sierraalta M. Restoring implants in the esthetic zone after sculpting and capturing the periimplant tissues in rest position: a clinical report. J Prosthet Dent. 2009;102:345-357.
- Brånemark PI Osseointegration and its experimental background. J Prosthet Dent. 1983;50:399-410.
- Eriksson AR, Albrektsson T. Temperature threshold levels for heat-induced bone tissue injury: a vital-microscopic study in the rabbit. J Prosthet Den. 1983;50:101-107.
- Bosshardt DD, Chappuis V, Buser D. Osseointegration of titanium, titanium alloy and zirconia dental implants: current knowledge and open questions. Periodontol 2000. 2017;73:22-40.
- Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1:11-25.
- Albrektsson T, Jacobsson M. Bone-metal interface in osseointegration. J Prosthet Dent. 1987;57:597-607.
- O’Sullivan M, O’Connell B. Multidisciplinary management of hypodontia. Prim Dent J. 2017;6:62-73.
From Decisions in Dentistry. July/August 2025;11(4):36-39.