 ANTONIO_DIAZ/ISTOCK/GETTY IMAGES PLUS
ANTONIO_DIAZ/ISTOCK/GETTY IMAGES PLUS
Evidence-Based Operatory Preparation Protocols
Dental teams must adhere to evidence-based guidelines to ensure the dental operatory is safe for patients and practitioners.
Professionals and researchers in dentistry, medicine and public health continue to discover innovative and more effective ways to prevent the spread of COVID-19. In dental settings, operatory preparation and disinfection are essential to providing safe care. Adequate hand hygiene, proper use of personal protective equipment (PPE), and thoroughly disinfecting environmental surfaces, devices and equipment are among the most important facets of infection prevention.1–3 Hand hygiene (e.g., handwashing or hand sanitizing) is one of the most critical standard precautions for reducing the risk of transmitting organisms to patients and oral health professionals, as it substantially reduces pathogens when performed properly.2,3 Meticulous planning and execution of disinfection and sterilization protocols for all aspects of the dental office, operatory and equipment provide the foundation for safe care. As scientific understanding of the SARS-CoV-2 pathogen remains fluid, oral health professionals should regularly seek updates on evidence-based guidelines and protocols.
Not all states require infection control continuing education for dental personnel; therefore, each clinician must strive to implement recommendations that represent current evidence and best practices. The U.S. Centers for Disease Control and Prevention (CDC) provides guidance on standard precautions in dental settings, specifically, its Guidelines for Infection Control in Dental Health-Care Settings — 2003, while the Occupational Health and Safety Administration (OSHA) is a regulatory agency responsible for enforcing standards. Dental practices are obligated to comply with OSHA’s Bloodborne Pathogens Standard (29 CFR 1910.1030) and Hazard Communication Standard (29 CFR 1910.1200).4–6
Because oral health professionals are routinely exposed to blood and other potentially infectious materials, OSHA requires employers to instill measures to protect clinicians from such exposure. This includes the provision of PPE (including gloves, masks, protective eyewear and protective garments), inoculation against hepatitis B, implementing safe work practices (including safety devices, such as sharps containers and needle recapping devices), and infection control training at least once per year.4,6 In addition, OSHA stipulates that employers provide training and PPE for employees who handle chemicals.3 Safety data sheets must accompany all chemicals and contain information about safe handling, including methods for storage, disposal and first aid instructions in the event of an accidental exposure. Current safety data sheet information must be kept for every chemical used and be accessible for at-risk employees at all times.3 Noncompliance with any of these regulations may result in OSHA violations.7
OPERATORY SURFACES
The CDC separates operatory surfaces into two categories: clinical contact surfaces and housekeeping surfaces. The former can be directly contaminated by patients’ bodily fluids or contact with contaminated gloves. Housekeeping surfaces (e.g., walls, window and sinks) generally do not contact patient material and pose a lower risk for disease transmission.
The potential for direct patient contact determines the protocols for cleaning and disinfecting surfaces. Other considerations are frequency of hand contact and probable contamination of the surface or area with bodily fluids or environmental sources of microorganisms (e.g., soil, dust or water).2,3
Frequently touched surfaces can serve as reservoirs for microbial contamination (e.g., light handles, switches, drawer knobs and chair controls). As such, barrier protection and/or disinfection of environmental surfaces must be performed prior to and between each patient to minimize the risk of disease transmission and healthcare–associated infections.2,3 Automated controls for soap dispensers, water faucets and towel dispensers are a convenient way to minimize contamination of frequently touched surfaces.
All items not essential to patient care should be removed from counters, such as supply containers, pamphlets or personal items. Disposable items and unit doses should be used whenever possible. Barriers should be implemented for areas and items that are difficult to clean.2,3 The dental operatory contains many items that are difficult to disinfect, including irregular surfaces, buttons, switches, electronics and keyboards. The decision to implement barriers and/or disinfection should be based on evidence-based standard precautions and must consider available manpower, cost and efficiency. Manufacturer-recommended custom-fit barriers should be used for intraoral cameras, curing lights, lasers and X-ray sensors which cannot be sterilized, but are used intraorally.
All clinical contact surfaces should be cleaned and disinfected at the beginning of the day, between patients, and at the end of the day using a U.S. Environmental Protection Agency (EPA)-registered hospital or intermediate-level disinfectant that remains wet for the recommended contact time.2,3,8 While housekeeping surfaces do not pose a significant risk for disease transmission in dental settings, floors and sinks should be cleaned on a daily basis, and spills cleaned up immediately. An EPA-registered low- or intermediate-level disinfectant or detergent designed for general housekeeping purposes should be used in patient-care areas.2,3,8 Per OSHA guidelines, puncture and chemical resistant gloves should be worn when using intermediate-level disinfectant.
The first step in cleaning is to remove any bioburden in order for disinfectant solutions to be effective within the recommended contact time. High ethyl alcohol solutions kill bacteria and deactivate viruses. The most commonly used disinfectants on the EPA’s list for effectively eliminating SARS-CoV-2 contain quaternary ammonium, sodium hypochlorite, hypochlorous acid, triethylene glycol and glycolic acid, hydrogen peroxide, chlorine dioxide, isopropanol, peroxyacetic acid, phenolic, ethanol, citric acid, sodium carbonate peroxyhydrate and/or thymol.2,3,9
EQUIPMENT
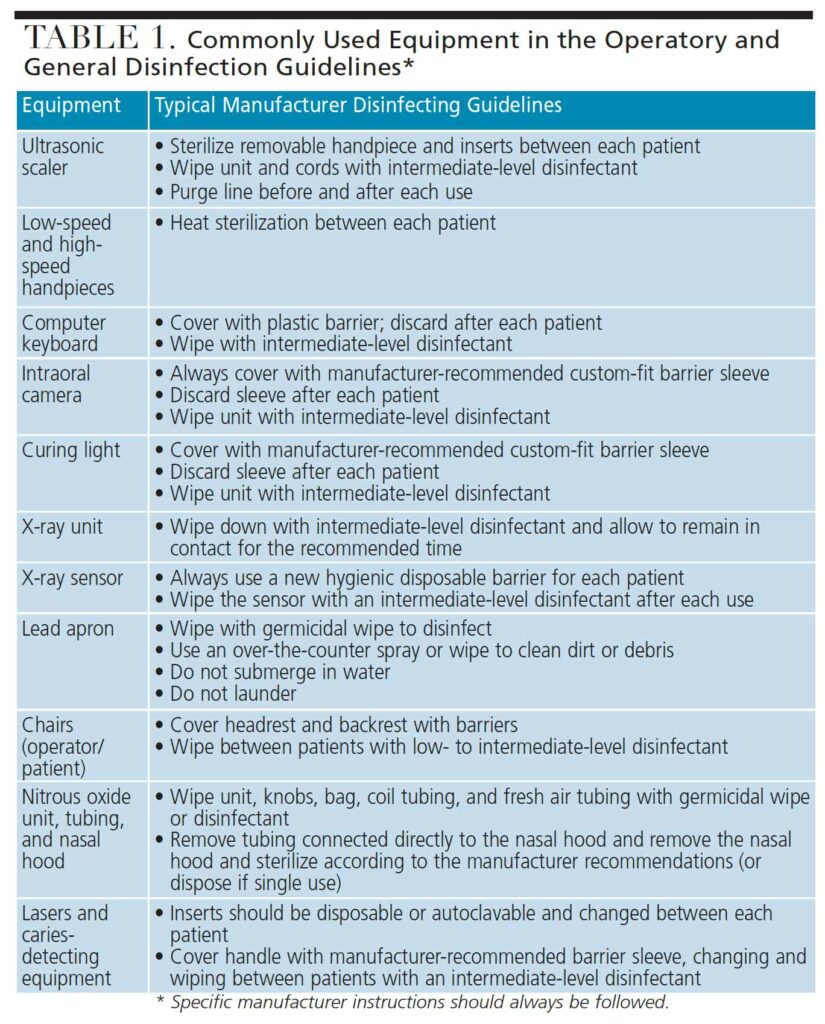
Manufacturers’ instructions for use should be reviewed to determine the appropriate method and products for the disinfection of dental equipment. Some equipment is sensitive to chemicals; therefore, products should be carefully selected for specific equipment and uses. Table 1 lists the most common equipment found in an operatory and general disinfection guidelines.10–12
As SARS-CoV-2 lingers in the air, it may be wise to wait before disinfecting patient rooms. However, the CDC does not currently recommend a specific wait time. In June 2020, the American Dental Association advised oral health professionals to allow some time before disinfecting an operatory.13 Considerations include air flow and filtration rates, number and length of any aerosol-generating procedures, patient volume, and use of rubber dams.13 Due to the potential for aerosols to linger, clinicians may consider donning PPE prior to entering the operatory and doffing PPE after they leave the operatory.
DENTAL AEROSOLS
Dental procedures produce aerosols, spatter and droplets contaminated with microorganisms, saliva and blood, which provide a potential route for disease transmission. The creation of aerosols by rotary handpieces, ultrasonic devices and air/water syringes is a major concern, and dental teams should attempt to minimize and capture potentially harmful aerosols. While the CDC’s current guidelines recommend avoiding aerosol-producing dental procedures if possible, when these procedures are indicated, the following strategies should be implemented: preprocedural rinsing, and use of high-volume evacuation (HVE), rubber dams, minimally invasive/atraumatic restorative techniques, hand scaling, and four-handed dentistry.11,12,14,15 An HVE tip measuring 8 mm or greater in diameter attached to an effective evacuation system can remove up to 100 cubic feet of air per minute.15
In addition to traditional HVE tips, many new HVE systems are available to reduce aerosols. Mandates from OSHA require employers to establish a respiratory program plan to protect employees from exposure to respiratory hazards. The respirator selected must be adequate to reduce the user’s exposure to aerosols, droplets, chemicals and other hazards.16
Dental unit waterlines can play a role in the creation of contaminated aerosols. The most common dental unit water sources are municipal water and closed-bottle systems. Both require cleaning and disinfection. Without appropriate waterline maintenance, microorganisms can adhere to the inner surface of waterlines and form biofilm that can enter the water stream. Microbial contamination of waterlines poses the greatest risk for older adults and the immunocompromised.17
Waterlines and related devices, including handpieces and ultrasonic scalers, should be run and flushed at the beginning of each day and between each patient for 20 to 30 seconds, even if anti-retraction valves are present.2,18 The EPA standard for safe drinking water and routine dental care is ≤ 500 colony-forming units per milliliter, but sterile saline or sterile water should be used for surgical procedures.2,14,17,18 The 2003 CDC guidelines recommend bacterial counts should be “as low as reasonably achievable,” but must meet the EPA standard for safe drinking water.2
Multiple systems are available for cleaning and maintaining waterlines, including chemical treatments, filters, and anti-retraction valves to control microbial contaminants and biofilms. Dental unit waterlines should be tested regularly based on the specific system recommendations to maintain the established standards.2,17,18
AIRFLOW
Heating, ventilating, and air conditioning (HVAC) systems in a dental facility may disperse aerosol contaminants. The COVID-19 pandemic has brought attention to the importance of a well-designed and maintained HVAC system to prevent the potential spread of pathogens. Operatories should be oriented parallel to the direction of airflow when possible.14 Increasing outside air flow, combined with the use of high efficiency particulate air (HEPA) filters that trap organisms in the HVAC system, may improve indoor air quality.
Some offices incorporate additional portable air filtration units with HEPA filters to further reduce airborne contamination in the operatory. Air exchange systems should be checked, measured and monitored to determine if modifications are required. Alternative disinfection methods, such as fogging, LED blue lights, and upper-room ultraviolet germicidal irradiation systems, are used in medical and dental settings as adjuncts, but additional research is needed to determine the effectiveness of these systems.14
CONCLUSION
Dental practices must use evidence-based guidelines and standard precautions when implementing infection control protocols. Patients trust dental teams to uphold the highest standards of infection prevention to ensure a safe care environment. Informing patients of additional measures and precautions implemented in the office for their safety will increase confidence in professional care.
REFERENCES
- Schneiderman MT, Cartee DL. Surface disinfection. In: DePaola L, Grant L, eds. Infection Control in the Dental Office. New York: Springer, Cham; 2019:169–191.
- Kohn WG, Harte JA, Malvitz DM, et al. Guidelines for infection control in dental health care settings — 2003. MMWR Recomm Rep. 2003;52(RR-17):1–61.
- U.S. Centers for Disease Control and Prevention. Summary of Infection Prevention Practices in Dental Settings: Basic Expectations for Safe Care. Available at: cdc.g/v/oralhealth/infectioncontrol/pdf/safe-care2.pdf. Accessed March 15, 2021.
- Occupational Safety and Health Administration. OSHA Laws & Regulations. Available at: osha.gov/laws-regs/oshact/section5-duties. Accessed March 15, 2021.
- Occupational Safety and Health Administration. Bloodborne Pathogens and Needlestick Prevention. Available at: osha.gov/bloodborne-pathogens. Accessed March 15, 2021.
- Garland K. Preventing and managing infection control breaches. Decisions in Dentistry. 2020;6(6):22–24.
- Occupational Safety and Health Administration. OSHA Penalties. Available at: osha.gov/penalties. Accessed March 15, 2021.
- U.S. Environmental Protection Agency. List N: Disinfectants for Use Against SARS-CoV-2. Available at: epa.gov/pesticide-registration/list-n-disinfectants-use-against-sars-cov-2. Accessed March 15, 2021.
- U.S. Environmental Protection Agency. List N Advanced Search Page: Disinfectants for Coronavirus (COVID-19). Available at: epa.gov/pesticide-registration/list-n-advanced-search-page-disinfectants-coronavirus-covid-19. Accessed March 15, 2021.
- Acosta-Gio E, Bednarsh H, Cuny E, Eklund K, Mills S, Risk D. Sterilization of dental handpieces. AJ J Infect Control. 2017;45:937–938.
- American Dental Association. Summary of ADA Guidance During the COVID-19 Crisis. Available at: https://success.ada.org/~/media/CPS/Files/COVID/COVID-19_Int_Guidance_Summary.pdf. Accessed March 15, 2021.
- American Dental Hygienists’ Association. ADHA Interim Guidance on Returning to Work. Available at: adha.org/resources-docs/ADHA_TaskForceReport.pdf. Accessed March 15, 2021.
- American Dental Association. ADA responds to change from CDC on waiting period length. Available at: https://www.ada.org/en/publications/ada-news/2020-archive/june/ada-responds-to-change-from-cdc-on-waiting-period-length. Accessed March 15, 2021.
- U.S. Centers for Disease Control and Prevention. Guidance for Dental Settings. Interim Infection Prevention and Control Guidance for Dental Settings During the COVID-19 Response. Available at: cdc.gov/coronavirus/2019-ncov/hcp/dental-settings.html. Accessed March 15, 2021.
- Harrel SK, Molinari J. Aerosols and splatter in dentistry, a brief review of the literature and infection control implications. J Am Dent Assoc. 2004;135:429–437.
- Occupational Safety and Health Administration. Respiratory Protection Program Guidelines. Available at: osha.gov/enforcement/directives/cpl-02-02-054. Accessed March 15, 2021.
- American Dental Association. Dental Unit Waterlines. Available at: ada.org/en/member-certer/oral-health-topics/dental-unit-waterlines. Accessed March 15, 2021.
- U.S. Food and Drug Administration. Dental Unit Waterlines. Available at: fda.gov/medical-devices/dental-devices/dental-unit-waterlines. Accessed March 15, 2021.
From Decisions in Dentistry. April 2021;7(4):21–23.


