
Imaging Technologies in Dental Implantology
Advances in radiography provide clinicians with more options than ever before for evaluating patients and planning implant treatment.
Over the last several decades, dental implants have grown in popularity and now demonstrate high survival rates over time,1 leading many clinicians to consider them the standard of care for the replacement of missing teeth. Long-term studies have consistently shown implant success rates of greater than 90%, with a recent study in a large cohort of Swedish patients examined nine years after implant placement showing that overall, only 7.6% of patients had lost at least one implant.2
However, dental implants present new challenges for dentists and may not be suitable for all patients — especially those with a history of past or current smoking, periodontal disease, uncontrolled or poorly controlled diabetes mellitus, or poor oral hygiene, all of which are risk factors associated with implant failure.2–4 In patients clinically determined to be good candidates to receive dental implants, thorough examination and careful planning are essential to avoid anatomical structures during osteotomy preparation and ensure placement of the implant in a position that maximizes restorative potential and preserves the health of the patient and long-term stability of the implant. There is also a need to routinely monitor and maintain implants that have already been placed, as this has been shown to reduce complications from peri-implant disease.5
Though essential, clinical exam alone often fails to detect the underlying and surrounding hard and soft tissue anatomy of the proposed or current implant site. Thus, radiographic examination plays an equally important part in the presurgical, intrasurgical and postsurgical placement and management of dental implants. The purpose of this review is to discuss dental radiography and, more specifically, the appropriate selection and use of radiographs in implant treatment.
GENERAL CONSIDERATIONS
Radiographic images are produced by passing X-ray radiation through oral structures and onto a film or digital sensor. In implant dentistry, radiographs are used to assess the anatomy of the region of interest, including both the quality and quantity of bone available to support an implant, the presence or absence of pathology in edentulous sites, around existing implants and adjacent teeth, and proximity of the implant or edentulous space to vital structures, such as neurovascular bundles, the maxillary sinus, and concavities or undercuts, like those that commonly occur on the facial of the anterior maxilla or the lingual of the posterior mandible.6 Although multiple imaging modalities are available, each of these images and imaging techniques has a specific application, and some (or all) of them may be used when planning an implant case. The clinician should be judicious in deciding which radiographs to take, always keeping the “as low as reasonable achievable” (ALARA) principle in mind to reduce the amount of radiation delivered to the patient.
TWO-DIMENSIONAL IMAGES
Periapical and panoramic radiographs are commonly used in implant dentistry and are two-dimensional (2D) representations of three-dimensional (3D) objects. Periapical radiographs are intended to provide a view of the entire tooth or implant, including the apex and surrounding bone. They are useful because they are readily available to most dentists, provide high resolution (at relatively low cost),7 and deliver a fairly low effective dose of radiation to the patient, estimated to be less than 5 microsieverts (µSv), or the dose delivered by taking four bitewing radiographs.8 However, periapical images have the potential for distortion; in addition, they offer limited reproducibility and limited size.7
While periapical images are useful for evaluating the mesiodistal dimension and vertical bony height of the area of interest, they do not provide an accurate assessment of the width of bone in a bucco-lingual or bucco-palatal dimension. Therefore, they have limited usefulness in assessing proposed implant sites in which the adequacy of the bucco-lingual or bucco-palatal width is in question following clinical examination. Further, when evaluating a previously placed implant for potential pathology, the buccal and lingual or palatal surfaces and surrounding hard and soft tissue are difficult to detect using a periapical image alone. In these situations, additional radiographs are often needed.9

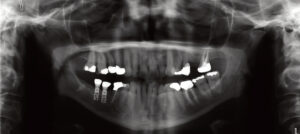
Panoramic images are produced by an X-ray source that rotates around the patient’s head, showing the structures that remain within the focal trough with minimal distortion, and those outside of the focal trough with more distortion.6 They are intended to show the majority of the maxilla and mandible, along with the surrounding and supporting structures, such as the location, size and extent of the nasal cavity and maxillary sinus, the course of the inferior alveolar canal, and the temporomandibular joint.10 Panoramic radiographs are useful for general patient evaluation, including assessment of the presence or absence of dental or bony pathology, the presence and extent of edentulous areas and their potential to support implants, and the anatomical limitations near each edentulous site. Furthermore, effective radiation dose to the patient is also relatively low, ranging from 3 to 24 µSv.11 However, as with periapical radiographs, they are a 2D representation of a 3D object, and therefore generally cannot be used alone in presurgical implant planning or post-placement implant evaluation. Compared to other modalities, they also have lower resolution and an increased potential for distortion due to difficulty in positioning the patient within the focal trough.7 Nevertheless, panoramic radiographs are useful as an initial diagnostic and screening tool (Figure 1).
THREE-DIMENSIONAL IMAGES
The introduction of 3D imaging to implant dentistry has dramatically improved the amount of diagnostic information that can be obtained. For example, cross-sectional images of the maxilla and mandible provide a more precise representation of bony height and width, in addition to the accurate 3D location of anatomic structures, offering improved safety and predictability during implant placement. Using cross-sectional images, the complex anatomical structures of the maxilla and mandible — such as the inferior alveolar canal and its anterior loop, mandibular incisive canal, mental foramen, lingual canal, maxillary nasopalatine canal, nasal cavity and maxillary sinus11 — can be evaluated prior to, and during, implant surgery. In cases in which peri-implant pathology is suspected, cross-sectional images will more accurately depict the buccal and lingual or palatal surface of the implant than traditional 2D imaging (such as periapical and panoramic radiographs.)9 However, it should be noted there is a certain degree of beam scattering that can be produced by the presence of implants, and this has been shown to reduce the accuracy and visualization of the bone-to-implant interface.12,13
Cone beam computed tomography (CBCT), which works by taking multiple thin axial slices with minimal distortion and uniform thickness and magnification,10 utilizes software that reconstructs these slices into valuable cross-sectional images of the area of interest. A CBCT varies from a computed tomogram (CT) in that there is only a single X-ray source that is focused in a beam, rather than the fan beam that is produced by conventional CT imaging.10 While radiation doses for most CBCT units vary considerably among manufacturers (largely due to the available fields of view [FOV] produced by the machine), the detector technology and the scanning times of most CBCT units deliver an effective radiation dose in the 50 to 200 µSv range. This is higher than the doses produced by standard 2D radiographs, but lower than the 1000 to 2000 µSv produced by multidetector CT protocols.11,14 The FOV refers to the area of anatomy that is captured by the CBCT unit. The smallest FOV possible should be used to ensure diagnostic goals are achieved while limiting radiation exposure to the patient.10 In adults, the amount of radiation delivered by small FOV CBCT units has been shown to range from 5 to 652 µSv, while medium FOV units range from 9 to 560 µSv, and large FOV units range from 46 to 1073 µSv.11 Individual doses may vary in children due to their smaller size and different position of radiosensitive organs in the body.14
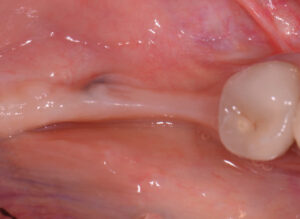
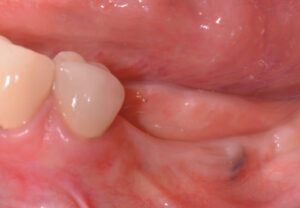
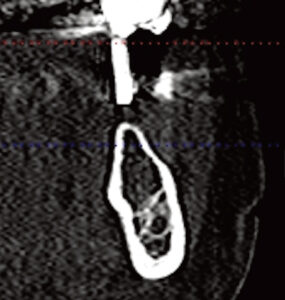
In addition to a lower radiation dose for the patient compared to conventional CT imaging, other advantages of CBCT include high accuracy, high resolution, less expensive equipment (compared to CT), and a relatively low cost for the patient.10,11 Figure 2 through Figure 5 show a case in which the clinical examination was combined with periapical and CBCT imaging to plan an implant in the edentulous site of the lower left first molar.
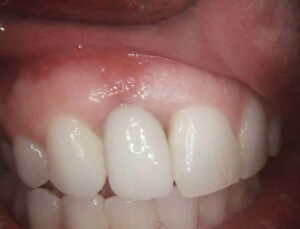
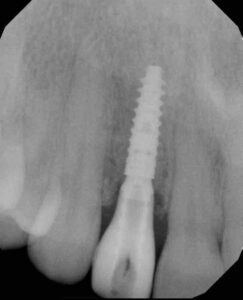
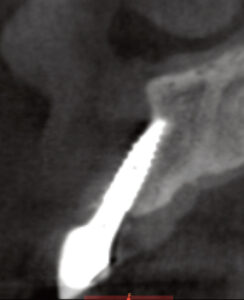
Implant surgeons can further improve the predictability and safety of implant placement by utilizing software that allows virtual placement of implants in the cross-sectional images produced by CBCT technology. In especially difficult cases, a surgical guide can be fabricated based on the virtual surgical plan to facilitate more accurate placement of the implant. However, the associated need for additional materials and increased cost may outweigh the benefits in more straightforward cases.11 Figure 6 through Figure 8 show a case in which a patient complained about the esthetics and tenderness of an implant placed in the upper right lateral incisor site less than 12 months prior.
While CBCT is useful in implant dentistry, it may not be necessary in all cases. As previously mentioned, CBCT still delivers a higher dose of radiation to the patient compared to conventional 2D radiographs, so clinicians should always consider the ALARA principle when deciding whether a CBCT image is needed.
SUMMARY AND CONCLUSION
Recent advances and improvements in dental radiography provide the dentist with more options to plan and evaluate implants than ever before. Clinicians should apply selection criteria to determine which radiographs will be needed for a particular case, based on the need for diagnostic information and treatment objectives. Periapical, panoramic and CBCT imaging each have their advantages and disadvantages, highlighting the importance of taking only the radiographs necessary for the case and adhering to the ALARA principle to minimize the radiation dose delivered to the patient. When appropriately applied, radiographic examination serves as an essential adjunct to a thorough clinical exam. Together, these provide a solid foundation on which to plan and evaluate dental implant therapy.
KEY TAKEAWAYS
- A thorough examination and careful planning are essential to ensure placement of dental implants in a position that maximizes restorative potential.
- Clinical examination alone often fails to detect the underlying and surrounding hard and soft tissue anatomy of the proposed or current implant site.
- Thus, radiography plays an equally important part in the presurgical, intrasurgical and postsurgical placement and management of dental implants.
- Panoramic radiographs are useful for general evaluation, including assessment of the presence or absence of dental or bony pathology, the presence and extent of edentulous areas and their potential to support implants, or other anatomical limitations.
- Clinicians can improve the predictability of implant placement by utilizing software that allows for virtual placement of implants in the cross-sectional images produced via cone beam computed tomography.
- Implantologists should apply selection criteria to determine which radiographs will be needed for a particular case, always striving to obtain the necessary information with minimum radiation exposure to patients.
References
- Jung RE, Zembic A, Pjetursson BE, Zwahlen M, Thoma DS. Systematic review of the survival rate and the incidence of biological, technical, and aesthetic complications of single crowns on implants reported in longitudinal studies with a mean follow-up of 5 years. Clin Oral Implants Res. 2012;23(Suppl 6):2–21.
- Derks J, Håkansson J, Wennström JL, Tomasi C, Larsson M, Berglundh T. Effectiveness of implant therapy analyzed in a Swedish population: early and late implant loss. J Dent Res. 2015;94(3 Suppl):44s–51s.
- Grisar K, Sinha D, Schoenaers J, Dormaar T, Politis C. Retrospective analysis of dental implants placed between 2012 and 2014: indications, risk factors, and early survival. Int J Oral Maxillofac Implants. 2017;32:649–654.
- Monje A, Catena A, Borgnakke WS. Association between diabetes mellitus/hyperglycaemia and peri-implant diseases: Systematic review and meta-analysis. J Clin Periodontol. 2017;44:636–648.
- Monje A, Wang HL, Nart J. Association of preventive maintenance therapy compliance and peri-implant diseases: a cross-sectional study. J Periodontol. 2017;88:1030–1041.
- Angelopoulos C, Aghaloo T. Imaging technology in implant diagnosis. Dent Clin North Am. 2011;55:141–158.
- Tyndall DA, Brooks SL. Selection criteria for dental implant site imaging: a position paper of the American Academy of Oral and Maxillofacial radiology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;89:630–637.
- Ludlow JB, Davies-Ludlow LE, White SC. Patient risk related to common dental radiographic examinations: the impact of 2007 International Commission on Radiological Protection recommendations regarding dose calculation. J Am Dent Assoc. 2008;139:1237–1243.
- Schliephake H, Wichmann M, Donnerstag F, Vogt S. Imaging of peri-implant bone levels of implants with buccal bone defects. Clin Oral Implants Res. 2003;14:193–200.
- Tyndall DA, Price JB, Tetradis S, et al. Position statement of the American Academy of Oral and Maxillofacial Radiology on selection criteria for the use of radiology in dental implantology with emphasis on cone beam computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;113:817–826.
- Rios HF, Borgnakke WS, Benavides E. The use of cone-beam computed tomography in management of patients requiring dental implants: an American Academy of Periodontology best evidence review. J Periodontol. 2017;88:946–959.
- Schulze RK, Berndt D, d’Hoedt B. On cone beam computed tomography artifacts induced by titanium implants. Clin Oral Implants Res. 2010;21:100–107.
- Benic GI, Sancho-Puchades M, Jung RE, Deyhle H, Hämmerle CH. In vitro assessment of artifacts induced by titanium dental implants in cone beam computed tomography. Clin Oral Implants Res. 2013;24:378–383.
14. Bornstein MM, Horner K, Jacobs R. Use of cone beam computed tomography in implant dentistry: current concepts, indications and limitations for clinical practice and research. Periodontol 2000. 2017;73:51–72.
Featured image by TEMPURA/E+/GETTY IMAGES PLUS
From Decisions in Dentistry. May 2018;4(5):21-24.


