
Caring for Individuals With Anxiety Disorders
Knowledge and preparation will facilitate effective — and ongoing — oral health care for this patient group.
This course was published in the May 2018 issue and expires May 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify various anxiety disorders and clinical approaches to therapy.
- Discuss the oral health implications of anxiety disorders and their treatment.
- Describe strategies for effectively caring for dental patients presenting with anxiety disorders.
Although anxiety disorders are among the most common mental disorders, affecting approximately 40 million American adults.1,2 only 36.9% of individuals with anxiety are actively receiving treatment. Women and non-Hispanic whites are most likely to experience an anxiety disorder.1 Among adults, the average age of onset is 21.2 Research indicates that 25.1% of teenagers ages 13 to 18 have an anxiety disorder; among the pediatric group, 11.5 years is the average age of onset.3,4
Pathologic anxiety disorders present when anxious responses are excessive, uncontrollable, lack a stimulus, and result in behavioral and cognitive changes.5,6 Stress, systemic illness, psychiatric disorders, genetics, environment, and a combination of psychological and biologic processes may be the cause.3,4,7,8 Patients with anxiety disorders are likely to present in the dental office, and oral health professionals are advised to prepare adequately in order to provide treatment in a safe and effective manner.
The most common anxiety disorders are panic disorder, obsessive-compulsive disorder (OCD), post-traumatic stress disorder (PTSD), and phobias, such as generalized anxiety disorder (GAD) and social anxiety disorder (SAD).3,7,9
Panic disorder results in sudden feelings of fear that lead to panic attacks.7,9 Individuals experiencing a panic attack might exhibit chest pain, heart palpitations, shortness of breath, dizziness, upset stomach, feelings of disconnect, and fear of death.7,9 Panic disorders can create feelings of shame, self-consciousness and fear of another attack.7–9 When patients fail to seek treatment early, panic disorders may cause them to avoid places where attacks have occurred.6–8
Individuals with OCD exhibit obsessions and compulsions that are difficult to control.9–11 If their compulsions are not performed numerous times a day in a specific way, they experience anxiety that often interferes with daily life.9–12
Patients with PTSD experience feelings of distress brought on by a previous traumatic event.6,9,13 When healthy individuals are faced with situations that are threatening or can cause harm, it triggers a fight-or-flight response.14 In contrast, those with PTSD experience the activation of this reaction in the absence of danger.14 Symptoms are divided into three categories: reexperiencing, avoidance or hyperarousal symptoms.14 Reexperiencing symptoms include nightmares, flashbacks and/or frightening thoughts.6,13,14 Avoidance symptoms involve isolation from places, events or objects that remind the individual of the traumatic experience.6,13,14 In addition, feelings of numbness, guilt, depression, worry, loss of interest in activities once enjoyed, and difficulty remembering the traumatic event are common.9,13,14 Becoming easily startled or scared, feeling tense and angry, and/or difficulty sleeping are symptoms of hyperarousal.6,9,13,14
Phobias are characterized by irrational fear.9 Patients with GAD have severe, chronic and inflated worry about events in daily life.7–9,15 Although most individuals realize their reactions are not proportionate to the situation, they are unable to control their anxiety.8 In addition, GAD may result in insomnia, difficulty concentrating, being easily startled, fatigue, headaches, muscle tension/aches, difficulty swallowing, trembling, twitching, irritability, sweating, nausea, lightheadedness, frequent urination, hot flashes and breathlessness.7,8 Manifesting as fear of public humiliation, SAD produces symptoms that include feeling self-conscious, being embarrassed around others, and worrying before events. Affected individuals may also have difficulty in communicating, and experience nausea, trembling, sweating and blushing.7–9
treatment modalities
Treatment of anxiety disorders includes psychological, behavioral and pharmacological modalities.5,8,9 While they do not provide a cure, medications can be effective in controlling symptoms.8 The most common medications are antidepressants, antianxiety drugs and beta-blockers.8,9,16
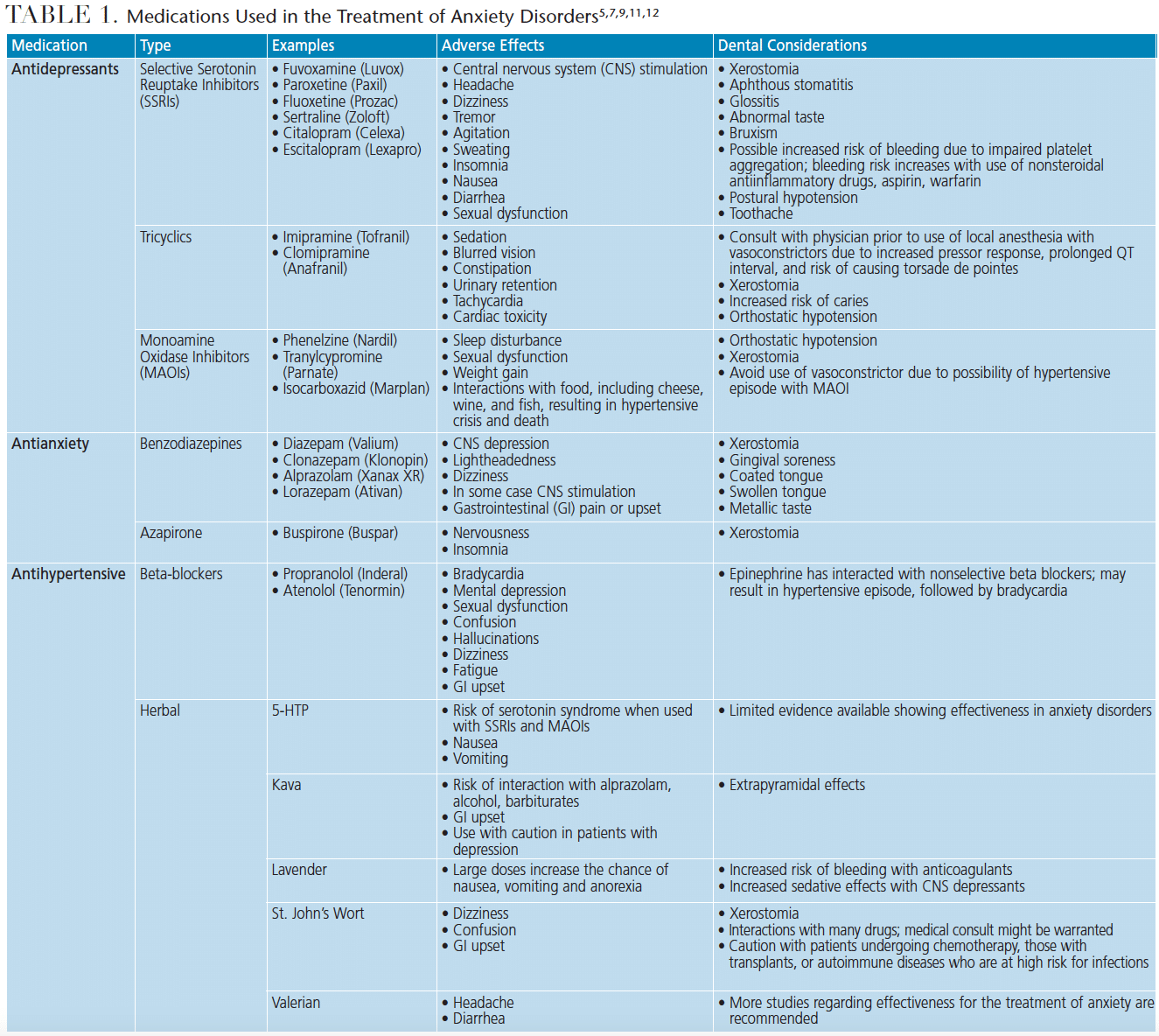
Table 1 lists the medications and herbal supplements commonly used to treat anxiety disorders, their adverse reactions, and associated dental considerations. Patients taking selective serotonin reuptake inhibitors, tricyclic antidepressants (TCAs), monoamine oxidase inhibitors (MAOIs), or benzodiazepines are at risk for xerostomia, which, in turn, increases caries risk.17,18 These medications may also interact with dental anesthetics. A medical consultation may be prudent for patients taking TCAs when the use of a vasoconstrictor is warranted, due to an increased pressor response, prolonged QT interval, and the risk of torsade de pointes.17,18 Furthermore, vasoconstrictors should be avoided in patients taking MAOIs due to an increased risk of hypertension, gastrointestinal upset, headache, dizziness, insomnia, central nervous system stimulation and tremors.17,18 Opioids should not be prescribed without a medical consultation, as some of these medications may intensify the opioid’s effects. Herbal supplements are often used by patients to control anxiety; they may be self-prescribing these supplements, and there may be interactions with prescribed medications for other systemic conditions or medications used in the dental office.
ORAL HEALTH IMPLICATIONS
Compared to the general population, patients with anxiety disorders are more likely to have unmet dental needs, are less likely to visit the dental office regularly, and tend to ignore oral conditions.19–22 They are also more likely to seek care in a hospital emergency department due to pain caused by caries, periodontal lesions, periapical lesions and/or oral cellulitis.21 Poor oral health among patients with anxiety disorders is linked to lifestyle choices and the effects of medications used to treat these conditions.20,22 This population may be more susceptible to caries, untreated restorative needs, stomatitis, glossitis, gingivitis, gingival recession, abrasion, periodontal disease, medication-related xerostomia, soft tissue lesions, temporomandibular joint disorders, and increased levels of biofilm and calculus.16,19–21,23
Oral health professionals are advised to approach patients experiencing anxiety disorders with a supportive, nonjudgmental attitude.16,24,25 Clinicians should verify patients’ medication usage to avoid drug interactions and note any oral symptoms.18 Selective serotonin reuptake inhibitors inhibit isoenzymes that metabolize codeine, erythromycin and carbamazepine.16 Antihistamines, muscle relaxants and opioid analgesics heighten the tranquilizing effects of benzodiazepines.16 Additionally, hydrocodone may induce symptoms of a panic attack.
The use of the Caries Management By Risk Assessment protocol is appropriate when treating patients with anxiety disorders. When a patient presents with a moderate to high caries risk, the dental team should adhere to the American Dental Association’s (ADA) clinical recommendations for radiographs and fluoride treatments. These state that children and adolescents at increased caries risk should have posterior bitewing exams at six to 12-month intervals, and adults at six to 18-month intervals.26 Patients at an increased risk of caries should receive professional 2.26% fluoride varnish applications every three to six months.27 Additionally, the ADA recommends that high caries risk patients use a 0.09% fluoride rinse weekly or a 0.5% fluoride gel or paste twice daily.27
Considering the increased risk for periodontal disease and caries, patients with anxiety disorders require thorough oral hygiene instructions.16,20,28 Oral education aids, such as brochures, pictures, models and software programs, can be helpful tools.28 Artificial saliva products should be considered to reduce the effects of medication-induced xerostomia.16,20
When local anesthesia is used, special precautions are indicated.16 Anesthetic selection should be based on the procedure, duration of anesthesia required, and needs and/or preferences of the patient.24 As an alternative to local anesthesia, topical sprays, rinses or subgingival gels may be used; nitrous oxide sedation might also be useful.24 For more severe cases of anxiety or in the event of extensive dental needs, intravenous conscious sedation might be indicated.24,25
In order to facilitate the comfort of patients with anxiety disorders, the dental team should help them feel in control of their appointments.24 Brief appointments scheduled early in the morning are helpful.28 Allowing patients to take breaks and sit up when needed provides opportunities to relax during treatment.16,24,25 Positive reinforcement can strengthen patients’ morale and encourage them to return for additional care.25 Oral health professionals are advised to use open communication to address patients’ values and concerns about treatment in order to achieve and maintain oral and overall health.24,25,28 Motivational interviewing might prove helpful in uncovering patients’ resistance to oral health behavior modification and provide the impetus needed to make positive changes.28
Implementing stress-reduction strategies, such as deep breathing and focusing on a particular spot, may help reduce anxiety.24,25,28 Oral health professionals can suggest that patients visualize themselves in a scene using all five senses, or listen to music throughout the appointment.25,28 Providers should use a calm voice and be conversational.24,25 In addition, various tools — such as noise-cancelling headphones, pillows, blankets or neck wraps — may be helpful. Aromatherapy with essential oils has been shown to reduce moderate anxiety due to its ability to reduce salivary and serum cortisol, increase blood flow, and decrease systolic blood pressure.25 Patients should be encouraged to share the stress-reduction protocols that work best for them.
MEDICAL EMERGENCIES
The risk of medical emergencies may be elevated when treating this patient population, and this underscores the importance of the office being prepared to react in an appropriate manner. Taking a thorough health history can help clinicians anticipate a medical emergency.29 Vital signs should be recorded for all patients, as they could provide early indication a patient is experiencing anxiety. Past dental experiences, including sights, sounds and smells, may induce a panic attack in patients with anxiety disorders.25,28 If a patient begins to exhibit the signs and symptoms of a panic attack, treatment should cease until the patient has calmed down and is ready to proceed. Early recognition of these signs might allow providers to reassure the patient so that treatment may be completed.28 If a patient is unable to continue, emergency medical services or the assistance of a family member — especially in providing transportation for the patient — may be necessary. Calling the patient that evening to check in is a helpful gesture that may encourage the patient to return to complete treatment.
In the case of a more severe panic attack, syncope may occur. If so, medical emergency management protocols call for taking vital signs and checking airway, breathing and circulation.29 The patient should be placed in the supine position and should regain consciousness within 60 seconds.29
CONCLUSION
With knowledge and preparation, dental teams can effectively treat patients with anxiety disorders, thus increasing the likelihood they will return for regular care. If providers and patients work together, individuals with anxiety disorders can have positive dental experiences that will help support optimal oral health.
References
- National Institute of Mental Health. Any Anxiety Disorder. Available at: nimh.nih.gov/health/statistics/prevalence/any-anxiety-disorder-among-adults.shtml. Accessed April 12, 2018.
- National Institute of Mental Health. Post by Former NIMH Director Thomas Insel: Mental Health Awareness Month: By the Numbers. Available at: nimh.nih.gov/about/directors/thomas-insel/blog/2015/mental-health-awareness-month-by-the-numbers.shtml. Accessed April 12, 2018.
- Anxiety and Depression Association of America. Facts and Statistics. Available at: adaa.org/about-adaa/press-room/facts-statistics. Accessed April 12, 2018.
- de Lijster JM, Dierckx B, Utens EMWJ, et al. The age of onset of anxiety disorder: a meta-analysis. Can Psychiatr Assoc J. 2017;62:237–246.
- Little JW, Falace DA, Miller CS, Rhodus NL. Dental Management of the Medically Compromised Patient. 9th ed. St. Louis: Elsevier Mosby; 2013:544–560.
- Little JW. Anxiety disorders: dental implications. Gen Dent. 2002;51:562–568.
- Medscape. Anxiety Disorders. Available at: emedicine.medscape.com/article/286227-overview. Accessed April 12, 2018.
- National Institute of Mental Health. Anxiety Disorders. Available at: nimh.nih.gov/health/topics/anxiety-disorders/index.shtml. Accessed April 12, 2018.
- National Alliance on Mental Illness. Anxiety Disorders. Available at: nami.org/Learn-More/Mental-Health-Conditions/Anxiety-Disorders. Accessed April 12, 2018.
- Anxiety and Depression Association of America. Understand the Facts: Obsessive-Compulsive Disorder. Available at: adaa.org/understanding-anxiety/obsessive-compulsive-disorder-ocd. Accessed on April 12, 2018.
- Mayo Clinic. Obsessive Compulsive Disorder. Available at: mayoclinic.org/diseases-conditions/obsessive-compulsive-disorder/symptoms-causes/syc-20354432. Accessed April 12, 2018.
- National Institute of Mental Health. Obsessive-Compulsive Disorder. Available at: nimh.nih.gov/health/topics/obsessive-compulsive-disorder-ocd/index.shtml. Accessed April 12, 2018.
- Anxiety and Depression Association of America. Understand the Facts: Posttraumatic Stress Disorder. Available at: adaa.org/understanding-anxiety/posttraumatic-stress-disorder-ptsd/symptoms. Accessed April 12, 2018.
- National Institute of Mental Health. Post-Traumatic Stress Disorder. Available at: nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd/index.shtml. Accessed April 12, 2018.
- Anxiety and Depression Association of America. Understanding the Facts: Generalized Anxiety Disorder. Available at: adaa.org/understanding-anxiety/generalized-anxiety-disorder-gad. Accessed April 12, 2018.
- Friedlander AH, Marder MD, Sung EC, Child JS. Panic disorder: psychopathology, medical management, and dental implications. J Am Dent Assoc. 2004;135:771–778.
- Wynn, RL, Meiller, TF, Crossley, HL. Drug Information Handbook for Dentistry. 23rd ed. Hudson, Ohio: Lexi-Comp Inc; 2017.
- Haveles EB. Applied Pharmacology for the Dental Hygienist. 7th ed. St. Louis: Elsevier Mosby; 2015.
- Heaton LJ, Mancl LA, Grembowski D, Armfield JM, Milgrom P. Unmet dental needs in community-dwelling adults with mental illness: Results from the 2007 medical expenditure panel survey. J Am Dent Assoc. 2013;144:16–23.
- Kisley S. No mental health without oral health. Can J Psychiatry. 2016;61:277–282.
- Nalliah RP, Da Silva JD, Allareddy V. The characteristics of hospital emergency department visits made by people with mental health conditions who had dental problems. J Am Dent Assoc. 2013;144:617–624.
- Edward KL, Felstead B, Mahoney AM. Hospitalized mental health patients and oral health. J Psychiatr Ment Health Nurs. 2012;19:419–425.
- Gatchel RJ, Garofalo JP, Ellis E, Holt C. Major psychological disorders in acute and chronic TMD: An initial examination. J Am Dent Assoc. 1996;127:1365–1370.
- Byrd E. Strategies for dental hygienists who treat patients with dental anxiety or phobia. Available at: dentistryiq.com/articles/2016/10/strategies-for-hygienists-who-treat-patients-with-dental-anxiety-or-phobia.html. Accessed April 12, 1018.
- Appukuttan DP. Strategies to manage patients with dental anxiety and dental phobia: A literature review. Clin Cosmet Investig Dent. 2016;8:35–50.
- American Dental Association. Dental radiographic examinations: recommendations for patient selection and limiting radiation exposure. Available at: ada.org/~/media/ADA/…/FIles/Dental_Radiographic_Examinations_2012.pdf. Accessed April 12, 2018.
- Weyant, RJ, Tracy, SL, Anselmo, T, et al. Topical fluoride for caries prevention: Executive summary of the updated clinical recommendations and supporting systematic review. J Am Dent Assoc. 2013;144:1279–1291.
- Sefo DL, Stefanou L. Quelling dental anxiety. Dimensions of Dental Hygiene. 2014;12:70–73.
- Reed, K.L. Basic management of medical emergencies: Recognizing a patient’s distress. J Am Dent Assoc. 2010;141(Suppl 1):20–24.
From Decisions in Dentistry. May 2018;4(5):53-56.




