Acquired Silent Sinus Syndrome Presents a Challenge
This case report highlights the critical role of oral health professionals in recognizing this rare but impactful condition.
This course was published in the July/August 2025 issue and expires August 2028. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
AGD Subject Code: 149
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the key clinical and radiographic features of silent sinus syndrome (SSS) relevant to dental practice.
- Discuss the implications of SSS on dental treatment planning, including orthodontic, surgical, and implant considerations.
- Recognize the importance of early detection and appropriate referral to improve functional and esthetic outcomes in patients with SSS.
Silent sinus syndrome (SSS) is a condition in which one eye gradually sinks backward (enophthalmos) and downward (hypoglobus) on one side of the face. First developing without symptoms, SSS typically occurs in people with no history of facial trauma or sinus surgery.1 This syndrome involves architectural bony changes such as inward bowing of antral walls and maxillary sinus atelectasis, as well as posterior retraction2 and occasional opacification.3 These resultant structural changes impact sinonasal, orbital, and surrounding anatomy in close proximity to the oral cavity, often requiring alterations to dental treatment. Such findings are often identified with an advanced imaging exam including cone-beam computed tomography (CBCT), magnetic resonance imaging (MRI), or multidetector CT (MDCT) scans.
Radiographic imaging sensitive to SSS detection can simplify diagnosis and treatment planning. Due to the scarcity in identification and reporting, many oral health professionals may be unaware of this condition and thus less likely to recognize and understand its impact. Although SSS is well documented in the otolaryngology, ophthalmology, and radiology literature, its discussion within dental literature remains sparse. In addition, pediatric cases of SSS are rarely reported.
Recently, case reports have discussed pediatric SSS diagnosed through MRI and MDCT scans that were initially conducted to evaluate unrelated diseases.4,5 Radiographic findings of maxillary hypoplasia and opacification present similarly in pediatric and adult populations. In children, symptoms may range from asymptomatic or sinusitis and headache.1,6 Once considered idiopathic in etiology, recent hypotheses suggests that craniofacial growth and variation in sinonasal structures may make children more susceptible to maxillary ostium obstruction and SSS.1,6
A retrospective study identified pediatric SSS in patients as young as 3, though no correlation was found between patients’ age and their orbital presentation such as hypoglobus, enophthalmos, diplopia, and dystopia.5 A recent literature review on cases of pediatric SSS further suggested that surgical interventions have led to promising outcomes in cases of maxillary sinus hypoplasia and facial asymmetry.6
This case report highlights the importance of recognizing SSS from a dental perspective and presents a unique incidence of a teenage patient with advanced SSS in conjunction with an impacted maxillary canine. This patient was monitored closely over the course of several years while she was treated at Midwestern University College of Dental Medicine, Arizona.
Case Report
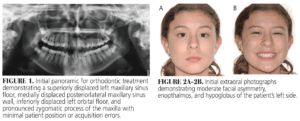
This study received exemption from the Institutional Review Board of Midwestern University College of Dental Medicine, Arizona. A 15-year-old adolescent girl presented to the orthodontic clinic at Midwestern University College of Dental Medicine, Arizona, with a request for an orthodontic consultation. The patient reported no known allergies, denied any history of nasal or sinus disease, and had no known medical history. The clinical examination revealed a Class I malocclusion with moderate overjet, deep overbite, minimal arch length discrepancies, maxillary midline coincident with her face, mandibular right midline deviation, a full complement of permanent teeth with retained primary #H, and near horizontally impacted #11 with the crown positioned at the root apex of #10 (Figure 1).
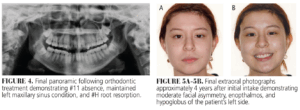
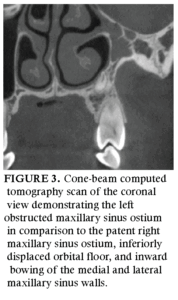 Extraoral photographs reveal moderate facial asymmetry with apparent enopthalmos and hypoglobus of the affected side (Figure 2). As part of the orthodontic workup, a 6-by-6-cm, 0.12-mm-resolution CBCT was captured to evaluate the position of #11. The CBCT was requested to identify anatomic structures for possible surgical exposure with bracket and chain of #11 for orthodontic extrusion. The CBCT report by a board-certified oral and maxillofacial radiologist identified left hypoplasia of the maxillary sinus with complete opacification and obstruction of ostium; lateral retraction of uncinate process, left middle turbinate, and medial sinus wall; enlargement of the middle meatus and posterior retraction of anterior wall of the sinus; and left orbital floor inferior retraction into the sinus lumen (Figure 3). The patient was unaware of her facial asymmetry and therefore did not recall noticing any esthetic changes over time.
Extraoral photographs reveal moderate facial asymmetry with apparent enopthalmos and hypoglobus of the affected side (Figure 2). As part of the orthodontic workup, a 6-by-6-cm, 0.12-mm-resolution CBCT was captured to evaluate the position of #11. The CBCT was requested to identify anatomic structures for possible surgical exposure with bracket and chain of #11 for orthodontic extrusion. The CBCT report by a board-certified oral and maxillofacial radiologist identified left hypoplasia of the maxillary sinus with complete opacification and obstruction of ostium; lateral retraction of uncinate process, left middle turbinate, and medial sinus wall; enlargement of the middle meatus and posterior retraction of anterior wall of the sinus; and left orbital floor inferior retraction into the sinus lumen (Figure 3). The patient was unaware of her facial asymmetry and therefore did not recall noticing any esthetic changes over time.
Due to the collapse and opacification of the left maxillary sinus, exposure of the impacted canine and predictability of orthodontic extrusion into the arch were deemed poor. The decision was made to extract the impacted tooth and maintain the retained primary #H for as long as possible. Retaining the primary canine helped preserve the alveolar bone’s height and width for potential future implant placement. An evaluation by an ear, nose and throat (ENT) specialist confirmed the diagnosis of SSS; however, the patient and her parent declined surgical correction of the ostiomeatal obstruction.
The impacted canine was extracted 6 weeks prior to the placement of fixed orthodontic appliances by an oral surgeon. The primary canine was not included in the fixed orthodontic appliance and remained in the arch throughout treatment and remains today. Treatment progressed uneventfully and appliances were removed after 4 years. Treatment time was prolonged due to pandemic shutdown and scheduling conflicts. The patient’s third molars were uneventfully removed 9 months after appliance removal. She remains in nighttime Hawley retainers and #H is intact with minimal apical root structure remaining (Figures 4 and 5).
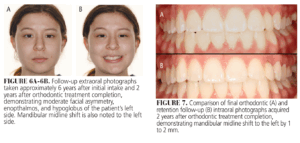
A 2-year follow up retention appointment afforded the opportunity to capture subsequent photographs. Figure 6 demonstrates minimal ocular height changes; however, there is apparent change in the mandibular midline. The patient reports cooperation with removable Hawley retainer wear at 18 hours per day. The mandibular midline has shifted to the patient’s left approximately 1 to 2 mm (Figure 7).
The occlusion, similarly, presents with changes, most noticeably an increased buccal overjet in the left posterior segment. The patient is seeking ENT surgery in the near future for correction of the airway to allow regular nasal breathing. She did not say whether she will also have the maxillary implosion corrected. The patient will continue to be closely monitored via retention and hygiene appointments.
The retained maxillary #H is still present and may soon require implant replacement. The patient is pleased with the results and has been advised to reduce her retainer wear to approximately 8 hours per day.
Discussion
SSS, known to most ophthalmologists and otolaryngologists, remains an uncommon entity in the dental community. A systematic review revealed that the most common diagnostic criteria were enopthalmus with maxillary atelectasis,7 simultaneously exhibiting hypoglobus, and the absence of sinus disease.8 Opacification, although not as commonly included as a diagnostic criterion, was a frequent radiographic finding.9
The precise pathophysiology of SSS remains a subject of ongoing discussion; however, three common theories explain its pathogenesis. The first and most commonly accepted theory suggests that the obstruction of the maxillary sinus ostium leads to sinus hypoventilation with resultant atelectasis due to negative sinus pressure and the accumulation of secretion.2,10-12 The maxillary sinus normally drains and ventilates into the middle nasal meatus of the nasal cavity via an ostium with an opening ranging from 1 to 13 mm in width.10
Obstructions, such as thickened mucus, mucocele, nasal polyps, or inflamed mucosa, can partially or completely block this ostium. Over time, the lack of adequate aeration in the maxillary sinus causes resorption of gas into the capillaries, resulting in the development of negative pressure from within the antrum.13 This subatmospheric pressure induces bone remodeling, thinning of the maxillary walls, and downward displacement of the orbital floor, causing maxillary sinus collapse and orbital volume to grow.14 The loss of support from the orbital floor is thought to directly contribute to hypoglobus and enophthalmos, the most common clinically visible signs in patients with SSS.2,10
A second theory highlights the role of a mechanical aspiration phenomenon, in which the negative pressure is created by masticatory muscle movements.10,15 It is hypothesized that the subatomospheric pressure in the sinus not only induces collapse of the sinus wall but also facilitates herniation of orbital fat into the pterygopalatine fossa through a defect in the orbital floor, such as a previous orbital floor fracture.10,15 This aspiration phenomenon is believed to directly contribute to the appearance of enophthalmos.10,15
The third theory, inflammatory erosion, proposes that osteopenia, as a result of inflammatory processes, leads to maxillary bone loss and erosion of the orbital floor.2 Chronic inflammation can inhibit synthesis of osteoblasts and collagen via cytokines produced by inflammatory cells, leading to sinus wall degradation and osteopenia.16,17 The following report is focused on a pediatric case in which osteopenic conditions are rare. This theory has been explored more in adults.
All of these findings support the concept that SSS is acquired and not developmental. Further, SSS should be differentiated from stage III chronic maxillary atelectasis (CMA).18 While both entities present with similar clinical and radiographic findings, nasal and sinus symptoms are distinguishing characteristics of CMA in adults.19 The role of sinonasal symptoms in early stage CMA tends to subside as it advances to stage III CMA,18,19 in which a negative history of sinonasal symptoms could be a natural progression of the same entity. It is hypothesized that stage III CMA may be the final pathway that brings about the asymptomatic SSS.20,21
The age of diagnosis in this case report was age 15, which differs from the previously reported average age of 30s to 50s.14,22 Recent reports support a revised average age. In a study of 83 pediatric patients presenting with SSS, the average age was 12.5 years.5 Pediatric populations frequently have a higher rate of upper respiratory infections, chronic rhinorrhea, adenoiditis, allergic rhinitis, and cough than adults. These common childhood afflictions typically subside with growth and development, therefore, a history of sinonasal symptoms should not exclude SSS for the pediatric population.5 Some consider SSS a subgroup of CMA III,19,20 and while both entities are described in the literature, this case exemplifies SSS due to a lack of chronic sinusitis or reported sinus symptoms.
The spontaneous nature and progression of SSS can be seen over the course of several weeks to months.19 This case report is unusual in the fact that early diagnosis and treatment may have impacted the patient’s functional and esthetic development and may have benefitted from early surgical intervention to restore sinus function, relieve negative pressures causing sinus collapse, and reverse or prevent further sinus opacification. Additionally, the condition was not self-reported and was only diagnosed via an incidental finding on a CBCT, an evaluation method used routinely in both general dentistry and dental specialties.
A dental-related implication to consider is referred pain to maxillary teeth due to the proximity of the maxillary sinus, which can result in misdiagnosis of pulpitis or dental-related infection. Additional considerations include reduction of bone height and sinus volume, which adds a significant complication to implant planning, as placement of dental implants may require sinus augmentation. Requisite sinus augmentation prior to implant planning typically mandates resolution of severe sinus pathology.
Malocclusions can also result from changes in boney structures with ensuing facial asymmetry. Maxillary canines are the second most commonly impacted teeth, and changes in the bony structures supporting the sinus walls may interfere with their normal eruption path.23 Removing boney obstacles and clearing the path for eruption may reduce the need for orthodontic correction and/or surgical exposure. The general dentist who is aware of the potential differential diagnosis of SSS when observing this complication could refer the individual for the appropriate care resulting in proper diagnosis and subsequent treatment.
SSS treatment aims to restore normal airflow in the maxillary sinus while correcting any changes in facial structure. Traditionally, this is done by clearing the blocked sinus drainage pathway using minimally invasive techniques, and if needed, repairing sunken eye appearance with implants in the orbital floor or medial wall.24,25
More recently, balloon sinuplasty has been a successful procedure to restore sinus volume. In this procedure, a small balloon is guided into the sinus opening and inflated, helping to reopen the sinus and relieve symptoms.26 The lack of consensus on the ideal treatment for SSS has made the single-stage surgery to restore airflow and monitor for resolution of secondary symptoms more popular. However, multistage procedures may be appropriate.3 Regardless of which path is chosen, early detection and intervention support the successful treatment of SSS.
Role of the Oral Health Professional
SSS affects dental patients and their available treatment options. As such, oral health professionals should be trained to identify such cases via clinical and radiographic presentation in both adult and pediatric populations. Periapical and panoramic radiographs are routine diagnostic tools in all patient care and provide valuable insights into sinus health. However, CBCT is the most common imaging modality that provides a definitive diagnosis of SSS.5 This technology assists oral health professionals in early diagnosis and intervention in pediatric patients, reducing the risk of disease progression and long-term complications. Increased use of CBCT in general dental practices should result in an increased diagnosis of uncommon clinical findings such as SSS.
While SSS can be identified through clinical presentation, the final diagnosis must be confirmed radiographically. Furthermore, recognizing SSS in patients with asymmetrical facial features encourages proper diagnosis and early corrective treatments for esthetic concerns. This is important if surgical procedures are planned or required in areas near the sinus walls. Additionally, identifying SSS in edentulous or partially edentulous patients is crucial for evaluating restorative options and determining implant eligibility. This allows for preemptive management of the sinus and alveolar bone to ensure optimal long-term results. Ultimately, more research is needed with long-term follow-up to assess the impact on dental health and treatment options as well as the ability to educate patients and provide appropriate referrals.
Conclusion
This case study highlights the need to raise awareness of SSS among oral health professionals. Due to its subtle presentation and slow progression, SSS frequently remains unrecognized in a dental setting. With the growing use of CBCT, a greater number of uncommon findings are likely to be identified. A comprehensive understanding of its clinical features and radiographic findings enables dentists to incorporate screening into patient examinations.
References
- Soparkar CNS, Patrinely JR, Cuaycong MJ, et al. The silent sinus syndrome: a cause of spontaneous enophthalmos. Ophthalmology. 1994;101:772-778.
- Manila NG, Tahmasbi Arashlow M, Ehlers S, Liang H, Nair MK. Cone-beam computed tomographic imaging of silent sinus syndrome: A case series and a literature review. Imaging Sci Dent. 2020;50:365-371.
- Mantsopoulos K, Thimsen V, Karkos P, Sievert M, Iro H, Constantinidis J. Silent sinus syndrome: Reduction of surgical invasiveness in an underdiagnosed clinical entity. Am J Otolaryngol.2022;43:103541.
- Farneti P, Sciarretta V, Macrì G, Piccin O, Pasquini E. Silent sinus syndrome and maxillary sinus atelectasis in children. Int J Pediatr Otorhinolaryngol.2017;98:150-157.
- Freiser ME, McCoy J, Shaffer AD, Stapleton AL. Silent sinus syndrome in children. Int J Pediatr Otorhinolaryngol. 2020;134:110034.
- Chernov ES, Ghanem A, Gonzales Parilla L, Carroll WW. Pediatric silent sinus syndrome: a case report and literature review. Ann Otol Rhinol Laryngol. 2025;134:284-290.
- Rosso C, Saibene AM, Felisati G, Pipolo C. Silent sinus syndrome: systematic review and proposal of definition, diagnosis and management. Acta Otorhinolaryngol Ital. 2022;42:305-316.
- Illner A, Davidson HC, Harnsberger HR, Hoffman J. The silent sinus syndrome: clinical and radiographic findings. AJR Am J Roentgenol. 2002;178:503-506.
- Gaudino S, Di Lella GM, Piludu F, et al. CT and MRI diagnosis of silent sinus syndrome. Radiol Med. 2013;118:265-275.
- Cobb ARM, Murthy R, Cousin GCS, et al. Silent sinus syndrome. Br J Oral Maxillofac Surg. 2012;50:e81-e85.
- Blackwell KE, Goldberg RA, Calcaterra TC. Atelectasis of the maxillary sinus with enophthalmos and midface depression. Ann Otol Rhinol Laryngol. 1993;102:429-432.
- Davidson JK, Soparkar CN, Williams JB, Patrinely JR. Negative sinus pressure and normal predisease imaging in silent sinus syndrome. Arch Ophthalmol. 1999;117:1653-1654.
- Raveggi E, Sobrero F, Gerbino G. Patient specific implants for orbital reconstruction in the treatment of silent sinus syndrome: two case reports. J Pers Med. 2023;13:578.
- Facon F, Eloy P, Brasseur P, Collet S, Bertrand B. The silent sinus syndrome. Eur Arch Otorhinolaryngol. 2006;263:567-571.
- Baujat MD, Bertrand P, Derbez MD, et al. Silent sinus syndrome: a mechanical theory. Orbit. 2006;25:145-148.
- Stashenko P, Dewhirst FE, Rooney ML, Desjardins LA, Heeley JD. Interleukin‐1β is a potent inhibitor of bone formation in vitro. J Bone Miner Res. 1987;2:559-565.
- Amano S, Hanazawa S, Hirose K, Ohmori Y, Kitano S. Stimulatory effect on bone resorption of interleukin-1-like cytokine produced by an osteoblast-rich population of mouse calvarial cells. Calcif Tissue Int. 1988;43:88-91.
- Salman S, Weber AL, Kass ES, Rubin PAD, Montgomery WW. Chronic maxillary atelectasis. Ann Otol Rhinol Laryngol. 1997;106:109-116.
- Vander Meer JB, Harris G, Toohill RJ, Smith TL. The silent sinus syndrome: a case series and literature review. Laryngoscope. 2001;111:975-978.
- Brandt MG, Wright ED. The silent sinus syndrome is a form of chronic maxillary atelectasis: a systematic review of all reported cases. Am J Rhinol. 2008;22:68-73.
- Salman S, Kass ES, Montgomery WW. Chronic maxillary atelectasis in a child. Ann Otol Rhinol Laryngol. 1998;107:623-625.
- Rose GE, Sandy C, Hallberg L, Moseley I. Clinical and radiologic characteristics of the imploding antrum, or “silent sinus,” syndrome. Ophthalmology. 2003;110:811-818.
- Al-Zoubi H, Alharbi AA, Ferguson DJ, Zafar MS. Frequency of impacted teeth and categorization of impacted canines: A retrospective radiographic study using orthopantomograms. Eur J Dent. 2017;11:117-121.
- Ferro A, Basyuni S, Santhanam V. Not so silent sinus syndrome: A case report. Int J Surg Case Rep. 2016;23:1-3.
- Cohn JE, Sokoya M, Hararah M, Kadakia S, Ducic Y. Management of enophthalmos from silent sinus syndrome with a customized orbital implant. Otolaryngology Case Reports. 2018;8:17-19.
- Kilty SJ. Maxillary sinus atelectasis (silent sinus syndrome): treatment with balloon sinuplasty. J Laryngol Otol. 2014;128:189-191.
From Decisions in Dentistry. July/August 2025;11(4):28-31.