Precision Planning in Full-Arch Implant Rehabilitation
A prosthetically driven digital workflow enables clinicians to optimize esthetics, function, and longevity in implant-supported and implant-assisted complete-arch prostheses.
This course was published in the July/August 2025 issue and expires August 2028. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
AGD Subject Code: 690
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the diagnostic tools and clinical criteria essential for treatment planning in full-arch implant rehabilitation.
- Compare the clinical indications, advantages, and limitations of implant-supported vs implant-assisted complete-arch prostheses using Misch’s classification.
- Apply principles of digital implant planning and guided surgery to enhance surgical accuracy, prosthetic.
Rehabilitation of complete-arch restorations necessitates meticulous planning to achieve optimal esthetics and function. A successful treatment approach begins with a thorough diagnostic assessment to accurately identify the patient’s chief complaint and underlying oral conditions. Establishing a precise diagnosis is essential, as all treatment interventions must be designed to directly address both functional and esthetic demands while aligning with the patient’s expectations and chief complaint.
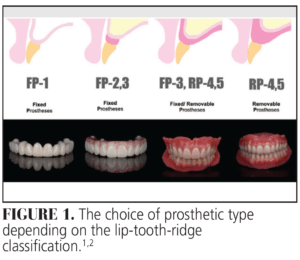
Implant-supported complete-arch fixed dental prostheses (ISCFDPs) or implant-assisted complete-arch removable dental prostheses (IACRDPs) can be categorized into five types according to Misch’s classification:1
- FP-1 (Fixed complete-arch implant prostheses that replace only the teeth)
- FP-2 (Fixed complete-arch implant prostheses with overcontoured teeth replacement)
- FP-3 (Fixed complete-arch implant prostheses that replace both teeth and gingiva)
- RP-4 (Removable complete-arch implant prostheses that majority of support obtained from an implant bar)
- RP-5 (Removable complete-arch implant prostheses whose support is obtained from the implant and mucosa)
The choice of prosthesis is tailored to each patient’s unique anatomy, including factors such as the ideal size and position of the maxillary central incisor, upper lip dynamics, facial support, the shape of the edentulous ridge (lip-tooth-ridge classification), required prosthetic volume, and the patient’s preferences (Figure 1).1,2
Research shows that overall patient satisfaction improves following implant rehabilitation for edentulous patients, regardless of whether an ISCFDP or an IACRDP is chosen.3 While ISCFDPs showed slightly better outcomes in esthetics, function, and personal satisfaction, these differences were not statistically significant. However, IACRDPs demonstrated a statistically significant improvement in oral hygiene after 1 year.3 Following are four steps to enhance the precision and efficiency of surgical and restorative procedures.
Step 1. Diagnostic Phase
Maxillary edentulous patient rehabilitation with implant-supported prostheses presents greater challenges compared to the mandibular arch due to anatomical constraints, biological considerations, and esthetic demands that influence prosthetic design, whether fixed or removable.4 The decision-making process requires careful assessment, beginning with the establishment of optimal teeth positions and an appropriate vertical occlusal dimension (VOD) in centric relation (CR) when necessary, regardless of maxillary or mandibular arch.5
If both parameters need to be determined, the fabrication of a conventional or digital diagnostic complete denture is typically the initial step in the diagnostic workflow. When the existing tooth position is deemed acceptable and a proper VOD in CR can be reliably recorded in terminal dentition, digital wax-ups can be generated using specialized software for virtual planning. However, whenever feasible, physical mock-ups or intraoral try-ins should be part of the diagnostic protocol to validate the proposed design.6
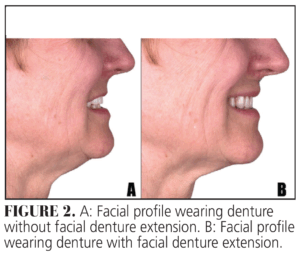
Within this diagnostic phase, intraoral scanning (IOS), facial scanning, and digital photography are essential tools for comprehensive data acquisition. A key advantage of diagnostic dentures is the ability to assess the patient’s facial profile in different conditions without a prosthesis, with a diagnostic denture, and with a flangeless diagnostic denture (Figure 2). This sequential evaluation facilitates an objective determination of the necessity for facial support, a factor that significantly impacts the final prosthetic design and its esthetic and functional outcomes.
Step 2. Cone-Beam Computed Tomography
Once the ideal tooth position, VOD in CR, and prosthesis design have been established, the next step is to obtain a cone-beam computed tomography (CBCT) scan. If a diagnostic denture is available, the dual-scan protocol becomes an essential technique.7
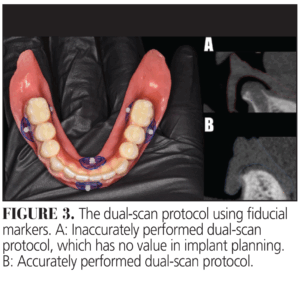
This protocol involves acquiring two CBCT scans: one with the patient wearing the diagnostic denture and another of the denture alone, while incorporating five to six fiducial markers on the denture (with a minimum of three). Two critical considerations in the dual-scan procedure are proper soft tissue adaptation and stable occlusion of the diagnostic denture.8 Inadequate adaptation of the denture base to the soft tissue or an unstable occlusal relationship can result in errors that mislead the planning process (Figure 3). Therefore, ensuring accuracy during the first diagnostic phase is paramount, as it serves as the foundation for the entire workflow.
A well-adapted and functionally stable diagnostic denture enhances the reliability of data integration in implant simulation software, allowing for a truly prosthetically driven treatment plan that optimizes implant positioning while maintaining biological, functional, and esthetic considerations.8 When using a digital wax-up for terminal dentition cases, the CBCT scan should be acquired with the two jaws separated.6 This separation ensures a clear distinction between the maxillary and mandibular arches, facilitating the registration process between STL and DICOM data. Unlike the dual-scan protocol used with diagnostic dentures in which the scan is taken in closed occlusion to capture the established tooth position and restorative space, the open-jaw CBCT approach prevents overlapping structures and enhances the accuracy of digital file alignment.6
Step 3. Verifying Implant Three-Dimensional Positions
Upon successful data importation into implant planning software and accurate registration, digital tools facilitate a prosthetically driven implant planning approach. This enables a comprehensive visualization of the ideal prosthetic tooth positioning, restorative space, osseous architecture, and soft tissue contours, ensuring a precise and predictable treatment outcome. Artificial intelligence (AI) is gaining significant attention in dentistry, particularly in digital implant planning.9 AI-based multimodal image registration for CBCT and IOS has demonstrated high accuracy, time efficiency, and consistency, making it a valuable tool for presurgical implant planning.10 Additionally, AI-driven segmentation of the mandibular canal in CBCT enhances efficiency and reliability in implant planning.11 However, manual verification remains essential to mitigate potential errors and ensure precise anatomical interpretation.
Systematic reviews and meta-analyses note that the use of fewer than five implants per arch to support a fixed prosthesis in completely edentulous maxillae or mandibles achieves survival rates comparable to those obtained with five or more implants per arch. The analysis demonstrated no statistically significant difference (p < 0.05, 95% confidence interval) between these approaches.12 Intentionally tilted implants demonstrate comparable clinical performance to axially positioned implants, providing significant advantages such as reduced need for bone grafting and minimized prosthetic cantilevers. These benefits are achieved without compromising implant survival rates or contributing to increased marginal bone loss, making tilted implants a predictable and effective treatment option in implant-supported prosthetic rehabilitation especially maxilla.13 However, implants should be placed in an axial orientation whenever feasible, as tilted implants increase the complexity of both surgical and prosthetic procedures.
With IACRDPs, the angulation of implants relative to each other plays a critical role in ensuring optimal prosthetic function, stability, and load distribution. This contrasts with ISCFDPs, in which the primary concern is often the angulation of the abutments rather than the implants themselves. However, in certain cases, individual abutments, such as locator abutments, allow for a specific range of acceptable divergence between implants, accommodating minor misalignments while maintaining prosthetic retention and function. Nevertheless, greater divergence among implants increases the likelihood of prosthetic complications, potentially compromising retention, stability, and long-term success. Therefore, precise evaluation and planning of implant angulation are essential to minimize prosthetic challenges and enhance the predictability of implant-supported and implant-assisted prosthetic rehabilitation.14
One of the key advantages of a digital workflow, particularly in digital implant planning for full-arch implant restorations, is the optimized selection of abutments, especially multi-unit abutments, which are frequently required for this type of rehabilitation. The decision-making process for abutment selection plays a crucial role in determining implant positioning and angulation. In particular, the selection of the height of multi-unit abutments is critical for maintaining long-term marginal bone stability and may also influence soft tissue stability.
Several studies have reported that shorter abutments (≤ 1.5 mm) are associated with greater marginal bone loss compared to taller abutments, highlighting the importance of precise abutment selection in digital implant planning.15-20 Abutment height should be at least 2 mm to minimize marginal bone loss.20 The required restorative space, encompassing both vertical and horizontal dimensions, is a critical consideration in prosthetic rehabilitation, as it directly influences the selection of prosthetic materials and the design of the final prosthesis. The minimum vertical restorative space, measured from the crestal soft tissue to the antagonist occlusal plane, varies depending on the type of prosthesis:4,5
- FP-1 prosthesis: 7 to 12 mm
- FP-2 and FP-3 prostheses: ≧ 12 mm
- RP-4 prosthesis: ≧ 15 mm
- RP-5 prosthesis: 8 to 9 mm
 Beyond vertical space, the horizontal restorative space must also be evaluated to ensure adequate prosthetic support, esthetics, and biomechanical stability. A comprehensive 3D assessment of restorative space is essential for achieving long-term functional and esthetic success in ISCFDPs and IACRDPs.
Beyond vertical space, the horizontal restorative space must also be evaluated to ensure adequate prosthetic support, esthetics, and biomechanical stability. A comprehensive 3D assessment of restorative space is essential for achieving long-term functional and esthetic success in ISCFDPs and IACRDPs.
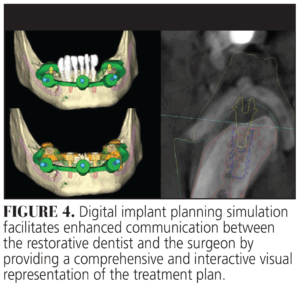
One of the significant advantages of digital implant planning is that it enables surgeons and restorative dentists to collaborate effectively by discussing and confirming implant positions, as well as simulating the surgical procedure prior to actual implant placement (Figure 4). Additionally, this technology facilitates patient involvement in the treatment planning process. By allowing for precise preoperative communication, digital implant planning minimizes the risk of misunderstandings or misinterpretations, ultimately enhancing treatment accuracy and predictability.
Step 4. Designing the Surgical Guide
Based on the restorative volume, prosthetic type, and implant positions, the necessity for bone reduction can be determined during the virtual implant planning phase. The required amount of bone reduction can be precisely evaluated during virtual implant planning, ensuring optimal implant positioning and prosthetic outcomes.21,22
There are three primary approaches for guided surgery: static computer-aided implant surgery (s-CAIS), dynamic computer-aided implant surgery (d-CAIS), and robot-assisted implant placement.23,24 Choosing among these techniques depends on clinical preferences, workflow integration, and case-specific requirements; though s-CAIS is predominantly used in a clinic. Regardless of the selected method, guided and robotic-assisted implant surgeries contribute to improved implant placement accuracy, reduced surgical invasiveness, and enhanced long-term treatment outcomes.25
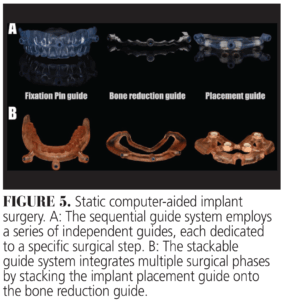 In s-CAIS, two primary guided systems are utilized: the sequential guide system and the stackable guide system (Figure 5). The sequential guide system employs a series of independent guides, each dedicated to a specific surgical step, including fixation pin placement, bone reduction, and implant placement. In contrast, the stackable guide system integrates multiple surgical phases by stacking the implant placement guide onto the bone reduction guide, creating a streamlined workflow that eliminates the need for repeated guide replacements. Both guided systems effectively translate digital preoperative planning into clinical execution, with the choice between them being dependent on case-specific requirements, surgical complexity, and clinician preference.
In s-CAIS, two primary guided systems are utilized: the sequential guide system and the stackable guide system (Figure 5). The sequential guide system employs a series of independent guides, each dedicated to a specific surgical step, including fixation pin placement, bone reduction, and implant placement. In contrast, the stackable guide system integrates multiple surgical phases by stacking the implant placement guide onto the bone reduction guide, creating a streamlined workflow that eliminates the need for repeated guide replacements. Both guided systems effectively translate digital preoperative planning into clinical execution, with the choice between them being dependent on case-specific requirements, surgical complexity, and clinician preference.
Material selection for each guide in s-CAIS plays a crucial role in ensuring surgical precision, durability, and procedural efficiency. The two predominant materials used for guide fabrication are printing resin and cobalt-chromium, each offering distinct advantages and considerations. Printing resin is the most used material due to its cost-effectiveness and ease of fabrication. However, to ensure sufficient strength and durability during the surgical procedure, a specific minimum material thickness is required to prevent fractures or deformations that could compromise guide stability. In contrast, cobalt-chromium guides, although more expensive, allow for a thinner design, which improves surgical accessibility and facilitates a less obstructive intraoperative workflow. Material selection also directly influences critical parameters, such as offset values in guide design and fabrication. Failure to account for these material-specific considerations may lead to technical complications.
Lastly, since various loading protocols for ISCFDPs have consistently demonstrated high implant survival rates,26,27 immediate loading with interim ISCFDPs has become an increasingly preferred approach for edentulous patients receiving at least four implants.28-31 The success of immediate loading is contingent on optimal primary implant stability, proper implant distribution, and strategic prosthetic planning, all of which must be carefully considered during the surgical planning phase. By incorporating immediate loading strategies into the surgical plan, clinicians can enhance efficiency, reduce treatment time, and improve patient satisfaction while maintaining long-term prosthetic and implant success.
The quality of the immediate loading prosthesis is a critical factor in fully utilizing the digital workflow during the prosthetic phase of treatment.32 A well-designed interim ISCFDP not only facilitates a smooth transition to the definitive prosthesis but also ensures optimal function, stability, and patient comfort throughout the healing phase. Durability is a key consideration for immediate loading devices, as they must withstand functional loads during osseointegration while maintaining structural integrity. To enhance both ease of fabrication and durability, various prosthetic conversion techniques have been developed, allowing for a more efficient and predictable workflow.
Conclusion
The integration of digital workflows in full-arch implant rehabilitation has significantly enhanced precision, efficiency, and predictability throughout the treatment process. A prosthetically driven approach, beginning with comprehensive diagnostic data collection and meticulous planning, ensures that implant positioning is optimized to meet both functional and esthetic demands. Advanced digital tools, including IOS, CBCT, digital wax-ups, and guided implant surgery, facilitate seamless communication between the surgical and prosthetic teams, minimizing errors and improving overall treatment outcomes. Furthermore, the use of s-CAIS, d-CAIS, and robot-assisted guided surgery has enabled clinicians to accurately transfer digital planning to the clinical setting, reducing intraoperative complications and enhancing surgical precision.
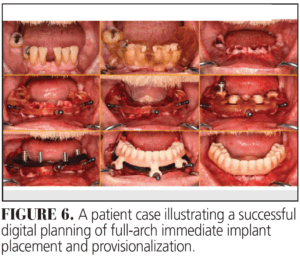
The selection of prosthetic materials, abutments, and restorative space parameters plays a critical role in ensuring long-term prosthetic stability and patient satisfaction. Additionally, the immediate loading protocol has emerged as a preferred treatment modality, offering shorter treatment times and improved patient experience while maintaining high implant survival rates. Ultimately, the successful rehabilitation of implant-supported and implant-assisted complete-arch prostheses relies on a comprehensive digital workflow, integrating diagnostic assessment, surgical precision, and prosthetic planning to achieve optimal long-term outcomes (Figure 6).
References
- Misch CE. Bone classification, training keys to implant success. Dentistry Today. 1989;8(4):39-44.
- Pollini A, Goldberg J, Mitrani R, Morton D. The lip-tooth-ridge classification: a guidepost for edentulous maxillary arches. diagnosis, risk assessment, and implant treatment indications. Int J Periodontics Restorative Dent. 2017;37:835-841.
- Martínez-González JM, Martín-Ares M, Cortés-Bretón Brinkmann J, Calvo-Guirado JL, Barona-Dorado C. Impact of prosthetic rehabilitation type on satisfaction of completely edentulous patients. A 5-year prospective study. Acta Odontol Scand. 2013;71:1303-1308.
- Sadowsky SJ, Fitzpatrick B, Curtis DA. Evidence-based criteria for differential treatment planning of implant restorations for the maxillary edentulous patient. J Prosthodont. 2015;24:433-446.
- Sadowsky SJ, Hansen PW. Evidence-based criteria for differential treatment planning of implant restorations for the mandibular edentulous patient. J Prosthodont. 2014;23:104-111.
- Papaspyridakos P, Bedrossian A, De Souza A,Bokhary A, Gonzaga L, Chochlidakis K. Digital workflow in implant treatment planning for terminal dentition patients. J Prosthodont. 2022;31:543-548.
- Resnik R. Dual CBCT scanning technique for completely edentulous arches. Dentistry Today. 2016;35(12):50-53.
- Moura GF, Siqueira R, Meirelles L, Maska B, Wang HL, Mendonça G. Denture scanning technique for computer-guided implant-supported restoration treatment of edentulous patients. J Prosthet Dent. 2021;125:726-731.
- Alfaraj A, Nagai T, AlQallaf H, Lin WS. Race to the moon or the bottom? applications, performance, and ethical considerations of artificial intelligence in prosthodontics and implant dentistry. Dentistry Journal. 2025;13(1):13.
- Elgarba BM, Fontenele RC, Ali S, et al. Validation of a novel AI-based automated multimodal image registration of CBCT and intraoral scan aiding presurgical implant planning. Clin Oral Implants Res. 2024;35(:1506-1517.
- Ntovas P, Marchand L, Finkelman M, Revilla-León M, Att W. Accuracy of artificial intelligence-based segmentation of the mandibular canal in CBCT. Clin Oral Implants Res. 2024;35:1163-1171.
- Daudt Polido W, Aghaloo T, Emmett TW, Taylor TD, Morton D. Number of implants placed for complete-arch fixed prostheses: A systematic review and meta-analysis. Clin Oral Implants Res. 2018;29:154-183.
- Lin WS, Eckert SE. Clinical performance of intentionally tilted implants versus axially positioned implants: a systematic review. Clin Oral Implants Res. 2018;29:78-105.
- Rabbani S, Juszczyk AS, Clark RK, Radford DR. Investigation of retentive force reduction and wear of the locator attachment system with different implant angulations. Int J Oral Maxillofac Implants. 2015;30:556-563.
- Derks J, Schaller D, Håkansson J, Wennström JL, Tomasi C, Berglundh T. Effectiveness of implant therapy analyzed in a swedish population: prevalence of peri-implantitis. J Dent Res. 2016;95:43-49.
- Galindo-Moreno P, León-Cano A, Monje A, Ortega-Oller I, O’Valle F, Catena A. Abutment height influences the effect of platform switching on peri-implant marginal bone loss. Clin Oral Implants Res. 2016;27:167-173.
- Nóvoa L, Batalla P, Caneiro L, Pico A, Liñares A, Blanco J. Influence of abutment height on maintenance of peri-implant crestal bone at bone-level implants: a 3-year follow-up study. Int J Periodontics Restorative Dent. 2017;37:721-727.
- Pico A, Martín-Lancharro P, Caneiro L, Nóvoa L, Batalla P, Blanco J. Influence of abutment height and implant depth position on interproximal peri-implant bone in sites with thin mucosa: A 1-year randomized clinical trial. Clin Oral Implants Res. 2019;30:595-602.
- Blanco J, Pico A, Caneiro L, Nóvoa L, Batalla P, Martín-Lancharro P. Effect of abutment height on interproximal implant bone level in the early healing: A randomized clinical trial. Clin Oral Implants Res. 2018;29:108-117.
- Chen Z, Lin CY, Li J, Wang HL, Yu H. Influence of abutment height on peri-implant marginal bone loss: A systematic review and meta-analysis. J Prosthet Dent. 2019l;122:14-21.
- Bidra AS. Technique for systematic bone reduction for fixed implant-supported prosthesis in the edentulous maxilla. J Prosthet Dent. 2015;113:520-523.
- Zhao W, Teng W, Su Y, Zhou L. Accuracy of dental implant surgery with freehand, static computer-aided, dynamic computer-aided, and robotic computer-aided implant systems: An in vitro study. J Prosthet Dent. 2024:S0022-3913:00702-9.
- Takács A, Hardi E, Cavalcante BGN, Szabó B, Kispélyi B, Joób-Fancsaly Á, Mikulás K, Varga G, Hegyi P, Kivovics M. Advancing accuracy in guided implant placement: A comprehensive meta-analysis: Meta-Analysis evaluation of the accuracy of available implant placement Methods. J Dent. 2023;139:104748.
- J Yang J, Li H. Accuracy assessment of robot-assisted implant surgery in dentistry: A systematic review and meta-analysis. J Prosthet Dent. 2024;132:747.
- Aghaloo T, Hadaya D, Schoenbaum TR, Pratt L, Favagehi M. Guided and navigation implant surgery: a systematic review. Int J Oral Maxillofac Implants. 2023;38(suppl):7-15.
- Papaspyridakos P, Chen CJ, Chuang SK, Weber HP. Implant loading protocols for edentulous patients with fixed prostheses: a systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2014;29(Suppl):256-270.
- Gallardo YNR, da Silva-Olivio IR, Gonzaga L, Sesma N, Martin W. A systematic review of clinical outcomes on patients rehabilitated with complete-arch fixed implant-supported prostheses according to the time of loading. J Prosthodont. 2019;28:958-968.
- Schimmel M, Araujo M, Abou-Ayash S, et al. Group 4 ITI Consensus Report: Patient benefits following implant treatment in partially and fully edentulous patients. Clin Oral Implants Res. 2023;34(Suppl 26):257-265.
- Horiuchi K, Uchida H, Yamamoto K, Sugimura M. Immediate loading of Brånemark system implants following placement in edentulous patients: a clinical report. Int J Oral Maxillofac Implants. 2000;15:824-830.
- Grunder U. Immediate functional loading of immediate implants in edentulous arches: two-year results. Int J Periodontics Restorative Dent. 2001;21:545-551.
- Misch CM. Immediate loading of definitive implants in the edentulous mandible using a fixed provisional prosthesis: The denture conversion technique. J Oral Maxillofac Surg. 2004;62(9 Suppl 2):106-115.
- Nagai T, Liu W, Yang CC, Polido WD, Morton D, Lin WS. Intraoral scanning for implant-supported complete-arch fixed dental prostheses (ISCFDPs): Four clinical reports. J Prosthodont. 2024 Nov 3.
From Decisions in Dentistry. July/August 2025;11(4):32-35.