 alex-mit / iStock / Getty Images Plus
alex-mit / iStock / Getty Images Plus
Preventing Inflammation With Implant Maintenance
Implant maintenance is key to preventing inflammatory disease that may jeopardize implant health. With no proven strategies to combat peri-implantitis, prevention is integral to the long-term success of implant therapy.
Peri-implant mucositis and peri-implantitis are often associated with an inflammatory reaction to bacterial invasion within the peri-implant tissue. The first signs of peri-implant mucositis include bleeding on probing and/or suppuration, increased probing depth, redness, and swelling. These signs are recognizable upon careful clinical examination.1
The main purpose of the maintenance protocol for patients with implant-supported restorations is to prevent the onset of inflammatory disease, and, if applicable, halt the progression from peri-implant mucositis to peri-implantitis. This is key, as there are no predictable and reliable methods to treat peri-implantitis.
Costa el al2 showed that subjects who lacked monitoring of the peri-implant tissues and preventive maintenance were associated with a higher prevalence of peri-implantitis than patients who underwent maintenance therapy.
Supportive periodontal and implant maintenance has even more value if patients have a history of periodontitis. Roccuzo et al3 conducted a prospective study to evaluate the long-term results of implant therapy in patients with periodontitis. This study revealed that patients with a history of periodontitis have a higher incidence of implant loss and peri-implant disease. In addition, patients with a history of periodontitis who do not follow a maintenance schedule experience a significantly higher rate of implant failures.
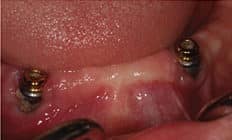
Patients with implant-supported restorations clearly should have regular maintenance visits. At each appointment, a comprehensive evaluation should include reviewing the medical history, followed by updating periodontal and peri-implant charting, evaluating oral hygiene, and assessing occlusion. Because poor oral hygiene is a risk factor for peri-implant disease (Figure 1), emphasizing the importance of optimal self-care, along with patient education, should be a part of the maintenance visit.
Because there is no consensus regarding a definitive frequency for maintenance visits, maintenance treatment should be individualized according to each patient’s systemic and local risk factors. For patients with history of periodontitis with acceptable self-care, a 3-month recare interval is usually adequate. On the other hand, when there are no systemic or local risk factors, recare visits might be scheduled every 6 months. If patients still maintain some natural teeth, alternating maintenance therapy between a general dentist’s office and specialist’s office may be beneficial for patients. Careful attention to the presence of inflammation and peri-implant tissue health can help sustain the long-term success of implant-supported restorative treatment.4,5
References
- Peri-implant mucositis and peri-implantitis: a current understanding of their diagnoses and clinical implications. J Periodontol. 2013;84:436–443.
- Costa FO, Takenaka-Martinez S, Cota LO, Ferreira SD, Silva GL, Costa JE. Peri-implant disease in subjects with and without preventive maintenance: a 5-year follow-up. J Clin Periodontol. 2012;39:173–181.
- Roccuzzo M, De Angelis N, Bonino L, Aglietta M. Ten-year results of a three-arm prospective cohort study on implants in periodontally compromised patient Part 1: implant loss and radiographic bone loss. Clin Oral Implants Res. 2010;21:490–496.
- Gay IC, Tran DT, Weltman R, et al. Role of supportive maintenance therapy on implant survival: a university-based 17 year retrospective analysis. Int J Dent Hyg. 2016;14:267–271.
- Armitage GC, Xenoudi P. Post-treatment supportive care for the natural dentition and dental implants. Periodontol 2000. 2016;71:164–184.
This information originally appeared in Hamada Y, Hill K, Chang J, John V. Addressing risks of implant complications. Decisions in Dentistry. 2017;3(10):14–21.


