 AMOKLV / ISTOCK / GETTY IMAGES PLUS
AMOKLV / ISTOCK / GETTY IMAGES PLUS
Alternative Restorative Treatment Of an Implant With Internal Thread Damage
This clinical report describes the use of a cast post-and-core to maintain functional restoration of an implant with internal thread damage.
Once an implant has osseointegrated, there are still factors which can cause failure of the restoration. These often arise from technical complications related to implant components — such as abutment screw loosening and screw fractures — or patient habits, including bruxism.1–4 A literature review by Katsavochristou and Koumoulis3 found that posterior implants experience a frequency of screw loosening and fractured components in the range of 7% to 11%, while Wie5 reported that 25% of this patient group presented with loose abutment screws at routine recalls.
When an abutment screw fractures, the implant may remain osseointegrated, but will not be restorable unless the apical end of the fractured screw can be removed. There are removal kits available for different brands of implants, but, on occasion, retrieval cannot be accomplished due to the location or size of the remaining screw fragment.1,6 In addition, the internal threads of an implant can be damaged to the extent that an abutment screw will not engage and therefore cannot retain an abutment.7 Under these circumstances, the alternative of restoring the implant with a cast post-and-core may allow continued function of the implant-supported restoration.8,9 This clinical case report describes the use of a cast post-and-core to maintain functional restoration of an implant with internal thread damage.
CASE REPORT
A 66-year-old male of American Society of Anesthesiologists (ASA) physical classification system ASA II health status presented for recall in the faculty practice at the Dental College of Georgia at Augusta University with cemented, implant-supported splinted gold crowns in the #14 and 15 sites. He reported the crowns had been “feeling loose for two days.” An examination and periapical radiograph showed two osseointegrated 4.8×10 mm implants, with adequate supporting bone height and no signs of inflammation or bleeding of the surrounding soft tissue. The patient also had a fractured abutment screw on #14.
The proposed treatment accepted by the patient was preparation through the occlusal surfaces of both implant crowns to gain access for removal of the abutment-retaining screws. This would be followed by removal of the crowns and fractured screw fragment from #14, with replacement using new screws for both abutments/crowns. These would then be functionally screw-retained, and the access openings filled.
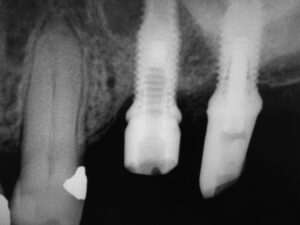
After removal of the crowns and abutments, retrieval of the screw fragment in #14 using the manufacturers’ rescue kit was unsuccessful due to the fragment being jammed into the implant threads. Use of an ultrasonic scaler to loosen the screw also proved unsuccessful. With the patient’s consent, it was decided to attempt removal of the fractured screw fragment with a high-speed handpiece. A straight carbide fissure bur was selected based on diameter, length, and end-cutting capability. This bur was used at 150,000 rpm with copious water coolant to attempt removal of the screw fragment. Unfortunately, a subsequent periapical radiograph taken to assess the extent of fragment removal showed the implant’s internal threads were damaged (Figure 1).
It was then determined the best alternative to maintain the implant-supported crowns was to discontinue removal of the screw fragment and replace the abutment on #14 with a cast post-and-core. Residual threads in the implant body were smoothed using the same bur, and a 0.90 mm burnout post was directly custom fitted to the internal walls of the implant using pattern resin. Next, the abutment was removed by heating from the #14 crown, and the existing crowns were secured using the abutment retaining screw for #15 (where the crown remained cemented to the abutment).
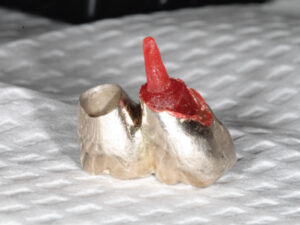
Using the screw access on the occlusal surface of the crown on #14, pattern resin was injected into the crown around the customized burnout post to form the core and complete the pattern (Figure 2). The crowns were then removed, the pattern removed and finished, and the pattern and existing crowns replaced to verify seating. Provisionalization was accomplished by securing the two crowns and their abutments using only the abutment retaining screw for #15.
At this stage, the resin pattern was invested and cast in a nickel-chromium alloy, yielding a one-piece, cast post-and-core. On the day of delivery, the casting was first tried into the implant and lightly adjusted to ensure a passive fit. The existing crowns, plus the abutment for #15, were tried in atop the casting to verify seating and a passive fit. The cast post-and-core was sandblasted and cemented into the implant using a resin composite cement.
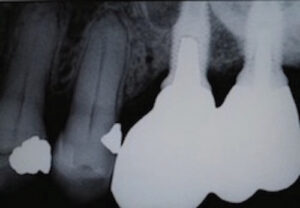
After removal of excess cement, the existing splinted gold crowns were replaced, with the crown on #14 cemented with the same product, and the crown and abutment on #15 secured with a new retaining screw. Lastly, both screw accesses on the occlusal surfaces of the crowns were closed with resin composite, occlusion was checked, and a final radiograph taken to verify the correct seating of the post (Figure 3).
DISCUSSION
Ideally, periodic recall exams should detect loose implant screws before they fracture so that restorations can be stabilized with the simpler process of screw replacement. In this case, however, a loose abutment screw went undetected until a facture occurred. Another factor to consider is the occlusion and shape of the implant-supported crowns. When heavy occlusal contacts exist, it may cause loosening of the screws that will eventually fracture with time. Although a post space inside an implant is necessarily short, the space at least has parallel walls to enhance retention. The need for an anti-rotation feature in a post space was minimized in this case by splinting the two crowns. Should this become a consideration for a single unit, anti-rotation should be accomplished without weakening the implant body — preferably by adapting the pattern into the anti-rotation feature for the abutment built into the implant body, such as an internal hex.
Since abutment screw loosening is not uncommon, it should be addressed through rigorous protocols for tightening retaining screws, probably including retorquing several minutes after initial placement. Because screw replacement is more complicated for cemented restorations, clinicians might also consider use of screw-retained restorations where high occlusal loading is anticipated. Based on this and other reports, use of a cast post-and-core seems to be justified and has previously been advocated as a conservative option for maintaining existing crowns when abutment screws have fractured and cannot be retrieved.10
SUMMARY
Although this patient presented soon after he felt looseness of his crowns, retrieval of the fractured retaining screw could not be accomplished and the internal threads of the implant were damaged in the attempt. Fortunately, the usual surgical removal and replacement of a damaged implant has thus far been avoided. The fabrication of a cast post-and-core as an alternative for maintaining the implant, as well as its existing crown, appears to have been a viable option in this case. More clinical long-term studies are needed to corroborate the efficacy of this technique.
Key Takeaways
- Failure of an osseointegrated implant restoration often arises from technical complications related to implant components, such as abutment screw loosening or screw fractures.
- When fracture of an abutment screw occurs, the implant may remain osseointegrated, but will not be restorable unless the apical end of the fractured screw can be removed.
- In cases in which an implant is damaged to the extent that an abutment screw will not engage and therefore cannot retain an abutment, the alternative of restoring the implant with a cast post-and-core may allow continued function of the implant-supported restoration.8,9
- Although a post space inside an implant is necessarily short, the space at least has parallel walls to enhance retention. And, in this case, the need for an anti-rotation feature in the post space was minimized by splinting the two crowns.
- Based on this case and other reports, use of a cast post-and-core has been advocated as a conservative option for maintaining existing crowns when abutment screws have fractured and cannot be retrieved.10
REFERENCES
- Satwalekar P, Chander KS, Reddy BA, Sandeep N, Sandeep N, Satwalekar T. A simple and cost effective method used for removal of a fractured implant abutment screw: a case report. J Int Oral Health. 2013;5:120–123.
- Carlson B, Carlsson GE. Prosthodontic complications in osseointegrated dental implant treatment. Int J Oral Maxillofac Implants. 1994;9:90–94.
- Katsavochristou A, Koumoulis D. Incidence of abutment screw failure of single or splinted implant prostheses: A review and update on current clinical status. J Oral Rehabil. 2019;46:776–786.
- Brägger U, Aeschlimann S, Bürgin W, Hämmerle CH, Lang NP. Biological and technical complications and failures with fixed partial dentures (FPD) on implants and teeth after four to five years of function. Clin Oral Implants Res. 2001;12:26–34.
- Wie H. Registration of localization, occlusion and occluding materials for failing screw joints in the Brånemark implant system. Clin Oral Implants Res. 1995;6:47–53.
- Luterbacher S, Fourmousis I, Lang NP, Brägger U. Fractured prosthetic abutments in osseointegrated implants: a technical complication to cope with. Clin Oral Implants Res. 2000;11:163–170.
- Sadid-Zadeh R, Kutkut A, Kim H. Prosthetic failure in implant dentistry. Dent Clin North Am. 2015;59:195–214.
- Froum SJ. Dental Implant Complications: Etiology, Prevention, and Treatment. Hoboken, NJ: Wiley-Blackwell; 2015.
- Dashti MH, Alshali SA, Haddad MJ. Management and restoration of an implant with irreversibly damaged internal threads: a clinical report. J Oral Implantology. 2016;42:417–420.
- Wiskott H, Belser UC. Mechanical resistance of cemented post and core buildups for ITI‐Bonefit implants. Clin Oral Implants Res. 1992;3:128–135.
From Decisions in Dentistry. July 2022;8(7)10,13-14.


