Maintenance Considerations for Prosthodontic Patients
A carefully organized and strategically implemented maintenance program is integral to maintaining the longevity of dental restorations, stability of soft tissue esthetics, and, ultimately, patient satisfaction.
PURCHASE COURSEThis course was published in the September 2016 issue and expires 09/30/19. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
OBJECTIVES
After reading this course, the participant should be able to:
- Identify strategies for creating an effective recall and maintenance schedule for patients with dental restorations.
- Discuss considerations for recall and maintenance for patients with tooth-borne restorations.
- List the key factors needed to maintain the longevity of implant-borne restorations.
A carefully organized and strategically implemented maintenance program is integral to maintaining the longevity of dental restorations, stability of soft tissue esthetics, and, ultimately, patient satisfaction
INTRODUCTION
Colgate is delighted to have supported the American College of Prosthodontists’ Education Foundation with an unrestricted educational grant to conduct the research behind the systematic reviews and clinical practice guidelines that form the basis of this article. So often excellent research remains hidden in esoteric journals and is difficult for the practicing dental professional to access and implement. The Clinical Practice Guidelines for Recall and Maintenance of Patients With Tooth-Borne and Implant-Borne Dental Restorations are designed to effectively bridge the gap to ensure patients receive evidence-based care. A summary of these guidelines is included with this issue so be sure to save the laminated card for future reference. The authors have done an excellent job bringing these guidelines to life with clinical examples and recommendations. I am sure this article will be of value to every practicing dental professional.
—Barbara Shearer, BDS, MDS, PhD
Director of Scientific Affairs
Colgate Oral Pharmaceuticals
FROM THE AMERICAN COLLEGE OF PROSTHODONTISTS
The American College of Prosthodontists (ACP) is proud to have collaborated with leading experts from the American Dental Hygienists’ Association, Academy of General Dentistry, and the American Dental Association in developing the Clinical Practice Guidelines for Recall and Maintenance of Patients With Tooth-Borne and Implant-Borne Dental Restorations. This landmark project was supported through the ACP Education Foundation and has helped transform a concept from being referred to as simply “maintenance,” into a patient-focused, patient-centered professional maintenance protocol. The clinical practice guidelines are founded on the best available science, whenever available, and designed to guide patient education and professionally prescribed protocols. Prevention and maintenance include supporting restorative and prosthodontic treatment outcomes, as well as providing patients with the information they need to maintain their oral health.
—Lily T. Garcia, DDS, MS, FACP
Past President of the American College of Prosthodontists
A structured plan for the maintenance of dental restorations is an important part of providing health care. A carefully organized and strategically implemented maintenance program is a strong predictor for the longevity of dental restorations, stability of soft tissue esthetics, and, ultimately, patient satisfaction.1–3 Even meticulously completed restorative care can fail unless the clinician and patient invest the time and energy into developing and following a structured maintenance program.

Patient maintenance plans have historically been discussed and implemented following the completion of restorative treatment. Waiting until restorative care is complete to discuss a maintenance strategy, however, may be a mistake. A plan for the maintenance of dental restorations should be discussed during the initial consultation and evaluation. If patient compliance is not expected, or if risk factors cannot be adequately controlled, the treatment plan and eventual care provided need to be structured accordingly.
During the initial consultation and evaluation, a careful review of patient history, medical status, medication usage, age, dexterity, compliance, planned treatment, and anticipated functional use are considered. The goal is to match the numerous variables that influence treatment with the anticipated requirements to maintain the planned restorations. A discussion of potential biologic complications, such as dental caries or periodontal diseases, as well as mechanical complications from bruxism and material limitations will support patient compliance and understanding. It is from this conversation that a maintenance strategy is developed and matched to treatment needs and anticipated compliance. Developing a maintenance plan may require additional diagnostic testing and/or the use of specific interventions to address patient-specific risk factors.
The maintenance protocol for patients with restorations includes recommendations for patient recall intervals, an at-home daily maintenance regimen, and a professional maintenance plan completed by the dental team in office. The elements of the maintenance program should be complementary, patient-specific, and address potential factors that could compromise restorative treatment.
Recent systematic reviews on the maintenance of tooth-borne and implant-borne restorations by Bidra el al4,5 and clinical practice guidelines6 (CPGs) provide the basis for effective maintenance programs. These systematic reviews and CPGs were sponsored by the American College of Prosthodontists (ACP) and included a scientific panel of experts appointed by the ACP, American Dental Association (ADA), Academy of General Dentistry (AGD), and American Dental Hygienists’ Association (ADHA), which critically evaluated and debated findings from two recent systematic reviews4,5 to develop CPGs on the maintenance of tooth-borne and implant-borne restorations.6
TOOTH-BORNE RESTORATIONS
As the number of older adults in the United States continues to rise, more patients will be living with complex dental restorations. As such, maintenance plans for dental restorations are more relevant now than ever before. In light of age-associated losses of tooth structure, oral environments often adversely affected by high-carbohydrate diets and medication-induced xerostomia, avoiding biologic and mechanical complications is challenging.
The 6-month recall for dental appointments is a longstanding tradition in dentistry. Unfortunately, there is limited evidence describing what the most appropriate recall regimens should be. In patients with complex tooth-borne removable and fixed restorations, there is even less evidence regarding appropriate recall schedules. A systematic review of dental recall intervals and incidence of dental caries found that a 6-month recall protocol for caries prevention was not supported by the biomedical literature.7,8 The authors concluded that clinicians should consider assigning recall intervals based on patients’ risk of developing caries. Traditionally, patients at either low risk or high risk for dental diseases have been placed on 6-month recall intervals because such intervals were thought to facilitate prevention and early detection of diseases, and also permit routine oral cancer screening. Additional considerations include facilitating earlier referral to physicians for the diagnoses of sleep disorders, diabetes, and hypertension. While all of these may be valid reasons to consider 6-month recall intervals, there are many reasons to support tailoring a plan to specific patient needs.
Recall programs based on risk assessment of potential complications, such as caries or periodontal diseases, have become increasingly accepted in dentistry. For example, rather than just assessing existing caries, the risk for future caries must be considered. This is important because the removal of caries — although an important therapeutic intervention — does not typically decrease the risk of future caries.9,10 Similarly, risk assessment has been applied to periodontal disease management, as equivalent volumes of plaque may result in varying levels of inflammation in individuals, thus suggesting the need for patient-specific recall intervals.11,12 More accurate risk assessment models are expected to result in improved outcomes at reduced cost.11 In creating a maintenance plan for a patient with complex dental restorations, patient-specific factors and the restorative care provided can both potentially add risk.
The exact at-home maintenance program for each patient will depend on many factors, including the patient’s history, medication usage, systemic health, age, dexterity, type of restorative procedures, and anticipated compliance. The use of specific oral topical agents, such as chlorhexidine, fluoride, and triclosan, can reduce the risk for gingival inflammation, dental caries, and candidiasis. Therefore, both the type of restoration and patient risk factors should be considered before creating an at-home maintenance program.
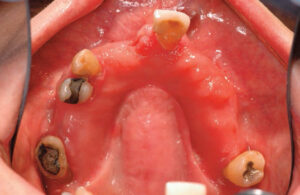
A carefully considered maintenance program is especially important for patients receiving complex tooth-borne dental restorations who are at increased risk for needing additional restorative care. For example, when evaluating caries risk of an abutment for a complex fixed dental prosthesis (FDP), compared with a less complex single crown, FDP abutments had a 27% greater risk for caries.13 Additionally, when complex tooth-borne restorations, such as FDPs, were placed and patients did not adhere to a maintenance program, plaque levels and tooth loss due to periodontitis were significantly higher compared with patients who complied with a maintenance program.13 In patients wearing a partial denture, maintenance programs accompanied by an illustrated manual resulted in decreased plaque accumulation on the device.14 In addition, regular supervision of patients with a removable dental prosthesis (RDP) resulted in acceptable oral and denture hygiene over a prolonged interval.14 Overnight wearing of an RDP, increased denture age, and substandard extraoral storage conditions also potentially increase the incidence of oral mucosal lesions (Figure 1).15
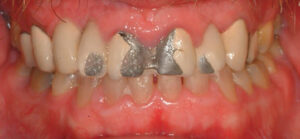
Complex fixed prostheses are more difficult to maintain than single crowns, thus, a structured maintenance program is critical in order to avoid complications (Figure 2). For example, in a study of 93 subjects, Ortolan et al16 found that patients with single crowns demonstrated better oral hygiene than those with FDPs during professional recall and maintenance. Similarly, Ikai et al13 found that patients with FDPs who did not participate in a professional maintenance program had a relatively high mean plaque index (43.2%) and a high failure rate (33%) over an average follow-up period of 16-plus years. Patients treated with removable partial dentures also needed more extensive maintenance than patients with fixed restorations.17
There is evidence that judicious use of fluoride, triclosan, and chlorhexidine can provide benefits for patients with dental restorations and those at risk for restoration failure. Ekstrand et al18 compared fluoride dentifrices with 5,000 ppm vs 1,450 ppm in a randomized control trial (RCT) on 125 patients and determined that the dentifrice with 5,000 ppm of fluoride was significantly more effective in limiting the progression of root caries and in promoting remineralization.
The use of chlorhexidine has been shown to help maintain the health of tissues around teeth restored with composite resins, and can be an adjunct in decreasing Candida albicans.19,20 In a study of 20 patients with diabetes mellitus, the periodontal tissues of teeth restored with class V composite resin improved with use of a 0.12% chlorhexidine rinse compared to the no-chlorhexidine group.19 In a double-blind RCT, López-Jornet et al20 showed that twice-daily use of a 10 ml of an alcohol-free 0.2% chlorhexidine rinse for 60 seconds significantly decreased colony forming units of C. albicans and improved gingival health in elderly patients with partial removable denture prostheses.20 The chronic use of chlorhexidine can decrease taste sensation, stain teeth and/or a prosthesis, and may leave an unpleasant taste, so chlorhexidine should only be used when necessary.
The use of a fluoride dentifrice containing 0.3% triclosan should be considered for patients at high risk for root caries, patients with numerous single crowns, and those with high-risk prosthetic procedures, such as FDPs.21 Although many regulatory agencies, including the U.S. Food and Drug Administration, have deemed triclosan safe for use where a health benefit has been demonstrated, concerns have been raised regarding its safety, and additional research is underway.22,23 As such, triclosan is best reserved for patients at high risk of oral disease.
In a large-scale RCT on 1,357 patients, fluoride toothpastes were compared with 0.3% triclosan fluoride toothpaste to evaluate primary caries on root surfaces and recurrent caries around crowns over a 3-year period.21 A 0.3% triclosan fluoride dentifrice significantly decreased root caries.21 The crown failure rate was three times less when using a dentriface with triclosan as compared to a dentriface without triclosan. As such, triclosan dentifrices can be considered for patients at risk for root caries or extensive prosthodontic treatment (Figure 3).
Professional maintenance helps boost oral health outcomes. Zenthöfer et al24 and Morino et al25 independently conducted studies in nursing homes on partially edentulous patients with both natural teeth and partial RDPs and concluded that professional oral health interventions, including professional teeth and denture cleaning and manual brushing by dental hygienists, significantly improved oral health conditions among the elderly. De Visschere et al26 noted that other factors, such as the unique characteristics of individual nursing homes, might also impact outcome improvement. Similarly, an RCT by Ribeiro et al14 concluded that a group that underwent oral hygiene instructions had improved gingival indexes compared with a control group which received no oral hygiene instructions. The authors also noted that reinforcement of oral hygiene instructions was necessary to maintain compliance.
IMPLANT-BORNE RESTORATIONS
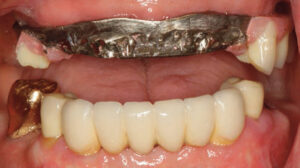
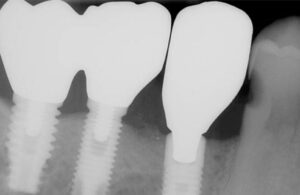
Implant-borne restorations present with unique biological and mechanical complications, all of which warrant a patient-specific and risk-based recall regimen (Figure 4 through Figure 6). Implant-supported single crowns and implant-supported FDPs have favorable survival rates, but they also frequently experience mechanical and biologic complications over the long-term. Ten-year survival rates for implants supporting single crowns were reported as approximately 95%.27 In addition, implant-supported FDPs were reported successful 93% of the time.28 Notably, 33.6% of patients had a mechanical and/or biologic complications in the first 5 years, prompting the authors to recommend that patients be placed in a well-structured maintenance program.28 Mechanical complications of implant-supported FDPs include veneering material fractures, screw loosening, loss of retention of cemented FDPs, and screw fracture over 5 years.28,29
The importance of maintenance programs for patients with dental implants is well illustrated in a study by Costa et al2 in which 80 partially edentulous patients restored with implants and diagnosed with peri-implant mucositis were monitored to determine how often they progressed to peri-implantitis over 5 years. Patients active in a maintenance program progressed to peri-implantitis much less frequently (18%) compared with those not active in a maintenance program (43.9%).2 Risk factors, such as a lack of manual dexterity, motivation, or compliance, need to be identified early so both the treatment plan and maintenance plan can reflect reality.
Comparative studies are needed to better understand the effects of various patient recall intervals on the maintenance of soft tissue health proximate to implants. By default, clinicians are using existing recall and maintenance protocols established for patients with natural dentitions. While the use of 6-month recall intervals is an adequate starting point, the interval needs to evolve based on the patient’s needs and influencing factors, such as prosthetic design, biologic and mechanical issues, and conditions of proximate tissues.
The at-home use of chlorhexidine and triclosan have shown promise in helping to maintain the health of soft tissues supporting dental implant restorations. Paolatonio et al30 evaluated microbial penetration in the peri-implant tissue in 30 subjects over 8 months. When a 1% chlorhexidine gel was applied to the internal portions of the implant prior to abutment placement, a decrease in internal bacterial colonization was observed when compared with no gel controls. Although chlorhexidine gel is not available in the U.S., application of chlorhexidine onto the internal portions of implant fixtures may be beneficial for patients who have an elevated risk of developing peri-implant diseases.
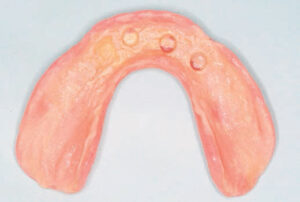
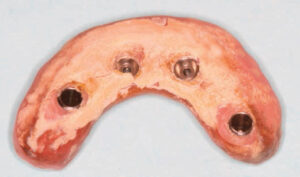
The at-home use of triclosan fluoride dentifrice has resulted in improvement of soft tissue health in patients with both implants and teeth. At-home use of triclosan was also effective in an edentulous population restored with implants and diagnosed with peri-implant mucositis.31,32 In a 6-month study of the effects of a 0.3% triclosan fluoride toothpaste on oral biofilms and gingival inflammation, Sreenivasan et al31 looked at 120 subjects in a double-blind study that evaluated plaque, gingival inflammation, and bleeding on probing, in addition to providing microbiological analyses. At 3 months and 6 months, the groups using triclosan toothpaste had significantly lower levels of dental plaque, gingivitis, and bleeding on probing compared with those not using triclosan.31
In another study of 120 edentulous patients restored with at least two implants and diagnosed with mucositis, the impact of triclosan on soft tissue and plaque measures was evaluated at baseline, 3 months, and 6 months.32 Patients using a triclosan dentifrice had better bleeding on probing scores (reduced from 53.8% to 29.1%), while the control group had a slight increase in percentage of sites displaying bleeding on probing. Triclosan dentifrice seems to support soft tissue health around dental implants and can be recommended for patients at high risk of peri-implant diseases.
Substantial evidence demonstrates the importance of professional and at-home maintenance of implant-borne restorations. Fischer et al33 collected data on outcomes and maintenance of screw-retained implant-supported complete-arch cast titanium-acrylic resin prostheses in the edentulous maxillae of 24 patients over 10 years. They evaluated the number of prosthetic teeth recemented or replaced, screw loosenings, and the number of remakes of fixed prostheses, cantilever lengths (as a potential risk for fracture) at baseline and 1, 3, 5, and 10 years. They concluded that the most frequent complication was related to fractured denture teeth (Figure 4). The status of the opposing dentition and length of cantilevers did not increase risk.33
Professional recommendations for oral hygiene aids used during self-care were evaluated in independent studies. Swierkot et al,34 Rasperini et al,35 and Vandekerckhove et al36 showed that power toothbrushes were a safe and efficient method for plaque removal around implant-borne restorations, and that they had no adverse effects on peri-implant health. Power toothbrushes were not shown to be superior to conventional brushing in removing plaque, however.
Mussano et al37 evaluated the use of polytetrafluoroethylene curets versus a glycine powder air polishing system. Periodontal probing depths, bleeding on probing, and bacterial infiltration within the gingival sulci were evaluated at baseline, 1 week, and 4 weeks. The authors concluded that glycine powder air polishing was more effective than curets for the maintenance of peri-implant soft tissues.37
CONCLUSION
The ACP — in collaboration with a scientific panel appointed by the ACP, ADA, AGD, and ADHA, and based on two rigorous systematic reviews — has developed and approved Clinical Practice Guidelines for Recall and Maintenance of Patients With Tooth-Borne Dental Restorations and Clinical Practice Guidelines for Recall and Maintenance of Patients With Implant-Borne Dental Restorations (available at onlinelibrary.wiley.com/doi/10.1111/jopr.12416/full).6 They serve as a baseline and reflect up-to-date scientific evidence and best clinical practices. These guidelines will aid in the prevention of post-procedural complications, early detection of risk factors and risk reduction, and will improve sustainability and longevity of tooth-borne and implant-borne dental restorations.
References
- Gay IC, Tran DT, Weltman R, et al. Role of supportive maintenance therapy on implant survival: a university-based 17 years retrospective analysis. Int J of Dent Hyg. December 22, 2015. Epub ahead of print.
- Costa FO, Takenaka-Martinez S, Cota LO, et al. Peri-implant disease in subjects with and without preventive maintenance: A 5-year follow-up. J Clin Periodontol. 2012;39:173–181.
- Jepsen S, Berglundh T, Genco R, et al. Primary prevention of peri-implantitits: managing peri-implant mucositis. J Clin Periodontol. 2015;42:S152–S157.
- Bidra AS, Daubert DM, Garcia LT, et al. A systematic review of recall regimen and maintenance regimen of patients with dental restorations. Part 1: Tooth-borne restorations. J Prosthodont. 2016;25:S2–S15.
- Bidra AS, Daubert DM, Garcia LT, et al. A systematic review of recall regimen and maintenance regimen of patients with dental restorations. Part 2: Implant-borne restorations. J Prosthodont. 2016;25:S16–S31.
- Bidra AS, Daubert DM, Garcia LT, et al. Clinical practice guidelines for recall and maintenance of patients with tooth-borne and implant-borne dental restorations. J Prosthodont. 2016;25:S32–S40.
- Patel S, Bay C, Glick M. A systematic review of dental recall intervals and incidence of dental caries. J Am Dent Assoc. 2010;14:527—539.
- Teich ST. Risk Assessment-Based Individualized Treatment (RABIT): a comprehensive approach to dental patient recall. J Dent Educ. 2013;77:448–457.
- Featherstone JDB, Gansky SA, Hoover CI, et al. Cariogenic bacteria trends in a randomized caries management clinical trial. J Dent Res. 2002;81:3813.
- Featherstone JDB. The caries balance: contributing factors and early detection. J Calif Dent Assoc. 2003;31:129–133
- Kye W, Davidson R, Martin J, et al. Current status of periodontal risk assessment. J Evid Based Dent Pract. 2012;12:2–11
- Chapple ILC, Van der Weijden F, Doerfer C, et al. Primary prevention of periodontitis: managing gingivitis. J Clin Periodontol. 2015; 42(Suppl 16):S71–S76.
- Ikai H, Kanno T, Kimura K, et al. A retrospective study of fixed dental prostheses without regular maintenance. J Prosthodont Res. 2010;54:173–178.
- Ribeiro DG, Pavarina AC, Giampaolo ET, et al. Effect of oral hygiene education and motivation on removable partial denture wearers: longitudinal study. Gerodontology. 2009;26:150–156.
- Ercalik-Yalcinkaya S, Ozcan M. Association between oral mucosal lesions and hygiene habits in a population of removable prosthesis wearers. J Prosthodont. September 17, 2014. Epub ahead of print.
- Ortolan SM, Viskić J, Stefancić S, et al. Oral hygiene and gingival health in patients with fixed prosthodontic appliances—a 12-month follow-up. Coll Antropol. 2012;36:213–220.
- Wolfart S, Weyer N, Kern M. Patient attendance in a recall program after prosthodontic rehabilitation: A 5-year follow-up. Int J Prosthodont. 2012;25:491–496.
- Ekstrand KR, Poulsen JE, Hede B, et al. A randomized clinical trial of the anti-caries efficacy of 5,000 compared to 1,450 ppm fluoridated toothpaste on root caries lesions in elderly disabled nursing home residents. Caries Res. 2013;47:391–398.
- Nassar CA, Serraglio AP, Balotin A, et al. Effect of maintenance therapy with or without the use of chlorhexidine in teeth restored with composite resin in patients with diabetes mellitus. Gen Dent. 2011;59:149–152.
- López-Jornet P, Plana-Ramon E, Leston JS, et al. Short-term side effects of 0.2% alcohol-free chlorhexidine mouthrinse in geriatric patients: A randomized, double-blind, placebo-controlled study. Gerodontology. 2012;29:292–298.
- Vered Y, Zini A, Mann J, et al. Comparison of a dentifrice containing 0.243% sodium fluoride, 0.3% triclosan, and 2.0% copolymer in a silica base, and a dentifrice containing 0.243% sodium fluoride in a silica base: A three-year clinical trial of root caries and dental crowns among adults. J Clin Dent. 2009;20:62–65.
- United States Food and Drug Administration. Triclosan: What Consumers Should Know. Available at: fda.gov/ForConsumers/ConsumerUpdates/ucm205999.htm. Accessed August 15, 2016.
- Yee AL, Gilbert JA. Is triclosan harming your microbiome? Science. 2016;353:348–349.
- Zenthöfer A, Dieke R, Dieke A, et al. Improving oral hygiene in the long-term care of the elderly—a RCT. Community Dent Oral Epidemiol. 2013;41:26–268.
- Morino T, Ookawa K, Haruta N, et al. Effects of professional oral health care on elderly: randomized trial. Int J Dent Hyg. 2014;12:291–297.
- De Visschere L, Schols J, van der Putten GJ, et al. Effect evaluation of a supervised versus non-supervised implementation of an oral health care guideline in nursing homes: A cluster randomised controlled clinical trial. Gerodontology. 2012;29:96–106
- Wittneben J, Buser D, Salvi GE, et al. Complication and failure rates with implant-supported fixed dental prostheses and single crowns: a 10-year retrospective study. Clin Impl Dent and Related Res. 2014;16:356–364.
- Pjetursson BE, Thomas D, Jung R, et al. A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after a mean observation period of at least 5 years. Clin Oral Implants Res. 2012;6:22–38.
- Pjetursson BE, Bragger U, Lang NP, et al. Comparison of survival and complication rates of tooth-supported fixed dental prostheses (FDPs) and implant-supported FDPs and single crowns (SCs). Clin Oral Impl Res. 2007;18:97–113.
- Paolantonio M, Perinetti G, D’Ercole S, et al. Internal decontamination of dental implants: An in vivo randomized microbiologic 6-month trial on the effects of a chlorhexidine gel. J Periodontol. 2008;79:1419–1425.
- Sreenivasan PK, Vered Y, Zini A, et al. A 6-month study of the effects of 0.3% triclosan/copolymer dentifrice on dental implants. J Clin Periodontol. 2011;38:33–42.
- Ramberg P, Lindhe J, Botticelli D, et al. The effect of a triclosan dentifrice on mucositis in subjects with dental implants: A six-month clinical study. J Clin Dent. 2009;20:103–107.
- Fischer K, Stenberg T. Prospective 10-year cohort study based on a randomized, controlled trial (RCT) on implant-supported full-arch maxillary prostheses. Part II: Prosthetic outcomes and maintenance. Clin Implant Dent Related Res. 2013;15:498–508.
- Swierkot K, Brusius M, Leismann D, et al. Manual versus sonic-powered toothbrushing for plaque reduction in patients with dental implants: An explanatory randomized controlled trial. Eur J Oral Implantol. 2013;6:133–144.
- Rasperini G, Pellegrini G, Cortella A, et al. The safety and acceptability of an electric toothbrush on peri-implant mucosa in patients with oral implants in aesthetic areas: A prospective cohort study. Eur J Oral Implantol. 2008;1:221–228.
- Vandekerckhove B, Quirynen M, Warren PR, et al. The safety and efficacy of a powered toothbrush on soft tissues in patients with implant-supported fixed prostheses. Clin Oral Investig. 2004;8:206–210.
- Mussano F, Rovasio S, Schierano G, et al. The effect of glycine-powder airflow and hand instrumentation on peri-implant soft tissues: A split-mouth pilot study. Int J Prosthodont. 2013;26:42–44.
From Decisions in Dentistry. August 2016;2(09):37–42.





Amazing article! A must read for all dental professionals!