
CE Sponsored by Zeiss: Restoring Endodontically Treated Teeth
A review of the key principles and treatment considerations that affect tooth and restoration survival following root canal treatment.
PURCHASE COURSE
This course was published in the January 2017 issue and expires 01/31/2020.The author has no commercial conflicts of interest to disclose.This 2 credit self-study activity is electronically mediated.
OBJECTIVES
After reading this course, the participant should be able to:
- Describe the challenges of restoring endodontically treated teeth (ETT), and how clinical choices can affect outcomes.
- List how the obturation technique in root canal therapy impacts tooth structure — and the possible ramifications for the restorative phase of treatment.
- Explain how the use of an operating microscope can help clinicians avoid complications during root canal treatment and when restoring ETT.
- Discuss how endodontic treatment can change dentin, and the role that timing plays in restorative success.
Introduction
ZEISS enables health care professionals worldwide to improve the lives of their patients in ophthalmology, microsurgery, and other medical and dental growth sectors. We advance the standard of care with our proven medical technology and application competence.
We are inspired by a clear vision: ZEISS wants to be the partner of choice for general dentists and specialists. Being a partner means understanding all aspects of dental providers’ requirements and the challenges they face to help them succeed. Success means optimal treatment for patients. Success also means being cost-efficient, achieving predictable outcomes, or offering what other oral health professionals cannot.
Our surgical microscopes for dentistry help clinicians visualize details and fine structures that are otherwise difficult to see, therefore enhancing the quality of treatment across all disciplines. With the goal of improving outcomes in root canal therapy and endodontic restoration, ZEISS is delighted to support the development of this article with an unrestricted educational grant. We hope it encourages a multidisciplinary approach to treatment and helps raise clinicians’ level of care.
The restoration of endodontically treated teeth (ETT) is often considered distinct from root canal therapy (RCT), yet the reality is they are inseparable in treatment planning, execution and prognosis. The restoration of ETT may be as important as the actual root canal obturation, as it has a profound effect in excluding the microorganisms that are the primary cause of endodontic disease.1 Following RCT, the clinician needs to protect the ETT from bacterial recontamination through the use of orifice barriers and/or provisional restorations. The ETT should be protected with a reliable interim prosthesis during and after RCT (Figure 1). The interim prosthesis enhances function and esthetics, while providing protection for the soft and hard tissues.
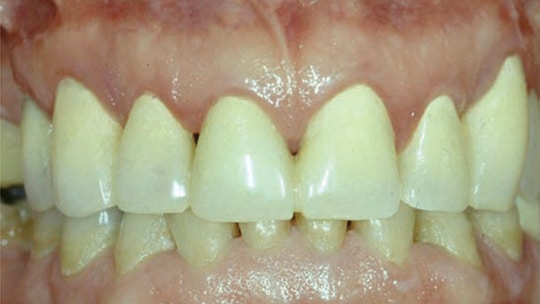
Directly following RCT, canal orifices are cleaned, etched and sealed with orifice barriers, such as flowable composite resin, glass ionomer, restorative composite resin, fissure sealant, or mineral trioxide aggregate.2 Both the interim prosthesis and orifice barriers prevent salivary recontamination and exposure of the canal to bacterial endotoxins — a source of bacterial inflammation and endodontic failure.1,3 The clinician should bear in mind that interim prostheses are short-term restorations that offer a poor coronal seal; this, in turn, can impact the prognosis of ETT.4 In a retrospective, nonrandomized cohort study of 775 ETT followed for 12 months, Willershausen et al5 found a higher survival rate for ETT when the final restoration was placed within two weeks after RCT. It is recommended to restore ETT immediately, as there is no benefit in postponing treatment until resolution or signs of healing appear (Figure 2).6 Following RCT, it is safe to remove the guttapercha and, if a post is used, prepare the post space directly with thermal and/or mechanical methods, as studies have shown no significant difference in leakage when post space is prepared immediately.7–10 Today, the use of computer aided design/computer aided manufacturing technology enables the dentist to design and mill a definitive restoration chairside, allowing the immediate sealing and protection of ETT.
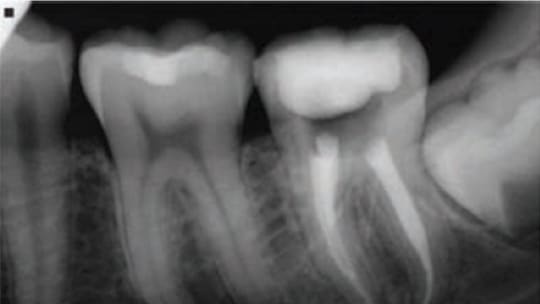
Over the years, a variety of methods and materials have been used to restore ETT.11 While prosthodontic, periodontal and endodontic therapies have been developed to retain compromised teeth, restoring ETT continues to be challenging — especially given the trend toward conservative endodontic and restorative treatment. Preserving ETT necessitates meticulous therapy based on the available evidence, with the goal of achieving an optimal endodontic/restorative interface. Despite clinicians’ best efforts, however, failures and complications in the restoration of ETT still exist, despite decades of clinical and laboratory research.12 Complications include root perforation, caries, periodontal failure, endodontic failure, root fracture, and post fracture or loosening. Of these, the two most common are post loosening and root fractures or cracks.12 The causes of cracks and fractures are multifactorial.13,14 The suggested primary causes of fracture are changes in dentin, reduced levels of proprioception caused by RCT, devitalization of the tooth, use of instrumentation and irrigants during RCT, loss of tooth structure, and the clinician’s restorative technique. In addition, various conditions — such as occlusion, periodontal issues, endodontic status, position of the restored tooth in the arch, and the amount of remaining tooth structure — can positively or negatively affect the prognosis of ETT.
While a number of papers have analyzed the principal factors that affect the long-term survival of ETT,15,16 this article will explore the concepts that affect tooth and restoration survival.
Impacts of Endodontic Therapy
Endodontic treatment causes several changes in dentin — for example, its water content, stiffness, elasticity and level of proprioception are reduced.14,17 In addition, dentin becomes sclerotic as a result of aging and exhibits no yielding before failure.18 Mechanical properties of the radicular dentin could be impacted by the utilization of endodontic medicaments and irrigants.19 As a result, dentin becomes weaker due to a decrease in microhardness. Following RCT, practitioners are advised to reduce the tensile forces applied to ETT by sealing the dentin cracks with a bonded composite core, covering the cusps with an occlusal material stiffer than dentin, and performing cuspal coverage.20,21
Root fractures in ETT can stem from apical or coronal origins. Studies have looked at the damage to root dentin caused during endodontic treatment with hand files and rotary instruments.22,23 The researchers concluded that using rotary instruments during RCT generates craze lines and partial cracks that could develop into fractures during endodontic retreatment, or following restoration of the tooth due to functional stresses caused by chewing and parafunction. Research has shown that lateral compaction causes significantly more defects than other types of obturation techniques.24 Other research has demonstrated that all filling techniques, except for single cone obturation, cause cracks in dentin.23 Other studies examined the impact of retreatment procedures on the occurrence of defects and cracks on the dentinal walls.23–25 They concluded that retreatment of ETT following various obturation techniques — except for the cold lateral condensation technique — leads to more cracks in dentin than during the initial RCT.
Importance of Visualization
The use of an operating microscope by the endodontist or treating dentist has proven to be very helpful in determining the presence of cracks and avoiding complications after restoration of ETT. The microscope could help determine the position and the extent of the cracks, thus contributing to a more accurate prognosis of ETT.
In addition to the operating microscope, a number of procedures — such as transillumination, occlusal tests and quantitative percussion diagnostics, to name a few — have been suggested to detect fractures and cracks when they are not clinically visible.26,27 Cone beam computed tomography (CBCT) has been used to diagnose vertical root fractures (VRFs), cracks and perforations.28 Research has shown that CBCT is more sensitive than conventional radiography in identifying VRFs.29 Neves et al30 evaluated CBCT in the diagnosis of VRFs and found that CBCT has little influence in the diagnosis of complete and incomplete fractures, and that the presence of intracanal material had a greater impact on diagnostic ability. They concluded that CBCT is not beneficial for diagnosing VRFs when a metal post is present in the canal. Moudi et al31 looked at the accuracy of CBCT in detecting VRFs by assessing the impact of obturation materials and intracanal posts in visualizing fractures. This study showed that CBCT is helpful in diagnosing VRFs, and that presence of a prefabricated post had little effect on the accuracy of the diagnosis — although the results were not statistically significant. In a systematic review and meta-analysis comparing the efficiency of CBCT and conventional radiography in the detection of VRFs, Corbella et al32 found that CBCT demonstrates high diagnostic accuracy in the detection of VRFs, and that diagnostic accuracy is higher in non-ETT than ETT. The presence of obturation materials or posts can complicate the visualization of VRFs.
Cervical Ferrule
Long-term outcomes for ETT rely on a number of key principles that affect tooth and restoration survival. Among these, the cervical ferrule is a crucial factor influencing the clinical outcome. It helps prevent coronal fractures, regardless of the type of post used (cast or prefabricated, metallic or nonmetallic). The ferrule’s length and form have been extensively investigated and proven to be indispensable to clinical success.33,34 If possible, maintaining 2 mm of intact tooth structure around the circumference of the tooth is desired to produce a beneficial crown ferrule (Figure 3). Rather than post length, the tooth’s resistance to fracture appears to be enhanced by the amount of tooth structure encompassed by the crown.
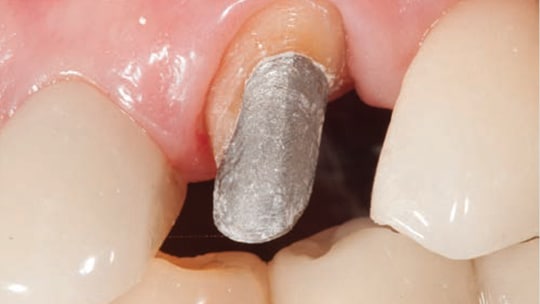
A uniform ferrule has significantly greater fracture resistance than a nonuniform ferrule.35,36 Naumann et al36 showed the absence of portions of the crown ferrule is related to the largest disparity in failure load. A long-term retrospective study of ETT restored with glass-reinforced epoxy resin posts (GFR) showed the presence of a nonuniform ferrule affected study results.37 Finite element analysis found a decrease in dentinal stress for both metallic and nonmetallic posts when a restored ETT had a ferrule.38 Recent research has shown the ferrule effect increases fracture resistance, irrespective of tooth location and restorative technique. The remaining coronal dental structure directly relates to the outcome; that is, the more tooth structure remaining after RCT, the better the outcome.39
In restorative procedures involving posts, the best prognosis for ETT is when the crown encompasses a 1.5 to 2 mm ferrule effect, a bonded core foundation is fabricated immediately after RCT (while the rubber dam is still in place to avoid canal contamination), and the tooth receives a full cuspal coverage (with posterior teeth). Jiang et al40 studied stress distribution in ETT and non-ETT restored with three types of inlays and onlays (gold, ceramic and composite resin). They found high concentrations of stress in dentin when teeth are endodontically treated; however, the use of proper restorations can minimize internal stresses. Cuspal coverage allows for more favorable stress distribution, regardless of the material or loading conditions — especially in the cervical portion of the root. In a randomized controlled clinical trial, Sterzenbach et al41 found that when a prefabricated post is placed with a self-adhesive cement in an ETT that has a 2 mm ferrule with two or fewer cavity walls, the postendodontic restoration will exhibit a high long-term survival rate, regardless of the post material used.
When inadequate cervical tooth structure is available to obtain a ferrule, surgical crown lengthening or orthodontic extrusion should be considered to expose additional tooth structure. In some cases, it may be difficult to acquire a ferrule; examples include dentition that has been substantially restored or subject to trauma, or a tooth that presents with significant caries. In this situation, it may be advisable to extract the tooth and place an implant and crown.
Cuspal Coverage
Most endodontically treated posterior teeth should be restored with crowns to enhance longevity. A large patient population that received RCT was studied to assess the survival rate of ETT. The researchers concluded that 85% of ETT that failed after eight years did not receive cuspal coverage following RCT.42 Studies have shown that ETT break during extraction, and pulpless molars without crowns can fracture.43 Aquilino et al44 report that ETT without crowns were lost at six times the rate of those with crowns. A systematic review found that ETT not restored with crowns had a lower long-term survival rate compared to teeth restored with crowns.45 The five-year post-delivery survival rate of teeth without cuspal coverage was 36%.46
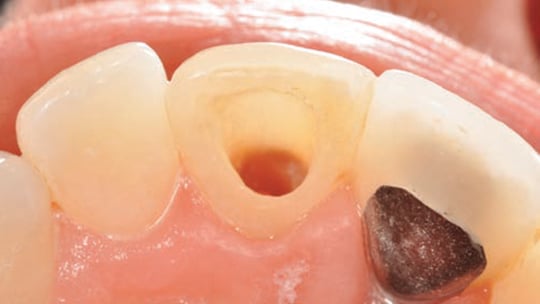
Anterior teeth that are intact (aside from the RCT access cavity) do not need to be crowned, except when they are compromised by large restorations or require extensive changes in shade or form (Figure 4). These teeth can be successfully restored with a composite resin or amalgam.46,47 Posterior teeth that are intact (except for the access cavity) can be restored successfully with composite resin (Figure 5).46,47 Composite is popular because it is esthetic, easy to use, and can be placed immediately.48 Studies have shown, however, that in the presence of a notable amount of missing tooth structure, the use of composite resin is a poor choice and ETT survival rates are likely to decrease.46,49
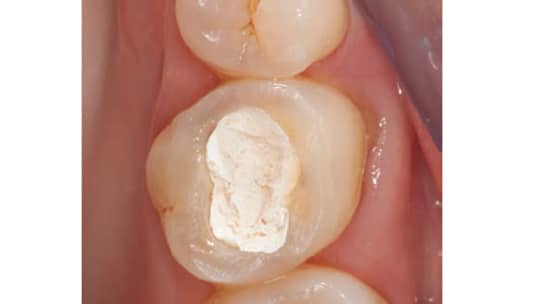
It has been suggested that a post be used to retain a composite core when less than 50% of the coronal tooth structure remains after RCT. Occlusion, adjacent teeth, and the planned definitive restoration should dictate the choice of buildup material. Clinicians are advised to restore posterior ETT with cuspal coverage when it has been previously restored and the remaining tooth structure weakened by multiple restorative procedures. If the posterior ETT is intact (except for a conservative access cavity) and shows little or no signs of occlusal wear to suggest deleterious occlusal forces, it can be restored with composite resin. Using a rubber dam for isolation, clinicians should consider placing a post and/or composite resin buildup material, being sure to comply with the manufacturer’s recommendations. A successful restoration requires the use of a low shrinkage composite resin50 built in small increments.51
The search for a conservative and esthetic restorative treatment modality that preserves maximum tooth structure — in combination with the advantage of covering the cusps — leads many clinicians to use all-ceramic onlays, endocrowns or crowns when restoring ETT.20,21,52
Post or No Post
Posts do not reinforce ETT; their purpose is to retain the core, rather than reinforce the root.53 Posts are not needed in ETT molars with sufficient tooth structure. In general, molars have enough retentive areas in the pulp chamber, divergent coronal portions, and in undercuts created during RCT and caries removal. Following RCT, if a molar presents with sufficient dentin to retain a core, clinicians are advised to ensure the post space is free of caries and cracks that could compromise ETT. The use of an operating microscope is recommended in such instances to avoid unnecessary tooth preparation, minimize the risk of perforation, and help improve the prognosis of the restored tooth.
In endodontically treated premolars and anterior teeth, posts are not needed if the teeth have satisfactory structure remaining to retain the core. A post is recommended if insufficient tooth structure is available to hold the core; it will also help clinicians achieve an optimum resistance form. The optimal prognosis of restored ETT will be achieved when a 2 mm ferrule encompasses intact tooth structure around the perimeter of the core, regardless of the type of post used.
When preparing a post space, another principle that affects tooth and restoration survival is leaving 5 mm of guttapercha at the apex. Studies show that having 4 to 5 mm of gutta-percha at the apex helps secure an appropriate seal,7,8 while ETT with only 2 to 3 mm of gutta-percha at the apex are subject to leakage.9,10
Mechanical, thermal and chemical methods have been suggested for removing gutta-percha during preparation of a post space.8,54,55 If the obturation material has been properly condensed, both rotary and heated hand instruments can be used to prepare the post space when 5 mm of gutta-percha is maintained apically.54,55 The immediate removal of guttapercha for post preparation has no adverse effects on the apical seal.7–10
Guidelines have been proposed to determine post length, because using the appropriate length will help minimize the potential for damage, optimize post retention, and maintain the apical seal. While short posts are not advised, research has shown that short posts are still used clinically56 and can cause stress that contributes to fractures.57
Although some clinicians embrace the concept of increasing post diameter to improve retention, research demonstrates that an increase in post diameter produces more stress in the root;58 another study suggests it decreases the tooth’s resistance to fracture.59 A third study also shows that larger post diameters are associated with root fracture.60 For every millimeter of decreased root diameter, an increase of 1.5 mm or more in post diameter increases the risk for root fracture by six-fold. During post preparation, it is important to use post preparation instruments that match the diameter of the posts and to drill the posts with the appropriate angulation.16,61
Types and Properties of Posts
Although chrome-cobalt, titanium and gold alloy posts are still widely used, clinicians can choose from a variety of prefabricated, nonmetallic tooth-colored posts; the most popular are made from GFR. Research suggests that tapered glass-fiber (GF) posts are less retentive than parallel-sided GF posts.62 In comparison to metallic posts, GFR posts are more flexible due to their low modulus of elasticity,63 which produces more stress cervically. When combined with minimal ferrule, these posts can fracture, causing debonding of the core or the posts themselves — accompanied by microleakage and secondary caries. Research suggests that the flexural strength of nonmetallic posts is reduced when the post is in contact with oral fluids, and strength is also reduced after thermocycling and cyclic loading.64 When compared to GF posts, metallic posts are stiffer and can produce more stresses apically — the main source of catastrophic root fracture. Though metal posts fracture less, their failure can potentially lead to nonrestorable root fractures.65
A literature review was conducted to evaluate the clinical performance of GFR and seek evidence regarding the treatment of teeth with nonmetallic posts.66 The results suggest failure might be due to weaknesses in the bonding of composite resin to the dentin and/or post. Based on these results and additional studies,67,68 clinicians may wish to consider using dual- or chemical-cure composite resin cement to ensure complete polymerization in the canal. Multiple causes have been attributed to post debonding, including shrinkage of the composite resin, lack of a comprehensive cementation protocol, absence of a ferrule effect, and inappropriate choice of post for a particular clinical situation.
Summary
Prior to RCT and restoration of ETT, dental professionals may wish to assess the remaining tooth structure for any cracks and/or craze lines, while also assessing the periodontal prognosis and restorability of the tooth. Once RCT is performed, ETT need to be rebuilt immediately, and a definitive restoration placed as quickly as feasible.
Given advances in conservative endodontic and restorative therapy — as well as today’s armamentarium — clinicians should plan treatment based on the best-available evidence. When treating these cases, optimal outcomes result when providers recognize that RCT and restorative care are inseparable parts of the planning, execution and prognosis for ETT.
REFERENCES
- Heling I, Gorfil C, Slutzky H, Kopolovic K, Zalkind M, Slutzky-Goldberg I. Endodontic failure caused by inadequate restorative procedures: review and treatment recommendations. J Prosthet Dent. 2002;87:674–678.
- Yamauchi S, Shipper G, Buttke T, Yamauchi M, Trope M. Affect of orifice plugs on periapical inflammation in dogs. J Endod. 2006;32:524–526.
- Gillen BM, Looney SW, Gu LS, et al. Impact of the quality of coronal restoration versus the quality of root canal fillings on the success of root canal treatment: a systematic review and meta-analysis. J Endod. 2011;37:895–902.
- Balto H, Al-Nazhan S, Al-Mansour K, Al-Otaibi M, Siddiqu Y. Microbial leakage of Cavit, IRM, and Temp Bond in post-prepared root canals using two methods of gutta-percha removal: an in vivo study. J Contemp Dent Pract. 2005;6:53–61.
- Willershausen B, Tekyatan H, Krummenauer F, Briseno Marroquin B. Survival rate of endodontically treated teeth in relation to conservative vs post insertion techniques — a retrospective study. Eur J Med Res. 2005;10:204–208.
- Iqbal MK, Kim S. For teeth requiring endodontic treatment, what are the differences in outcomes of restored endodontically treated teeth compared to implant-supported restorations. Int J Oral Maxillofac Implants. 2007;22(Suppl):96–116.
- Madison S, Zakariasen KL. Linear and volumetric analysis of apical leakage in teeth prepared for posts. J Endod. 1984;10:422–427.
- Bourgeois RS, Lemon RR. Dowel space preparation and apical leakage. J Endod. 1981;7:66–69.
- Portell FR, Bernier WE, Lorton L, Peters DD. The effect of immediate versus delayed dowel space preparation on the integrity of the apical seal. J Endod. 1982;8:154–160.
- Zmener O. Effect of dowel preparation on the apical seal of endodontically treated teeth. J Endod. 1980;6:687–690.
- Prothero JH. Prosthetic Dentistry. 2nd ed. Chicago: Medico-Dental Publishing; 1916:1116,1152–1162.
- Goodacre CJ, Baba NZ. Restoration of endodontically treated teeth. In: Ingle JI, Bakland LK, eds. Ingle’s Endodontics. 6th ed. Toronto, Canada: BC Decker Inc; 2008.
- Meyenberg K. The ideal restoration of endodontically treated teeth – structural and esthetic consideration: a review of the literature and clinical guidelines for the restorative clinician. Eur J Esthet Dent. 2013;8:238–268.
- Randow K, Glantz PO, Zöger B. Technical failures and some related clinical complications in extensive fixed prosthodontics: An epidemiological study of long-term clinical quality. Acta Odontol Scand. 1986;44:241–255.
- Baba NZ, Goodacre CJ, Daher T. The restoration of endodontically treated teeth: the seven keys to success. Gen Dent. 2009;57:596–603.
- Baba NZ, Goodacre CJ. Key principles that enhance success when restoring endodontically treated teeth. Roots. 2011;7:30–35.
- Helfer AR, Melnick S, Schilder H. Determination of the moisture content of vital and pulpless teeth. Oral Surg. 1972;34:661–670.
- Kinney JH, Nalla RK, Pople JA, Breunig TM, Ritchie RO. Age-related transparent root dentin: mineral concentration, crystallite size, and mechanical properties. Biomaterials. 2005;26:3363–3376.
- Ballal NV, Mala K, Bhat KS. Evaluation of the effect of maleic acid and ethyleneaminetetraacetic acid on the microhardness and surface roughness of human root canal dentin. J Endod. 2010;36:1385–1388.
- Guess PC, Selz CF, Steinhart YN, Stampf S, Strub JR. Prospective clinical split-mouth study of pressed and CAD/CAM all-ceramic partialcoverage restorations: 7-year results. Int J Prosthodont. 2013;26:21–25.
- Magne P, Carvalho A, Bruzi G, Anderson R, Maia H, Giannini M. Influence of no-ferrule and no-post buildup resin on the fatigue resistance of endodontically treated molars restored with resin nanoceramic CAD/CAM crowns. Oper Dent. 2014;39:595–602.
- Bier CA, Shemesh H, Tanomaru-Filho M, Wesselink PR, Wu MK. The ability of different nickel-titanium rotary instruments to induce dentinal damage during canal preparation. J Endod. 2009;35:236–238.
- Çapar ID, Saygili G, Ergun H, Gok T, Arslan H, Ertas H. Effects of root canal preparation, various filing techniques and retreatment after filling on vertical root fracture and crack formation. Dent Traumatol. 2015;31:302–307.
- Barreto MS, Moraes Rdo A, Moreira CH, Só MV, Bier CA. Vertical root fractures and dentin defect: effects of root canal preparation, filling, and mechanical cycling. J Endod. 2012;38:1135–1139.
- Kamaran P, Sivapriya E, Indhramohan J, Gopikrishna V, Savadamoorthi KS, Pradeepkumar AR. Dental defects before and after rotary root canal instrumentation with three different obturation techniques and two obturation materials. J Conserv Dent. 2013;16:522–526.
- Wright HM Jr, Loushine RJ, Weller RN. Identification of resected rootend dentinal cracks: a comparative study of transillumination and dyes. J Endod. 2004;30:712–715.
- Sheets CG, Stewart DL, Wu JC, Earthman JC. An in vitro comparison of quantitative percussion diagnostics with a standard technique for determining the presence of cracks in natural teeth. J Prosthet Dent. 2014;112:267–275.
- Shemesh H, Cristescu RC, Wesselink PR, Wu MK. The use of conebeam computer tomography and digital periapical radiographs to diagnose root perforations. J Endod. 2011;37:513–516.
- Wang P, Yan XB, Lui DG, Zhang WL, Zhang Y, Ma CX. Detection of dental root fractures by using cone-beam computed tomography. Dentomaxillofac Radiol. 2011;40:290–298.
- Neves FS, Freitas DQ, Campos PS, Ekestubbe A, Lofthag-Hansen S. Evaluation of cone-beam computed tomography in the diagnosis of vertical root fractures: the influence of imaging modes and root canal materials. J Endod. 2014;40:1530–1536.
- Moudi E, Haghanifar S, Madani Z, Alhavaz A, Bijani A, Bagheri M. Assessment of vertical root fracture using cone-beam computed tomography. Imaging Sci Dent. 2014;44:37–41.
- Corbella S, Del Fabbro M, Tamse A, Rosen E, Tsesis I, Taschieri S. Cone beam computed tomography for the diagnosis of vertical root fractures: a systematic review of the literature and meta-analysis. Oral Surg Oral Med Oral Pathol Oral Radiol. 2014;118:593–602.
- Ng CCH, Dumbrigue HB, Al-Bayat MI, Griggs JA, Wakefield CW. Influence of remaining coronal tooth structure location on the fracture resistance of restored endodontically treated anterior teeth. J Prosthet Dent. 2006;95:290–296.
- Morgano SM, Hashem AF, Fotoohi K, Rose L. A nationwide survey of contemporary philosophies and techniques of restoring endodontically treated teeth. J Prosthet Dent. 1994;72:259–267.
- Tan PL, Aquilino SA, Gratton DG, et al. In vitro fracture resistance of endodontically treated central incisors with varying ferrule heights and configurations. J Prosthet Dent. 2005;93:331–336.
- Naumann M, Preuss A, Rosentritt M. Effect of incomplete crown ferrules on load capacity of endodontically treated maxillary incisors restored with fiber posts, composite build-ups, and all ceramic crowns: An in vitro evaluation after chewing simulation. Acta Odontol Scand. 2006;64:31–36.
- Signore A, Benedicenti S, Kaitsas V, Barone M, Angiero F, Ravera G. Long-term survival of endodontically treated, maxillary anterior teeth restored with either tapered or parallel-sided glass-fiber posts and fullceramic crown coverage. J Dent. 2009;37:115–121.
- Eraslan O, Aykent F, Yücel MT, Akman S. The finite element analysis of the effect of ferrule height on stress distribution at post-and-corerestored all-ceramic anterior crowns. Clin Oral Investig. 2009;13:223–227.
- Skupien JA, Kreulen C, Opdam N, Bronkhorst E, Pereira-Cenci T, Huysmans MC. Effect of remaining cavity wall, cervical dentin, and post on fracture resistance of endodontically treated, composite restored premolars. Int J Prosthodont. 2016;29:154–156.
- Jiang W, Bo H, Yongchun G, LonXing N. Stress distribution in molars restored with inlays or onlays with or without endodontic treatment: a three-dimensional finite element analysis. J Prosthet Dent. 2010;103:6–12.
- Sterzenbach G, Franke A, Naumann M. Rigid versus flexible dentinelike endodontic posts — clinical testing of a biomechanical concept: seven-year results of a randomized controlled clinical pilot trial on endodontically treated abutment teeth with severe hard tissue loss. J Endod. 2012;38:1557–1563.
- Salehrabi R, Rotstein I. Endodontic treatment outcomes in a large patient population in the USA: and epidemiological study. J Endod. 2004;30:846–850.
- Eckerbom M, Magnusson T, Martinsson T. Prevalence of apical periodontitis, crowned teeth and teeth with posts in a Swedish population. Endodont Dent Traumatol. 1991;7:214–220.
- Aquilino SA, Caplan DJ. Relationship between crown placement and the survival of endodontically treated teeth. J Prosthet Dent. 2002;87:256–263.
- Stavropoulou AF, Koidis PT. A systematic review of single crowns on endodontically treated teeth. J Dent. 2007;35:761–767.
- Nagasiri R, Chitmongkolsuk S. Long-term survival of endodontically treated molars without crown coverage: a retrospective cohort study. J Prosthet Dent. 2005;93:164–170.
- Mannocci F, Qualtrough AJ, Worthington HV, Watson TF, Pitt Ford TR. Randomized clinical comparison of endodontically treated teeth restored with amalgam or with fiber posts and resin composite: five-year results. Oper Dent. 2005;30:9–15.
- Fedorowicz Z, Carter B, de Souza RF, Chaves CA, Nasser M, Sequeira-Byron P. Single crown versus conventional fillings for the restoration of root filled teeth. Cochran Database Syst Rev. 2012;5:CD009109.
- Sedgley CM, Messer HH. Are endodontically treated teeth more brittle? J Endod. 1992;18:332–335.
- Palin WM, Fleming GJ, Nathwani H, Burke FJ, Randall RC. In vitro cuspal deflection and microleakage of maxillary premolars restored with novel low-shrink dental composites. Dent Mater. 2005;21:324–335.
- Visvanathan A, LLie N, Hickel R, Kunzelmann KH. The influence of curing times and light curing methods on the polymerization shrinkage stress of a shrinkage-optimized composite with hybrid-type prepolymer fillers. Dent Mater. 2007;23:777–784.
- Dejak B, Motkowski A. 3D-Finite element analysis of molars restored with endocrowns and posts during masticatory simulation. Dent Mater. 2013;29:e309–e317.
- Pontius O, Hutter JW. Survival rate and fracture strength of incisors restored with different post and core systems and endodontically treated incisors without coronoradicular reinforcement. J Endod. 2002;28:710–715.
- Hiltner RS, Kulild JC, Weller RN. Effect of mechanical versus thermal removal of gutta-percha on the quality of the apical seal following post space preparation. J Endod. 1992;18:451–454.
- Haddix JE, Mattison GD, Shulman CA, Pink FE. Post preparation techniques and their effect on the apical seal. J Prosthet Dent. 1990;64:515–519.
- Grieve AR, McAndrew R. A radiographic study of post-retained crowns in patients attending a dental hospital. Br Dent J. 1993;174:197–201.
- Standlee JP, Caputo AA. The retentive and stress distributing properties of split threaded endodontic dowels. J Prosthet Dent. 1992;68:436–442.
- Mattison GD. Photoelastic stress analysis of cast-gold endodontic posts. J Prosthet Dent. 1982;48:407–411.
- Trabert KC, Caputo AA, Abou-Rass M. Tooth fracture — A comparison of endodontic and restorative treatments. J Endo. 1978;4:341–345.
- Standlee JP, Caputo AA, Collard EW, Pollack MH. Analysis of stress distribution by endodontic posts. Oral Surg Oral Med Oral Pathol Oral Radiol. 1972;33:952–960.
- Shillingburg HT, Kessler JC, Wilson EL. Root dimensions and dowel size. Calif Dent Assoc J. 1982;10:43–49.
- Teixeira ECN, Teixeira FB, Piasick JR, Thompson JY. An in vitro assessment of prefabricated fiber post systems. J Am Dent Assoc. 2006;137:1006–1012.
- Plotino G, Grande NM, Bedini R, Pameijer CH, Somma F. Flexural properties of endodontic posts and human root dentin. Dent Mater. 2007;23:1129–1135.
- Lassila LV, Tanner J, Le Bell AM, Narva K, Vallittu PK. Flexural properties of fiber reinforced root canal posts. Dent Mater. 2004;20:29–36.
- Torbjorner A, Fransson B. A literature review on the prosthetic treatment of structurally compromised teeth. Int J Prosthodont. 2004;17:369–376.
- Baba NZ, Golden G, Goodacre CJ. Nonmetallic prefabricated dowels: A review of compositions, properties, laboratory, and clinical test results. J Prosthodont. 2009;18:527–536.
- Mjor IA, Smith MR, Ferrari M, Mannocci F. The structure of dentine in the apical region of human teeth. Int Endod J. 2001;34:346–353.
- Mannocci F, Pilecki P, Bertelli E, Watson TF. Density of dentinal tubules affects the tensile strength of root dentin. Dent Mater. 2004;20:293–296.
Featured photo by MOODBOARD/THINKSTOCK
From Decisions in Dentistry January 2017; 3(1):37-42.




