
Role of Aloe Vera in Oral Health Management
Recognized for its antioxidant and antimicrobial action, aloe vera’s anti-inflammatory properties can also be beneficial as an alternative dental therapy.
This course was published in the November 2018 issue and expires November 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the properties that make aloe vera a suitable alternative therapy for various dental procedures.
- Identify the plant’s viscous secretions, and its effects in promoting wound healing through its antimicrobial, antioxidant and anti-inflammatory actions.
- Describe preventive uses for aloe vera in oral health care.
In many parts of the world, herbal and natural remedies are commonly used to treat injuries and illnesses.1,2 Similarly, some U.S. patients gravitate toward natural, homeopathic and holistic medicaments as part of their health care regimens. In addition, the use of antibiotics to treat infections has contributed to an increase in bacterial resistance3,4 and the rise of so-called superbugs. As a result, alternative medicine has been a popular topic of interest, as researchers investigate ways to incorporate natural products into therapeutic treatments.4 With a historical reputation in holistic healing, aloe vera is one of the most popular medicinal plants. Due to the naturally occurring chemical compounds, it has been shown to demonstrate beneficial inhibitory effects on gram-positive and gram-negative bacteria, such as Staphylococcus aureus, Pseudomonas aeruginosa and Porphyromonas gingivalis.3,5 Besides its antimicrobial effects, aloe vera’s antioxidant and anti-inflammatory action can also aid the healing process following dental treatment.
Anti-inflammatory Properties: As noted, the aloe vera plant has been found to contain anti-inflammatory properties.6 Research shows it inhibits histamine and leukotrienes released by mast cells and can cause macrophages to release nitric oxide and cytokines.7 It also has been shown to inhibit the cyclooxygenase pathway, which reduces prostaglandin E2 (PGE2) and breaks down bradykinin to reduce pain.7 There is a reduction of leukocyte adherence and tumor necrosis factor-α (TNF-α), which, in turn, blocks the inflammatory process.8 Each of the pathways deals with the immune system, which helps explain its method of action.7 Additionally, the anti-inflammatory fatty acids in aloe vera juice, such as 𝛽-sitosterol and campesterol, can help with a variety of immune system diseases.5
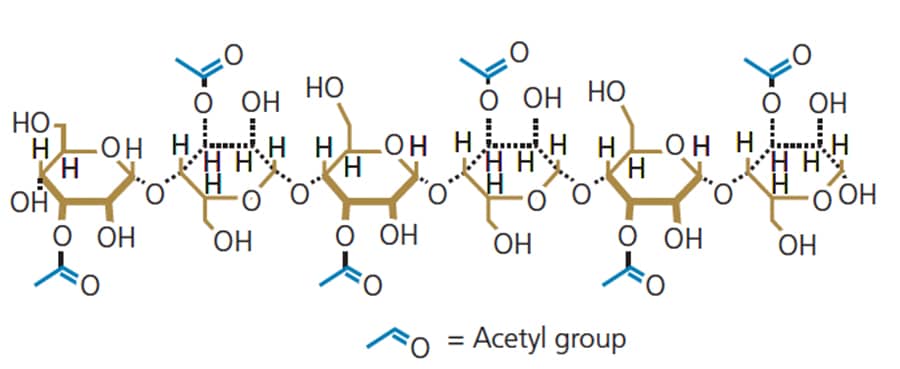
Antioxidant Properties: The viscous secretion in aloe vera, known as mucilage, contains various vitamins and amino acids. Specifically, vitamins A, C and E are antioxidant compounds which contribute to ridding potentially damaging oxidative agents and carcinogens.9,10 Additionally, the mucilage contains antioxidant enzymes, such as glutathione peroxidase and superoxide dismutase, that work to counteract free radicals produced from the site of infection.9 The plant’s antioxidant properties work synergistically with the anti-inflammatory components to expedite wound healing.9 Daily consumption of aloe vera gel extract was found to reduce the amount of Lactobacillus spp. and Streptococcus mutans in saliva, which are oral pathogenic bacteria.11 In addition, the gel extract helps increase plasma total antioxidant capacity, with no clinical adverse effects.11
Antimicrobial Properties: The antimicrobial effect of aloe vera is mainly due to the anthraquinones found in the sap, which are associated with inhibiting bacterial protein synthesis.3 The plant contains an antibacterial agent called acemannan that plays an indirect role in its therapeutic activities through phagocytosis (Figure 1).12 Studies completed in vitro and in vivo contribute to scientific understanding of how it fights pathogens by reducing secondary infections, increasing the activity of T-lymphocytes, and increasing the activity of macrophages (Figure 2), thus promoting wound healing.1
Wound Healing: Aloe vera possesses several beneficial properties, as noted above; together the anti-inflammatory, antioxidant and antimicrobial properties work simultaneously to aid wound healing. Takzaree et al13 demonstrated its ability to expedite wound healing. Specifically, this study showed the increase of transforming growth factor-𝛽 (TGF-𝛽) gene expression with aloe vera application to wounds on rat subjects. TGF-𝛽 is known to be one of the most important factors in wound healing; this is due to the gene stimulating epithelialization and angiogenesis, which is critical to healing.13 Although the discussion of aloe vera’s wound-healing properties is dependent on this one study and more research is needed, these findings underscore its potential benefits as an alternative therapy in the dental and medical fields.
PREVENTIVE ACTION
Prevention is a key element of sustaining optimal oral health. Prabhakar et al12 conducted a randomized clinical trial in vivo using a split-mouth design to determine aloe vera’s efficacy as a potential cavity-disinfecting agent following minimally invasive hand excavation of caries. Three solutions (distilled water, aloe vera extract and propolis extract) were compared with a control, and the results showed significant amounts of cariogenic bacteria remained following hand excavation alone. In addition, bacterial counts were statistically significant in post-cavity disinfection. Compared to distilled water, disinfecting caries sites with propolis and aloe vera extract resulted in a statistically significant reduction in bacterial counts. The two extracts had similar disinfecting potential, but aloe vera was marginally more efficacious and the authors reported no adverse effects.12 This suggests using aloe vera as an alternative cavity-disinfecting agent may aid in the prevention of secondary caries and contribute to the long-term success of restorative procedures.
Using distilled water for the control group, Patri and Sahu14 conducted a similar in vivo study comparing two herbal antimicrobial agents — 1% tea tree oil and aloe vera gel — to 2% chlorhexidine (CHX) gel. The purpose was to determine each group’s efficacy as a cavity disinfectant in minimally invasive dentistry. Similar to the Prabhakar et al12 study, hand excavation alone did not eliminate all the cariogenic bacteria.14 According to Patri and Sahu,14 all four test groups showed a statistically significant reduction in total viable count (TVC) between pre-excavation and post-excavation of dental caries. Except for the control group, there was a significant reduction in TVC between post-excavation and post-disinfection in the other three groups. In regard to post-disinfection of dental caries, 2% CHX gel exhibited the highest reduction in TVC, followed by 1% tea tree oil and aloe vera gel, respectively. The difference in post-disinfection between tea tree oil and aloe vera gel was not statistically significant. Both herbal agents displayed the capability of acting as cavity-disinfectants with no adverse effects.14
Although CHX is extremely effective against S. mutans14 and is commonly used as a cavity disinfectant or antimicrobial rinse following periodontal therapy, a more cost-effective antimicrobial agent, such as aloe vera, might represent a promising alternative preventive therapy.12,14
NONSURGICAL THERAPY FOR PERIODONTITIS
The first step in treating periodontitis is reducing the pathogens and risk factors that allow the disease to progress, and providing therapy that helps patients regain lost attachment. Nonsurgical treatment includes scaling and root planing (SRP) to debride bacterial biofilm, endotoxins and calculus embedded in the tooth surface.15,16 This is often accompanied by the adjunctive use of chemotherapeutic agents released subgingivally into the periodontal pockets.17 Compared to other agents, recent studies have demonstrated topical use of aloe vera within a periodontal pocket as an adjunct to nonsurgical SRP is effective in the treatment of periodontal disease.15,16
In one of these studies, a clinical trial was completed on subjects diagnosed with moderate to severe periodontitis.15 The subjects received nonsurgical SRP on all their teeth. After the procedure, they were instructed to use a specific toothpaste and not change their oral hygiene self-care regimen. Using a split-mouth design, one quadrant had aloe vera gel injected into the periodontal pockets, and the other quadrant was injected with distilled water. Measurements of plaque index, gingival index and probing depth at various intervals were compared based on differences using an independent t-test (significance level of p<0.05). The quadrants injected with aloe vera gel showed a statistically significant improvement in relation to gingival index and probing depth, but results for the plaque index did not show a statistically significant difference between the control and test groups. The statistically significant difference of the gingival index (p=0.001) and probing depth (p=0.026) supports aloe vera as effective in aiding the gingiva during periodontal therapy.15
The other study compared the effectiveness of aloe vera gel and metronidazole gel, a common antifungal agent, as adjuncts to nonsurgical SRP in patients diagnosed with periodontitis.16 Results were compared based on plaque index, gingival index and probing depths at 30-, 60- and 90-day intervals. Aloe vera was found to produce statistically significant benefits across all clinical parameters. The results support this agent as a substitute for metronidazole delivery after nonsurgical SRP procedures.16
These studies and additional research support aloe vera gel as an alternative adjunctive therapy for periodontitis.15–18 Local subgingival delivery of aloe vera gel has been associated with a decrease in plaque index, reduction in probing depths, and improved rate of attachment. This was attributed to its antimicrobial effects in eradicating Aggregatibacter actinomycetemcomitans and P. gingivalis, along with its anti-inflammatory and antioxidant properties.8,17
ORAL WOUNDS
Wounds in the oral cavity can adversely affect speaking, swallowing and mastication, potentially leading to xerostomia and oral dysesthesia.19 Oral lesions may result from infection, physical insult, chemical contact, immunological reactions, systemic diseases, trauma, neoplasia or oral habits,19 and proper management is necessary to alleviate detrimental symptoms.
Sahebjamee et al20 investigated aloe vera in the prevention of radiation-induced oral mucositis (RIOM). This condition results in erythematous and ulcerative lesions of the oral mucosa that lead to pain, weight loss, and difficulty eating, drinking and speaking. Although benzydamine hydrochloride has traditionally been used to reduce incidence of RIOM, a burning mouth sensation has been reported as a side effect. Within this study, head and neck cancer patients receiving conventional radiation therapy were given a benzydamine mouthrinse or an aloe vera mouthrinse three times daily throughout the treatment.20 Results showed that aloe vera rinse was just as effective as benzydamine, but produced no side effects.20 Although neither product is capable of preventing RIOM, this study suggests both agents can delay its onset and severity.
In a 2017 study, Ali and Wahbi7 demonstrated aloe vera’s efficacy in managing oral lichen planus (OLP) wounds. They concluded that while it is inferior to synthetic corticosteroid triamcinolone acetonide (the gold standard) in managing OLP, it appears to be a promising aid for OLP due to its lack of adverse effects or contraindications found with corticosteroids.7
SUGGESTIONS FOR FUTURE RESEARCH
Further studies are needed to evaluate the use of aloe vera in dentistry as an alternative therapeutic agent. Future research should include larger sample sizes and longer time intervals to follow-up as longitudinal studies. Another interesting prospect includes using aloe vera in conjunction with other herbal, natural and homeopathic products. For example, Sahgal et al21 showed pomegranate (Punica granatum) offers similar effects to CHX in eliminating periodontal pathogens. Future studies might include the combination of aloe vera and pomegranate to evaluate if the two yield enhanced antimicrobial effects.
Rezaei et al22 showed that when used as a mouthrinse with intubated patients in an intensive care unit, 10 mg dried Salvadora persica ethanol extract, combined with 940 mg aloe vera gel, had superior healing effects on the gingival index compared to CHX. It would be useful to investigate the impact on using this alternative formula in patients undergoing periodontal therapy.
CONCLUSION
Current research supports aloe vera’s use as an alternative therapy in oral health management. It appears the synergistic relationship between its anti-inflammatory, antioxidant and antimicrobial properties contribute to the wound-healing process. Additionally, findings suggest aloe vera can help prevent caries, and is an effective adjunct to nonsurgical SRP in patients with periodontitis.
Aloe vera is readily accessible, cost-effective, clinically applicable, utilizes minimal equipment, and is associated with minimal adverse outcomes. This makes it an intriguing alternative therapy for oral health care.
REFERENCES
- Mangaiyarkarasi SP, Manigandan T, Elumalai M, Cholan PK, Kaur, RP. Benefits of aloe vera in dentistry. J Pharm Bioallied Sci. 2015;7:S255–S259.
- Pereira RF, Bártolo PJ. Traditional therapies for skin wound healing. Adv Wound Care (New Rochelle). 2016;5:208–229.
- Cataldi V, Di Bartolomeo S, Di Campli E, Nostro A, Cellini L, Di Giulio M. In vitro activity of aloe vera inner gel against microorganisms grown in planktonic and sessile phases. Int J Immunopathol Pharmacol. 2015;28:595–602.
- Nimma VL, Talla HV, Bairi JK, Gopaldas M, Bathula H, Vangdoth S. Holistic healing through herbs: effectiveness of aloe vera on post extraction socket healing. J Clin Diagn Res. 2017;11:ZC83–ZC86.
- Kumar A, Sunkara MS, Pantareddy I, Sudhakar S. Comparison of plaque inhibiting efficacies of aloe vera and propolis tooth gels: a randomized PCR study. J Clin Diagn Res. 2015;9:ZC01–ZC03.
- Chhina S, Singh A, Menon I, Singh R, Sharma A, Aggarwal V. A randomized clinical study for comparative evaluation of aloe vera and 0.2% chlorhexidine gluconate mouthwash efficacy on de-novo plaque formation. J Int Soc Prev Community Dent. 2016;6:251–255.
- Ali S, Wahbi W. The efficacy of aloe vera in management of oral lichen planus: a systematic review and meta-analysis. Oral Dis. 2017;23:913–918.
- Anuradha A, Patil B, Asha VR. Evaluation of efficacy of aloe vera in the treatment of oral submucous fibrosis — a clinical study. J Oral Pathol Med. 2017;46:50–55.
- Hashemi SA, Madani SA, Abediankenari S. The review on properties of aloe vera in healing of cutaneous wounds. Biomed Res Int. 2015;2015:1–6.
- Neena IE, Ganesh E, Poornima P, Korishettar R. An ancient herb aloe vera in dentistry: a review. J Oral Res Rev. 2015;7:25–30.
- Prueksrisakul T, Chantarangsu S, Thunyakitpisal P. Effect of daily drinking of aloe vera gel extract on plasma total antioxidant capacity and oral pathogenic bacteria in healthy volunteer: a short-term study. J Complement Integr Med. 2015;12:159–164.
- Prabhakar AR, Karuna YM, Yavagal C, Deepak BM. Cavity disinfection in minimally invasive dentistry – comparative evaluation of aloe vera and propolis: A randomized clinical trial. Contemp Clin Dent. 2015;6:S24–S31.
- Takzaree N, Hadjiakhondi A, Hassanzadeh G, Rouini MR, Manayi A, Zolbin MM. Transforming growth factor-β (TGF-β) activation in cutaneous wounds after topical application of aloe vera gel. Can J Physiol Pharmacol. 2016;94:1285–1290.
- Patri G, Sahu A. Role of herbal agents — tea tree oil and aloe vera as cavity disinfectant adjuncts in minimally invasive dentistry — an in vivo comparative study. J Clin Diagn Res. 2017;11:DC05–DC09.
- Moghaddam AA, Radafshar G, Jahandideh Y, Kakaei N. Clinical evaluation of effects of local application of aloe vera gel as an adjunct to scaling and root planing in patients with chronic periodontitis. J Dent (Shiraz). 2017;18:165–172.
- Singh HP, Muzammil, Sathish G, Babu KN, Vinod K, Rao HP. Comparative study to evaluate the effectiveness of aloe vera and metronidazole in adjunct to scaling and root planing in periodontitis patients. J Int Oral Health. 2016;8:374–377.
- Pradeep A, Garg V, Raju A, Singh P. Adjunctive local delivery of aloe vera gel in patients with type 2 diabetes and chronic periodontitis: a randomized, controlled clinical trial. J Periodontol. 2016;87:268–274.
- Yeturu SK, Acharya S, Urala AS, Pentapati KC. Effect of aloe vera, chlorine dioxide, and chlorhexidine mouth rinses on plaque and gingivitis: a randomized controlled trial. J Oral Biol Craniofac Res. 2016;6:54–58.
- Nair, GR, Naidu GS, Jain S, Nagi R, Makkad RS, Jha A. Clinical effectiveness of aloe vera in the management of oral mucosal diseases — a systematic review. J Clin Diagn Res. 2016;10:ZE01–ZE07.
- Sahebjamee M, Mansourian A, Hajimirzamohammad M, et al. Comparative efficacy of aloe vera and benzydamine mouthwashes on radiation-induced oral mucositis: a triple-blind, randomised, controlled clinical trial. Oral Health Prev Dent. 2015;13:309–315.
- Sahgal A, Chaturvedi SS, Bagde H, et al. A randomized control trial to evaluate efficacy of anti-bacterial and anti-inflammatory effect of aloe vera, pomegranate and chlorhexidine gel against periodontopathogen. J Int Oral Health. 2015;7:33–36.
- Rezaei S, Rezaei K, Mahboubi M, et al. Comparison the efficacy of herbal mouthwash with chlorhexidine on gingival index of intubated patients in intensive care unit. J Indian Soc Periodontol. 2016;20:404–408.
Featured image by DVULIKAIA/ISTOCK/GETTY IMAGES PLUS
From Decisions in Dentistry. November 2018;4(11):42–45.




