
Transmission Precautions for Dental Aerosols
Understanding the risk posed by aerosols will help minimize the possibility of infection transmission during dental procedures.
This course was published in the December 2018 issue and expires December 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Explain the risk factors and basic properties of aerosols generated during routine dental procedures.
- Describe ways in which dental aerosols are generated, and the types of pathogens they can harbor.
- List aerosol management techniques to mitigate the risk of cross-contamination to patients and providers.
Respiratory infections — both chronic and acute — contributed to 6 million deaths in 2016, and they are highly communicable.1–3 Many respiratory infections have been linked to the oral microbiota.4–10 Dental procedures that use low- or high-speed handpieces, lasers, electrosurgery units, ultrasonic scalers, air polishers, prophy angles, hand instruments or air/water syringes can create bioaerosols and spatter.9,11 Ultrasonic scalers and high-speed handpieces produce more airborne contamination than any other instrument in dentistry.9,12,13 Inhalation of airborne particles and aerosols produced during dental procedures may cause adverse respiratory health effects and bidirectional disease transmission.8,9,11,12,14–24 While transmission-based precautions can minimize the risk, many may not be routinely practiced.9,12,17,19,21 Oral health professionals should be aware of these invisible dangers in the operatory and follow recommended infection prevention protocols before, during and after patient care.
The oral cavity is inhabited by more than 700 microbial species, including fungi and viruses from the respiratory tract.4,9,25 Temperature, pH, nutrients, host defenses and host genetics contribute to microbial growth.26,27 Common inhabitants of the oral cavity include species of Streptococcus, Actinomyces, Neisseria, Campylobacter, Porphyromonas, Prevotella, Capnocytophaga and Fusobacteria.5,21,26 The oral microenvironment can be altered by factors such as age, tooth eruption or loss, oral disease status, pregnancy and drug use. Several of these changes can alter the virulence and pathogenicity of micro-organisms.27,28
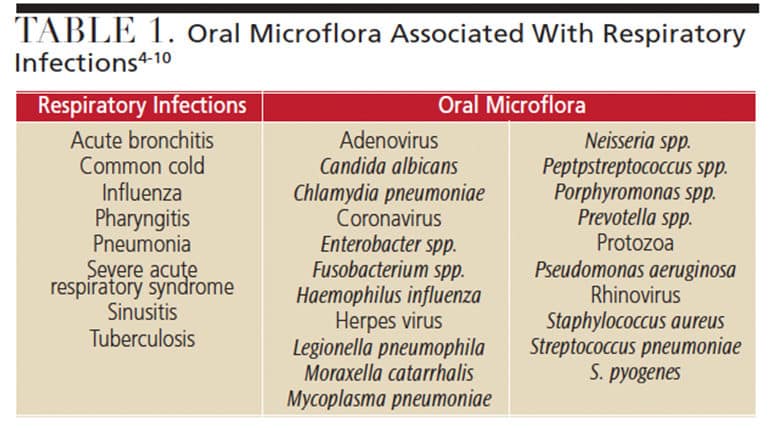
Although direct disease transmission has not been confirmed, oral microflora in healthy and diseased states has been linked to respiratory infections.6–9,29 These include the common cold, influenza, sinusitis, pharyngitis, pneumonia, tuberculosis, and severe acute respiratory syndrome (Table 1).4–10 Furthermore, nasal congestion, headaches and asthmatic episodes have also been triggered by dental bioaerosols.30
Potential routes of infection in dental settings include direct and indirect contact, inhalation and injections/punctures.9,13,31 These routes can be bidirectional, meaning transmission may occur from patient-to-patient, patient-to-clinician, or clinician-to-patient.24 Inhalation of bioaerosols is considered a moderate risk for disease transmission.31 Dental personnel and patients are exposed to tens of thousands of bacteria per cubic meter, and the potential to breathe infective material that is aerosolized during routine procedures is high.13,30 Due to their size, composition and ability to linger, airborne particles pose an increased health risk.14,17,19,31
AEROSOL DIFFERENTIATION
Aerosols are differentiated based on particle size: spatter (> 50 µm), droplet (≤ 50 µm), and droplet nuclei (≤ 10 µm).9,14,18,31 In dental settings, 90% of the aerosols produced are extremely small (< 5 µm).18 Spatter, being the larger particle, will fall until it contacts other objects (e.g., floor, countertop, sink, bracket, table, computer, patient or operator).9,19 Droplets remain suspended in the air until they evaporate, leaving droplet nuclei that contain bacteria related to respiratory infections.9,14 Droplet nuclei can contaminate surfaces in a range of three feet and may remain airborne for 30 minutes to two hours.9,10,13,17,18,30 If inhaled, the droplet nuclei can penetrate deep into the respiratory system.9,14,17–19,31 Furthermore, the susceptibility of developing an infection is influenced by virulence, dose and pathogenicity of the microorganisms, along with the host’s immune response.10
Oral biofilm is resistant to antibiotics, antimicrobial agents and the body’s immune system; therefore, removal of bacteria in dental biofilms is best achieved by physical disruption — yet this very process contributes to aerosol production.5,7 Aerosols, both visible and invisible, are created during surgical and nonsurgical procedures that may include extractions, crown preparations, caries restorations, periodontal therapies, prophylaxes and endodontic treatment.13,22,32 Aerosols consist of water, saliva, blood, debris and microorganisms (e.g., bacteria, fungi, viruses and protozoa), along with their metabolites, such as lipopolysaccharides/endotoxins and other toxins.11,30
Numerous studies have identified specific microbes aerosolized during dental procedures.21,22,33,34 Manarte-Monteiro et al33 determined species of Micrococcus, Staphylococcus, and Streptococcus were aerosolized during endodontic and restorative therapies. Rautemaa et al34 found the most common bacteria aerosolized during restorative treatment using high-speed instruments were viridans streptococci and staphylococci. Pina-Vaz et al22 discovered streptococci were aerosolized during endodontic access. Feres et al21 identified species of Actinomyces, Fusobacterium, Capnocytophaga, and Streptococcus that were aerosolized during periodontal therapy.
Dental unit waterlines have also been shown to harbor microbial pathogens. The specific bacteria likely to cause diseases include Legionella, Pseudomonas, and Nontuberculous mycobacteria.13,35 Dental treatments and aerosolized bacteria from waterlines can cause serious infections and even death.13,35,36
PREVENTION AND REDUCTION
Recommended transmission-based precautions should be incorporated into daily practice to minimize aerosol production and prevent disease transmission from emitted particles. The risks of dental aerosols can be reduced with the use of high-velocity air evacuation and preprocedural antimicrobial mouthrinses, as well as by flushing waterlines at the beginning of the workday and between each patient, wearing personal protective equipment (PPE), and using air purifications systems.9,11–13,22 These recommendations are outlined in the U.S. Centers for Disease Control and Prevention (CDC) Guidelines for Infection Control in Dental Health-Care Settings — 2003.13 In 2016, the CDC published the Summary of Infection Prevention Practices in Dental Settings: Basic Expectations for Safe Care.35 This guide highlights the existing CDC recommendations, provides basic infection prevention principles and recommendations, reaffirms standard precautions as the foundation for preventing transmission of infectious agents, and provides links to the full guidelines and source documents.35
The high-volume evacuator’s (HVE) large diameter (> 8 mm) allows for removal of high volumes of air in a short time, which reduces the amount of bioaerosols by up to 90%.9,11–18 The HVE can be challenging to maneuver simultaneously during instrumentation; therefore, many clinicians find the saliva ejector easier to use and prefer this device for removing excess fluids from the oral cavity.9 From a practice and safety standpoint, it is important to note the opening size of the saliva ejector makes it inadequate for reducing aerosols compared with the HVE or an isolation-and-evacuation device.9,19,22,31
Although the CDC does not offer specific recommendations for using preprocedural antimicrobial mouthrinses to reduce aerosol exposure, studies show their use for 60 seconds significantly reduces the level of oral microorganisms in the aerosols generated during routine dental procedures.9,11,17,18,20
AIR AND WATERLINE PRECAUTIONS
Water in the dental treatment setting should meet U.S. Environmental Protection Agency standards for drinking water (< 500 colony forming units/ml of heterotrophic water bacteria).13,35 To ensure the delivery of safe water, manufacturer instructions for use (IFU) should be followed for the dental unit and any waterline treatment products.13,35 Water-quality monitoring can be conducted by an outside laboratory or internally with in-office testing kits.13,35 The use of independent reservoirs, chemical treatment, filtration, sterile water delivery systems, or combinations of technologies is an additional means for improving and maintaining dental water quality.13,35
The CDC recommends water and air should be discharged for a minimum of 20 to 30 seconds after each patient.13,35 This should be completed for all devices that connect to a waterline and enter patients’ mouths, such as handpieces, ultrasonic scalers and air/water syringes.13,35 Some IFU recommend purging at the beginning of the workday and between patients for two minutes; therefore, providers should follow the IFU specific to their devices. Additionally, the manufacturer advice for testing and maintaining anti-retraction devices (that prevent water/fluid backflow in a waterline) must be followed.13,35
PERSONAL PROTECTIVE EQUIPMENT
Standard precautions, as outlined by the CDC, involve the use of PPE.13,35 Primary PPE includes donning properly fitting gloves and surgical masks, protective eyewear with solid side shields or face shield, and protective clothing/disposable gowns.13,35 This equipment should be worn whenever there is a potential to encounter spray or spatter during patient care, and while disinfecting the treatment area (as noted, bioaerosols remain suspended for 30 minutes to two hours posttreatment).9,10,13,17,18,30,35 Masks and gloves should be changed between patients; moreover, all PPE should be changed if torn, wet or visibly soiled.13,35 If providing care for patients with a known infectious disease, the National Institute for Occupational Safety and Health (NIOSH) requires the wearing of a NIOSH-certified particulate-filter respirator.13 To reduce disease transmission, all PPE must be removed prior to exiting the treatment area.13
VENTILATION MANAGEMENT
Aerosol control in confined, poorly ventilated spaces where the air exchange with filtration cannot be successfully applied presents a challenge.15 Another hurdle is to decrease the indoor concentration of bioaerosols.15 While some indoor air purification techniques aim solely at reducing aerosol concentrations, others are designed to inactivate viable bioaerosols.15 Strong evidence demonstrates ventilation in a practice setting can impact the spread of airborne infections.37
Air cleaning systems — such as high-efficiency particulate air (HEPA) filters, gas filter cartridges and electrostatic filters — assist in purifying the air in and outside of dental operatories.11 The HEPA systems direct air through a series of prefilters, which help to continuously catch airborne microorganisms and retain particles as small as 0.3 µm.11 The four-cylinder gas filter cartridge systems aid in reducing gases and vapors, including mercury, formaldehyde and glutaraldehyde.11 The electrostatically charged post-filters/ion emitters aid in purification by reducing dust, particulates and vapors.11,16,38 Studies show that all three systems have successfully reduced bioaerosols created during dental procedures, most notably during cavity preparations, tooth extractions and use of ultrasonic units.15,38,39
Ultraviolet germicidal irradiation units, commonly employed in hospital operatories and waiting areas, are successful adjunctive means for eliminating aerosols.39 The high spectral emission lamps from these units produce photons that expose microorganisms to a short light wavelength (254 nm) that is lethal to a variety of microorganisms, especially Mycobacterium tuberculosis and Escherichia coli.17,19,39
CONCLUSION
Due to the risk of infectious transmission posed by dental aerosols, transmission-based precautions should be a key element of daily practice. Patients and practitioners are regularly exposed to tens of thousands of aerosols generated during procedures,30 and this exposure increases the potential for respiratory infections.24,30 To ensure patient and provider safety, oral health professionals should abide by the latest CDC guidelines and recommendations. This includes using HVE or an isolation-and-evacuation device, providing preprocedural mouthrinses, maintaining dental unit water quality, and wearing proper PPE.30 To further reduce risks and improve air quality, air cleaning systems can be employed.11,12,15–17,21,37–39 Ultimately, combining multiple methods may be the most effective approach for managing dental aerosols.
REFERENCES
- World Health Organization. The Top 10 Causes of Death. Available at: who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death. Accessed October 26, 2018.
- GBD 2015 LRI Collaborators. Estimates of the global, regional, and national morbidity, mortality, and aetiologies of lower respiratory tract infections in 195 countries: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Infect Dis. 2017;17:1133–1161.
- Murphy SL, Xu J, Kochanek KD, Curtin SC, Arias E. Deaths: final data for 2015. Natl Vital Stat Rep. 2017;66:1–75
- Aas JA, Paster BJ, Stokes LN, Olsen I, Dewhirst FE. Defining the normal bacterial flora of the oral cavity. J Clin Microbiol. 2005;43(11):5721–5732.
- Avila M, Ojcius DM, Yilmaz Ö. The oral microbiota: living with a permanent guest. DNA Cell Biol. 2009;28:405–411.
- Brook I. Microbiology of sinusitis. Proc Am Thorac Soc. 2011;8:90–100.
- Gomes-Filho, IS, Passos JS, Seixas da Cruz S. Respiratory disease and the role of oral bacteria. J Oral Microbiol. 2010;2:5811.
- Scannapieco F. Role of oral bacteria in respiratory infection. J Periodontol. 1999;70:793–801.
- Harrel SK, Molinari J. Aerosols and splatter in dentistry: A brief review of the literature and infection control implications. J Am Dent Assoc. 2004;135:429–437.
- Zemori C, de Soet H, Criellard W, Laheij A. A scoping review on bioaerosols in healthcare and the dental environment. PLoS One. 2017;12:eo178007.
- Hallier C, Williams DW, Potts AJC, Lewis MAO. A pilot study of bioaerosol reduction using an air cleaning system during dental procedures. Br Dent J. 2010;209(8):E14.
- Rao RM, Shenoy N, Shetty V. Determination of efficacy of pre-procedural mouth rinsing in reducing aerosol contamination produced by ultrasonic scalers. Nitte University JHS. 2015;5:52–56.
- Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection control in dental health-care settings — 2003. MMWR Recomm Rep. 2003;52(No. RR-17).
- Atkinson J, Chartier Y, Pessoa-Silva CL, et al. Natural Ventilation for Infection Control in Health-Care Settings. Geneva: World Health Organization; 2009.
- Grinshpun SA, Adhikari A, Honda T, et al. Control of aerosol contaminants in indoor air: Combining the particle concentration reduction with microbial inactivation. Environ Sci Technol. 2007;41:606–612.
- Lee BU, Yermakov M, Grinshpun SA. Removal of fine and ultrafine particles from indoor air environments by the unipolar ion emission. Atmos Environ. 2004;38:4815–4823.
- Veena HR, Mahantesha S, Joseph PA, Patil SR, Patil SH. Dissemination of aerosol and splatter during ultrasonic scaling: A pilot study. J Infect Public Health. 2015;8:260–265.
- James R, Mani A. Dental aerosols: A silent hazard in dentistry! Int J Sci Res. 2016;5:1761–1763.
- Szymanska J. Dental bioaerosol as an occupational hazard in a dentist’s workplace. Ann Agric Environ Med. 2007;14:203–207.
- Thomas MV, Jarboe G, Frazer RQ. Infection control in the dental office. Dent Clin N Am. 2008;52:609–628.
- Feres M, Figueiredo LC, Faveri M, Stewart B, de Vizio W. The effectiveness of a preprocedural mouthrinse containing cetylpyridinium chloride in reducing bacteria in the dental office. J Am Dent Assoc. 2010;141:415–422.
- Pina-Vaz I, Pina-Vaz C, de Carvalho MF, Azevedo A. Evaluating spatter and aerosol contamination during opening of access cavities in endodontics. Rev Clin Pesq Odontol. 2008;4(2):77–83.
- Polednik B. Aerosol and bioaerosol particles in a dental office. Environ Res. 2014;134:405–409.
- Laheij AMGA, Kistler JO, Belibasakis GN, Välimaa H, de Soet JJ. Healthcare-associated viral and bacterial infections in dentistry. J Oral Microbiol. 2012;4.
- Scannapieco F. The oral environment. In Lamont R, Hajishengalis G, Jenkinson H, eds. Oral Microbiology and Immunology. 2nd ed. Washington, DC: ASM Press; 2014:51–76.
- Sowmya Y. A review on the human oral microflora. J Dent Sci. 2016;9:1–5.
- Aas JA, Griffen AL, Dardis SR, et al. Bacteria of dental caries in primary and permanent teeth in children and young adults. J Clin Microbiol. 2008;46:1407–1417.
- Najjar T. Bacterial mouth infections. Medscapes. Available at: emedicine.medscape.com/article/1081424-overview. Updated September 26, 2017. Accessed October 26, 2018.
- Paju S, Scannapieco FA. Oral biofilms, periodontitis, and pulmonary infections. Oral Dis. 2007;13:508–512.
- Dutil S, Meriaux A, de Latremoille MC, Lazure L, Barbeau J, Duchaine C. Measurement of airborne bacteria and endotoxin generated during dental cleaning. J Occup Environ Hyg. 2009;6:121–130.
- Sawhney A, Venugopal S, Babu G, et al. Aerosols how dangerous they are in clinical practice. J Clin Diagn Res. 2015;9:52–57.
- Yamada H, Ishihama K, Yasuda K, Hasumi-Nakayama Y, Shimoji S, Furusawa K. Aerial dispersal of blood-contaminated aerosols during dental procedures. Quintessence Int. 2011;42:399–405.
- Manarte-Monteiro P, Carvalho A, Pina C, Oliveira H, Manso MC. Air quality assessment during dental practice: Aerosols bacterial counts in an university clinic. Rev Port Estomatol Med Dent Cir Maxilofac. 2013;54:2–7.
- Rautemaa R, Nordberg A, Wuolijoki-Saaristo K, Meurman JH. Bacterial aerosols in dental practice: a potential hospital infection problem? J Hosp Infect. 2006;4:76–81.
- Summary of Infection Prevention Practices in Dental Settings: Basic Expectations for Safe Care. Atlanta: Centers for Disease Control and Prevention; October 2016.
- Ricci ML, Fontana S, Pinci F, et al. Pneumonia associated with a dental unit waterline. Lancet. 2012;379:684.
- Li Y, Leung GM, Tang JW, et al. Role of ventilation in airborne transmission of infectious agents in the built environment: a multidisciplinary systematic review. Indoor Air. 2007;17:2–18.
- Martin SB, Moyer ES. Electrostatic respirator filter media: filter efficiency and most penetrating particle size effects. Appl Occup Environ Hyg. 2000;15:609–617.
- Noakes CJ, Fletcher LA, Beggs CB, Sleigh PA, Kerr KG. Development of a numerical model to simulate the biological inactivation of airborne microorganisms in the presence of ultraviolet light. J Aerosol Sci. 2004;35:489–507.
Featured image by NIK LEBOWSKI/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. December 2018;4(12):30—32,35.





[…] never use water) so these should be more than enough for us. A great article on dental aerosols is HERE. (Note that there is A LOT on the web about dental aerosols when one is using water, but very […]
[…] https://decisionsindentistry.com/article/transmission-precautions-for-dental-aerosols/ (Bauman, J Hospital Infection, 2006) […]