Alternative Approach to Gingival Retraction
Consider this gingival retraction technique for exposing crown margins during fixed prosthodontic impressions.
Gingival retraction techniques to expose crown preparation margins have been well documented in the literature.1–5 During impression procedures, effective gingival retraction is required to capture accurate preparation margins and the tooth structure apical to them. The fit of the planned restoration hinges on the accuracy of this impression, from which fixed prosthodontic restorations can be fabricated that exhibit marginal accuracy and an appropriate emergence profile.
While many factors contribute to inaccurate impressions, a common problem relates to how well the clinician captured the prepared margin finish line,6 especially with subgingival or equigingival margins. In cases involving deeper preparation margins, the impression material must resist displacement from the gingival tissue, sulcular fluid and/or blood.7 The goal of gingival retraction is to atraumatically provide access for impression material beyond the preparation margins, while allowing sufficient thickness to prevent tearing and distortion upon removal.8,9 To ensure accuracy with vinyl polysiloxane (VPS) impression materials, at least a 0.2-mm thickness of impression material is needed in the sulcular area.10 Impressions with less sulcular width have higher incidences of voids and impression tears, which can result in decreased marginal accuracy.9,10
Methods commonly used for gingival retraction include retraction cord (in combination with various chemical solutions and gels that act as astringents or hemostatic agents), electrosurgical units, soft tissue diode lasers and retraction pastes — or a combination of these techniques. Gingival electrosurgery for crevicular troughing involves considerable risk for causing permanent periodontal damage.11 Thus, retraction cord has traditionally been the preferred means of achieving tissue retraction and hemostasis. A survey of more than 1200 members of the American College of Prosthodontists demonstrated that 98% of prosthodontists use retraction cord. Of those using cord, 81% soaked it first in a hemostatic solution, and of those who soaked their cord, 55% used aluminum chloride.1
Any time retraction cord is utilized, however, there is a risk for gingival recession, depending on the placement technique,12 as well as the patient’s periodontal tissue biotype13 and periodontal health. Use of retraction cords can damage the delicate epithelial lining of the sulcus and underlying connective tissues.14 Consequently, it is advantageous to use the smallest single-strand retraction cord possible (especially in the esthetic zone) to minimize tissue trauma and possible gingival recession. Studies by Ruel et al14 and Kazemi et al15 have shown that cord impregnated with aluminum chloride can cause up to 0.2 mm of gingival recession after 28 days. Additionally, use of minimal force is recommended when placing retraction cord, as excessive force may lead to crevicular bleeding, gingival inflammation and shrinkage of the marginal tissues.12 However, use of a single retraction cord often provides inadequate gingival retraction;5 in these cases, larger cords are often used in an attempt to provide adequate gingival displacement.
RETRACTION PASTE SYSTEMS
Retraction pastes were introduced to overcome some of the issues associated with retraction cord. These are touted as being gentle to the tissue, often eliminating the use of retraction cord altogether. The first to reach market was Expasyl (Kerr Dental), a clay-like material (kaolin) containing an astringent (aluminum chloride) that was intended to expand the sulcular tissue laterally, and concurrently provide hemostasis. Other products have since been introduced, such as Magic FoamCord (Coltene), GingiTrac (Centrix), Traxodent (Premier Dental), and, most recently, Retraction Capsule (3M ESPE). While most of these products provide good hemostasis, they have limited ability to displace tissue, especially in preparations with deeper subgingival margins or tissue that is more fibrous in nature. The exceptions regarding hemostasis are Magic FoamCord and GingiTrac, which do not have a hemostatic component, but, rather, release hydrogen following placement to expand the sulcus.
placed over preparation and the patient
closed into maximum intercuspation.
Following placement of the paste, some directions recommend compressing the paste into the tissue by use of a compression cap to create hydrostatic pressure to displace the tissue laterally and enhance retraction. Other techniques recommend having the patient bite on a cotton roll (placed over the paste) to accomplish a similar effect. These materials can be used alone in cases in which only hemostasis or minimal soft tissue retraction are needed. When additional hemorrhage control or soft tissue retraction are indicated, the materials can be combined with retraction cord, electrosurgery or soft tissue laser treatment. Traxodent, like Expasyl, also contains 15% aluminum chloride, and produces tissue contraction, shrinkage, precipitation of protein, constriction of blood vessels, and extraction of fluids from tissues.16
Aluminum chloride is the least irritating of the retraction medicaments17 and can be left in the sulcus for up to 15 minutes without causing permanent damage.18 Investigators have shown that certain retraction cord medicaments can modify the surface detail reproduction of impression materials,19 whereas de Camargo et al20 showed no ill effects on accuracy or polymerization of impression materials by hemostatic solutions used with retraction cords. It was their conclusion that inhibition of polymerization shown in other studies was likely caused by inadvertent contamination from latex gloves. As a precaution, it is recommended that all traces of medicaments be carefully removed before taking the definitive impression.

material trimmed.
Featuring a hydrophilic matrix, Traxodent — which was used in the procedure depicted here — can be flushed away with relative ease from the gingival sulcus, but care should be taken to remove any possible remaining residue prior to taking the final impression. The advantages of this system are that it provides reliable hemostasis and comes in an individually packaged syringe delivery system that does not require a separate carrier for administration of the material intraorally.
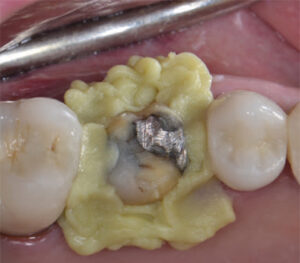
syringed around preparation margins.
As stated earlier, the main disadvantage of retraction paste systems is their limited ability to retract tissue in cases involving deeper subgingival margins.21 While these pastes have been shown to be less harmful to gingival tissues, their use results in less sulcular penetration of impression material when compared to the double retraction cord technique.22 As a result, they may not provide as much gingival retraction when used alone. In a 2012 study, Bennani et al23 showed the pressure of retraction paste was only one-tenth that of retraction cord. Each retraction method offers desirable clinical characteristics, which makes it imperative to match the features of a chosen technique or material to the specific case.24
As described by the authors, the following technique has shown good success for routine fixed prosthodontic impressions by providing gingival retraction and reliable hemostasis, while minimizing trauma and thereby reducing risk for future gingival recession.
ALTERNATIVE TECHNIQUE
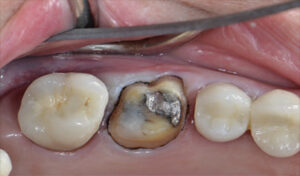
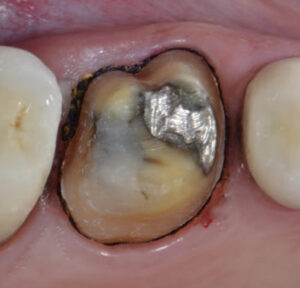
- Prepare the tooth for indirect restoration initially by keeping the preparation margins slightly supragingival or equigingival.
- Place a single strand of small 00 (or 0 in cases of a deeper sulcus) nonimpregnated gingival knitted retraction cord saturated for 20 minutes25 with aluminum chloride, cut so as to encompass the circumference of the tooth without overlapping, thereby protecting the soft tissue. Complete the preparation and final margin placement atraumatically (Figure 1).
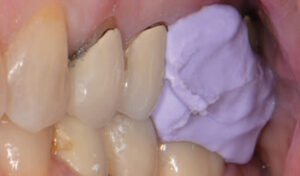
- Inject a rigid VPS interocclusal registration material around the margins and over the preparation(s). Instruct the patient to bite together on the back teeth (maximum intercuspation) and hold until the material has set (Figure 2). Clinicians may wish to rehearse this closure position with the patient to ensure the proper maxillo-mandibular position prior to actual placement of the material.
- Remove the VPS material and trim any flash to allow proper reseating intraorally (Figure 3).
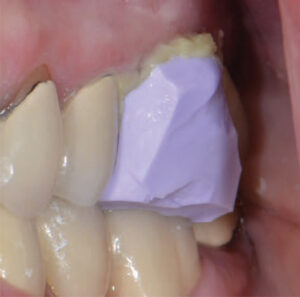
- Thoroughly rinse the tooth to remove any debris, lightly dry it, and slowly inject a hemostatic retraction paste through a syringe tip around the gingival margins of the preparation (Figure 4). Gently bend the tip to keep it parallel to the long axis of the tooth while injecting. Immediately reseat the VPS material over the preparation and have the patient close into the predetermined position and hold for three to five minutes (Figure 5); under occlusal load, pressure from the VPS material over the retraction paste provides tissue retraction and hemostasis.
- Remove the VPS interocclusal record and thoroughly rinse all of the retraction paste from the preparation and inspect carefully to ensure all residue is removed and adequate soft tissue retraction has been accomplished (Figure 6). If any residual paste remains, it can be removed by means of a wet cotton pellet. If the tissue bleeds upon rinsing and drying, but only minimally, reapply a hemostatic agent. If significant hemorrhage remains, reapply the hemostatic retraction paste and leave on for an additional three to five minutes, and rinse thoroughly prior to taking the impression. Leaving the 00 cord in place, dry the preparation and inject a light-bodied impression material around the preparation, followed by seating the tray containing the impression material.
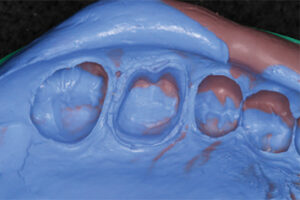
- When the material has reached its recommended set time, remove the impression tray. Inspect the impression for accuracy and completeness to ensure that all critical areas are captured and free from distortion, voids, tears or contamination (Figure 7).
SUMMARY
In most cases, using the described technique provides adequate tissue retraction with a single strand of 00 (or 0 if clinically indicated) retraction cord, followed by application of a hemostatic retraction paste. Placement of a hemostatic paste generally requires less time than placing a second retraction cord, and reduces the risk for tissue trauma and possible gingival recession, especially for patients with thin tissue biotypes. An additional advantage of this technique is the VPS material used to compress the retraction paste can be further trimmed and utilized for articulation of working casts (especially in cases of multiple adjacent preparations that include the terminal tooth). It can also be used to verify accuracy of the occlusal mounting prior to fabrication of the definitive restoration.
Even with increasing use of digital impressions in restorative dentistry, the need for tissue retraction and hemostasis still exists in order to capture accurate preparation margins. The technique described here can be utilized to improve marginal visualization for digital scans, and the interocclusal registration material/record used to compress the hemostatic paste can be scanned (if desired) to capture the opposing occlusion for use in the restorative digital design process.
KEY TAKEAWAYS
- Accurate impressions help ensure well-fitting, highly functional indirect restorations with the appropriate emergence profile.
- Even with the increasing use of digital impressions in restorative dentistry, the need for tissue retraction and hemostasis still exists in order to capture accurate preparation margins.
- The goal of gingival retraction is to atraumatically provide access for impression material beyond the preparation margins, while allowing sufficient thickness to prevent tearing and distortion upon removal.8,9
- Use of retraction cord poses risk for gingival recession, depending on the placement technique,12 as well as the patient’s periodontal tissue biotype13 and periodontal health. Cord can also damage the epithelial lining of the sulcus and underlying connective tissues.14
- Consequently, it is advantageous to use the smallest single-strand retraction cord possible (especially in the esthetic zone).
- Designed to overcome the issues associated with retraction cord, retraction pastes are touted as being gentle to the tissue and may eliminate the need for cord altogether.
- The main disadvantage of retraction paste systems is their limited ability to retract tissue in cases involving deeper subgingival margins.21
- Each retraction method offers desirable clinical characteristics, which makes it imperative to match the features of a chosen technique or material to the specific case.24
REFERENCES
- Hansen PA, Tira DE, Barlow J. Current methods of finish-line exposure by practicing prosthodontists. J Prosthodont. 1999;8:163–170.
- Shillingburg HT, Sather DA, Wilson Jr EL, et al. Fundamentals of Fixed Prosthodontics. 4th ed. Chicago, Ill: Quintessence Publishing Co; 2012:269–290.
- Baba NZ, Goodacre CJ, Jekki R, Won J. Gingival displacement for impression making in fixed prosthodontics: contemporary principles, materials, and techniques. Dent Clin N Am. 2014;58:45–68.
- Prasad KD, Hegde C, Agrawal G, Shetty M. Gingival displacement in prosthodontics: a critical review of existing methods. J Interdiscip Dent. 2011;1:80–86.
- Albaker AM. Gingival retraction — techniques and materials: a review. Pak Oral Dent J. 2010;30:545–551.
- Albashaireh ZS, Alnegrish AS. Assessing the quality of clinical procedures and technical standards of dental laboratories in fixed partial denture therapy. Int J Prosthodont. 1999;12:236–241.
- Lawson NC, Burgess JO. Clinicians reaping benefits of new concepts in impressioning. Compend Contin Educ Dent. 2015;36:152–153.
- Wassell RW, Barker D, Walls AW. Crowns and other extracoronal restorations: impression materials and technique. Br Dent J. 2002;192:679–684,687–690.
- Donovan TE, Chee WW. Current concepts in gingival displacement. Dent Clin North Am. 2004;48:433–444.
- Laufer BZ, Baharav H, Ganor Y, Cardash HS. The effect of marginal thickness on the distortion of different impression materials. J Prosthet Dent. 1996;76:466–471.
- Klung RG. Gingival tissue retraction following electro surgery. J Pros Dent. 1966;16:955.
- Parker S. The use of lasers in fixed prosthodontics. Dent Clin North Am. 2004;48:971–998,vii,viii.
- Sanavi F, Weisgold AS, Rose LF. Biologic width and its relation to periodontal biotypes. J Esthet Dent. 1998;10:157–163.
- Ruel J, Schuessler PJ, Malament K, Mori D. Effect of retraction procedures on the periodontium in humans. J Prosthet Dent. 1980;44:508–515.
- Kazemi M, Memarian MA, Loran V. Comparing the effectiveness of two gingival retraction procedures on gingival recession and tissue displacement: a clinical study. Res J Biol Sci. 2009;4:335–339.
- Burrell KH, Glick M. Hemostatics, astringents and gingival retraction cords. In: Ciancio SG, ed. ADA Guide to Dental Therapeutics. 2nd ed. Chicago, Ill: American Dental Association; 2000;104–118.
- Dental Product Spotlight. Gingival retraction. J Am Dent Assoc. 2002;133:653.
- Reiman MB. Exposure of subgingival margins by nonsurgical gingival displacement. J Prosthet Dent. 1976;36:649–654.
- O’Mahony A, Spencer P, Williams K, Corcoran J. Effect of 3 medicaments on the dimensional accuracy and surface detail reproduction of polyvinyl siloxane impressions. Quintessence Int. 2000;31:201–206.
- de Camargo LM, Chee WW, Donovan TE. Inhibition of polymerization of polyvinyl siloxanes by medicaments used on gingival retraction cords. J Prosthet Dent. 1993;70:114–117.
- Beier US, Kranewitter R, Dumfahrt H. Quality of impressions after use of the Magic FoamCord gingival retraction system — a clinical study of 269 abutment teeth. Int J Prosthodont. 2009;22:143–147.
- Martin TA, Rudolph H, Hrusa M, et al. Penetration depth of impression material after different soft-tissue management measures (abstract). J Dent Res. 2013;92(spec issue A):Abstract 3057.
- Bennani V, Aarts JM, He LH. A comparison of pressure generated by cordless gingival displacement techniques. J Prosthet Dent. 2012;107:388–392.
- Al Hamad KQ, Azar WZ, Alwaeli HA, Said KN. A clinical study of the effects of cordless and conventional retraction techniques on the gingival and periodontal health. J Clin Periodontol. 2008;35:1053–1058.
- Csempesz F, Vág J, Fazekas A. In vitro kinetic study of absorbency of retraction cords. J Prosthet Dent. 2003;89:45–49.
The authors have no commercial conflicts of interest to disclose.
From Decisions in Dentistry. January 2019;5(1):18–20,22.